Does Pregnancy Medicaid Cover Dental
Although pregnant women enrolled in Medicaid and CHIP are entitled to ?pregnancy-related services,? dental care is not explicitly included as a pregnancy-related service, and federal Medicaid law leaves dental care for adult enrollees as a state option.3 CHIP requires coverage of dental care for youth, including
Dont Miss: Vagisil While Pregnant
Will Medicaid Cover Dental For My Kids
The Affordable Care Act expanded Medicaid eligibility so that the program could cover more low-income Americans.¹ In addition to making more people eligible for coverage, this expansion provided funds that many states used to improve their dental coverage. Some states increased the Medicaid reimbursements for childrens dentistry as well as expanded the number of services covered¹.
Medicaid covers dental services for children, but covered dental services for children may vary from state to state.
At a minimum, states must provide dental services for children through the Medicaid program that covers the following¹:
-
Pain relief and infections
-
Teeth restorations (such as fillings and some types of crowns
-
Maintenance of dental health ¹
Dental services for Medicaid-eligible children cannot be limited to only emergency services. Medically necessary care must be provided. Each state determines its own definition of which dental services fall into the medically necessary category.
What Does South Carolina’s Medicaid Cover
Fillings are also included.
Dental coverage also includes preventive services, such as cleanings and exams, that help keep your teeth healthy. These services include:
Breath tests to check for signs of diabetes or other illnesses
Blood glucose monitoring supplies
Cavity prevention treatments
Checkups
Cosmetic dentistry procedures such as tooth whitening and veneers
Fillings
Prosthodontics . This includes complete or partial dentures, which are necessary when some of the teeth have been lost due to decay or injury.
Root canals . Root canals are painful procedures they require local anesthesia and several visits to the dentist. However, this is the only way to save the tooth.
About Article Author
You May Like: Dentist In Columbus Ms That Accepts Medicaid
Medicaid For Pregnant Women & Chip Perinatal
Pregnant women might be able to get free health coverage during their pregnancy through Medicaid for Pregnant Women or the CHIP Perinatal program.
Medicaid provides health coverage to low-income pregnant women during pregnancy and up to two months after the birth of the baby.
CHIP Perinatal provides similar coverage for women who can’t get Medicaid and don’t have health insurance.
To get Medicaid for Pregnant Women or CHIP Perinatal, you must be a Texas resident. You must be a U.S. citizen or qualified non-citizen to get Medicaid for Pregnant Women.
If you have other health insurance, you are not eligible for the CHIP Perinatal program.
When you apply, we’ll ask about your family’s monthly income to see if you can get Medicaid or CHIP Perinatal.
Early And Periodic Screening Diagnostic And Treatment
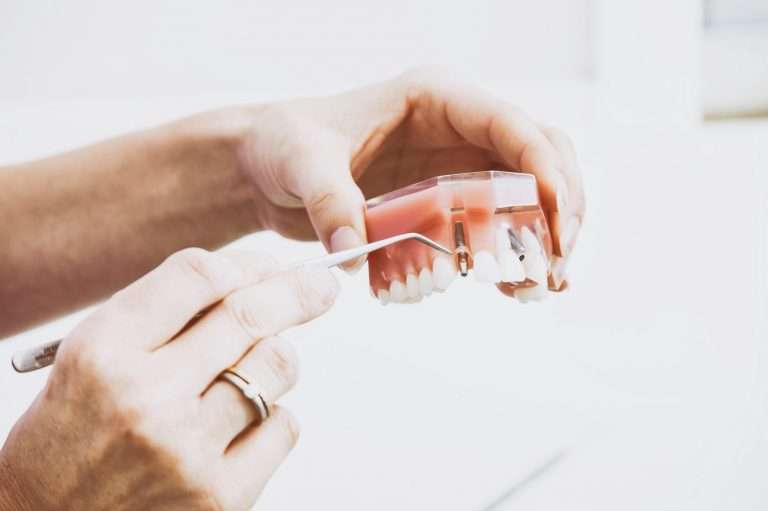
The Early and Periodic Screening, Diagnostic and Treatment benefit provides comprehensive and preventive health care services. EPSDT is key to ensuring that children and youth receive appropriate preventive, dental, mental health, developmental and specialty services.
All Health First Colorado coverable, medically necessary services must be provided even if the service is not available under the state plan to other people who qualify for Health First Colorado. Benefits not listed are not considered to be a state plan benefit and are therefore outside of EPSDT coverage and exceptions. No arbitrary limitations on services are allowed, e.g., one pair of eyeglasses or 10 physical therapy visits per year.
Who Qualifies?
Children and Youth ages 20 and younger who are enrolled in Health First Colorado.
Top Benefits:
- Providing physical, mental, developmental, dental, hearing, vision, and other screening tests to detect potential problems
- Arrange for corrective treatment as determined by child health screenings
- Lead Screening
Co-pay Costs:
Children under the age of 19 do not have co-pays. Co-pay costs for youth ages 19 and 20 vary, see program information page.
| Program Information Page |
Read Also: Can I Sell My House While On Medicaid
Dental Services Covered By Medicaid
Children under 21 years of age enrolled in Medicaid receive a comprehensive set of benefits known as the Early and Periodic Screening, Diagnostic and Treatment benefit. At minimum, children must receive dental services that:
- Maintain dental health
- Restore teeth
- Relieve pain and infections
In addition, if a dental condition is uncovered through a regular dental examination and it requires treatment, the state must also provide the necessary treatment even if it isnt normally part of what that state covers.
Here are examples of common dental services that might be provided include:
- Regular dental cleanings and exams
- Fluoride treatments
- Extractions
- Other dental services that are medically necessary
If your child is covered by Medicaid, you will not need to pay co-payments or premiums for your childs dental care. Our office is familiar with and will interact with the Medicaid office if there are any questions about our treatment plan. Find Medicaid and the Childrens Health Insurance Program coverage options for your family.
States Decide What Dental Services They Will Cover For Adults So Benefits Vary From State To State
Dental care is necessary to keep your teeth and gums healthy, but many low-income people may have no access to dental care. As of 2016, about 74 million Americans dont have any dental insurance.¹ Medicaid, is a federal-state assistance program for low-income people and children, that helps fill in the gaps for health and hospital care and typically provides limited dental coverage for adults.
What Medicaid covers depends on where you live. While Medicaid guidelines require states to provide some level of dental care for children, states are not required to provide dental benefits to adults². Each state decides whether to provide dental care to adults and, if so, which dental services they will cover. As of 2020, there are 35 states along with the District of Columbia that have expanded their Medicaid coverage to include some limited dental coverage for adults.³
Also Check: My Texas Benefits Pregnancy Medicaid
Does Medicaid Cover Dental For Adults In 2021
Medicaid covers dental care for adults in every state, except for Delaware, Maryland and Tennessee. Coverage varies widely between states, from basic emergency care to extensive coverage.
Many states have mandatory limits on the amount of dental work Medicaid will cover. Some states cap the annual funding per beneficiary, and limits range between $500 and $2,500. Other states limit the number of dental procedures that can be covered by Medicaid each year or over the course of a lifetime. For example, Connecticut and Illinois only fund one root canal per tooth over the beneficiary’s lifetime. Most state Medicaid plans only pay for one dental examination or hygiene treatment per year.
If you are pregnant or have certain disabilities that make dental problems more likely, you may be entitled to more extensive dental coverage through Medicaid than most adults in your state. Roughly half of all states offer enhanced Medicaid dental coverage to pregnant women.
You’ll usually require authorization before Medicaid will cover planned dental treatment. However, the requirement for authorization is often waived if you need emergency treatment or pain relief.
Colorado Indigent Care Program
The Colorado Indigent Care Program provides discounted health care services to low income people and families. CICP is not a health insurance program. Services vary by providers.
Who Qualifies?
You must be 18 and olderYou must be at or below 250% of the Federal Poverty Level You must be lawfully present in the United States and a legal resident of ColoradoYou cannot be eligible for Health First Colorado or Child Health Plan Plus
Top Benefits:
Discounted health care services provided by participating Colorado hospitals and clinicsNo premium costsYou are allowed to have primary health insurance or have MedicareCICP ratings are good for a full year, see program information page for exceptions
Co-pay Costs:
| Program Information Page |
Don’t Miss: Does Medicaid Cover Gym Memberships
Does Medicaid Cover Dental Dentures In The Dental Services
Many states do not provide such facilities, and some provide complete or partial assistance. But in this case, the recipient has to qualify first to get treatment.
For this purpose, meeting the eligibility criteria according to some of the guidelines part of this program is mandatory. Alaska, North Dakota, New York, Michigan, Idaho, etc., are some of the states that allow and pay for dentures. These include both partial and complete treatments that facilitate people greatly. For instance, in New York, even adults can get dentures, and New York Medicaid undertakes all their costs.
Does Medicaid Cover Dental Implants
This question, although simple, cannot get a simple answer. Since the program differs from state to state, it has its terms and conditions everywhere. Does Medicaid cover dental implants for everyone? The procedures are termed cosmetic Medicaid does not pay for them. Since this program is government-run, it indeed covers and provides aid to financially weak individuals. Dental implants are usually cosmetic, and thus, the Medicaid program does not cover such treatments, but there indeed are some exceptions. So, if you are someone who needs implants for another medically essential procedure, then you may find yourself eligible for this treatment.
Read Also: Denture Places That Accept Medicaid
Dental Benefits For Children In Medicaid
Medicaid covers dental services for all child enrollees as part of a comprehensive set of benefits, referred to as the Early and Periodic Screening, Diagnostic and Treatment benefit. Though oral screening may be part of a physical exam, it does not substitute for a dental examination performed by a dentist. A referral to a dentist is required for every child in accordance with the periodicity schedule set by a state.
Dental services for children must minimally include:
- Relief of pain and infections
- Restoration of teeth
- Maintenance of dental health
The EPSDT benefit requires that all services must be provided if determined medically necessary. States determine medical necessity. If a condition requiring treatment is discovered during a screening, the state must provide the necessary services to treat that condition, whether or not such services are included in a states Medicaid plan.
Each state is required to develop a dental periodicity schedule in consultation with recognized dental organizations involved in child health care. Dental services may not be limited to emergency services for children entitled to EPSDT.
Does Private Insurance Also Cover A Newborn

It depends. Small group employer-sponsored plans must include the EHBs, including maternity and newborn care, but large group and self-insured employer-sponsored plans are exempt from this requirement. While the requirement for newborn care covers childbirth and immediate care following birth, women must enroll their babies in coverage soon after birth.
Don’t Miss: Does Disability Count As Income For Medicaid
States That Provide Extensive Dental Medicaid To Their Citizens
On the brighter side, some states provide a lot of dental procedures and treatments as part of their Medicaid programs. These states are precisely 18 in number and are as follows:
- California
- North Carolina
- North Dakota
These states offer Medicaid programs that provide extensive dental procedures and treatments to their citizens. Roughly benefits of around 1000$ to 1500$ are given annually. And these exclude all cosmetic procedures. So these are the states for which you do not have to ask anyone if/does Medicaid cover dental practices and services?
Child Health Plan Plus
Child Health Plan Plus is a public health insurance program for children ages 18 and younger and pregnant women who earn too much to qualify for Health First Colorado , but cannot afford private health insurance. Note: Health First Colorado and Child Health Plan Plus are both public health insurance programs for Coloradans who qualify. When you apply for Health First Colorado, you are applying for both Health First Colorado and CHP+. You do not need to turn in more than one application for you or your family.
Who Qualifies?
- Children ages 18 and younger
- Pregnant women
- All who qualify must meet certain income level requirements
Top Benefits:
- Regular checkups
- Mental health and substance use disorder services
Co-pays and Enrollment Fees:
| Program Information Page |
Recommended Reading: How Can I Check The Status Of My Medicaid Application
Dental Benefits For Adults In Medicaid
States have flexibility to determine what dental benefits are provided to adult Medicaid enrollees. While most states provide at least emergency dental services for adults, less than half of the states currently provide comprehensive dental care. There are no minimum requirements for adult dental coverage.
What Is Medicaid For Pregnant Women
With Medicaid for pregnant women, you get full health care benefits during your pregnancy and for two months after your babys birth. Medicaid may also cover your medical bills for the three months before you enroll. You also get dental benefits during your pregnancy. Dental services are through the Smiles for Children program. For help finding a dentist or to learn more, call Smiles For Children at 1-888-912-3456. Also read the Guide to Dental Coverage.
Recommended Reading: Medicaid Fraud Cases In Louisiana
Get Important News & Updates
Sign up for email and/or text notices of Medicaid and other FSSA news, reminders, and other important information. When registering your email, check the category on the drop-down list to receive notices of Medicaid updates check other areas of interest on the drop-down list to receive notices for other types of FSSA updates.
Does Pregnancy Medicaid Cover Tooth Extraction
Some people, who have many problems in their mouth and teeth, may have to undergo many dental procedures and may not be able to afford them. Many people, including pregnant women, with low income can enroll into Medicaid, depending on their states program . Like other people, pregnant women still need to visit the dentist, and fortunately, they can utilize their Medicaid coverage for dental services.
Pregnant women need dental care, but they could postpone some procedures until they give birth to their baby. They should visit the dentist for Preventive dental cleanings and annual exams because The rise in hormone levels during pregnancy causes the gums to swell, bleed, and trap food causing increased irritation to your gums . If these women do not receive preventive care, they can develop oral infections such as gum disease, which has been linked to preterm birth .
Pregnant women should also undergo other needed procedures, such as root canals and extractions in emergencies as well as cavity fillings and crowns to reduce the chance of infection . Usually, women in their second trimester can undergo dental procedures safely, but women in their third trimester may find on your back for an extended period of time . Expectant women could schedule less urgent procedures, such as teeth whitening and other cosmetic procedures after the birth since some procedures may endanger the developing baby .
Medicaid Dental Coverage for Pregnant Women
MORE POSTS:
Also Check: Dual Enrollment Medicare And Medicaid
Types Of Medicaid Plans Including Dental
The type of Medicaid that you have could impact whether it pays for dental work for adults. Each state offers a variety of plans designed for different groups of low-income individuals.
In addition to the straight or regular program, you could enroll in unique plans for pregnant women, dual-eligible Medicare recipients, and individuals deemed medically needy.
Upcoming Changes To Dental Services In Florida Medicaid
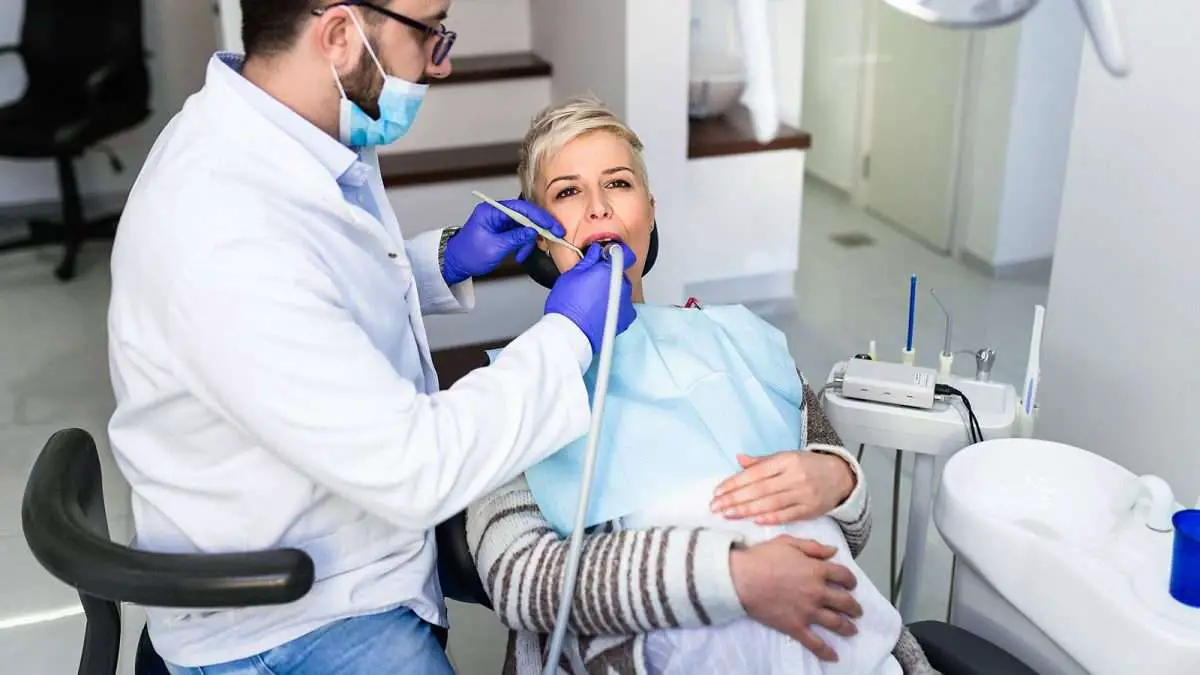
In 2016, the Florida Legislature directed the Agency for Health Care Administration to enroll most Medicaid recipients into dental plans. Recipients will receive a dental plan based on the below schedule. The schedule is separated into phases by the recipients county location.
Recipients will begin to receive letters soon. They will be mailed out about 45 days before each phase starts. For example, recipients will begin to receive letters for Phase 1 in the middle of October. For more information, please click on the following link:
Also Check: Emblemhealth Enhanced Care Prime Medicaid
Does Medicaid Cover The Cost Of Dental Care
Each state has different qualifications and requirements that must be met for dental care to be covered by Medicaid. You will need to do some research to find out what the specific requirements are for your state.
About less than half the states will provide comprehensive dental benefits. On the other hand, in thirty-two states, Medicaid will cover dental care for certain categories, such as emergency dental services and medically necessary dental work.
How Much Do Dentures Cost With Medicaid Coverage
Dentures can be quite costly, especially if you need a full set. The cost of dentures with Medicaid coverage will vary depending on the type of dentures you need and your specific coverage. In general, however, you can expect to pay anywhere from a few hundred to a few thousand dollars for your dentures with Medicaid coverage.
Recommended Reading: Emergency Clinics That Take Medicaid
What Does Medicaid Pay For In The Health Field
Medicaid is thus a program that pays for several healthcare methods and treatments. It covers various therapies and medical treatments. This is why many US citizens enroll themselves in this program and utilize all its health benefits. Families can also help from this initiative that the government has put forward for its public. Individuals such as children, adults, disabled people, etc., all have their own set of health that they can use. Following are some of the health areas that Medicaid covers and pays for:
Who Requires A Dental Crown
Since we previously said that crowns are most of the time required and therefore covered by Medicaid, we will discuss a few instances where a crown must be fitted:
- To aid in the protection of a weaker tooth that is about to break or is already damaged
- To aid in the restoration of a fractured or worn-down tooth
- To keep your prosthesis in a place as a bridge
- To conceal discolored or damaged teeth
Your dentist can advise that all of the aforementioned scenarios are medically required. In some circumstances, you will either be fully covered by Medicaid or will be required to pay a co-payment, depending on your state of residency.
Also Check: Does Wv Medicaid Cover Dentures
