How Much Does Magi Medicaid Cost
Medicaid provides free health insurance to individuals who qualify based on income and family size. If you qualify for MAGI Medicaid, you may be required to enroll into a managed care plan to receive your medical services. Some services may be subject to co-payments, these co-payments can be as little as 50 cents . The maximum you will pay out of pocket for the year cannot exceed $200.
Magi Medicaid For Adults Children & Families
What does MAGI mean?
- MAGI stands for Modified Adjusted Gross Income
- MAGI-based budgeting is used to calculate a person’s household size and income, using federal income tax rules and a tax filer’s family size to determine eligibility for Medicaid
- The MAGI Medicaid program started January 1, 2014, as part of the Affordable Care Act
Who is potentially eligible for MAGI Medicaid?
- Single, childless adults
- Families with children ages 19 and under
- Children up to age 19
What are the income guidelines?
It depends. There are different categories of MAGI Medicaid. All guidelines are based on gross income:
- Parents and Caretaker Relatives : up to 90% of the federal poverty level for their household size
- Expansion Adults : up to 133% of the federal poverty level for their household size
- Children with Insurance: up to 156% of the federal poverty level for their household size
- Pregnant Women: up to 200% of the federal poverty level for their household size
- Children without Insurance: up to 206% of the federal poverty level for their household size
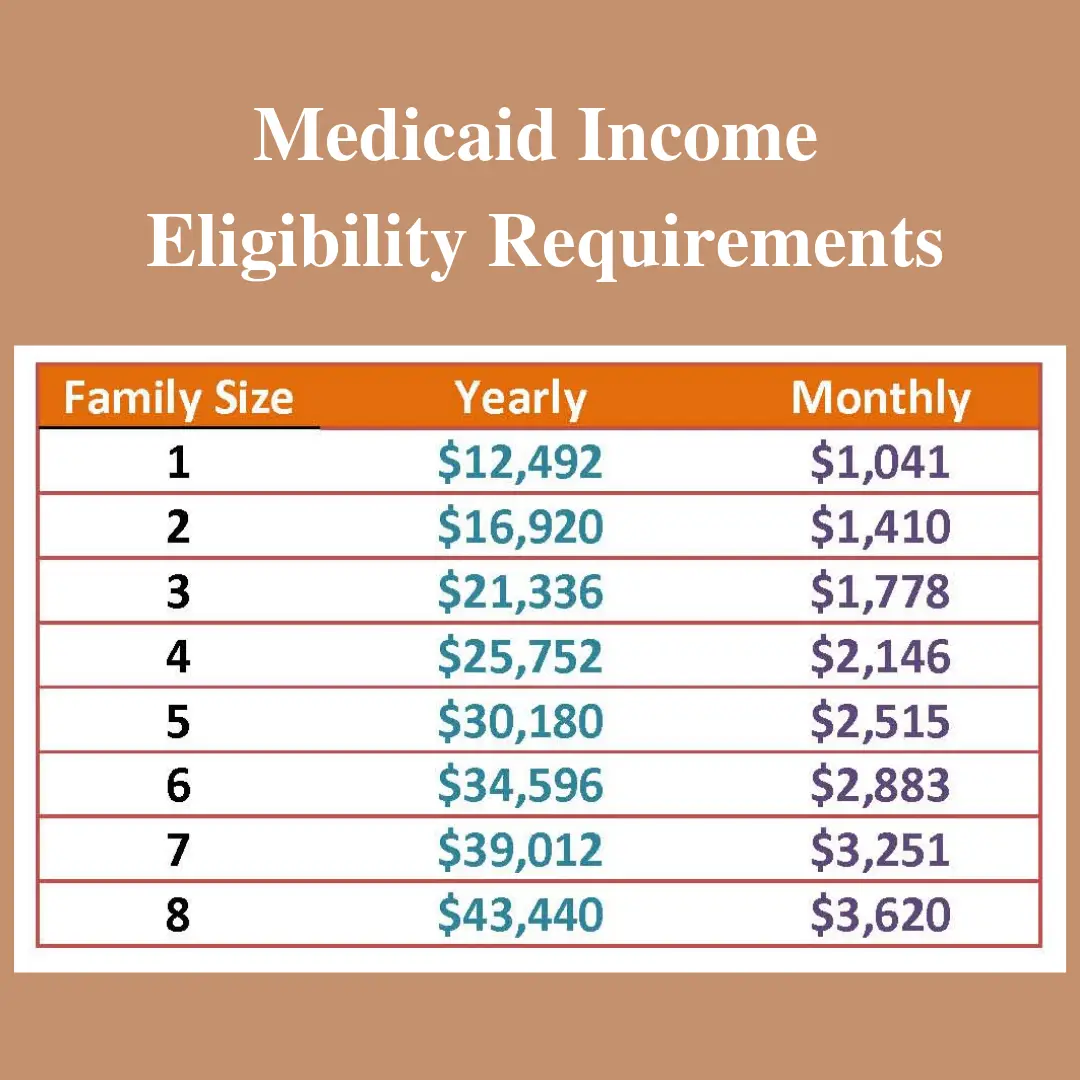
Below is a chart showing the 2021 standards for MAGI Medicaid eligibility:
Medicaid HH Size
Taking Advantage Of Magi
The Affordable Care Act simplified Medicare eligibility and enrollment for millions of Americans. Using MAGI for eligibility simplified the application process. The administrative burden of confirming assets was put to the wayside. Unfortunately, it also gave wealthy people the opportunity to take advantage of taxpayer dollars.
This loophole occurs because the majority of Americans now qualify for Medicaid through MAGI, which unless you are seeking long-term nursing home care no longer uses the asset test. People who are asset rich, particularly those who have investments or real estate properties, can still technically meet MAGI criteria.
Someone could own a home worth $850,000, a Lamborghini, a second vehicle, hundreds of acres of farmland, and still technically be eligible for Medicaid.
These Americans would be considered wealthy by any standards but by sheltering their net worth under the current tax laws, they would be legally eligible for Medicaid or subsidized plans through the Health Insurance Marketplace. This is the case even when they could easily dip into their assets to pay for health insurance.
If the intent is to provide health care to the most financially needy, MAGI Medicaid may need to consider how it addresses this loophole. The GOP is currently looking to repeal Obamacare which would, in effect, put an end to MAGI Medicaid altogether.
You May Like: How To Apply For Medicaid In Florida Online
How Do I Invalidate Modified Adjusted Gross Income N01 Or N02 In Acesonline
When it has been discovered that an individual was opened on a N01 or N02 Assistance Unit in error for a particular month take the following steps:
The page refreshes and displays the updated checkbox and the medical coverage group is invalidated for the given month.
Note:
If it is discovered the invalidation was done in error workers can go back to the AU’s Demographics page and remove the checkmark next to the Exclude from N01/N02 Determination for any given month.
Workers must go back into Healthplanfinder to invoke an eligibility call to the Eligibility Service.
The Magi Population Groups
The MAGI population groups include the following:
- Pregnant women
- Dependent children under the age of 19
- Parents/caretaker relatives of children under 19
- Applicants 65 and over, as well as applicants with Medicare, are typically budgeted as non-MAGI.
- However, if such an applicant is a parent/caretaker relative with children under 19, they may choose to be classified as MAGI and MAGI budgeting rules and application and renewal procedures would apply.
Recommended Reading: How Much Money Disqualifies You For Medicaid
Modified Adjusted Gross Income
Your modified adjusted gross income is your AGI with excluded foreign income, non-taxable portions of your Social Security income, and tax-exempt interest.
Essentially, this adds back certain deductions from the AGI. For most people, the AGI and MAGI will be the same.
When it comes to Medicaid eligibility, however, MAGI has two components. The first is your household income, and the second is the size of your household.
If you are on your own, in a family of two, or in a family of five, you will have different qualifying MAGI levels to become eligible for these programs. Each state will have different MAGI levels too, depending on whether or not they enacted Medicaid expansion.
Qualifying For Magi Medicaid
MAGI is the new methodology for determining household composition, household size, as well as how income is counted to evaluate eligibility for MAGI Medicaid. The MAGI methodology basically follows the same rules as when a household files their federal income taxes and is based on the adjusted gross income that a filing unit reports on their federal income tax return with certain modifications, thus modified adjusted gross income MAGI. Income thresholds were expanded up to a minimum of 138% of the federal poverty levels for the MAGI Medicaid population, and could be higher depending on the applicant. In addition, the asset test was eliminated under the ACA for the MAGI groups. And immigration criteria follow the federal Medicaid immigration criteria, for the most part. For more information, see below, Qualifying for MAGI Medicaid.
Also Check: How To Apply For A Replacement Medicaid Card
Income Definitions For Marketplace And Medicaid Coverage
Financial eligibility for the premium tax credit, most categories of Medicaid, and the Childrens Health Insurance Program is determined using a tax-based measure of income called modified adjusted gross income . The following Q& A explains what income is included in MAGI.
Note that many guidelines and thresholds are indexed and change each enrollment year. For reference, please see the Yearly Income Guidelines and Thresholds Reference Guide.
How do marketplaces, Medicaid, and CHIP measure a persons income?
For the premium tax credit, most categories of Medicaid eligibility, and CHIP, all marketplaces and state Medicaid and CHIP agencies determine a households income using MAGI. States previous rules for counting income continue to apply to people who qualify for Medicaid based on age or disability or because they are children in foster care.
MAGI is adjusted gross income plus tax-exempt interest, Social Security benefits not included in gross income, and excluded foreign income. Each of these items has a specific tax definition in most cases they can be located on an individuals tax return .
| FIGURE 1:Formula for Calculating Modified Adjusted Gross Income |
What is adjusted gross income?
What types of income count towards MAGI?
All income is taxable unless its specifically exempted by law. Income does not only refer to cash wages. It can come in the form of money, property, or services that a person receives.
Does MAGI count any income sources that are not taxed?
Alien Emergency Medical Programs
AEM is for individuals who have a qualifying medical emergency and do not qualify for any other Apple Health program due to citizenship/immigration requirements. This includes qualified aliens who have not met the 5-year and are not exempt from the 5-year bar, nonpregnant nonqualified aliens, and undocumented individuals.
To qualify for AEM, an individual must have or need at least one of the following:
- A qualifying emergent medical condition such as emergency room care, inpatient admission, or outpatient surgery
- A cancer treatment plan
- Antirejection medication for a postorgan transplant or on long-term care services *
- Assessment and treatment for the COVID-19 virus**
Income qualifications are determined by the eligibility requirements and income listed below:
Modified Adjusted Gross Income Medicaid, Processed by the Washington State Health Care Authority
- Individual is age 19 through 64
- Individual is not eligible for Medicare and
- Follows MAGI rules established through the Healthplanfinder.
| Total number |
|---|
Also Check: Dentist In Tyler Tx That Accept Medicaid
What Happens When Changes Are Reported In Washington Healthplanfinder
When changes are reported by an individual in Washington Healthplanfinder for a Modified Adjusted Gross Income Assistance Unit , and there is a related Cash, Classic Medicaid, or Basic Food AU in ACES, the system takes the appropriate action on the related AU which could include:
- Overlaying some of the ACES data with the Healthplanfinder data.
- Displaying some of the MAGI data in ACES.online for comparison against existing ACES data.
- Generating a Barcode Tickle.
- Invoking a call to the Eligibility Service for a benefit recalculation.
NOTE:
Complete And Submit An Application
Self-service application options:
Online: Log on to Georgia Gateway at to apply for benefits. Available 24/7.
Call the Customer Contact Center at to submit an application by telephone.
An application is considered filed when it has the name of the head of household, address, date and signature of the head of household or another household member and is received by DFCS.
Notice of Free Interpretation ServicesIf you have difficulty communicating with us because you do not speak English or have a disability, please notify a staff person. Free interpretation services, translated materials or other assistance is available upon request.
For additional support with requesting large print versions of DFCS applications, please visit .
DFCS Reasonable Modifications and Communication Assistance Request Form for Persons with Disabilities
Do you have a disability and need a reasonable modification or communication assistance to access DFCS services? to request a reasonable modification, communication assistance, extra help or to learn more about the rights of customers with disabilities.
Medicaid Benefit Renewal
All benefits recipients are required to undergo periodic review of continued program eligibility. A renewal form and any required accompanying verification can be submitted in Georgia Gateway or by using Form 508 the FOOD STAMP/MEDICAID/TANF Renewal Form.
Read Also: Obgyn In Broward County That Accept Medicaid
Applying For Magi Medicaid
Most MAGI applicants apply online at the NY State of Health Insurance Marketplace. However, there are few exceptions. Local counties and HRA in NYC will continue to handle the following type of cases for MAGI applicants/recipients:
- Medicaid spenddown participants
- Managed Long-Term Care Plan participants
- Assisted living participants
- All Medicaid consumers who need long-term nursing home care, institutional Medicaid
- Adults or children in need of waiver services
- Consumers residing in a congregate care facility.
For more information, see below, Applying for MAGI Medicaid.
Medicaid And The Asset Test
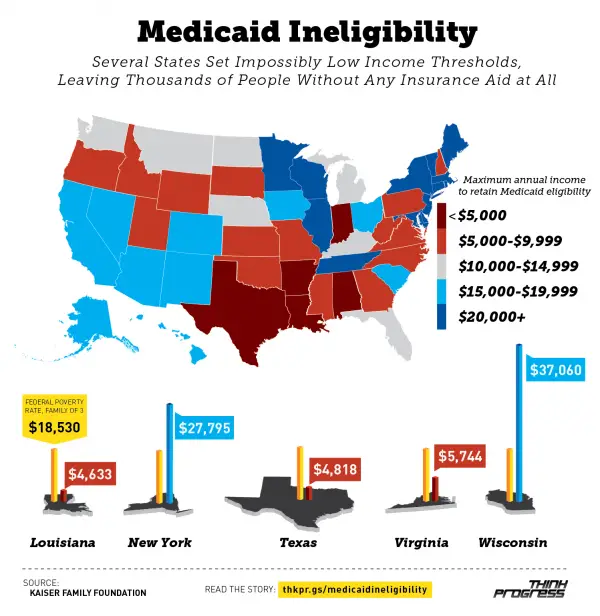
When it comes to non-MAGI Medicaid eligibility, both your income and your assets come into play. Most of the government programs that qualify you for Medicaid use an asset test. SSI sets the standard.
If your income and assets are above a certain level, you will not qualify for the program. In 2021, the income limit is set at $2,382 per month and the asset limits at $2,000 for an individual.
MAGI Medicaid does not cover everything. Your assets come into play when it comes to Long-Term Services and Supports , the part of Medicaid that pays for long-term care in a nursing home.
Not everything you own will count toward your assets. If you have too many assets, you will need to spend down before you will be eligible for Medicaid. How you spend down, however, is important, because you can be penalized for high-value gifts or transfers made within the past 60 months , aka the Medicaid look-back period.
Recommended Reading: Will Medicaid Pay For Cremation
How Do I Invalidate Continuous Eligibility Tracking For Children’s Washington Apple Health Modified Adjusted Gross Income In Acesonline
When it has been discovered that the CTCN period for Children’s WAH has been opened in error take the following steps:
Note:
Workers must go back into Healthplanfinder to invoke an eligibility call to the Eligibility Service.
How Do I Flag An Individual To Identify That They Have Incorrectly Attested To Their Income Citizenship Or Immigration Status
When an individual has been found to have incorrectly attested to their income, citizenship or immigration status, workers with Unit Type 76 can update the Prevent WAH/MAGI Approval flag in ACES.online by taking the following steps:
On the Welcome back page, complete the following fields in the Quick Navigation section:
- Select a Type of ID drop down box – Select Client.
- Enter an ID field – Enter the .
- Select a Page drop down box – Select Demographics.
- Click the Go button and the Summary page displays.
Note:Yes
See ACES Screens and Online pagesfor an example of pages or screens used in this chapter.
Read Also: If You Are On Disability Are You Eligible For Medicaid
Canceling Medicaid Managed Care
What Is Modified Adjusted Gross Income Based Medical
MAGI-based medical refers to Medicaid and Children’s Health Insurance Premium coverage for individuals who are relatable to Medicaid/CHIP if they are:
- A child under age of 19,
- A custodial parent/caretaker, or
- An eligible adult between ages 19 and 65 whose income is below the Federal Poverty Level threshold for the program using the MAGI income methodology.
Also Check: Job And Family Services Ohio Medicaid
Canceling Classic Medicaid Coverage
Note On Incarcerated Beneficiaries
Medicaid suspends the eligibility of Medicaid beneficiaries who are incarcerated in Rhode Island. The corrections system must provide basic healthcare for inmates, and Medicaid is responsible for reimbursing costs of acute care hospital stays of 24 hours or more provided off the premises of the corrections facility.
Medicaid coverage that has been suspended due to incarceration must be reinstated promptly upon the persons release.
You May Like: Nassau County Social Services Medicaid
Effective Date Of Coverage
Once an individual is determined eligible for Medicaid, coverage is effective either on the date of application or the first day of the month of application. Benefits also may be covered retroactively for up to three months prior to the month of application, if the individual would have been eligible during that period had he or she applied. Coverage generally stops at the end of the month in which a person no longer meets the requirements for eligibility.
Who Is Responsible For Modified Adjusted Gross Income Medical Assistance Units
MAGI medical AUs belong to the Health Care Authority and are processed in the Washington Healthplanfinder system. They are assigned to the following HCA Community Service Offices :
- 181 – MAGI AUs that belong to Region 1 geographical/zip catchment
- 182 – MAGI AUs that belong to Region 2 geographical/zip catchment
- 183 – MAGI AUs that belong to Region 3 geographical/zip catchment
ACES users are not be able to screen, initiate a review, add a person, reopen or reinstate MAGI AUs.
Any user with inquiry access in ACES or ACES.online is able to see limited data pertaining to MAGI AUs in ACES Mainframe and in ACES.online.
Recommended Reading: Weight Loss Pills Covered By Medicaid