About Humana Healthy Horizons In Ohio
Nationally, we serve Medicaid members through:
- Medicaid Managed Care
Humana is the brand name for plans, products and services provided by one or more of the subsidiaries and affiliate companies of Humana Inc. . Plans, products, and services are solely and only provided by one or more Humana Entities specified on the plan, product, or service contract, not Humana Inc. Not all plans, products, and services are available in each state.
Medical Plans
Humana group medical plans are offered by Humana Medical Plan, Inc., Humana Employers Health Plan of Georgia, Inc., Humana Health Plan, Inc., Humana Health Benefit Plan of Louisiana, Inc., Humana Health Plan of Ohio, Inc., Humana Health Plans of Puerto Rico, Inc. License # 00235-0008, Humana Wisconsin Health Organization Insurance Corporation, or Humana Health Plan of Texas, Inc., or insured by Humana Health Insurance Company of Florida, Inc., Humana Health Plan, Inc., Humana Health Benefit Plan of Louisiana, Inc., Humana Insurance Company, Humana Insurance Company of Kentucky, Humana Insurance of Puerto Rico, Inc. License # 00187-0009, or administered by Humana Insurance Company or Humana Health Plan, Inc. For Arizona residents, plans are offered by Humana Health Plan, Inc. or insured by Humana Insurance Company. Administered by Humana Insurance Company.
Go365® is not an insurance product. Not available with all Humana health plans.
Individual Dental and Vision Plans
Group Dental and Vision Plans
Life Insurance Plans
Enhanced Maternal And Reproductive Care
The Ohio Department of Medicaid’s Enhanced Maternal and Reproductive Care File Specifications
Purpose/Intent:
ODM and its Managed Care Plans are focused on improving birth outcomes, reducing infant mortality, and optimizing health outcomes for women and their infants. Early identification of women with a history of poor birth outcomes, allows MCPs to more timely connect women to needed services and supports and is one way of reducing the probability of future poor outcomes. To aid in this process, ODM has partnered with ODH to provide MCPs with an Enhanced Maternal Care File that links vital statistics birth certificate data to historical Medicaid claims data.
The purpose of the EMCF is to identify women of reproductive age who are at high risk of poor birth outcomes and would benefit from enhanced maternal care services as outlined in the attachment.
The primary goal in using the EMCF, is to identify high-risk women and link them to the services and supports needed to prevent future poor outcomes. MCPs should use the EMCF in conjunction with other information sources to timely identify high risk women in need of EMCS. The file is not an exhaustive list of all women who are high risk. It is very important to use all of the data sources available to you.
Examples of information available to use in conjunction with the EMCF:
ECMF Location
Medicaid Recipient ID – Character, length 12
Risk Indicator – Character, length 5
Risk Indicators
Examples
Wellhop For Mom & Baby
Connect with other expectant moms. Get support and information during your pregnancy and after you deliver. This program is part of your health plan and there is no extra cost to you.
Heres how it works:
- Join video conversations every other week with women who have similar due dates and a group leader.
- Chat and share experiences with moms from your group on the Wellhop app or website.
- Visit the Wellhop library. Youll find articles, videos and more.
-
PDF 4.58MB – Last Updated: 04/20/2021
Don’t Miss: Can I Change Medicaid Plan
Medicaid State Plan Services
Administered by the Ohio Department of Medicaid, Ohios Medicaid State Plan services cover a wide range of needs, including doctor visits, prescriptions, medical equipment at home, dental and vision services, pregnancy care, and mental health services.
Visit the Medicaid.Ohio.gov for more information about the kinds of services, who can get services, or how to apply for Medicaid State Plan services.
Managed Care Policy Guidance
ODM policy guidance for managed care organizations regarding: behavioral health, pharmacy, dental, hospital services, long term care, provider enrollment, laboratory services, substance use disorder treatment, file specifications, EPSDT, EVV, MyCare Ohio, hospice, medical necessity and prior authorization limitations, episodes of care, and more.
2022
Recommended Reading: Family Doctors In Charleston Wv That Accept Medicaid
How To Choose Caresource
Medicaid health care coverage is available for eligible Ohioans with low income, pregnant women, infants and children, older adults and individuals with disabilities.
| Choose CareSource |
|---|
| When you apply for Ohio Medicaid, you can choose CareSource as your managed care plan. Whether you apply online, by mail, over the phone or at your local Department of Job and Family Services , tell them you want to choose CareSource. |
| Switch to CareSource |
|---|
| If you were assigned to another managed care plan and want to switch to CareSource, call the Ohio Medicaid hotline, complete a change request within 90 days and tell them you want to switch to CareSource. If you have been on your plan more than 90 days, you can switch to CareSource during your next open enrollment period. |
How Do I Track My Provider Enrollment Applications
After you have entered your basic demographic information, the web-based system will issue you an Application Tracking Number . You should record this ATN immediately, because it will serve as your secure key to return to your application or to track it through the enrollment process.Once an application has been submitted, you can go to the Medicaid Provider Portal to check the status. Select the enrollment tracking search link.Once a provider is enrolled, they will be sent an email confirmation. This will be sent to the email that was provided during the application process.
Don’t Miss: Medicaid Cost Sharing With Medicare
Health Care With Heart
There is a reason more Ohioans choose CareSource for their Medicaid plan than all other plans combined. Its because CareSource is more than just quality health care. We care about you and your familys health and wellbeing. CareSource members get access to a large provider network, reward programs like Kids First and Babies First®, free rides to health care appointments, pharmacies and more. Plus, we never charge a copay for any medical or behavioral health service!
Choose CareSource for your Ohio Medicaid health care plan and join over 1.2 million members who trust us with their health and well-being.
Previous Procurement Phases: Request For Applications And Requests For Information
We begin by first considering feedback and suggestions from individuals and providers when making decisions about how to evolve the Medicaid managed care program in Ohio. The feedback received through our first Request for Information informed development of RFI #2, outlining our vision for the next generation of Ohio’s Medicaid managed care program. The second RFI sought input from providers, associations, advocacy groups, data and information technology vendors, and managed care organizations. The response period for both RFI #1 and RFI #2 closed on Tuesday, March 3, 2020.
This feedback informed the program design reflected in Ohio Medicaids next generation program structure and procurement processes.
Recommended Reading: Does Anthem Medicaid Cover Dental
How Ohio Grades Medicaid Managed Care Plans
The 2019 Ohio Department of Medicaid Managed Care Plans Report Card is a comparison of each plans performance across five reporting categories.
The report card serves as a side-by-side comparison of plan performance for consumers specifically addressing areas of interest to consumers in an easy to read, user-friendly format.
Information used for this report is collected from the managed care plans and their members and was reviewed for accuracy by independent organizations. Additionally, 2019 HEDIS® and 2019 CAHPS® data is used for this report. The yearly report cards create transparency for people choosing a Medicaid managed care plan.
Medicaid: Managed Care Plans
What is a managed care plan?
A managed care plan is a health insurance company the Ohio Department of Medicaid pays to provide health care services to some people. In Ohio, most people who have Medicaid must join a managed care plan to receive their health care. Ohios five managed care plans are: Buckeye Health Plan, CareSource, Molina Healthcare, Paramount Advantage and United Healthcare. If you have a managed care plan, you should receive a managed care card in the mail.
Some people in Ohio are in a special managed care program called MyCare Ohio, which is supposed to coordinate both Medicare and Medicaid benefits. The MyCare Ohio plans include: Aetna, Buckeye, CareSource, Molina and United Healthcare. This factsheet does not discuss MyCare Ohio plans.
What services do managed care plans provide?
Managed care plans must provide the same services as traditional Medicaid. However, a managed care plan may have different rules for deciding whether you can get a service. They might also make you get approval ahead of time before you can get a service. Some managed care plans offer optional benefits that are not included in traditional Medicaid. When you enroll in a managed care plan, you should receive a member booklet with information about the benefits. Your doctor or other medical provider should also be able to help you find out these limits and how to request authorization for your medical services.
How do I enroll in and choose a managed care plan?
Also Check: What Diabetic Supplies Are Covered By Medicaid
How Does Caresource Rank
CareSource is tied for first place in quality on the Ohio Department of Medicaids 2019 Managed Care Plans Report Card. The report card shares aggregated results of Managed Care Program sponsored member surveys for the 2019 period. CareSource was one of two plans to receive 18 stars across five different categories.
Using information collected from the managed care plans and their members, CareSource earned five stars in the Womens Health category, measuring breast cancer, chlamydia and cervical cancer screenings, as well as perinatal and post-partum care. CareSource received four stars in the Doctors Communication and Service category, measuring how happy members are with their physicians and how members collaborate with their doctors in decisions about their care.
Ranking high in quality demonstrates how CareSource puts our members first, said Steve Ringel, CareSource Ohio Market President. As a leader in quality, CareSource is proud to bring value-based care to our members and all Medicaid enrollees.
CareSource provides Medicaid coverage to more than 1.3 million Ohioans, making it the largest provider in Ohio and among the largest in the U.S.
Next Generation Of Ohio Medicaid Managed Care

Learn about the future Ohio Medicaid Managed Care program
You May Like: What Does Anthem Medicaid Cover
Medicaid Managed Care Plans
People accessing services through a Home and Community-based Services Waiver, like DODD’s Level One, Individual Options, or Self-Empowered Life Funding waivers, can enroll in a Medicaid managed care plan, which offers benefits like
- one permanent card, rather than a new paper card each month,
- more health care providers in your network and help finding health care providers,
- a dedicated toll-free number for questions and 24-hour nurse advice line,
- health and wellness programs,
Prior Authorization And Notification Resources
- Ohio Department of Medicaid Emergency Provider Agreement Changes
- The ODM Provider FAQs has specific information on Ohios changes:
- Prior authorization requirements resume for services rendered July 1, 2020 and later. Providers must submit prior authorization requests in accordance with UnitedHealthcare policies and procedures.
- Timely filing for claims extended to 365 calendar days from the date of service.
- Access to telehealth services is expanded.
- For the pharmacy benefit, there are changes to prescription guidance, refill limits and prior authorization requirements.
Monday-Friday, 8 a.m. 5 p.m.
Postal Mailing Address
9200 Worthington Road, 3rd FloorWesterville, OH 43082
Attn: Complaint and Appeals DepartmentP.O. Box 31364Salt Lake City, UT 84131Fax: 994-1082
Attn: Complaint and Appeals DepartmentP.O. Box 31364Salt Lake City, UT 84131Fax: 994-1082
UHC Connected For MyCare Ohio Appeals Mailing Address
Part C Appeals or Grievances:UnitedHealthcare Community PlanAttn: Complaint and Appeals DepartmentP.O. Box 31364Salt Lake City, UT 84131Fax: 994-1082
Attn: Complaint and Appeals DepartmentP.O. Box 31364Salt Lake City, UT 84131Fax: 994-1082
Attn: Part D Standard AppealsP.O. Box 6103
For Credentialing and Attestation updates, contact the National Credentialing Center at 1-877-842-3210.
Need to make a change to your provider or facility directory information?
Behavioral Health Providers
The Centers for Medicare & Medicaid Services established the Medicaid Managed Care Rule to:
You May Like: Apply For Medicaid Rochester Ny
Big Step Forward For Ohio Medicaid But More To Come
On April 9, Ohio Department of Medicaid Director Maureen Corcoran made a long-awaited announcement revealing the names of the Medicaid managed-care insurance companies that would get to share in a 20 billion dollar, five-year contract to provide health care services for 3 million Ohioans.
Director Corcoran said repeatedly that she wanted to focus on people and not just the business of managed care.
The announcement had been delayed likely because of a lawsuit that Ohio Attorney General David Yost had filed against Centene accusing the company of a conspiracy to wrongfully and unlawfully obtain tens of millions of dollars in Medicaid payments. Its not clear how this situation will resolve itself, but it seems likely that Centene has a strong incentive to settle this case.
The announcement of the winning plans was the culmination of a process that began a little more than two years ago. In fact, Governor Mike DeWine signaled early that he wanted to re-procure Ohios Medicaid managed-care contracts. Director Corcoran said repeatedly that she wanted to focus on people and not just the business of managed care.
The Next Generation Of Ohios Medicaid Managed Care Program
In response to Ohio Governor DeWines call to ensure Ohioans get the best value in providing quality care, ODM embarked on an effort to procure new managed care contracts to support a future program with a mission to “focus on the individual rather than the business of managed care.”
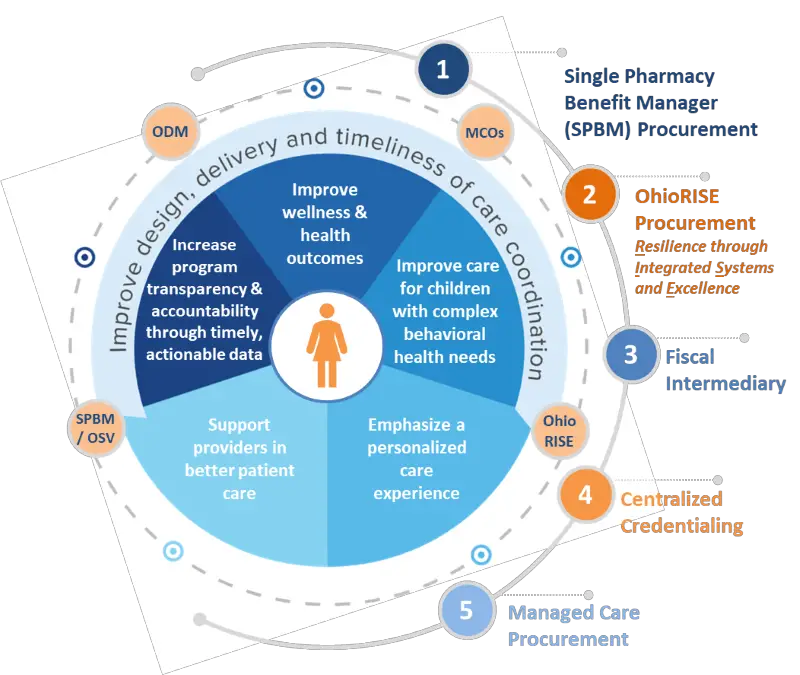
ODM has designed its future Medicaid managed care program to achieve the following goals:
- Improve wellness and health outcomes
- Emphasize a personalized care experience
- Support providers in better patient care
- Improve care for children and adults with complex needs
- Increase program transparency and accountability
Many of these goals will be advanced through ODMs population health approach, which is designed to address health inequities and disparities and achieve optimal outcomes for the holistic well-being of individuals receiving Medicaid.
For additional details about the future Ohio Medicaid managed care program and procurement, visit managedcare.medicaid.ohio.gov.
Recommended Reading: Is My Medicaid Still Active
Ohio Takes Steps To Refocus Medicaid Managed Care Program
The Ohio Department of Medicaid has announced several new steps in the evolution of its managed care program, including selecting six managed care organizations that will operate statewide. New features include a single pharmacy benefits manager, centralized credentialing, and a specialized managed care program for children with complex needs. The newly designed program is targeted for launch in January 2022.
The six MCOs are The six managed care organizations announced April 9 are UnitedHealthcare Community Plan of Ohio Inc., Humana Health Plan of Ohio Inc., Molina Healthcare of Ohio Inc. AmeriHealth Caritas Ohio Inc. Anthem Blue Cross and Blue Shield, and CareSource Ohio Inc. They will provide services for more than 3 million members and thousands of medical providers in Ohios $20 billion managed care program.
ODMs next-generation program emphasizes plan coordination with OhioRISE , which addresses care for children with complex behavioral needs and the single pharmacy benefit manager, which is designed to ensure more accountability and transparency in Medicaids pharmacy program. Initiatives such as centralized credentialing and fiscal intermediary are designed to streamline administrative functions and reduce duplicative processes for providers.
Ohio Medicaids procurement also required respondents provide more flexibility in establishing alternative payment models with providers who focus on patient care and improve outcomes.
Unitedhealthcare Connected For Mycare Ohio
UnitedHealthcare Connected® for MyCare Ohio is a health plan that contracts with both Medicare and Ohio Medicaid to provide benefits of both programs to enrollees. If you have any problem reading or understanding this or any other UnitedHealthcare Connected® for MyCare Ohio information, please contact our Member Services at from 7 a.m. to 8 p.m. Monday through Friday for help at no cost to you.
Si tiene problemas para leer o comprender esta o cualquier otra documentación de UnitedHealthcare Connected® de MyCare Ohio , comuníquese con nuestro Departamento de Servicio al Cliente para obtener información adicional sin costo para usted al de lunes a viernes de 7 a.m. a 8 p.m. .
Also Check: Florida Medicaid Primary Care Providers
We Know Youre Going To Have Questions
Ohio Medicaids new approach to managed care is based on extensive feedback we received from providers, patients, and other key stakeholders about the way the system was working for them.
It is designed to make access to care simpler, more personal, and more effective. But, we know youll still have questions. Feel free to contact us at with suggestions, questions and guidance on the changes ahead.
For information related to the next generation of managed care, please visit managedcare.medicaid.ohio.gov.
Ohio Medicaid Members Update Contact Information

Exciting new changes are coming to Ohio Medicaids program in 2022, and we want to make sure all members receive information about actions they will need to take and information about the programs next generation services, supports, and managed care plans.
Ohio Medicaid members are encouraged to update the contact information below to make sure they do not miss any important updates. When an Ohio Medicaid member updates their contact information, it helps make sure that ODM can reach them to provide important updates about their Ohio Medicaid managed care plan and coverage.
- Name
- Mailing Address
- Phone Number
- Email Address
Ohio Medicaid members can update their contact information at any time by contacting their County Department of Job and Family Services . Ohio Medicaid members can also contact their CDJFS with questions about how to update their contact information. Ohio Medicaid members can find their CDJFS by viewing the County Directory at .
You May Like: Will I Lose My Medicaid If I Get Married
