How Are These Categories Different From Normal Medicaid Eligibility
Each of these eligibility programs are designed to meet the unique needs of people who are aging, disabled or have excessive medical bills. In almost all cases, they do not otherwise qualify for Medicaid. However, once enrolled, all of these recipients get the same full benefit Medicaid coverage as everyone else.
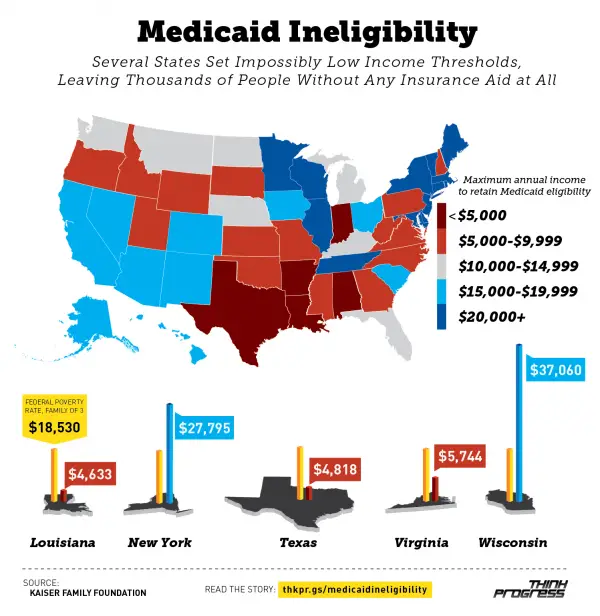
What Is The Medicaid Income Limit In My State
Most states use a standard of 138% of the federal poverty level as a basis for Medicaid eligibility. But each state is free to set its own limits.
The table below shows the income limit as a percentage of the FPL required for Medicaid eligibility in each state for two-parent households and for individuals adults.
If 0% appears, that means individuals may not qualify for Medicaid in that state based on income alone and must meet other criteria, such as being pregnant or disabled.
|
State |
|
|---|---|
| 52% | 0% |
FPL is used to determine eligibility for Medicaid, certain welfare benefits and other assistance programs. The FPL is computed by the U.S. Census Bureau and can be adjusted every year based on inflation.
Medicaid uses a percentage of the FPL to determine its income limits for eligibility. For example, you may qualify for Medicaid if you earn less than 133% of the federal poverty level. Or you may qualify if you earn less than 150% of the federal poverty level and are disabled. Again, each state sets its own income limits to determine Medicaid eligibility.
Contact your state Medicaid program for more eligibility information, as most states offer different types of Medicaid programs that may each have their own income limits and other qualifying criteria. Even if you make more than the standard limit found below, there may be additional programs for which you still qualify.
Effective Date Of Coverage
Once an individual is determined eligible for Medicaid, coverage is effective either on the date of application or the first day of the month of application. Benefits also may be covered retroactively for up to three months prior to the month of application, if the individual would have been eligible during that period had he or she applied. Coverage generally stops at the end of the month in which a person no longer meets the requirements for eligibility.
Recommended Reading: Does Medicare Or Medicaid Pay For Weight Loss Surgery
Q How Much Income Can I Receive And Still Be Eligible For Medicaid
A. Income is money that you get from working, or money that someone gives you, or checks that you receive, such as a Social Security check, unemployment benefits, child support, retirement benefits, or sick pay. Whether your income level qualifies you or your family for Medicaid depends on the size of your family and the Medicaid program for which you are applying.
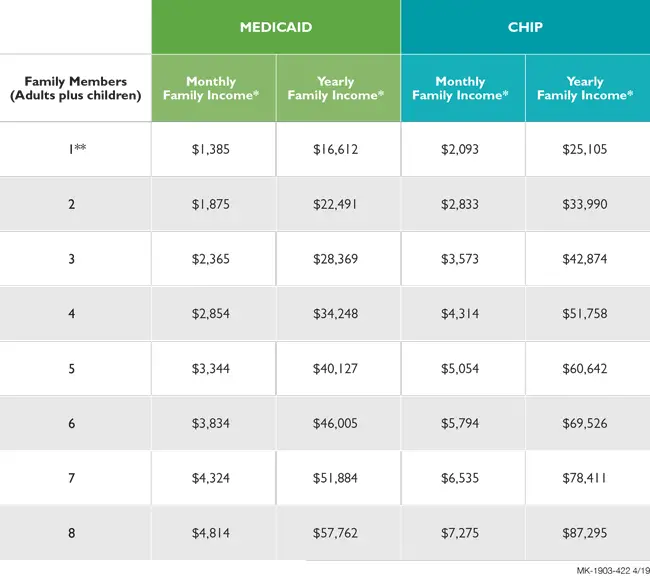
Income limits are set each year by the federal government to define the Federal Poverty Level for different family sizes. In general, if your household income is at or below the current 100% Federal Poverty Level for your household size, your family is likely to be eligible for Medicaid. Children from age 1 to under age 6 can qualify for Medicaid benefits when household income is at or below 133% of the Federal Poverty Level. Pregnant women and infants under age 1 qualify for Medicaid with family income at or below the 200% Federal Poverty Level, and pregnant women count as 2 family members.
See our tables of income limits for applying for DMMA programs to find out where your family income is, in relation to these income benchmarks.
Medical assistance programs other than Medicaid have different income level requirements. For example, uninsured children under age 19 who live in families with incomes at or below the 200% Federal Poverty Level are eligible for low cost health insurance under the Delaware Healthy Children Program.
What Medicaid Helps Pay For
If you have Medicare and qualify for full Medicaid coverage:
- Your state will pay your Medicare Part B monthly premiums.
- Depending on the level of Medicaid you qualify for, your state might pay for:
- Your share of Medicare costs, like deductibles, coinsurance, and copayments.
- Part A premiums, if you have to pay a premium for that coverage.
Also Check: Information Needed To Apply For Medicaid
Who Would Be Impacted By The Loss Of These Eligibility Categories
People who are impacted get their Medicaid from four eligibility categories:
- Provisional Medicaid covers individuals who are either age 65 and older or disabled with monthly income less than $750.
- The Medically Needy and Medically Needy Spend Down Programs cover some individuals whose medical expenses exceed their income.
The Long Term Care Special Income Level program covers individuals who are aged, blind or disabled who qualify for institutional level of care because of their medical needs and who have monthly income between $750 and $2,250.
Unemployed Applicants Should Use State Or Federal Marketplace
An unemployed person can apply for health insurance on the federal or state exchanges. They may find affordable low-premium options based on family income. Should they not find an affordable option, they may qualify for an exemption, Medicaid, or the CHIP.
Many states offer assistance to low-income families to help them qualify for affordable health insurance including payment assistance. If income is below the minimum needed for Obamacare, then applicants can seek coverage under the applicable state Medicaid program or CHIP for minors.
Also Check: How Can I Get Medicaid In Florida
You May Like: Louisiana Medicaid Weight Loss Surgery
How Much Will Medicaid Cost Me
It depends. Every state is different. You will probably not have to pay a monthly premium for Medicaid, but most people do have some out-of-pocket costs.2 Emergency services, family-planning services, pregnancy-related services and preventive care for children are all fully covered with no additional cost to you.
Medicaid As Secondary Insurance
Can you use Medicaid as a secondary insurance? If you take your employers insurance or you have private coverage, you might still have trouble paying deductibles and co-pays. But qualified low-income families and individuals might be able to cover co-pays, deductibles, and insurance premiums by using Medicaid as a secondary insurance.
Just keep in mind that Medicaid is always the last resort payer if you have coverage through another agency. Secondary payers usually cover the smaller amount, like coinsurance or co-pay, while primary insurance covers the bigger costs.
Recommended Reading: Dentist In Madisonville Ky That Accept Medicaid
Q How Long Will My Medicaid Benefits Remain Active
A. Medicaid is based on month to month eligibility. However, your benefits are redetermined on a yearly basis by DMMA to confirm whether you still remain eligible for the program you are receiving. Certain Medicaid programs require you to report changes in your situation within 10 days of the change. One example of a change that must be reported is new employment.
Medicaid Enrollees Experience Income Changes That Lead To Coverage Disruption
Medicaid eligibility is based on a familys current monthly income. Once they enroll, most enrollees have 12 months before they must renew their coverage, but during the 12 months they must report any changes that affect their eligibility. If they report a change that makes them ineligible, they lose coverage. In addition to the requirement that enrollees report changes, many states regularly check data sources such as quarterly wage reports and, if they find information suggesting enrollees may be ineligible, they require that enrollees provide information showing they remain eligible. If enrollees dont respond to the request for information within a short period of time or are unable to show they remain eligible, they lose coverage.
People often dont receive a request for information or dont respond to it in time, or they may have worked overtime or picked up an extra shift that temporarily put them over the eligibility threshold. Many enrollees reenroll in Medicaid within months of losing coverage, a process known as churn. Others arent aware they are still eligible or are unable to successfully reapply, and they remain uninsured.
Also Check: Arkansas Medicaid Program Phone Number
Why Are Letters Going Out Now
Two reasons. First, we want to give everyone impacted by this cut as much notice as possible in order to make plans for such a change and begin the process of seeing if individuals may be eligible for other services. We know from speaking with some individuals and their families already that explaining these complex reductions can take time.
Second, because of federally required timelines and approval processes, we must start the public notice step of rulemaking, CMS notification and their approval process. This could be lengthy. We believe it to be responsible to explain to enrollees what that public notice means, provide advice on applying for other available programs, and how to contact us if they have questions.
When And Why Was The Federal Poverty Level Established
The federal poverty thresholds were first introduced in 1965, based on the work of the Social Security Administrations Mollie Orshansky. The amounts were tied to the bare minimum amount that people needed in order to have adequate food, with a multiplier used to account for other necessary expenses. Orshansky noted at the time that the poverty thresholds were a measure of the amount of income that would be inadequate for people to live, as opposed to a minimum adequate amount.
Dont Miss: Apply For Montana Medicaid Online
Recommended Reading: Healthy Connections Medicaid Sc Phone Number
Medicaid Is Structured As A Federal
Subject to federal standards, states administer Medicaid programs and have flexibility to determine covered populations, covered services, health care delivery models, and methods for paying physicians and hospitals. States can also obtain Section 1115 waivers to test and implement approaches that differ from what is required by federal statute but that the Secretary of HHS determines advance program objectives. Because of this flexibility, there is significant variation across state Medicaid programs.
The Medicaid entitlement is based on two guarantees: first, all Americans who meet Medicaid eligibility requirements are guaranteed coverage, and second, states are guaranteed federal matching dollars without a cap for qualified services provided to eligible enrollees. The match rate for most Medicaid enrollees is determined by a formula in the law that provides a match of at least 50% and provides a higher federal match rate for poorer states .
Figure 2: The basic foundations of Medicaid are related to the entitlement and the federal-state partnership.
How To Apply For Medicaid
If youre eligible for Medicaid, you can apply all year round through your state’s Medicaid website or HealthCare.gov, the federal health insurance marketplace. If you apply for Medicaid through Healthcare.gov and it looks like you qualify, the federal government will notify your state agency, which will contact you about enrollment. States also generally let you print out paper applications you can mail, fax or return directly to your local government office.
To complete your Medicaid application, you will likely need to provide documentation that you meet your state’s requirements. This documentation may include:
-
Your birth certificate or driver’s license to serve as proof of age and citizenship
-
Recent pay stubs or tax returns to serve as proof of income
-
Copies of bank statements
-
Proof of address, which could include a lease, utility bill statements or a copy of your mortgage
-
Medical records to serve as proof of disability
States have 45 days to process your Medicaid application. They have 90 days if eligibility is tied to a disability . Processing can take longer if applicants do not supply all of the required documentation. If you don’t qualify for Medicaid, you might be able to get subsidized health insurance through Healthcare.gov. However, only certain life events allow you to apply for a marketplace health care plan outside of open enrollment, which takes place from Nov. 1 to Jan. 15.
Ready to shop for life insurance?
Don’t Miss: How Soon Can I Get Medicaid
Coverage Gaps Lead To Higher Health Care Costs
When individuals lose Medicaid coverage, go for a period without health care, and then reenroll, their health care costs are often higher than if they received continuous coverage. A gap in coverage may lead to interruptions in access to Medicaid, therapies, and other medical care. It can also lead to delays in screening, detection, and treatment of cancer.
Delayed or skipped treatment often leads to worsening conditions and greater use of high-cost care. Studies show individuals may only reenroll when they receive expensive hospital care, which often could have been avoided had enrollees coverage and access to care continued without interruption. For example, one study showed that adults with Type 1 diabetes who experience an interruption in coverage used acute care five times more frequently after the interruption than before.
Studies of Medicaid expenditure data have shown higher costs for individuals enrolled for shorter periods of time. An adult enrolled for a full 12 months had estimated average Medicaid costs of $326 per month, while someone enrolled for only one month has average Medicaid costs of $705 per month, data from 2012 showed.
Q How Will I Receive My Medical Care
A. In Delaware, Medicaid benefits are provided mainly through a managed care organization, or MCO, under contract with the state. Managed care is an organized way to ensure that people receive the quality medical care they need in the most cost-effective manner. Some Medicaid recipients in Delaware those who also receive Medicare and those in Long Term Care Medicaid programs such as the Nursing Facility program do not receive their medical care through a managed care organization.
DMMA provides a choice of managed care organizations so you can select the MCO plan that is best for you and your family. Delaware contracts with two managed care plans AmeriHealth Caritas and Highmark Health Options.
The Medicaid MCO provides almost all of the care for Medicaid members who join their plan. Prescription and non-emergency medical transportation services are covered directly by Medicaid, not through the MCO. Medicaid recipients need to show their Medicaid card to pharmacies and transportation providers when receiving these services.
Recommended Reading: What Is Needed To Apply For Medicaid
Calculating Your Cpp Benefit
To know how much CPP youll get, you need to calculate your benefit. It goes off a number of factors:
- How long you worked.
- How much you paid in.
- The age at which you took the benefit.
- Whether you have other pension income .
Doing all the CPP calculations by hand can be tough. So, I recommend using the retirement income calculator on Canada.ca. This online app walks you through a series of questions that leads you to an estimate of your monthly CPP benefit. It may not be 100% accurate, but it should be in the right ballpark.
Read Also: General Doctor That Accepts Medicaid
Im Single And Just Lost My Job Is Medicaid For Me
Maybe. Medicaid eligibility is based on where you live, how much money you make each year and the number of people in your household.
Its worth applying even if you dont think you qualify. Whether you have children, are pregnant or have a disability are all taken into consideration. You can check to see whats offered in your state through the Aetna Better Health website.
Do I qualify for Medicaid?
Those who earn less than a certain amount can qualify for Medicaid.
Depending on the state where you live, you can be covered if your income is below these ranges:
$16,970-$25,520 for a household of one
$22,929-$34,480 for a household of two
$28,887-$43,440 for a household of three
$34,846-$52,400 for a household of four
Also Check: Best Medicaid Plan In Utah
If I Get Medicaid But Am Offered Private Insurance With Work But Cost Too Much Can I Stay With Medicaid
There is no easy answer to this question because there are several different things that could happenâ¦.you could keep the Medicaid and not take the insurance through your job however if for some reason you lose the Medicaid you may have missed the open enrollment period with your employer. If that happens you will still be able to get health insurance but based on your income you may not qualify for any tax credits.
Hope this helps clarify everything!!
Read Also: How To Qualify For Medicaid In Utah
Medicaid Is Jointly Financed By States And The Federal Government
Medicaid is financed jointly by the federal government and states. The federal government matches state Medicaid spending. The federal match rate varies by state based on a federal formula and ranges from a minimum of 50% to nearly 75% in the poorest state. Under the ACA, the federal match rate for adults newly eligible was 100% for 2014-2016, phasing down gradually to 90% in 2020 and thereafter . The federal matching structure provides states with resources for coverage of their low-income residents and also permits state Medicaid programs to respond to demographic and economic shifts, changing coverage needs, technological innovations, public health emergencies such as the opioid addiction crisis, and disasters and other events beyond states control. The guaranteed availability of federal Medicaid matching funds eases budgetary pressures on states during recessionary periods when enrollment rises. Federal matching rates do not automatically adjust to economic shifts but Congress has twice raised them temporarily during downturns to strengthen support for states.
Total federal and state Medicaid spending was $577 billion in FY 2017. Medicaid is the third-largest domestic program in the federal budget, after Social Security and Medicare, accounting for 9.5% of federal spending in FY 2017. In 2017, Medicaid was the second-largest item in state budgets, after elementary and secondary education .
Figure 8: Medicaid is a budget item and a revenue item in state budgets.
Don’t Miss: Are Breast Pumps Covered By Medicaid