Who Is Eligible For Both Medicare And Medicaid
To qualify for Medicare, individuals generally need to be 65 or older or have a qualifying disability. There are several levels of assistance an individual can receive as a dual eligible beneficiary. The term full dual eligible refers to individuals who are enrolled in Medicare and receive full Medicaid benefits.
Medicaid Buy In Program For Working People With Disabilities And Medicare Savings Programs
The Medicaid Buy-In Program for Working People with Disabilities provides Medicaid coverage for people ages 16-64 who have a disability and are engaged in a work activity for which they are paid. In order to be considered for this program, the individual must be determined disabled as defined by the Social Security Administration. The persons net income must be at or below 250% of the federal poverty level.
How Long Does Health Insurance Take To Start
Once youve enrolled and made your first payment it can take about 3 weeks, for your application to be processed. If you applied for major medical health insurance and your enrollment was received in the first fifteen days of the month, your coverage will typically begin on the first day of the following month.
You May Like: How To Get Approved For Medicaid In Florida
Do You Have To Renew Medical Insurance Every Year
Most general insurance policies run for 12 months, though some policies allow policyholders to choose a semi-annual policy if they wish, and others such as travel insurance cover specific dates. Under the terms of some policies, they will automatically renew unless you notify your insurer otherwise.
How Do I Apply For Medicaid

You can apply for Medicaid in any one of the following ways:
- Write, phone, or go to your .
- In New York City, contact the Human Resources Administration by calling 557-1399.
- Pregnant women and children can apply at many clinics, hospitals, and provider offices. Call your local department of social services to find out where you can apply.
> >
Recommended Reading: Amerigroup Medicaid Texas Breast Pump
Apply Through The Dutchess County Department Of Community & Family Services If You Are:
- Age 65 and older
- Enrolled in Medicaid Buy-In for Working People with Disabilities enrollees
- Former foster care youth
- Resident of adult homes and nursing homes
- Resident of treatment center/community residences operated by the Office of Mental Health
- Applying for AIDS Health Insurance Program or Medicaid Cancer Treatment Program
- Applying for Medicare Savings Program
- Your eligibility is based on being blind or disabled or you request coverage for community based long term care services including those individuals with an immediate need for Personal Care Services or Consumer Directed Personal Assistance Services
Is Healthfirst Better Than Fidelis
Fidelis Cares brand is ranked #- in the list of Global Top 1000 Brands, as rated by customers of Fidelis Care. Healthfirsts brand is ranked #- in the list of Global Top 1000 Brands, as rated by customers of Healthfirst. Their current valuation is $5.35M.Fidelis Care vs Healthfirst. 28% Promoters 12% Passive 60% Detractors.
Also Check: Dental Places That Accept Medicaid
How To Renew Medicaid Online
Medicaid is a federally funded, state administered program that provides health care coverage to eligible low-income individuals and families. Each state sets its own rules regarding eligibility requirements. States approve Medicaid based on factors such as income, disability, pregnancy and citizenship status.
Gather all of your documents to show proof of income, identity and citizenship along with social security numbers for each member of your household. You will need these documents to renew your Medicaid benefits.
Go online to your State’s Health and Human Services website. To locate a state-specific Medicaid website, type the name of the state and then type Medicaid into your preferred search engine. In addition, The Centers for Medicare and Medicaid Services provides links to Medicaid program websites by state .
Complete the application in its entirety or save your application by clicking the save button. Log out and return within 30 days to complete and submit your application for renewal. After submitting your application, Medicaid will ask you to mail in documents to prove United States citizenship and income.
Tips
-
Keep a record of your account passwords for future login access or application completion. Print your application summary page to keep for your records, it includes your application number.
References
Unitedhealthcare Connected Benefit Disclaimer
This is not a complete list. The benefit information is a brief summary, not a complete description of benefits. For more information contact the plan or read the Member Handbook. Limitations, copays and restrictions may apply. For more information, call UnitedHealthcare Connected® Member Services or read the UnitedHealthcare Connected® Member Handbook. Benefits, List of Covered Drugs, pharmacy and provider networks and/or copayments may change from time to time throughout the year and on January 1 of each year.
You can get this document for free in other formats, such as large print, braille, or audio. Call , TTY 711, 8 a.m. – 8 p.m., local time, Monday – Friday . The call is free.
You can call Member Services and ask us to make a note in our system that you would like materials in Spanish, large print, braille, or audio now and in the future.
Language Line is available for all in-network providers.
Puede obtener este documento de forma gratuita en otros formatos, como letra de imprenta grande, braille o audio. Llame al , TTY 711, de 08:00 a. m. a 08:00 p. m., hora local, de lunes a viernes correo de voz disponible las 24 horas del día,/los 7 días de la semana). La llamada es gratuita.
Puede llamar a Servicios para Miembros y pedirnos que registremos en nuestro sistema que le gustaría recibir documentos en español, en letra de imprenta grande, braille o audio, ahora y en el futuro.
Los servicios Language Line están disponibles para todos los proveedores dentro de la red.
Don’t Miss: How To Apply For Medicaid In Houston
How Do I Renew My Medicaid
Look out for a renewal packet in the mail. The packet may come about 60 days prior to your renewal date from the New York State Department of Health, Human Resources Administration , or Local Department of Social Services , depending on how you signed up. It is important to note the date when you have to submit the renewalthis can be found in the packet along with a renewal form and instructions on how to renew.
Answer all questions in the renewal form as completely and accurately as you can. Once the form is completed, you can return it in the postmarked envelope that came in the renewal packet, or have a social worker submit it on your behalf. Important information such as the web address, phone number and address where you can send your application will also be listed in the packet.
Since receiving the renewal packet is key, you need to make sure that your address on record at the Medicaid office is always updated. Notify them right away of any changes in residence or other information such as change in your legal name, DOB , and/or phone number.
Where Is Healthfirst Accepted
Your insurance is accepted at the following hospitals: NYC Health + Hospitals/Bellevue. NYC Health + Hospitals/Coney Island. NYC Health + Hospitals/Elmhurst. NYC Health + Hospitals/Harlem. NYC Health + Hospitals/Jacobi. NYC Health + Hospitals/Kings County. NYC Health + Hospitals/Lincoln. NYC Health + Hospitals/Metropolitan.
Also Check: What Is The Difference Between Medicare & Medicaid
No Existing Medicaid Coverage
If you dont already have Medicaid coverage, and you meet the above conditions, you may ask to have your Medicaid application processed more quickly by sending in a completed Access New York Health Insurance Application and the Access New York Supplement. If needed, you will also need to provide a physicians order for services and a signed Attestation of Immediate Need
.
American Disabilities Act Notice
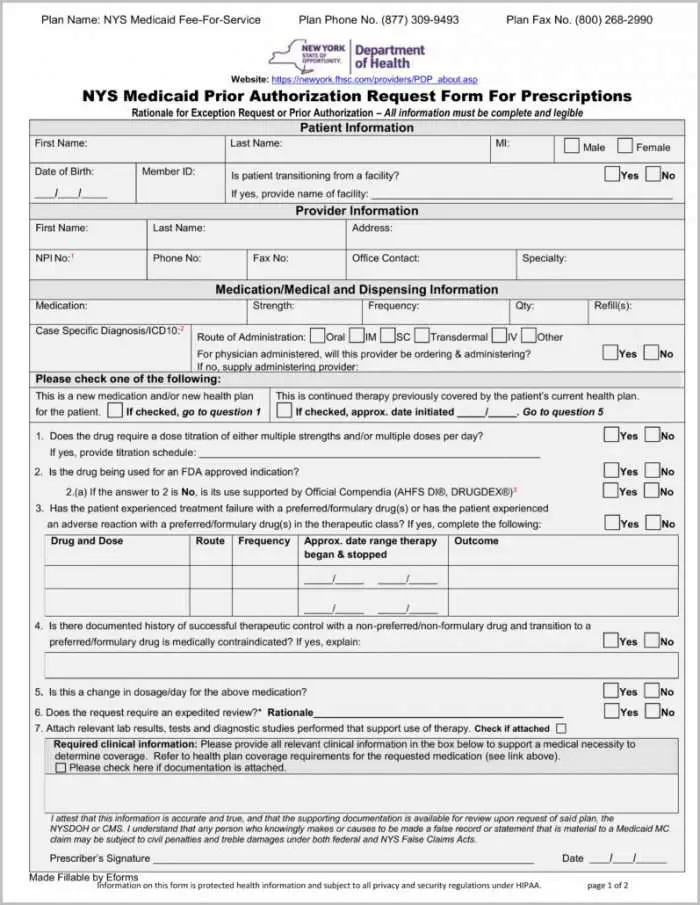

In accordance with the requirements of the federal Americans with Disabilities Act of 1990 and Section 504 of the Rehabilitation Act of 1973 , UnitedHealthcare Insurance Company provides full and equal access to covered services and does not discriminate against qualified individuals with disabilities on the basis of disability in its services, programs, or activities.
Read Also: Medicaid Primary Care Physicians Arkansas
When Can I Renew My Ny Medicaid
Renewing through the NY State of Health Marketplace Pay close attention to the date on your letter you must renew by that date in order to keep your coverage. You can typically renew 30 days from the date you receive your letter. If you dont understand your letter or if you need help, call us at 1-888-432-8026.
How To Send Your Renewal Packet To Hra:
Make two complete copies of the signed renewal form and all attachments.
Mail the original renewal packet and all required documents to HRA in the barcoded gray envelope you received in the mail. If you downloaded the form and you do not have the return bar-coded envelope, then mail it to the address below.
Mail another complete copy of the renewal packet and all attachments in a separate envelope to the same address via certified mail return receipt requested so you have proof you sent it and when it was received. Save the return receipt.
PLEASE MAIL YOUR RENEWAL TO:
After you send your renewal packet, you can 1-888-692-6116 to check the status of your renewal. Have your Medicaid case number available, which can be found on the top right corner of your renewal form. Be advised it may take some time for the renewal packet to be received and processed.
You May Like: Does Missouri Medicaid Cover Assisted Living
Renew Your Coverage With Mvp
Automatic Renewal During COVID-19 Crisis
Medicaid, Child Health Plus, and Essential Plan members that are due for renewal during the COVID-19 emergency will be automatically renewed for a four-month period.
Questions? Call Member Services/Customer Care at1-800-852-7826
Renewing your coverage is easy:
1. Click below to find the information that you need to renew:
-
Child Health Plus
To renew, you will need to provide:
- Social Security Number or Document Numbers for you and your child
- Dates of birth for you and your child
- Employer and income information
- Information about any additional insurance available
- Your email address
Medicaid Managed Care
To renew, you will need to provide the following information for each person in your household:
Essential Plans
Does Health Insurance Automatically Renew
You can choose to renew your health insurance or not In many cases, you dont need to do anything your health insurance will renew automatically. However, your plan may vary, so check with your insurance company for details. They might be able to help you find a different plan that works better for you.
Don’t Miss: Does Medicaid Cover Gastric Bypass In Michigan
How To Fill Outthe Renewal Form
WRITE in big, clear letters on top of the form and in any white space if you get any special type of Medicaid budgeting — such as Spousal Impoverishment, Spousal Refusal, MBI-WPD, Pooled Trust, MAGI-like, DAC, Pickle, or Special MLTC Housing Standard. Also write in if you want the Medicare Savings Program as well as Medicaid. For info about these special Medicaid budgeting rules, see this article
Include all household members and their information. This includes your spouse if your spouse lives with you, and any minor dependent children under age 18 or under 19 if in school who live with you. Do not list your adult children, your siblings, or other roommates.
Make any changes, if applicable, to the amount of your rent, your insurance premiums, your income, and your resources.
If you have a Pooled Income Trust, be sure to check the box saying you are enclosing a Verification of Deposits and obtain this document from your Pooled Trust organization reflecting all deposits you have made for the last year. Many Pooled Trusts now make this document available online for download.
Consumers Must Enroll Or Renew By December 15 For Coverage Effective January 1
ALBANY, N.Y. – NY State of Health, the state’s official health plan Marketplace, today announced that beginning November 16, the Marketplace will be open for individuals looking to renew or change their health plan for 2020. Open Enrollment for new customers seeking to enroll in a Qualified Health Plan began November 1 and runs through January 31, 2020. New Yorkers must enroll by December 15 for coverage beginning January 1, 2020.
“The message to all consumers new and returning is to shop now and enroll by December 15,” said NY State of Health Executive Director Donna Frescatore. “New York’s commitment to coverage is unwavering, and we will continue our efforts to provide New Yorkers with the quality, affordable health coverage they deserve.”
Renewal notices have been sent to nearly 500,000 households with current Marketplace coverage with information about their 2020 eligibility, health plan options and costs. These notices inform consumers of what actions, if any, they need to take to renew their coverage for 2020.Since the start of the 2020 Open Enrollment Period on November 1, the Customer Service Center has received over 177,000 calls, and more than 334,000 people have visited the NY State of Health website.
Consumers can enroll in, renew or change, a health plan by:
- Logging onto the website at nystateofhealth.ny.gov
- Meeting with an in-person assistor. Find an assistor here:
You May Like: Dentist In Meridian Ms That Accept Medicaid
Keep Track Of Your Medicaid Authorization Period So You Know When To Expect Your Medicaid Renewal
You can find the starting month of your authorization period on your Medicaid acceptance letter. The starting month listed in the acceptance letter will be EARLIER than the date of the notice at the top of the acceptance letter. The attached sampleNotice of Decision on Your Medical Assistance is dated July 31, 2019, and the starting month of the Medicaid authorization is July 1, 2019 . The renewal in that case would be sent between January March 2019.
If you are enrolled in an MLTC plan, your MLTC plan will probably notify you of an upcoming renewal shortly before HRA mails you the renewal packet.
If you receive your renewal packet in the mail, dont throw out the enclosed gray return envelope. As explained below, you will send back the completed renewal packet in the gray envelope.
Renewing Through The Ny State Of Health Marketplace
You need to renew your Medicaid coverage every year. You can call us at 1-888-432-8026, Monday through Friday, from 8:30 am to 6:00 pm and Saturday 9:00 am to 1:00 pm or visit an enrollment site near you.
The NY State of Health Marketplace will send you a letter or an email with your renewal date for you to call and renew without losing any coverage. Pay close attention to the date on your letter you must renew by that date in order to keep your coverage. You can typically renew 30 days from the date you receive your letter. If you dont understand your letter or if you need help, call us at 1-888-432-8026.
Any information provided on this Website is for informational purposes only. It is not medical advice and should not be substituted for regular consultation with your health care provider. If you have any concerns about your health, please contact your health care provider’s office.
Also, this information is not intended to imply that services or treatments described in the information are covered benefits under your plan. Please refer to your Membership Agreement, Certificate of Coverage, Benefit Summary, or other plan documents for specific information about your benefits coverage.
Back to Top
Don’t Miss: The Phone Number For Medicaid
What Happens If My Medicaid Application Is Not Completed
If a Medicaid beneficiary does not complete the redetermination process in time, Medicaid benefits will cease and there will be a lack of coverage. However, under federal law, the individual has 90 days from the date in which the case was closed to provide the Medicaid agency with all of the required information.
Immediate Need For Personal Care Services / Consumer Directed Personal Assistance Services
If you think you have an immediate need for Personal Care Services or Consumer Directed Personal Assistance Services , such as housekeeping, meal preparation, bathing, or toileting, your eligibility for these services may be processed more quickly if you meet the following conditions:
- You are not receiving needed help from a home care services agency
- You have no adaptive or specialized equipment or supplies in use to meet your needs
- You have no informal caregivers available, able and willing to provide or continue to provide care
- You have no third party insurance or Medicare benefits available to pay for needed help
Read Also: Blue Choice Healthy Connections Medicaid
Renew Your Medicaid Benefits
Medicaid benefits must be renewed at least once every 12 months.
Eligible Medicaid members will receive a notice, online or by mail, the month before their renewal month. You must submit a renewal by the end of the renewal month or your coverage may be terminated. You can submit a renewal within 90 days after termination to have coverage reinstated back to the first of the month following termination.
Changes to your personal situation for example, if you get a different job, if your family size changes, or if you move may affect your eligibility for Medicaid. If that happens, a case worker must review your eligibility.
