Expansion Under The Affordable Care Act
The Affordable Care Act provided for the expansion of Medicaid to cover childless adults whose income is 138 percent of the federal poverty level or below. The provision for expanding Medicaid went into effect nationwide in 2014. As of November 2018, a total of 36 states and Washington, D.C., had expanded or voted to expand Medicaid.
On November 6, 2018, voters approved Nebraska Initiative 427, the Medicaid Expansion Initiative. The initiative required the state to provide Medicaid for persons under the age of 65 and with incomes equal to or below 138 percent of the federal poverty line. In 2018, this amounted to an annual income of $16,753 for an individual and $34,638 for a household of four. Initiative 427 required the Nebraska Department of Health and Human Services to file a state expansion plan with the federal Centers for Medicare and Medicaid Services on or before April 1, 2019.
GovernorPete Ricketts expressed opposition to Medicaid expansion in his 2016 State of the State address, stating, “One of the biggest long-term risks we face to the budget is Medicaid expansion. This body has wisely rejected Medicaid expansion three times in the past three years because it is an unreasonable risk to Nebraska taxpayers.”
Support
Opposition
Medicare Advantage And Prescription Drug Plan Enrollment Periods
Initial enrollment for Medicare Advantage may be completed during Medicares 7-month initial enrollment period or during the annual enrollment period, which occurs between October 15 and December 7. At this time, beneficiaries may switch between Original Medicare and Medicare Advantage plans. Enrollees who havent previously purchased a Part D plan may also do so at this time.
A second Medicare Advantage enrollment period is available between January 1 and March 31. During this period, current MA beneficiaries may switch to a different Advantage plan or revert coverage back to Original Medicare.
How Many People Are On Medicaid
According to the Centers for Medicare & Medicaid Services, as of November 2020, here are the number of people enrolled in Medicaid and Chip in the entire United States:
- 78,521,263 individuals were enrolled in Medicaid and CHIP
- 72,204,587 individuals were enrolled in Medicaid
- 6,695,834 individuals were enrolled in CHIP
Read Also: Can Medicaid Be Transferred To Another State
Expanded Medicaid In Nebraska
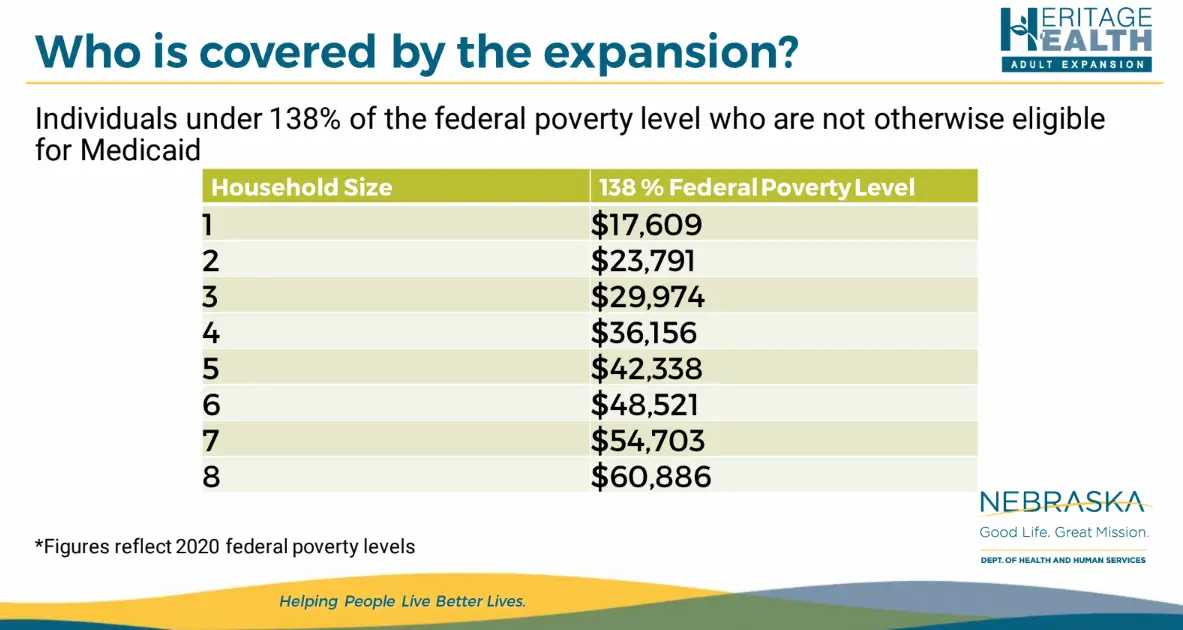
Access to quality, affordable, and equitable health care can be life-changing. Nebraska has expanded Medicaid benefits to low-income, able-bodied adults of working age . You must meet income requirements to qualify. Benefits include doctor services, emergencies, hospitalization, maternity and newborn, dental services, vision services and more. Find DHHS fact sheets, flyers, rack cards, and more on expanded Medicaid at dhhs.ne.gov/Pages/Medicaid-Expansion.aspx.
How Do I Enroll In Medicare In Nebraska
Eligible applicants who aren’t automatically enrolled may apply for Medicare benefits through the Social Security Administration. You may sign up for benefits by doing one of the following:
- Filling out an online application through the Social Security Administration’s website
- Visiting your local Social Security office
Also Check: What Age To Apply For Medicaid
State And Federal Spending
During fiscal year 2016, Medicaid spending nationwide amounted to nearly $553.5 billion. Spending per enrollee amounted to $7,067 in fiscal year 2013, the most recent year for which per-enrollee figures were available as of June 2017. Total Medicaid spending grew by 33 percent between fiscal years 2012 and 2016. The Medicaid program is jointly funded by the federal and state governments, and at least 50 percent of each state’s Medicaid funding is matched by the federal government, although the exact percentage varies by state. Medicaid is the largest source of federal funding that states receive. Changes in Medicaid enrollment and the cost of healthcare can impact state budgets. For instance, in Nebraska, the percentage of the state’s budget dedicated to Medicaid fell from 17.2 percent in 2010 to 16.9 percent in 2015. However, state cuts to Medicaid funding can also mean fewer federal dollars received by the state.
During fiscal year 2016, combined federal and state spending for Medicaid in Nebraska totaled about $2 billion. Spending on Nebraska’s Medicaid program increased by about 16.5 percent between fiscal years 2012 and 2016. Hover over the points on the line graph below to view Medicaid spending figures for Nebraska. Click on the red bar below the graph to view these figures as compared with three of Nebraska’s neighboring states.
Who Can Get Medicaid In Nebraska
You should apply for Medicaid if your income is low and you match one of the descriptions below:
- You think you are pregnant
- The parent or caretaker of a child and/or teenager under the age of 19.
- You are a child or teenager age 18 or under.
- An adult age 65 or older.
- You are legally blind.
- Living with a disability or disabled.
- You are in need of nursing home care.
Don’t Miss: Does Sc Medicaid Cover Weight Loss Surgery
Children’s Health Insurance Program
The Children’s Health Insurance Program is a public healthcare program for low-income children who are ineligible for Medicaid. CHIP and Medicaid are related programs, and the former builds on Medicaid’s coverage of children. States may run CHIP as an extension of Medicaid, as a separate program, or as a combination of both. Like Medicaid, CHIP is financed by both the states and the federal government, and states retain general flexibility in the administration of its benefits.
CHIP is available specifically for children whose families make too much to qualify for Medicaid, meaning they must earn incomes above 138 percent of the federal poverty level, or $33,948 for a family of four in 2017. Upper income limits for eligibility for CHIP vary by state, from 175 percent of the federal poverty level in North Dakota to 405 percent of the FPL in New York. States have greater flexibility in designing their CHIP programs than with Medicaid. For instance, fewer benefits are required to be covered under CHIP. States can also charge a monthly premium and require cost sharing, such as copayments, for some services the total cost of premiums and cost sharing may be no more than 5 percent of a family’s annual income. As of January 2017, 14 states charged only premiums to CHIP enrollees, while nine states required only cost sharing. Sixteen states required both premiums and cost sharing. Eleven states did not require either premiums or cost sharing.
Applying For Heritage Health
Nebraska Total Care is a health plan available through the Nebraska Department of Health and Human Services Heritage Health program.
We do not decide who is eligible for the plan. If you would like information about eligibility, please contact ACCESSNebraska at 1-855-632-7633. You can visit ACCESSNebraska.
Read Also: How To Qualify For Medicaid
Learn About Chip In Nebraska
For almost 20 years, the Nebraska Childrens Health Insurance Program has helped many children access affordable health coverage. NE CHIP is designed for children who do not meet the eligibility requirements for Medicaid, but cannot otherwise afford health insurance. Medicaid for children and the CHIP program are not the same, even though they are similar in nature. Those who want to apply to the program may be asking themselves, What is CHIP Medicaid? and, Is CHIP considered Medicaid? as they are researching the program. Get the answers to those questions and learn what is covered by CHIP Medicaid by reading the rest of the information below.
What is Nebraskas Childrens Health Insurance Program?
All 50 states have a version of the CHIP program, but it can be managed differently. Some states allow you to apply for both programs at the same time, while others do not. That is why is it important to know how CHIP and Medicaid enrollment is managed in Nebraska.
The factors of Medicaid eligibility children cannot meet are typically satisfied under CHIP in NE. Once enrolled, recipients will be able to choose whichever health care providers they would like to go to, as long as the providers are in-network with CHIP. It is important for all CHIP and Medicaid enrollees to see in-network providers, as out-of-network services may not be covered by the program. Certain services may come with copays for CHIP enrollees.
to read more about both the CHIP and Medicaid programs.
Nebraska Medicaid Enrollment Numbers
By mid-April 2014, 9,879 Nebraska exchange applicants had enrolled in Medicaid or CHIP. They were already eligible based on the pre-2014 enrollment guidelines, but may not have known that Medicaid was available to them.
But from the fall of 2013 through July 2016, total net enrollment in Nebraskas Medicaid program actually by 9,764 people, which amounted to a decrease of 4%. , however, enrollment was back to nearly where it had been in 2013, with only 188 fewer enrollees.
The state estimated that about 90,000 people would gain coverage under Medicaid expansion, although that number is likely to be higher now that the COVID-19 pandemic has resulted in widespread job losses. The pandemic had increased the number of people relying on Medicaid even before expansion took effect.
As of May 2021, 324,200 Nebraskans are enrolled in Medicaid/CHIP programs.
Also Check: Medicaid Ms Gov Programs Managed Care
Automatic Enrollment In Medicare
Seniors whove been receiving retirement benefits from Social Security or the Railroad Retirement Board for four months or longer prior to their 65th birthday are automatically enrolled in Original Medicare, with coverage beginning the first day of their birthday month. Beneficiaries who would prefer Medicare Advantage may select an MA plan during the qualifying enrollment period.
Effective Date Of Coverage
Once an individual is determined eligible for Medicaid, coverage is effective either on the date of application or the first day of the month of application. Benefits also may be covered retroactively for up to three months prior to the month of application, if the individual would have been eligible during that period had he or she applied. Coverage generally stops at the end of the month in which a person no longer meets the requirements for eligibility.
You May Like: How Does A Person Get On Medicaid
Option 3 Download Application
You can , complete it, and mail it to your county DHHS office or submit it in person.
Additionally, you can call one of the numbers below to apply over the phone or to request a paper Medicaid application.
The phone lines are open from 8:00 a.m. to 5:00 p.m. Monday through Friday.
1- 632-7633
A ballot initiative to expand Medicaid coverage under the ACA passed in November 2018.
Medicaid expansion enrollment in Nebraska began on August 1, 2020.
Coverage takes effect October 1, 2020.
Nebraskas plan to expand Medicaid includes the following:
- Two tiers of coverage, with various requirements
- Work requirements starting in year two in order to receive enhanced benefits.
Nebraskas Medicaid current managed care system, Heritage Health, took effect in January 2017.
The state of Nebraska initially expected roughly 90,000 people to become newly eligible for Medicaid coverage in Nebraska under the expanded eligibility guidelines.
However, a recent Families USA analysis indicates that an additional 33,000 people could be eligible due to the job losses caused by the COVID-19 pandemic.
Past Efforts To Expand Coverage Via Legislation Were Unsuccessful
In 2013, LB577, which would have created a modified Medicaid expansion program, was rejected by the legislature in Nebraska. A year later, the Wellness in Nebraska Act was introduced in January 2014 by Senator Kathy Campbell, but it didnt pass during the 2014 legislative session, and was indefinitely postponed in April 2014.
The Wellness in Nebraska Act would have expanded traditional Medicaid to people with incomes up to the poverty level , and would have relied on federal Medicaid funding to purchase private coverage for people with incomes between 100% and 138% of poverty. Several states are using waivers to implement unique approaches to Medicaid expansion, and New Hampshire and Arkansas both use waivers purchasing private coverage for at least some Medicaid enrollees.
In 2015, lawmakers introduced Legislative Bill 472 to expand Medicaid, but it did not pass out of committee. Also in 2015, two professors from the University of Nebraska-Kearney that found that expanding Medicaid would result in significant financial benefits for the state. After exhaustive study, the researchers concluded that expansion of Medicaid passes a rigorous cost/benefit analysis.
In January 2016, Nebraska State Senator John McCollister , introduced Legislative Bill 1032 in an effort to expand Medicaid in Nebraska. McCollister had been leading the push for Medicaid expansion in the state for almost a year at that point, but his legislation failed to advance out of committee.
Read Also: New Mexico Medicaid Provider Portal
The Specifics Of Nebraskas Medicaid Expansion 1115 Waiver Approved By Cms In October 2020
Although lawmakers in Utah and Idaho passed legislation in 2019 to adjust the terms of the Medicaid expansion ballot initiatives that voters had passed in those states, Nebraska lawmakers did not . Instead, the Nebraska-specific modifications to Medicaid expansion have come from Governor Ricketts administration. And while the modifications are not as draconian as those implemented in other states , Nebraska is still deviating from the version of Medicaid expansion called for in the ACA and approved by the states voters and is adding administrative cost and additional complexity.
To expand Medicaid, Nebraska has added the Heritage Health Adult Program to its existing Heritage Health Program. Initially, the state had planned to transition about 25,000 low-income parents and caretaker relatives who are already eligible for Medicaid in Nebraska to the Heritage Health Adult Program for these enrollees, rather than the enhanced matching rate that applies to the newly-eligible population). But the draft 1115 waiver proposal that the state published in October 2019 noted that the Heritage Health Adult Program would only include people who are newly eligible for Medicaid under the expansion guidelines .
Starting in year two , enrollees will also have to fulfill a work requirement in order to qualify for Prime Coverage. For 80 hours each month, they will need to either be working , going to school, volunteering for a public charity, or serving as a caregiver for a relative.
Enrolling With Nebraska Total Care
Heritage Health has an open enrollment period once each year. You can choose Nebraska Total Care during open enrollment or when you are new to Heritage Health.
The Enrollment Broker will help you make an informed choice about your health plan. Contact them at 1-888-255-2605. You can visit Heritage Health.
Also Check: How Much Do You Have To Earn To Get Medicaid
Coordinated System Has Three Managed Care Organizations
As of 2013, nearly 76% of Nebraskas Medicaid enrollees were in managed care programs run by Aetna, AmeriHealth, and UnitedHealthcare. The state overhauled its Medicaid managed care system in 2016, and managed care contract bids were submitted by six carriers in early January.
The overhauled program is called Heritage Health, and it combines coverage of physical health, behavioral health, and pharmacy care into one coordinated system. The new system took effect January 1, 2017. Three carriers were awarded contracts to serve as managed care plans under Heritage Health:
- Nebraska Total Care
- UnitedHealthcare Community Plan
- Wellcare of Nebraska
These three carriers will also serve the new Heritage Health Adult population once Medicaid expansion takes effect in late 2020.
Where Can I Apply For Medicaid In Nebraska
The Medicaid program is administered by the Nebraska Department of Health and Human Services . Seniors and people with disabilities can apply for Medicaid by visiting this website, calling 632-7633 or visiting a local Public Assistance office.
Josh Schultz has a strong background in Medicare and the Affordable Care Act. He coordinated a Medicare technical assistance contract at the Medicare Rights Center in New York City, where he represented clients in extensive Medicare claims and appeals. In addition to advocacy work, Josh helped implement federal and state health insurance exchanges at the technology firm hCentive. He has also held consulting roles, including at Sachs Policy Group, where he worked with hospital, insurer and technology clients.
Don’t Miss: Pueblo Dentists That Take Medicaid
What Are The Requirements For Medicaid In Nebraska
In the state of Nebraska, Medicaid services are available to qualifying low-income or very-low-income applicants who meet state-specific eligibility requirements. Medicaid eligibility requirements require a beneficiary to be low-income, elderly, disabled or pregnant, or to be low-income and have children.
Additionally, Medicaid benefits are available to candidates who are 65 or older or who are under the age of 65 and have a disability. Requirements for Medicaid also apply to candidates who are 18 or younger.
Dependent children who meet the requirements of the Aid to Dependent Children Program may also be eligible for Medicaid. As a whole, the following Medicaid requirements apply to all potential beneficiaries planning to enroll in Medicaid benefits in Nebraska:
- An application must be completed
- Beneficiaries must be U.S. citizens or hold legal alien status
- Applicants must reside in Nebraska
- A Social Security Number is required
- Income restrictions must be satisfied
- Current health insurance policies must be stated, if applicable
- Household members must be noted
Children who do not meet Medicaid eligibility requirements and who do not have other health insurance coverage may be eligible to receive assistance from the Childrens Health Insurance Program . Nebraska CHIP is an expansion of Nebraska Medicaid and provides many of the same Medicaid services. to learn about the different requirements for Medicaid.
Apply For Medicaid In Nebraska

You can enroll online at HealthCare.gov or use the call center at 1-800-318-2596. You can also enroll online at ACCESSNebraska, or print a paper application from their website.
Eligibility: Parents with dependent children are eligible with household income up to 57% of poverty. Pregnant women with income up to 194% of poverty, and children with income up to 213% of poverty.
Read Also: Does Maryland Medicaid Cover Abortions