Medicaid Facilitates Access To Care
A large body of research shows that Medicaid beneficiaries have far better access to care than the uninsured and are less likely to postpone or go without needed care due to cost. Moreover, rates of access to care and satisfaction with care among Medicaid enrollees are comparable to rates for people with private insurance . Medicaid coverage of low-income pregnant women and children has contributed to dramatic in the U.S. A growing body of research indicates that Medicaid eligibility during childhood is associated with reduced teen mortality, improved long-run educational attainment, reduced disability, and lower rates of hospitalization and emergency department visits in later life. Benefits also include second-order fiscal effects such as increased tax collections due to higher earnings in adulthood. Research findings show that state Medicaid expansions to adults are associated with increased access to care, improved self-reported health, and reduced mortality among adults.
Figure 7: Nationally, Medicaid is comparable to private insurance for access to care the uninsured fare far less well.
What Types Of Health Care Does Medicaid Cover
There are 56 different Medicaid programs — one for each state, the District of Columbia, and the U.S. territories. Each Medicaid program may help pay for different types of health care. What you pay varies, too.
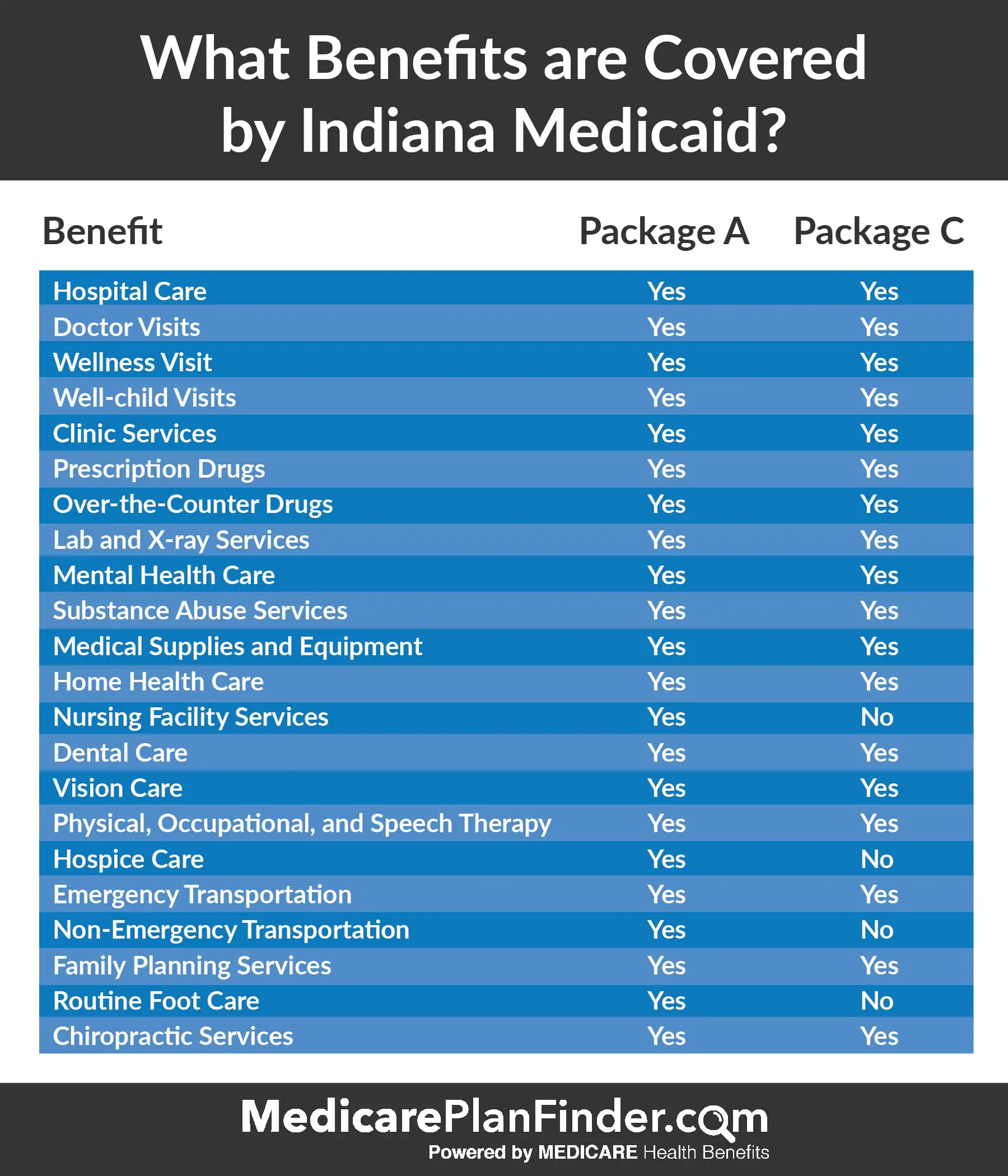
You can use Medicaid for many types of health care. Medicaid covers screening and diagnostic tests, including X-rays. It helps pay for hospital stays and doctor visits. Prescription drugs are covered and so is family planning. It also covers nursing home and long-term care services for people with lower incomes.
If you have a child who qualifies, Medicaid covers even more. You may get financial help if your child needs to see an eye doctor or needs glasses. Mental health services are covered. So is long-term care in your home if your child needs it.
You can get financial help if your spouse needs to be in a nursing home. Long-term care is costly. If you qualify, Medicaid can help make sure you have enough money to stay in your home while your spouse gets care elsewhere.
Unmarried Dependent Child Of Veteran/active Duty Member
Eligibility as an unmarried dependent child of a veteran or active duty member ends with the month after the month any of the following occur:
- Loss of dependent status.
- The active duty member separates from the armed forces with a discharge that is not characterized as honorable or that is based on alien status.
- Legal adoption by someone other than the veteran or active duty member of the armed forces or the veteran/active duty memberâs spouse.
Recommended Reading: Is Health Insurance Required In Florida
Read Also: Does Medicaid Cover Swimming Lessons
Two Categories Of Medicaid Eligibility
Before the Affordable Care Act, Medicaid eligibility was based on how much money you earned and how much you owned, e.g., your income, your assets, and your net worth. After the law was enacted, however, eligibility was split into two distinct groups.
Some people continued to qualify for Medicaid the old fashioned way, while others qualify based on their modified adjusted gross income .
Read Also: Will My Health Insurance Pay For An Auto Accident
Who Can Get Medicaid
- No matter your state, you may qualify for Medicaid based on your income, household size, disability, family status, and other factors. But if your state has expanded Medicaid coverage, you can qualify based on your income alone.
- Enter your household size and state. We’ll tell you who is eligible for Medicaid, if your state expanded and if you qualify for Medicaid based only on your income.
- If you think you have Medicaid eligibility, you can create an account and fill out a Marketplace application. If it looks like anyone in your household qualifies for Medicaid or CHIP, we’ll send your information to your state agency. They’ll contact you about enrollment. You can apply any time of year.
- If you don’t qualify for Medicaid, we’ll tell you if you qualify for financial help to buy a Marketplace health plan instead.
You May Like: Birthing Centers That Accept Medicaid
Q If I Dont Qualify For Medicaid Is There Any Other Help For Me Or My Children
A. Yes. Many organizations in Delaware are dedicated to the principle that health care should never be beyond the reach of those who need it. If you need health care, but do not have insurance coverage, the people at the Delaware HelpLine have a wealth of information about organizations that provide health care at reduced rates for uninsured individuals. Call the Delaware HelpLine toll-free at 1-800-464-HELP from Monday Friday from 8:00 a.m. to 5:00 p.m. The Delaware Helpline service is also available in Spanish. Additional information about the support provided by the Delaware Helpline can also be found by visiting www.delawarehelpline.org.
For example, you may qualify to receive discounted medical services through the Community Healthcare Access Program . CHAP helps connect uninsured individuals with affordable health care from primary care doctors, medical specialists, and other health providers including prescription programs, laboratory and radiology services. To find out more about this program, visit the website for the Community Healthcare Access Program, or call 1-800-996-9969 for eligibility guidelines.
You can read about CHAP and other healthcare resources for uninsured individuals in the Delaware Healthcare Resource Guide. This guide is also available in Spanish: Guía de Recursos de Salud.
Under 18:
Over 65:
Disadvantages Of Having Medicaid And Private Insurance
If youre eligible for Medicaid, youre no longer eligible for any premium tax credits on Obamacare coverage. As a result, rather than Medicaid saving you money, it could actually increase your premiums if you continue to carry the plan you bought from the Marketplace.
There could also be a disadvantage even if your private insurance plan isnt a Marketplace plan, but is provided by your employer. If you choose to keep Medicaid and your employer insurance, maintaining your employer-sponsored coverage likely means continuing to pay substantial costs for premiums.
Read Also: Does Ssdi Count As Income For Medicaid
How To Apply For Medicaid
If you are 18 or older, you can apply for Medicaid through your local Home and Community Services office or online.
There are three main parts to the application process:
How Mepd Services Are Provided
If you’re an adult with a disability and qualify for MEPD, these services are typically provided by STAR+PLUS. You will choose a STAR+PLUS health plan from the ones available in your service area.
If you have a child with a disability who qualifies for MEPD, these services are typically provided by STAR Kids. You will choose a STAR Kids health plan from the ones available in your service area.
You might also be enrolled into traditional Medicaid. Traditional Medicaid just means the state pays your doctors, nurses and other caregivers directly.
You May Like: Is Medicaid Available In All States
Medicaid For The Elderly & People With Disabilities
Seniors, adults with disabilities and some children with disabilities who don’t have health insurance might be able to get health coverage through the Medicaid for the Elderly and People with Disabilities program.
You might be able to get Medicaid even if you’re already on Medicare. If you need help paying your Medicare premiums, click here.
To learn more about all your options, contact your local Aging and Disability Resource Center or call 2-1-1.
To get MEPD, you must be a Texas resident and a U.S. citizen or qualified non-citizen. When you apply, we’ll ask about your income, your age, and your disability to see if you qualify.
MEPD covers health care services, including:
- Regular checkups at the doctor.
- Medicine and vaccines.
- Access to medical specialists and mental health care.
- Treatment of special health needs and pre-existing conditions.
MEPD also covers long-term services and supports, including:
- Home care and personal care, like having someone help monitor your health and help you with daily activities.
- Having somebody take your child to their medical appointments.
- Nursing home care.
- A hospital for mental illnesses.
- A place of care for people with intellectual disabilities.
Do All Health Insurance Companies Have To Offer Cover Mental Health
Health insurance providers arent legally required to offer mental health coverage. The federal parity law instead says that insurers that provide mental health coverage must provide mental health/substance use disorder treatment thats equal to or better than physical health coverage.
For example, under the federal parity law, an insurance company cant charge a $25 copay for an annual checkup with a primary care provider and a $100 copay for a psychologist visit. The law also makes it harder for insurance companies to limit mental health-related appointments annually.
The federal parity law applies to many types of health insurance, including ACA marketplace plans, employer-sponsored coverage , Medicaid and the Childrens Health Insurance Program . Medicare is exempt from the federal parity law.
Read Also: Best Dentist That Accept Medicaid
If Your Income Is Low And Your State Hasnt Expanded Medicaid
If your state hasnt expanded Medicaid, your income is below the federal poverty level, and you dont qualify for Medicaid under your states current rules, you wont qualify for either health insurance savings program: Medicaid coverage or savings on a private health plan bought through the Marketplace.
- Find out why
-
- When the health care law was passed, it required states to provide Medicaid coverage for all adults 18 to 65 with incomes up to 133% of the federal poverty level, regardless of their age, family status, or health.
- The law also provides premium tax credits for people with incomes between 100% and 400% of the federal poverty level to buy private insurance plans in the Health Insurance Marketplace®.
- The U.S. Supreme Court later ruled that the Medicaid expansion is voluntary with states. As a result, some states havent expanded their Medicaid programs.
- Adults in those states with incomes below 100% of the federal poverty level, and who dont qualify for Medicaid based on disability, age, or other factors, fall into a gap.
- Their incomes are too high to qualify for Medicaid in their states.
- Their incomes are below the range the law set for savings on a Marketplace insurance plan.
-
States are continuing to make coverage decisions. They could expand Medicaid in the future.
Who Qualifies As A Dependent For Insurance

Generally speaking, you can include any child who fits the following criteria: Age: Your child has to be under the age of 26. Relationship to You: For a child to qualify as your dependent, he or she needs to be your biological child, your stepchild, your adopted child, or a foster child you are taking care of.
Recommended Reading: How Much Can You Make And Still Receive Medicaid
Q Who Qualifies For Medicaid
A. Citizenship and Residency – To obtain full Medicaid benefits in Delaware, you must be a Delaware resident and either a U.S. citizen or a legally residing noncitizen. Full coverage for noncitizens which include DACA recipients is dependent on the availability of state funding. However, noncitizens can qualify for coverage for emergencies and labor & delivery services if income requirements are met.
Income Level – Qualifying for Medicaid is also based on need. Household income must be under certain limits as defined by the Federal Poverty Level and is based on family size. For Long Term Care programs, financial resources must also be under a certain amount. There are also specific programs for individuals who meet certain medical or disability tests, or who qualify due to age or pregnancy. To find out more about different Medicaid and other medical assistance programs, visit DMMA Programs & Services.
What Makes Health Care So Expensive
The price of medical care is the single biggest factor behind U.S. healthcare costs, accounting for 90% of spending. These expenditures reflect the cost of caring for those with chronic or long-term medical conditions, an aging population and the increased cost of new medicines, procedures and technologies.
$383 a monthincreases with age
There are seven ways to obtain insurance if you are aging off of your parents insurance plan. But before choosing an insurance plan as a young adult, you need to evaluate your own situation, determining, for example, what you need in a health plan and how much you can afford.
If you are healthy, you may not need a comprehensive and more expensive health plan that is designed for someone with chronic illnesses. By the same token, if you are a young adult with a chronic illness, you may need a more comprehensive plan.
There are other considerations. A young adult who is planning to start a family will have different coverage needs than a young, single adult starting their first job and living alone.
Also Check: What State Has The Best Medicaid Benefits
Also Check: Where Can I Apply For Medicaid In Florida
How Do You Get Health Insurance If You Dont Qualify For Medicaid
Every state has different criterias to find out who qualifies for Medicaid. You may be qualified for Medicaid if:
- Youre handicapped.
- District of Columbia
Although there is no penalty for being uninsured, it is still advised that people have some sort of health coverage. Healthcare costs in America are constantly rising. Therefore, it is better to have an insurance plan that keeps you covered in times of need. If you unfortunately have to go to the hospital for an emergency, need to have a surgery, or face a severe accident, you will end up in the hospital. You do not want to be handed a hospital bill of worth thousands of dollars now, do you? Therefore, having health insurance will provide coverage in dire situations and you wont have to worry about huge hospital bills.
What Changes When A Woman Already Enrolled In Medicaid Becomes Pregnant
Generally, nothing. A woman who was previously eligible and enrolled in full-scope Medicaid who becomes pregnant continues to be eligible, and will be able to access pregnancy services. A woman who becomes pregnant while enrolled in Medicaid Expansion can stay in that coverage, at least until redetermination. The state must inform the woman of the benefits afforded to pregnant women under other coverage categories, such as pregnancy-related Medicaid, and provide the option to switch categories if the woman is eligible.
Also Check: Can I Change Medicaid Plan
What Is A 1095
- Form 1095-B is a tax document that includes information about the health coverage provided for one or more months during the year to you, your spouse and individuals you can claim as dependents.
- This form relates only to coverage provided by state Medicaid and CHIP agencies.
- The healthcare law requires health coverage providers, including state Medicaid and CHIP agencies, to provide these documents to the IRS and covered individuals.
- Receipt of this form does not create a federal tax return filing requirement with the IRS. Please check IRS.gov and the Form 1040 instructions to determine if you have a federal income tax return filing requirement.
- Keep Form 1095-B with your records. You do not need to attach the form to your income tax return.
- For more information about Form 1095-B, and other health care tax documents, please visit IRS.gov/aca.
Please note: Effective April 1st, 2021, Wyoming Medicaid will no longer require 40 qualifying work quarters for Lawful Permanent Residents.
Types Of Health Insurance Plans
- Health maintenance organization health insurance plans generally require referrals to see specialists. You wont be covered if you seek care outside of the network, unless its for emergency care.
- Preferred provider organization health insurance plans usually dont require referrals from your primary doctor to see specialists. PPO plans allow you to get medical care from a provider outside the network, but the services are covered at a much smaller percentage.
- Exclusive provider organization health insurance plans allow you to see a specialist without a referral, as long as its in network. EPO plans dont pay for out-of-network care, unless its a medical emergency.
Recommended Reading: Methadone Clinics That Take Medicaid
Reasons Relating To Material Change In Income Or Resources During Six Months Preceding Approval For Assistance
A change in income or resources should be regarded as material only if the amount of the reduction or loss of income is substantial in relation to the need for assistance. A loss of income that is based on need, such as assistance from a public or private agency, is not regarded as a material change in income.
Is It Worth It To Keep Both
To decide whether its worth it to maintain both coverages, run the numbers to see what your total out-of-pocket cost would be for only Medicaid versus Medicaid with your private insurance. Pay special attention to what your states Medicaid covers since it could be worth it to keep your private insurance if your states Medicaid doesn’t provide all the coverage you need.
To help you decide, lets back up a bit and go over some basic information about Medicaid and private health insurance.
Also Check: Psychiatrist That Accept Medicaid Nyc
Medicaid As Secondary Insurance
Can you use Medicaid as a secondary insurance? If you take your employers insurance or you have private coverage, you might still have trouble paying deductibles and co-pays. But qualified low-income families and individuals might be able to cover co-pays, deductibles, and insurance premiums by using Medicaid as a secondary insurance.
Just keep in mind that Medicaid is always the last resort payer if you have coverage through another agency. Secondary payers usually cover the smaller amount, like coinsurance or co-pay, while primary insurance covers the bigger costs.