Apply For Medicaid In Florida
Online at ACCESS Florida, or submit a paper application by mail, fax or in person to a local service center. For help with the application process, call 866-762-2237.
Eligibility: Children up to 1 year old with family income up to 206% of FPL children 1-5 with family income up to 140% of FPL children 6-18 with family income up to 133% of FPL pregnant women with family income up to 191% of FPL young adults 19-20 with family income up to 30% of FPL adults with dependents with family income up to 30% of FPL.People who qualify for Supplemental Security Income automatically qualify for Medicaid. For information: SSI-Related Programs Financial Eligibility Standards
Section 1115 Demonstration Waiver
On July 31, 2014, CMS approved Florida to continue its §1115 Managed Medical Assistance demonstration waiver through June 30, 2017. The waiver was initially approved in 2005. Under the demonstration, managed care participation is mandatory for TANF-related populations and the Aged and Disabled group, as well as individuals eligible for both Medicare and Medicaid. The following populations may choose to be participants in the managed care demonstration: Individuals who have other creditable health care coverage, excluding Medicare individuals age 65 and over residing in a mental health treatment facility meeting the Medicare conditions of participation for a hospital or nursing facility individuals in an intermediate care facility for ID individuals with DD enrolled in the HCBS waiver pursuant to state law and Medicaid recipients waiting for waiver services. Fact Sheet
On March 27, 2015, the Florida Agency for Health Care Administration posted its draft §1115 Medical Managed Assistance Waiver Amendment Request, along with a Public Notice of two April meetings to solicit public input about the waiver amendment request. The state is seeking the waiver amendment to change the auto-assignment criteria and remove the 30-day wait period between eligibility determination and managed care plan enrollment.
How To Apply / Learn More
When the applicant senior is not in a nursing home, the application process starts with a call to the Florida seniors local Area Agency on Aging. One can also call the Elder Helpline. Find the number by county here. Callers should request a screening for home and community based services. The representative schedules a time for the phone screening with the primary caregiver or closest family member, usually one to two weeks out. The screening interview typically lasts 30 to 40 minutes. The interview covers basic demographic information for the applicant as well as his/her income and assets. The interview mostly asks about the elders needs for care, including his/her ability to perform Activities of Daily Living.
Following the interview, the elder receives a prioritization decision. This letter indicates whether services can begin immediately or whether the senior needs to be waitlisted. If the senior is prioritized for home or community supports to start immediately, he/she must apply to the Department of Children and Family Services through the ACCESS System for their formal Medicaid approval.
To learn more about SMMC LTC, .
Like Floridas HCBS Medicaid Waivers that served this population before the creation of this program, SMMC LTC has a limit on the number of persons who can receive assistance at the same time. Waiting lists for some services likely exist in areas throughout the state.
Recommended Reading: How Do I Apply For Medicaid Online
No Aca Medicaid Eligibility Expansion In Florida
Florida is one of 12 states that has not expanded Medicaid eligibility as allowed under Affordable Care Act . The ACA doesnt provide subsidies for people with income below the poverty level, because the law called for them to have Medicaid instead. But in states that have refused Medicaid expansion people who arent eligible for Medicaid and whose income is too low for exchange subsidies are in whats called the coverage gap.
Federal
Floridas eligibility standards are:
- Children up to 1 year old: 206% of the federal poverty level
- Children ages 1-5: 140% of FPL
- Children ages 6-18: 133% of FPL
- Pregnant women: 191% of FPL
- Adults with dependent children: 27% of FPL
People who qualify for Supplemental Security Income automatically qualify for Medicaid in Florida. See more information in the SSI-Related Programs Financial Eligibility Standards.
History Of Floridas Medicaid Program
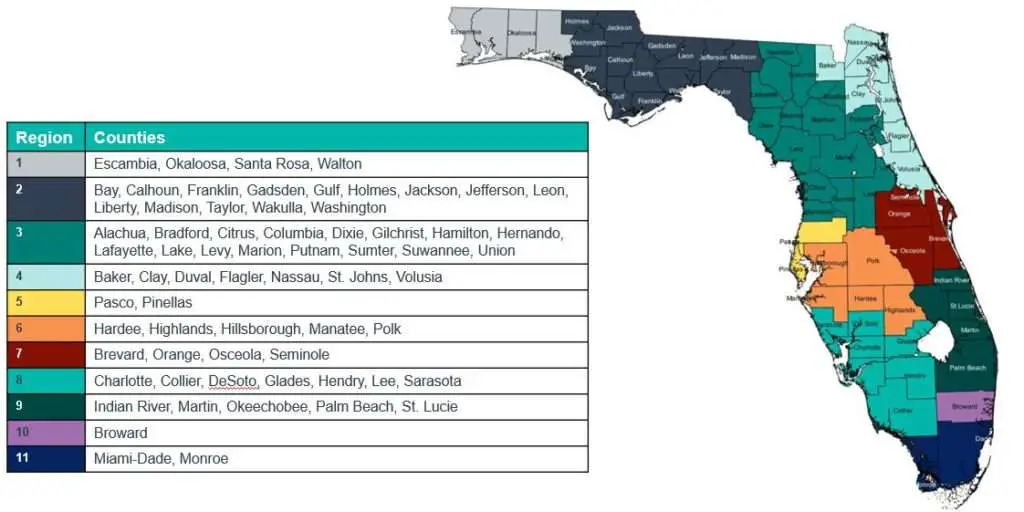
Florida was one of the later states to implement a Medicaid, not adopting the program until January of 1970 .
Florida Medicaid spending grew 13.5% on average every year between 1980 and 2004. In an effort to slow that trend, Florida applied for and received approval for an 1115 waiver for its Medicaid Reform pilot. The pilot implemented managed care in two counties in 2006 and added three more counties in 2007 the waiver was extended several times.
In 2013, the federal government approved an amendment for statewide expansion of managed care the amendment also renamed Medicaid Reform as Managed Medical Assistance . Ninety percent of all Florida Medicaid beneficiaries are now enrolled in managed care plans, like health maintenance organizations . The state hopes to improve quality through better coordination of care and save money through smaller networks of providers.
Part of the reason Medicaid enrollment has grown is the extensive outreach on the part of ACA navigators some residents were already eligible for Medicaid or CHIP prior to 2014 , but werent aware of their eligibility until enrollment outreach efforts under the ACA. But since Florida hasnt expanded Medicaid, the newly insured population is covered according to the normal state/federal split.
Floridas decision not to expand Medicaid leaves nearly 400,000 people in the state in the coverage gap ineligible for Medicaid and also ineligible for tax subsidies to help them afford private health insurance .
Read Also: Fertility Doctor That Takes Medicaid
What Are My Florida Medicaid Waiver Long
The Statewide Medicaid Managed Care program providers can be found on the Florida Medicaid Managed Care website. Some of the Florida Statewide Medicaid Managed Care LTC Plan Choices are :
Waiting lists / waiting times for home and community based care are not expected to change. Priority is given to individuals based on their level of need for services.
LTC providers will provide personal care services for those who qualify, and if specified in the enrolleeâs plan of care , including: pest control, homemaker, companion, chore, enhanced chore, and home delivered meals. Through the Participant Direction Option the participant can sometimes choose who will provide their services . Rates for PDO services are set by the LTC plans.
Additional Smmc Ltc Information:
For additional SMMC LTC information, including a program overview and summary, please visit AHCAs website at .
For information regarding the LTC plans available in each region and how to choose an LTC plan, please visit the Choice Counseling website at www.flmedicaidmanagedcare.com.
For more information regarding the SMMC LTC waitlist, please contact your local Aging and Disability Resource Center. Click here for the direct contact information of the ADRC in your region. You can also call the statewide Elder Helpline at 1-800-96-ELDER for immediate assistance.
For assistance in addressing a complaint with your LTC plan, please visit AHCAs website at and click on the Report a Complaint button.
Don’t Miss: How Old Do You Have To Be To Get Medicaid
Evv And Claims Billing For Floridas State Medicaid Managed Care Program
Starting on December 1, 2018, Humana, Staywell, and Sunshine Health will require providers to use HHAeXchange to submit confirmed visits and bill directly to each MCO through the free HHAeXchange Portal.
The first step in effectively working with the MCOs is to fill out the Florida SMMC Provider Portal Configuration Questionnaire questionnaire for your organization. The answers from your questionnaire will allow HHAeXchange to configure your agencys portal. Please note that you only need to fill out the questionnaire once, regardless of how many MCOs you are contracted with.
Importing Caregivers Into Hhaexchange
To assist organizations with a large census of Caregivers, HHAeXchange has created a Caregiver Bulk Import tool to expedite the entry process.
Please to access the Caregiver Bulk Import Process Guide, which provides instructions for how to:
- Access and Save the Caregiver Import Template
- Prepare the Caregiver import File for your Agency
- Send the file to HHAeXchange for File Processing
Recommended Reading: Does Md Anderson Take Medicaid
Your Agencys Billing Options
Option 1, Free HHAeXchange EVV: Our agency wants to use HHAeXchanges free EVV system, provided by the MCOs. Great! If youve indicated that youd like to use HHAeXchanges free EVV system, the contact person listed on your questionnaire will receive more information in the coming weeks on how to set up your agencys 800 numbers, upload caregivers into the HHAeXchange Portal, and begin processing EVV and claims.
Option 2, Use my Current EVV System: Our agency has an existing EVV system that wed like to keep. Its simple to connect your existing EVV system to the MCOs through the HHAeXchange Portal. Ensure that youve completed the questionnaire, and the HHAeXchange Integrations Team will coordinate with you to create an interface to process your existing EVV visits and claims.
Florida State Medicaid Managed Care Provider Information Center
At HHAeXchange, we believe that healthcare should be simple, effective, and transparent. Our mission is to provide better outcomes for patients who represent some of the most vulnerable and fragile members of our society. Since 2008, we have been at the forefront of delivering industry-leading homecare management solutions by helping payers and providers achieve operational efficiency, increased compliance, and improved patient outcomes.
Today, HHAeXchange is the premiere homecare management software solution for the Medicaid LTSS population. We act as the single source of truth in connecting payers, providers, and patients through our intuitive web-based platform, enabling unparalleled communication, transparency, and visibility.
- OVERVIEW
- CONTACT
Also Check: Get A Copy Of Medicaid Card
Medicaid Transformation Watched Closely In Florida
This week the federal government signed off on the first part of a plan that could eventually steer more than 3 million low-income Floridians on Medicaid into a managed care, or HMO system. The decision comes two years after Florida lawmakers approved the conversion in an attempt to control costs in the $21 billion program.
At that time, retirees were skeptical of how it would work.
Gov. Scott
For-profit companies have a fiduciary responsibility to do what? Make money. So theyre not going to manage their care, theyre going to ration their care, said Joseph Flynn, a retiree living in the Central Florida community of the Villages, where Gov. Rick Scott was holding a budget signing ceremony.
That skepticism has not gone away but now the federal Centers for Medicaid & Medicare Services has signed off on part of a waiver allowing Florida to begin its transition to managed care for Medicaid recipients in long-term care.
Under the states current fee-for-service model, when the patient goes to a nursing home, hospital or doctor, the health provider bills the state, and the state cuts a check. But that system is expensive, difficult for frail patients to navigate and doesnt necessarily result in good care. Florida officials and industry representatives say managed care will be an improvement.
This story is part of a reporting partnership that includes WFSU, NPR and Kaiser Health News.
Helping States Help Providers
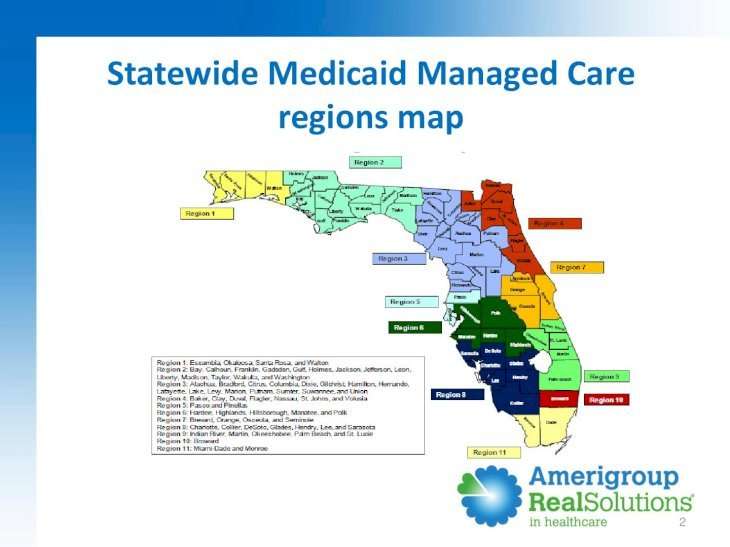
Through Medicaid managed care, providers benefit as well. MCOs use value-based payment models that incentivize, empower, and reward providers for their quality of care.
MCOs also help maintain strong provider networks and offer clinical support, continuing education, and technological innovations that enable providers to deliver higher quality care.
Managed care in Florida also helps to reduce administrative burdens by allowing high-performing providers to bypass prior authorization and completing credentialing for network contacts in 60 days.10
Recommended Reading: Can I Work And Still Get Medicaid
How Does Medicaid Provide Financial Help To Medicare Beneficiaries In Florida
Many Medicare beneficiaries receive Medicaid financial assistance that can help them with Medicare premiums, lower prescription drug costs, and pay for expenses not covered by Medicare including long-term care.
Our guide to financial assistance for Medicare enrollees in Florida includes overviews of these programs, including Medicaid nursing home benefits, Extra Help, and eligibility guidelines for assistance.
Coordinated Care For Floridians
MCOs coordinate care and provide a single point of contact for Floridians. By coordinating care, MCOs can help treat the whole person, serving as the glue that binds community resources with a unified health strategy, integrating physical and mental health services.
The managed care model, unlike the fee-for-service approach, is built to bring together disparate parts of the delivery system. MCOs are incentivized to partner with community groups to address social determinants of health, which can have a significant impact on the health of Floridians.
On a national level, MCOs social determinants initiatives are widespread and address numerous aspects of health, with 77% of MCOs reporting housing activities, 73% reporting nutrition activities, and 51% reporting education activities that aid the Medicaid population.9
of MCOs nationally report nutrition activities.9
Also Check: How To Get Help With Medicaid
Medicaid Managed Care An Eye On Florida And The Us
Medicaid Managed Care an eye on Florida and the US
The managed care takeover of states Medicaid funded long term care systems has resulted in a general acceptance of the private, for profit, centralized model of care with a goal of moving care into the community and away from nursing homes. Forty states now have Medicaid Managed Care involved in their long term care systems. The stated intent was to have better budget control and increased services to the growing boomer population that will double to 84 million by 2050 the 85+ population will triple to 15 million by 2040.
Medicaid is the primary payer for long term care services with Medicare only covering brief stays in long term care hospitals and skilled nursing home facilities. An important consideration is that nursing home care is considered an entitlement while home and community based services are not. Florida has maintained a cap on home and community based slots at 62,500 annually with CMS approval. This is why Florida is allowed to maintain a wait list for community-based services. In fact, Florida has one of the longest wait lists in the country as the state has successfully ratcheted down the institutional rate in Florida from 54% in 2014 to 43% in 2019.
Floridas Statewide Medicaid Managed Care Long
The SMMC Long-term Care Program is a nursing home diversion program meant to meet the needs of elderly or disabled Florida residents. Seniors who are eligible under Medicaid and require long-term care can receive assistance in their homes, in the community, or in assisted living spaces. Different regions within Florida have different Managed Health Care Organizations that provide services to eligible residents.
A senior who requires care and is eligible will select a plan from one of the providers in the geographical region. The provider will then be responsible for the participants long-term care needs. The ideal plan will provide the patient with the necessary treatment in the least restrictive environment appropriate for the recipient for example, living at home rather than living in an assisted-living facility where medically appropriate. Family members can even be hired and compensated for providing services for their eligible elderly family members.
Recommended Reading: Bariatric Surgeons That Accept Medicaid In Louisiana
Plan For Your Medicaid Eligibility
A dedicated West Palm Beach Medicaid planning attorney can help you and your family plan appropriately to maximize your chances to qualify for Medicaid and other needs-based governmental programs. If you are in need of an experienced and effective Florida Medicaid planning and elder law attorney, contact the West Palm Beach trust and estates attorneys Shalloway & Shalloway at 561-686-6200.
Helping 35 Million Floridians
In Florida, MCOs are responsible for program administration, including network management, claims payment, care coordination, and utilization management.
Since their launch in the state, MCOs have helped to:
- Double the amount of primary care providers in each network
- Expand access to after-hours care
- Improve transportation to ensure members get to appointments on time 10
In 2019, 1 in 9 adults, 3 in 7 children, and 1 in 3 individuals with disabilities were covered by Florida Medicaid.4
nursing home residents covered by Florida Medicaid4
You May Like: Medicaid Office In Corpus Christi
Florida Termination And Sanction Lists
Exclusion actions in Florida, unlike other states that closely mirror federal law, is founded upon a complex set of legal authorities that are captured in multiple statutes. Checking Florida exclusion lists can be equally daunting. There are actually two lists that need to be reviewed. Florida maintains lists of both providers who have been financially sanctioned by the state as well as provides who have been terminated for cause from participation in Floridas Medicaid programs.
The Sanctioned List contains the name, address and license number of persons, providers or entities sanctioned by the agency. In some circumstances, the agency has discretion to, and in others must, impose a sanction against a person, provider or entity, for failure to comply with Medicaid laws, rules or policies. Sanctions may vary significantly, depending on the nature and seriousness of the violation. By way of example, sanctions may include, but are not limited to, corrective actions such as education or selfaudits, monetary penalties , suspensions and terminations.
The Terminated List contains the name, address and license number of persons, providers or entities which are terminated for cause from participation in the Medicaid program. Such terminations are imposed by the agency under its statutory and/or regulatory authority, and are commonly referred to, and known as, for cause or with cause terminations. .
