Is Iowa Total Care Medicare
If I have both Medicare and Medicaid, will I have to change my Medicare plan as part of Iowa Total Care ? No. Your Medicare services and doctors will stay the same. Its the responsibility of your Medicaid MCO to make sure that they coordinate your services with your Medicare Primary Care Provider .
Federal Poverty Level Guidelines Chart
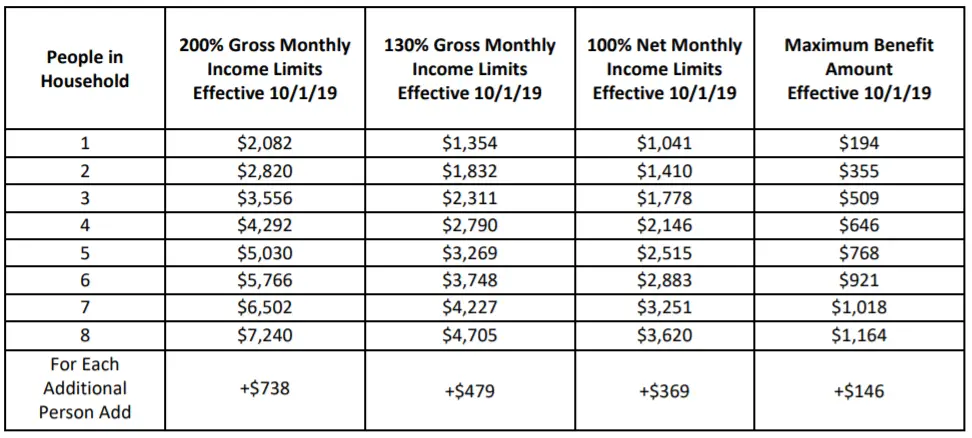
Use the chart below to see if you meet income requirements. First, youll need to find the row with number of people in your household. Then, use the program requirements to find the column with program eligibility percent. If your household income is under that amount, you may qualify for services. For example, if you have a household size of 4, and the program eligibility is 200% of the Federal Poverty Level, then you may qualify for the program if your household income is under $53,000.
Iowa Medicaid Expansion Update
Iowa initially expanded Medicaid with a privatized approach but switched to straight Medicaid expansion as of 2016.
The state used a waiver to implement an Iowa-specific version of Medicaid expansion.
However, in 2015, that plan was abandoned in favor of straight Medicaid expansion as called for in the ACA.
The state uses a managed care approach that utilizes private insurers to provide coverage and care coordination.
The state has seen a 42% reduction in the uninsured population from 2013 to 2017.
You May Like: Is Wisdom Teeth Removal Covered By Medicaid
Medicaid Eligibility Expansion In Iowa With A Waiver
The federal government laid out very specific parameters for Medicaid expansion under the ACA. But states have the option of seeking a waiver from CMS in order to implement unique approaches to Medicaid expansion, and still receive federal funding to do so.
In December 2013, Iowa received a waiver for its alternative to the ACAs Medicaid expansion. Under a program called the Iowa Health and Wellness Plan , very low-income residents would be enrolled in a state-run health plan and, in some cases, be required to pay modest premiums. Other residents with slightly higher incomes would purchase insurance through the marketplace via a program called the Iowa Marketplace Choice Plan , with premiums paid by the federal government.
The federal government approved two waiver amendments in December 2014. One allowed Iowa to continue not providing non-emergency transportation. The other allowed Iowa to continue charging a monthly premium for beneficiaries with income under 138% FPL. Beneficiaries could reduce or eliminate the premium if they completed a wellness exam and health risk assessment.
The Iowa Health and Wellness Plan launched Jan. 1, 2014, and about 120,000 people were enrolled as of late December 2014 . But problems began to crop up early on.
Transition In Iowa To Medicaid Managed Care In 2016 And Subsequent Shifts In Insurer Participation

Iowa opted to switch the entire Medicaid program to managed care, intending to make the switch as of January 1, 2016. The federal government determined in December 2015 that Iowa needed additional time to make the transition to Medicaid managed care, and the new system, dubbed Iowa Health Link, took effect April 1, 2016. Patients and providers reported a fairly rocky switch to the privatized Medicaid system.
Democrats in the Iowa Senate tried to halt the switch to managed care, and passed Senate File 2125 in February 2016, which would have terminated the managed care contracts and instructed the existing Medicaid fee-for-service program to focus on improving patient outcomes and access to care, and increasing efficiency .
There were initially three insurers offering Medicaid managed care through Iowa Health Link: Amerigroup, AmeriHealth Caritas, and UnitedHealthcare. But Iowa and AmeriHealth Caritas were unable to agree on the terms of a contract renewal in late 2017, and AmeriHealth Caritas withdrew from Iowa Health Link at the end of November, 2017, when their contract ended. And around the same time, Amerigroup informed the state that they did not have the capacity to accept new members.
You May Like: Does Medicaid Pay For Dentures In Nc
Medicaid Payment For Nursing Home Care
Many people rely on Medicaid, also known as Title 19, to pay for their nursing home care or in-home services under the Medicaid Elderly Waiver program. Medicaid is a needs-based program for people who cannot afford the care they need. The financial eligibility rules for nursing home Medicaid and the Elderly Waiver are the same. In general, people are financially eligible for Medicaid for nursing home care if their income in 2021 is $2,382 or less per month and their nonexempt resources are $2,000 or less. In some instances, people with incomes above $2,382 per month may be eligible for Medicaid if they can establish a medical assistance income trust, also known as a Miller Trust. All non-exempt resources count toward the $2,000 limit. Exempt resources that do not affect your eligibility include a car, homestead, household goods, and prepaid funeral plans.
Medicaid eligibility is much more complicated for married people. The Medicaid program allowsthe spouse who lives outside of the nursing home to have more than $2,000 in resources withoutdisqualifying the spouse who lives in the nursing home from receiving Medicaid. The community spouses income does not count toward the $2,382 income limit. In addition, if the community spouses monthly income is less than $3,260 then part or nearly all the income from the spouse in the nursing home may be kept by the community spouse.
Meeting Program Income Requirements
In order to receive help from many services offered by community action, you have to meet income requirements, based on the Federal Poverty Level. The requirement level for each program may be different. Look at the chart below to get an idea of what your income eligibility may be. Your local Community Action Agency will work with you to determine your eligibility for various programs and services. Find your local agency.
Don’t Miss: Who Gets Medicaid In Florida
Who Can Get Medicaid In Iowa
You should apply for Medicaid if your income is low and you match one of the descriptions below:
- You think you are pregnant
- The parent or caretaker of a child and/or teenager under the age of 19.
- You are a child or teenager age 18 or under.
- An adult age 65 or older.
- You are legally blind.
- Living with a disability or disabled.
- You are in need of nursing home care.
How To Apply / Learn More
This waiver is available statewide in all Iowa counties. Waivers are not considered entitlement programs. This means that it is possible to be fully qualified and still be wait listed for services. This waiver has been improved to service a maximum of approximately 10,459 in 2020 and no more than 7,850 concurrently. That said, as of last check, there was no waiting list.
To apply, one should contact his/her Iowa Department of Human Services county office. A detailed, although slightly dated description of benefits is available here. Persons can also call 800-338-8366 to reach Iowa Medicaid Member Services for assistance.
Read Also: Dentist In Lafayette That Accept Medicaid
Iowa Medicaid Income Limit Charts
The Iowa Medicaid eligibility income limit charts are divided by groups.
For example, the first chart is focused on income limits for children who qualify for Medicaid.
Similarly, the second chart below focuses on the Medicaid income limits for adults in Iowa who qualify for Medicaid.
Iowa Medicaid Income Limit for Children
Below is the income limit for children by age category. Find the age category your child falls into and you will see the income limit by household size.
| Iowa Medicaid Income Limit Children |
| Children Medicaid Ages 0-1 |
| $59,398 |
How to Read the Iowa Medicaid Income Limits Charts Above
You cannot have an income higher than the Federal Poverty Level percentage described for your group to be eligible for Medicaid.
Similarly, when you identify the income group that applies to you, the income limit you see refers to the maximum level of income you can earn to qualify for benefits.
For example, if you are pregnant, to qualify for Medicaid, you cannot have an income higher than 375% of the Federal Poverty Level which for a family of two is $65,325 as shown in the chart above.
Iowa Medicaid Asset Limits 2019
Individuals in Iowa are allowed to keep $2,000 when they apply to Medicaid for long term care. If they are over this amount, they must spend down on care. It is important to note, that individuals are not allowed to give gifts of any amount for a period of 5 years prior to applying to Medicaid. If an individual’s assets are more than $2,000, they should learn about Medicaid Planning strategies. This asset limit only applies to assets that are considered countable assets. Some examples of countable assets include savings accounts, bank accounts, retirement accounts and a second home. If you have multiple assets and are looking to access Medicaid, it may make sense to speak with a Medicaid Planner or Elder Law attorney in Iowa.
Couples that both require Medicaid for long term care in Iowa are allowed to keep $3,000 in assets. If there is one spouse that requires care, and one that does not, the spouse that does not receive care is referred to as the Community Spouse. The Community spouse is allowed to keep 50% of their assets up to $123,600 in countable assets which is known as the Community Spouse Resource Allowance. The Community Spouse is allowed to keep 100% of their marital assets up to $24,720 .
Also Check: How To Obtain Medicaid In Florida
Apply For Medicaid In Iowa
Apply online via the Iowa DHS site or HealthCare.gov. Print an application in English or Spanish and mail it to Imaging Center 4 PO Box 2027 Cedar Rapids, Iowa 52406. Call 1-855-889-7985 to get help with your application.
Eligibility: Children up to age 1 with family income up to 375% of FPL. Children ages 1 to 18 with family income up to 167% of FPL children with family income up to 302% of FPL may qualify for the hawk-i program. Pregnant women with family income up to 375% of FPL. Adults with family income up to 138% of FPL.
How Do I Apply For Medicaid For My Child
In Iowa, Medicaid funding is administered by managed care organizations however the Department of Human Services determines eligibility and manages applications. You can apply for any program for your child by visiting your local DHS office. You can find the nearest office by visiting the DHS website.
If you have any questions while you are completing the Medicaid application, you can call the DHS Help Center at .
You May Like: What Is The Difference Between Medicare & Medicaid
Does Iowa Help With My Medicare Premiums
Many Medicare beneficiaries who struggle to afford the cost of Medicare coverage are eligible for help through a Medicare Savings Program . This program pays for Medicare Part B premiums, Medicare Part A and B cost-sharing, and in some cases Part A premiums.
- Qualified Medicare Beneficiary : QMB pays for Part A and B cost sharing as well as Part B premiums. QMB will also pay Part A premiums if a beneficiary owes them. The income limits for QMB are $1,083 a month if single or $1,457 a month if married.
- Specified Low-income Medicare Beneficiary : SLMB pays for Part B premiums. The income limit for SLMB is up to $1,296 a month if single or $1,744 a month if married.
- Expanded Specified Low-income Medicare Beneficiary : E-SLMB pays for Part B premiums for beneficiaries with income up to $1,456 a month if single or $1,960 a month if married.
- Qualified Disabled Working Persons : QDWP pays Part A premiums owed by certain disabled beneficiaries who have returned to work. Few beneficiaries enroll in QDWP due to other Medicaid benefits available to disabled workers. The income limit is $2,126 a month if living alone and $2,873 a month if living with one other person.
MSP asset limits: Iowa uses the federal asset limits for QMB, SLMB and QI: $7,860 if single and $11,800 if married. The QDWI asset limit is $4,000 if single and $6,000 if living with others.
Medicaid Eligibility Program Overview
Medicaid pays for the cost of Nursing Home care in Iowa that meet certain financial and health criteria. The average cost of Skilled Nursing Care in Iowa is $66,432, so securing Medicaid coverage is essential. In Iowa there are 451 Nursing Homes, of which 99% accept Medicaid insurance as a form of payment. The most expensive Nursing Home in Iowa is Mercy Living Center South which costs $685 per day and the least expensive Nursing Home is Newton Health Care Center which costs $108 per day. Nursing Homes in Iowa are currenlty 78.03% full with 23,960 patients currently using the 30,708 beds available.
To learn about the entire Medicaid eligibilty process, we have put together a comprehensive medicaid nursing home guide which you can read here.
Also Check: Dermatologist In Lake Charles That Accept Medicaid
How Do You Apply For Medicaid In Iowa
Apply online via the Iowa DHS site or HealthCare.gov. Print an application in English or Spanish and mail it to Imaging Center 4 PO Box 2027 Cedar Rapids, Iowa 52406. Call 1-855-889-7985 to get help with your application . Eligibility : Children up to age 1 with family income up to 375% of FPL.
How Does Iowa Regulate Long
Long-term care is an increasingly needed benefit in the U.S. given the aging population, but it is generally not covered under Medicare. However, Medicaid does cover long-term services and supports for people who meet eligibility requirements.
Medicaid nursing home coverage
Most seniors who needed long-term care used to receive it in nursing homes. Today, more enrollees receive long-term care at home. But medical conditions or living situations can make nursing home care a better choice.
Income limits: The income limit is $2,349 a month if single and $4,698 a month if married . Only income of the spouse who needs nursing home benefits is counted toward this limit.
Nursing home enrollees are required to pay most of this allowed income to their nursing home, but may keep money to pay for health insurance premiums, such as Medicare Part B, Medicare Advantage and Medigap).
Assets limits: The asset limit is $2,000 if single and $3,000 if married . If only one spouse has Medicaid, federal rules allow the other to keep up to $128,640. Certain assets are never counted toward this asset limit, including many household effects, family heirlooms, certain prepaid burial arrangements, and one car.
Home and Community Based Waiver services
Income limits: The income limit is $2,349 a month if single and $4,798 a month if married . When only one spouse needs HCBS, only income received by that spouse is counted toward this limit.
Spousal impoverishment protections in Iowa
You May Like: Kids Dentist That Take Medicaid
What Is Federal Poverty Level Income
2020 Federal Poverty Guidelines Chart The HHS Department issues poverty guidelines for each household size. For example, the poverty level for a household of four in 2020 is an annual income of $26,200. To get the poverty level for larger families, add $4,480 for each additional person in the household.
Children At Home Program
The Children at Home Program is a program that can help you and your family receive services and supports you think are necessary in helping your child remain at home. It also can help you receive the services and supports that are not available in other programs.
Eligibility for the Children at Home Program is for families who meet all of the following conditions:
- The family resides in Iowa
- The family includes an individual with a disability, which is defined as an individual who is less than 22 years of age and meets the definition of a developmental disability
- The family expresses an intent for the individual with a disability to remain living in the familys home
- The familys net taxable income is the most recently completed tax year is less than $60,000
If you have any questions about this program or want to apply for assistance, please contact the Iowa Family Support Network.
You May Like: Does Medicaid Pay For Prescription Glasses
Arizona Medicaid Income Limits Summary
We hope this post on Arizona Medicaid Income Limits was helpful to you.
If you have any questions about Medicaid in the state of Arizona, you can ask us in the comments section below.
Help us spread the word! If you found this post on Arizona Medicaid Income Limits helpful, help us spread the word by sharing it using the Share this button below.
Be sure to check out our other articles about Medicaid.
Medicaid Eligibility Expansion In Iowa Without A Waiver But With Managed Care
In July 2015, Iowa officials announced that they were abandoning their Medicaid demonstration waiver, and would instead implement Medicaid expansion as called for in the ACA, but with a Medicaid Modernization managed care waiver instead, switching Iowa Medicaid enrollees to a Medicaid managed care system .
560,000 Iowa Medicaid beneficiaries were scheduled to transition to the Medicaid managed care system as of January 1, 2016. The Medicaid enrollees were supposed to select a managed care program by mid-December, but many enrollees were having trouble determining which managed care programs included their doctors and hospitals. As a result, the federal government delayed Iowas switch to Medicaid managed care until March 1, 2016. The federal government ultimately gave the go-ahead for the switch on February 23, but added an extra month to allow enrollees, MCO carriers, and providers time to make the change. The Medicaid managed care system in Iowa took effect April 1, 2016.
Eligibility for coverage under Iowas Medicaid expansion was unchanged Medicaid coverage continued to be available to Iowa residents with household income up to 138% of the poverty level. But enrollees with incomes between 101% and 138% of the poverty level were no longer enrolled in private exchange plans as of 2016. Instead, they are enrolled in a private Medicaid managed care program, just like the rest of the Medicaid population in Iowa.
You May Like: Family Of Three Income For Medicaid
