Diagnosis And Treatmentmedicaid Childrens Services
Children eligible for Medicaid may receive medically necessary diagnostic and treatment services that are not usually covered for the total Medicaid population or that exceed Medicaid limits. A service is medically necessary when it corrects or ameliorates the patients disability, physical or mental illness, or chronic condition.
These additional services are available through Medicaid Childrens Services , the D and T portions of EPSDT. Medicaid Childrens Services in Texas is known as the Comprehensive Care Program .
Some medically necessary services not usually covered for the total Medicaid population or those that exceed Medicaid limits, but which CCP may cover include:
Medical and Dental
Your answer is incorrect. Try again. The correct answer is C. Ankle foot-orthosis falls within the orthotics and prosthetics medical equipment category.
Your answer is correct!Ankle foot-orthosis falls within the orthotics and prosthetics medical equipment category.
To learn more about Medicaid Childrens Services , enroll in the Texas Health Steps provider education module titled Medicaid Childrens Services.
Can Uninsured Immigrant Women Receive Medicaid Or Chip Services
Maybe. Immigrants with qualified non-citizen status are eligible to enroll in Medicaid if they otherwise meet state Medicaid eligibility requirements, but are subject to a five-year waiting period from the time they receive their qualifying immigration status before becoming eligible. Some categories of qualified non-citizens are exempt from the five-year ban because they are considered lawfully residing immigrants. For lawfully residing immigrants, the five-year waiting period was waived in 2010, giving states the option to provide lawfully residing immigrant women with pregnancy-related Medicaid regardless of the length of time they have been in the U.S. Twenty-three states provide pregnancy-related Medicaid to lawfully residing immigrants without waiting periods. For undocumented and DACA-eligible immigrants, states may provide undocumented immigrant women with federally funded prenatal services through CHIP. Some states may also provide prenatal care entirely using state funds.
Regulation Of Birth Attendants In Texas
The birth of your baby is not regulated by the US government, but by individual states. In Texas, out-of-hospital births are almost exclusively performed by midwives. The majority of these midwives are Licensed Midwives, and some are Certified Nurse Midwives. Physicians will be discussed because information about their regulation is useful for comparison. At this time, physician-attended home birth is very rare in Texas, if it happens at all. The differences in training between these practitioners can be found on the PROVIDERS page. This page will cover the legal regulation of these delivery attendants and of the practice of OOH birth in Texas. Licensed Midwives will be emphasized because they are the predominant providers of out-of-hospital birth. The state has regulated midwifery practice since the Texas Midwifery Act was passed in 1983.
In some states, midwifery is still unregulated. This means that simply anyone is allowed to advertise as a traditional midwife and deliver babies. Due to higher safety standards in our state, that type of practice has been eliminated here.
The State of Texas looks to MANA to define what midwifery is, and what makes a midwife competent to perform her job. The State then uses that information, combined with available evidence, to regulate the practice of midwives in the state.
You May Like: Does Medicaid Cover Glasses In Texas
Delivering A Baby Without Health Insurance Coverage
If you dont have health insurance, youll be responsible all the costs for prenatal care and the birth of your child. However, many states make it easier for pregnant women to enroll in Medicaid or a state-sponsored health insurance program, through which all of your health care will be free or very low cost. In California, for example, a pregnant single woman with no other children can get Medicaid even if she earns up to $24,481 per year. If she were not pregnant, she would have to earn less than $15,654 to qualify.
Those who cant get coverage through a public program or through an employer should be able to buy a plan through their states health insurance exchange or through healthcare.gov. Important caveat: unless you have another qualifying event like getting married or divorced or moving to another state, you can only sign up for one of these plans during the open enrollment period between November and January, even if you get pregnant at another time during the year.
If you dont have health insurance, you may be able to negotiate prices with the doctor and hospital where you deliver your child. However, be aware that without insurance, your expenses for a complicated delivery or a seriously ill newborn could reach into the high tens, or even hundreds, of thousands of dollars.
Can An Uninsured Woman Enroll In A Public Health Insurance Plan Upon Becoming Pregnant

Yes, women who meet the eligibility criteria for Medicaid or Childrens Health Insurance Program can enroll in one of these public programs at any point during pregnancy:
Full-Scope Medicaid
A pregnant woman is eligible for full-scope Medicaid coverage at any point during pregnancy if eligible under state requirements. Eligibility factors include household size, income, residency in the state of application, and immigration status. An uninsured woman who is already pregnant at the time of application is not eligible for enrollment in expansion Medicaid.
Pregnancy-Related Medicaid
If household income exceeds the income limits for full-scope Medicaid coverage, but is at or below the states income cutoff for pregnancy-related Medicaid, a woman is entitled to Medicaid under the coverage category for pregnancy-related services and conditions that might complicate the pregnancy. The income limits for pregnancy-related Medicaid vary, but states cannot drop eligibility for this coverage below a legal floor that ranges from an income of 133% to 185% of FPL , depending on the state. States are permitted to set a higher income cutoff.
Childrens Health Insurance Program
Recommended Reading: Ga Medicaid Eligibility Income Chart
Are Ultrasounds Covered By Insurance
If you are able to get insurance during your pregnancy, you will likely find that one or two ultrasounds are mostly covered by insurance. However, if youre unable to get insurance or your carrier does not appear to cover ultrasounds, you may be able to find a facility that offers free ultrasounds in your area.
What Does A Gynecological Exam Include
What the Gynecological Exam Includes Pelvic Exam. The pelvic exam in your gynecological exam is comprised of four main steps: the external genital exam, the speculum exam, the Pap Smear test and the bimanual exam. Pap Smear. A Pap Smear checks for precancerous or cancerous cells. Breast Exam. Urine Sample.
Don’t Miss: How Can You Get Medicaid And Medicare
What If Something Goes Wrong At My Birth
Childbirth, while a natural process, carries risk. There is risk in the process of childbirth that is completely unavoidable. There is also avoidable risk in the process due to human error. This section will explore those human factors and what protections exist for the public surrounding birth attendant malpractice.
Again, well address each provider individually. The hypothetical scenario is the injury or death of mother or baby during labor and delivery. We will mostly discuss the legal consequences of an adverse event during a Texas birth, and what type of accountability exists for these providers. Differences in the types of medical crises or adverse events that different providers are trained to manage are discussed on the PROVIDERS page.
For Physicians:
If there is an adverse outcome in a hospital such as the death of a child, an internal review of the case by a team of physicians and other professionals is immediately triggered. Peer review can include evaluating the merits of a complaint regarding a practitioner, the accuracy of a diagnosis, the quality of care provided, or the qualifications of a practitioner. This review happens as rapidly as possible.
Independent of the Board review process, a malpractice lawsuit may be filed against the physician in question. Any Texas physician employed by a health system or other entity carries malpractice insurance, which will be discussed below.
Licensed Midwives
Application And Renewal For Medicaid Coverage
- The patient/family must complete an application, provide supporting documentation, and have a face-to-face-interview with a benefits counselor before being approved for Medicaid coverage.
- Medicaid coverage must be renewed every six months. A childs coverage may lapse because of changes in the familys financial status, delayed or lack of application for renewal, and other causes. When coverage lapses and then the patient re-enrolls, the patient is not automatically assigned to the same PCP.
- Medicaid provides up to three months of retroactive coverage to new enrollees, including those who have re-enrolled following a lapse.
The State Childrens Health Insurance Program provides health coverage for children in families that earn too much to qualify for Medicaid but cannot afford private health-care coverage. Due to changes in family income status, many children transition from Medicaid to CHIP, or vice-versa. Unlike Medicaid, CHIP does not offer retroactive coverage. Under Texas law, the Department of State Health Services must assist a family whose child loses Medicaid eligibility in making a transition to CHIP without an interruption in coverage.
For questions or information about Medicaid eligibility, patients should contact their caseworker or the local HHSC office. on Medicaid Eligibility and Enrollment that may be used to assist patients in finding online and telephone resources.
Reference Guide to Information on Medicaid Eligibility and Enrollment
Read Also: Bariatric Surgeons That Accept Medicaid In Louisiana
How Much Does It Cost For A Newborn Circumcision
It can be costly to undergo a circumcision to the tune of between $250 and $400 depending on the type.In many cases, you will be forced to bear one bill for the procedure and one bill for the health care provider. How much you owe to your insurance provider can be determined by your policy benefits.
When You Really Really Really Need It Youre Denied
How Texas came to have the worst insurance gaps in the country is no mystery: It was an accumulation of deliberate policy choices by state lawmakers going back decades, driven largely by an aversion to government-mandated insurance and a desire to keep taxes low.
The design of our entire system is to be very limited, and historically we are very distrustful of government in general, said Texas Rep. Sarah Davis, a Houston Republican who chairs the House Appropriations Subcommittee on Health and Human Services. Dr. Amy Raines-Milenkov, a University of North Texas Health Science Center professor and member of the states maternal mortality review committee, believes the states culture of personal responsibility leads it to abandon its most vulnerable. We dont have the belief here that people should have access to health care, she said. Even the safety nets are built on keeping people out rather than pulling people in.
People who dont have children or disabilities cant receive Medicaid, no matter how poor they are. A single mother with two children only qualifies if she earns the equivalent of 17 percent of the federal poverty level or less $230 to $319 per month, depending on whos doing the calculation.
But after the US Supreme Court ruled that states couldnt be forced to accept the Medicaid expansion, Texas became one of 14 states that opted not to a decision that has denied coverage to 1.4 million Texans who would have otherwise qualified for insurance.
Also Check: How Do You Apply For Medicaid In Nj
Medicaid Vs Medicare: They Are Not The Same
Before understanding what services Medicaid covers, its important to clear up any confusion regarding the relationship and the differences between Medicaid and Medicare. Both were created in 1965 in response to the inability of older and low-income Americans to buy private health insurance. Their goal was to allow the financial burdens of illnesses to be shared among sick and healthy people, and affluent and low-income families.
There are clear differences between Medicaid and Medicare, although many people may be eligible for both programs.
Medicaid is a state and federal program that provides health coverage if you have a very low income.
Medicare is a federal program that provides health coverage if you are 65 or older or have a severe disability, no matter what your level of income is.
Medicaid is jointly funded by the federal government and state governments. It is administered by state governments, and each one has broad leeway in determining how Medicaid is implemented. To be reimbursed by the federal government, there are certain mandatory Medicaid benefits that states much offer qualified participants.
For example, if you live in Texas, the federal government requires that inpatient and outpatient hospital services must be covered, among many other mandatory benefits. However, coverage for other services that are considered optional will vary depending on one of the four particulars plan that you decide to enroll in.
What Does Medicaid Cover In Texas
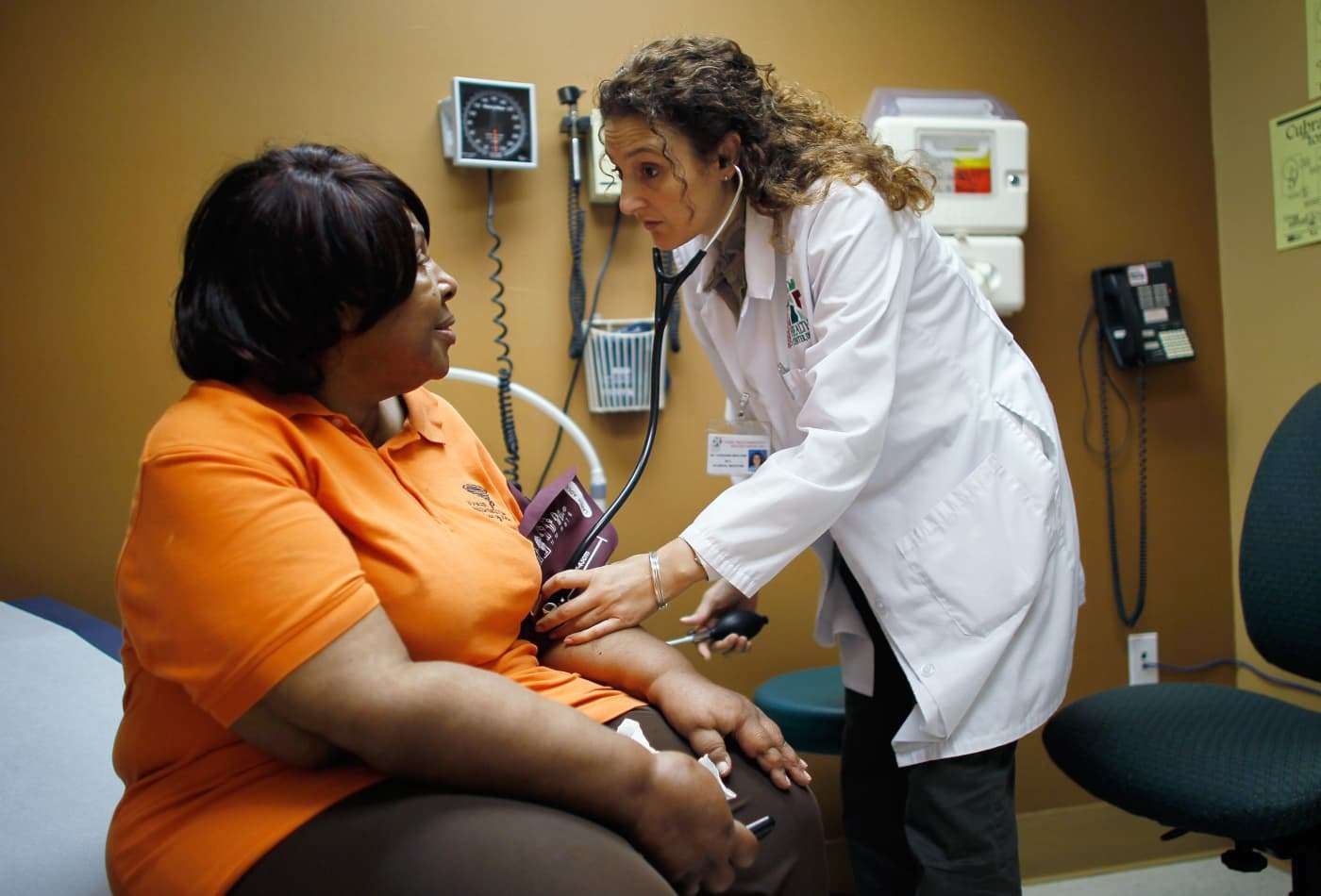
The Texas Medicaid system today covers medical expenses, coordinates complex medical care, and gives Texans access to caring professionals who offer individualized support to enable them to maintain their highest levels of health and wellbeing. Providing medical care, at-home nursing care, and home care at a patients home is one of its many benefits.
You May Like: Medicaid Funded Home Care Services
How Long Does Medicaid Or Chip Coverage For Pregnancy Last
Medicaid or CHIP coverage based on pregnancy lasts through the postpartum period, ending on the last day of the month in which the 60-day postpartum period ends, regardless of income changes during that time. Once the postpartum period ends, the state must evaluate the womans eligibility for any other Medicaid coverage categories.
7. Is abortion covered by Medicaid or CHIP?
The Hyde Amendment, an annual requirement added by Congress to a federal appropriations bill, prohibits using federal funds abortion coverage except when a pregnancy results from rape or incest, or when continuing the pregnancy endangers the womans life. However, states may use their own funds to cover abortions, and 17 states currently do.
Does Medical Cover Newborn Circumcision
With a doctors recommendation on medically necessary for both newborn and non-newborn males, Medicaid must cover the procedure.Some states, such as Louisiana, provide benefits to Medicaid recipients who require frequent urinary tract infections or congenital conditions that cause symptoms of the disorder.
Read Also: Air Purifier Covered By Medicaid
What Does Medicaid Cover In Your State
To give you a better idea of how wide the range of services can be from state to state, heres a comparison of optional benefits for Medicaid coverage in four states:
Medicaid Coverage in Nevada
What does Medicaid cover in Nevada?
Nevada Medicaid provides quality health services to low-income Nevadans who qualify based on state and federal law. Nevada Medicaid does not reimburse an individual for medical services. Payments are sent directly to health care providers when they render services to Medicaid recipients.
Nevada Check Up is offered concurrently with Medicaid and is designed for children who do not qualify for Medicaid but who come from families with incomes that are at or below 200% of the Federal Poverty Level. Nevada Medicaid is the payer of last resort, meaning that if you have other health insurance that can pay a portion of your bills, then payment will be collected from them first. Benefits covered by Nevada Medicaid and Nevada Check Up include:
- Ambulance/Transportation
- Transportation Services
- Waiver Program Services
Medicaid Coverage in Texas
What does Medicaid cover in Texas?
Texas Health and Human Services administers Medicaid and CHIP in the state. It administers four Medicaid programs: STAR, STAR+PLUS, STAR Health and traditional Medicaid. The type of Medicaid coverage a person gets depends on where the person lives and what kind of health issues the person has.
These benefits include:
Medicaid Coverage in New York
What does Medicaid cover in New York?
A Few Frequently Asked Questions About What Medicaid Covers
What coverage do pregnant women get under Medicaid?
Pregnant women are covered for all care related to the pregnancy, delivery and any complications that may take place during pregnancy and up to 60 days postpartum.
Pregnant women may also qualify for care that was received for their pregnancy before they applied and received Medicaid. Some states call this Presumptive Eligibility and it was put in place so that all women would start necessary prenatal care as early in pregnancy as possible. Pregnant women are usually given priority in determining Medicaid eligibility. Most offices try to qualify a pregnant woman within about 2-4 weeks.
Does Medicaid cover VSG?
Vertical sleeve gastrectomy, also known as VSG, is surgery to help with weight loss. Medicaid does not cover weight loss surgery in most cases. However, it is best to check with your state on an individual basis to confirm that they do not offer it as a benefit separate from mandatory federal benefits.
Does Medicaid cover dental services?
Medicaid pays for emergency and medically necessary dental work across the country. Medicaid also pays for comprehensive dental care in more than 30 states. However, others may only cover certain categories of treatments. Medicaid does cover dental services for all child enrollees as part of the Early and Periodic Screening, Diagnostic and Treatment benefit. Check with your state to see what your exact level of dental coverage is.
What does Medicaid cover for children?
Read Also: Moving To Another State Medicaid
Gov Abbott Signs Bill Extending Medicaid Coverage For New Texas Mothers
Starting Sept. 1, new mothers will get a full six months of coverage before being removed from the program.
Gov. Greg Abbott signed a bill this week that expands health care for new moms on Medicaid.
Women whove just given birth in Texas currently can receive health care services through Medicaid only for up to 60 days after they have the baby. Starting Sept. 1, new mothers will get a full six months of coverage before being removed from the program.
The Maternal Mortality and Morbidity Task Force and Department of State Health Services have been combing through maternal death data for years to come up with solutions on how to reduce deaths in Texas. Several years ago, they recommended Medicaid coverage be extended up to a year after a woman gives birth.
According to their report from July 2016, extending coverage for up to a year would “improve continuity of care, promote safe birth spacing, and reduce maternal morbidity,” which includes near-death experiences or serious health complications that arise during a pregnancy.
Members of the state health agency and task force also told lawmakers it could save the state money.
After years of failed efforts to extend coverage, lawmakers did manage to passa version of the task forces recommendation this year. But House Bill 133 falls short of what was advised instead of one year of postpartum coverage, lawmakers agreed to extend the coverage to only up to six months.
