Which Medicaid Plan Is Best In Florida
Each Medicaid plan in Florida comes with the same core benefits which are listed here. You can also compare the performance data for the various plans in your area by using what is known as the Medicaid Health Plan Report Card. You will also have to consider things like the types of services that might be needed along with how many doctor visits that will be necessary, the plan that is accepted by your doctors, the types of doctors you will need, and what extra benefits will meet your needs.
How To Apply / Learn More
When the applicant senior is not in a nursing home, the application process starts with a call to the Florida seniors local Area Agency on Aging. One can also call the Elder Helpline. Find the number by county here. Callers should request a screening for home and community based services. The representative schedules a time for the phone screening with the primary caregiver or closest family member, usually one to two weeks out. The screening interview typically lasts 30 to 40 minutes. The interview covers basic demographic information for the applicant as well as his/her income and assets. The interview mostly asks about the elders needs for care, including his/her ability to perform Activities of Daily Living.
Following the interview, the elder receives a prioritization decision. This letter indicates whether services can begin immediately or whether the senior needs to be waitlisted. If the senior is prioritized for home or community supports to start immediately, he/she must apply to the Department of Children and Family Services through the ACCESS System for their formal Medicaid approval.
To learn more about SMMC LTC, .
Like Floridas HCBS Medicaid Waivers that served this population before the creation of this program, SMMC LTC has a limit on the number of persons who can receive assistance at the same time. Waiting lists for some services likely exist in areas throughout the state.
Who Is Eligible For Medicaid In Florida
The following people may qualify for Florida Medicaid if they meet certain financialrequirements:
- Infants and children under the age of 21
- People who are aged 65 or older
- People who are blind or expected to be disabled for at least a year
- Recipients of Supplemental Security Income
- People who need nursing home care or home and community-based care
- People who are on Medicare
- Aliens and refugees under a special assistance program
- Individuals who are medically needy
Read Also: Does Medicaid Cover Cord Blood Banking
Floridas Requirements For Medicaid Qualification
In order to get Medicaid in Florida, you have to meet certain eligibility requirements. You have to be a certain type of patient for one thing. These include:
- Pregnant women
- Parents or relatives who are caretakers
- Families who might have lost Medicaid because of an increase in income or alimony
- Florida residents who receive SSI through the Social Security Administration
- Patients who are disabled or over the age of 65
- Children under 21
- Those who are eligible to receive Temporary Cash Assistance
- People under age 26 who were in a foster home
- People in nursing homes or those who receive community or home-based care.
You also have to be a Florida resident who has a valid social security number and a citizen of the U.S.
If Denied Request An Appeal

If you have received notice that your Medicaid has been denied, you have 90 days from the date of the notice to ask for a Fair Hearing. A Fair Hearing is the process that allows you to dispute the denial decision if you believe it was decided unfairly. Instructions on how to ask for a Fair Hearing should be included with the notice of denial that DCF sends to you. If you are currently on Medicaid and are informed that you are no longer eligible, you have only ten days to appeal in order to keep your Medicaid open pending the outcome of your appeal.
You may also complete a public assistance fair hearing form on this Florida Department of Children and Families webpage:
It can take several weeks for your Fair Hearing request to be processed. Once it is processed, you will receive a letter telling you the date, time, and location of your Fair Hearing.
Don’t Miss: How To Apply For Medicaid In Delaware
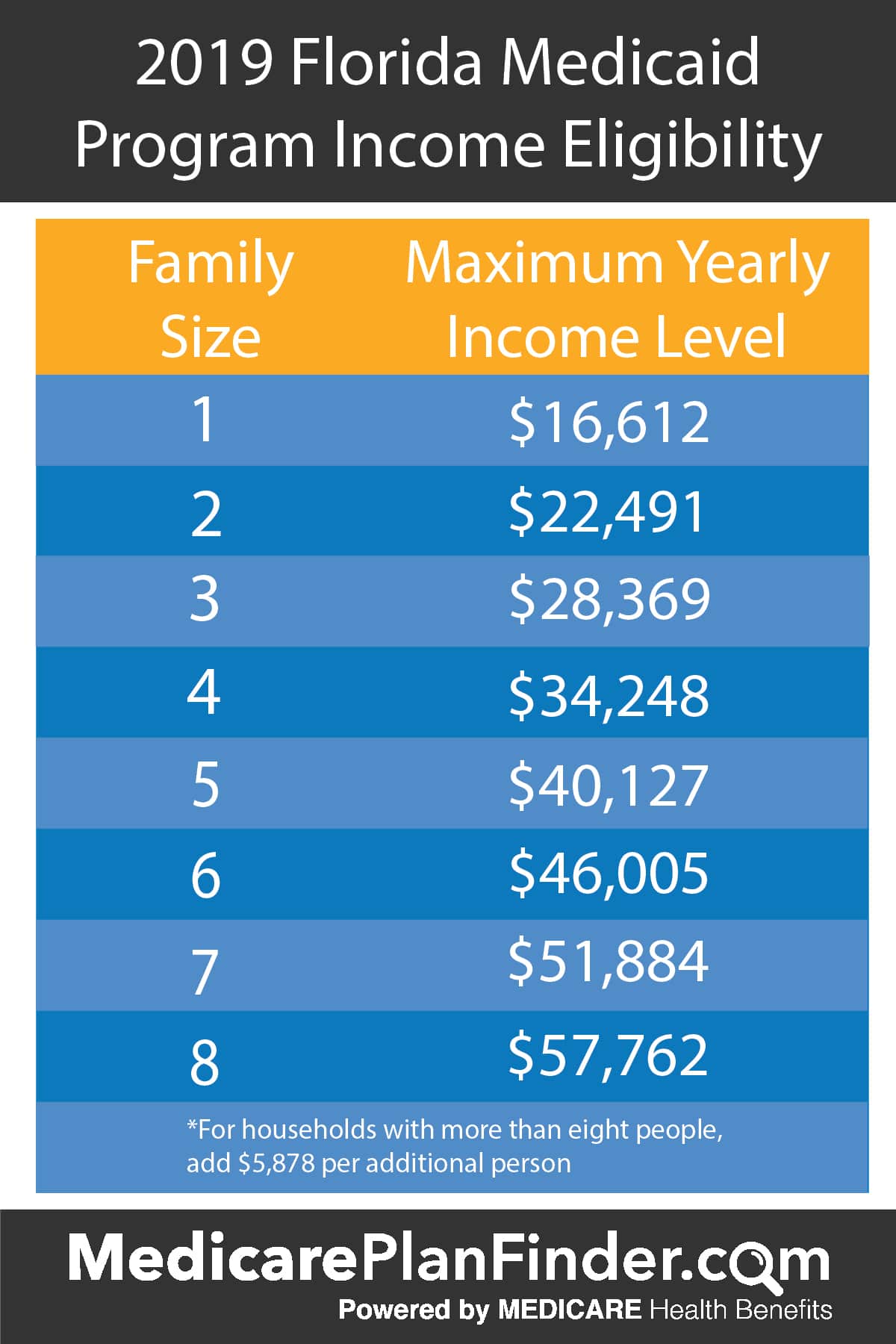
Florida Medicaid Income Limit
The FL Medicaid eligibility income limit charts are divided by groups.
For example, the first chart is focused on income limits for children who qualify for Medicaid.
Similarly, the second chart below focuses on the Medicaid income limits for adults in Florida who qualify for Medicaid.
Florida Medicaid Income Limit for Children
Below is the income limit for children by age category. Find the age category your child falls into and you will see the income limit by household size.
| Florida Medicaid Income Limit Children |
| Children Medicaid Ages 0-1 |
| N/A |
How to Read the Florida Medicaid Income Limits Charts Above
You cannot have an income higher than the Federal Poverty Level percentage described for your group to be eligible for Medicaid.
Similarly, when you identify the income group that applies to you, the income limit you see refers to the maximum level of income you can earn to qualify for benefits.
For example, if you are pregnant, to qualify for Medicaid, you cannot have an income higher than 191% of the Federal Poverty Level which for a family of two is $33,272 as shown in the chart above.
How to Apply for Medicaid in Florida
There are 3 ways you can apply for Medicaid in Florida.
Eligibility For Medicaid For Low
- Applicant must be a U.S citizen or a qualified alien
- Applicants must be residents of Florida
- Applicant must be able to provide Social Security Number
- Applicants must be able to provide proof of their identity
- Applicants must cooperate with Child Support Enforcement
- Applicants must provide a proof of their earned income and assets should be
- Parents applying for Medicaid should have at least one child meeting all the eligibility criteria of Medicaid
- Resource limit for Medicaid is set at $2,000
- Family income should be below the TCA limit. You can see the complete TCA eligibility chart HERE.
- Relatives within specified degree of relationship can also receive benefits from Medicaid if they are caretakers of the eligible children.
- Applicants’ assets should be below the limit, which is $2,000
Individuals receiving Temporary Cash Assistance benefits will be eligible to receive Medicaid benefits if they qualify.
Although most factors in the eligibility criteria can be verified electronically but authorities can request a documents for manual verification.
Also Check: Is Neighborhood Health Plan Medicaid
Medicaid For Aged Or Disabled
Medicaid for low-income individuals who are either aged or disabled is called SSI-Related Medicaid.
Florida residents who are eligible for Supplemental Security Income are automatically eligible for Medicaid coverage from the Social Security Administration. There is no need to file a separate ACCESS Florida Application unless nursing home services are needed.
Individuals may apply for regular Medicaid coverage and other services using the online ACCESS Florida Application and submitting it electronically. If long-term care services in a nursing home or community setting are needed, the individual must check the box for HCBS/Waivers or Nursing Home on the Benefit Information screen. HCBS/Waiver programs provide in-home or assisted living services that help prevent institutionalization.
Medicare Savings Programs help Medicare beneficiaries with limited finances pay their Medicare premiums and in some instances, deductibles and co-payments. Medicare Buy-In provides different levels of assistance depending on the amount of an individual or coupleâs income. Individuals may apply for Medicare Buy-In coverage only by completing a Medicaid/Medicare Buy-In Application.
Print the form, complete it and mail or fax it to a local Customer Service Center.
When Applying For Medicaid In Florida: Divide And Conquer
As Florida elder care lawyers and Medicaid-planning attorneys, we try to do as much of the heavy lifting for you as possible. But there are certain required Medicaid-planning items that make sense for the client to handle since time is of the essence. For example locating previously-executed Will and Trust documents powers of attorney bank account information, retirement account, and brokerage account statements are tasks that just make logical sense for the client to retrieve, rather than the elder-law attorney.
However, once these items are obtained and presented to the elder law or Medicaid-planning attorney, all the heavy lifting is done on our end, including preparing all necessary documents, deploying Medicaid-qualification strategies, and filling out and following through with the Medicaid application until it is approved. We even provide you with detailed instructions on your obligations after you have been approved for Medicaid and what you need to do in order to maintain Medicaid eligibility.
When applying to the Home and Community Based Services Waiver program, there is an interview process. We can coach you through the Medicaid screening to improve your placement on the Medicaid waiver wait list.
Recommended Reading: How To Find Case Number For Medicaid
Learn How To Apply For Medicaid In Florida
UPDATE: In 2020, the requirements and application steps for obtaining Medicaid insurance have undergone no significant changes.
Where do you sign up for Medicaid in Florida? Filing Medicaid application forms is the first step in requesting Medicaid benefits in the Sunshine State. However, not everyone interested in obtaining state-sponsored medical assistance knows exactly where to apply for Medicaid. Continue below to learn about the following Medicaid application topics:
Florida Medicaid Application What To Expect When You File
Filling out the Florida Medicaid application is your first step to finding out if you meet Florida Medicaid qualifications.
In our Elder Law practice we concentrate in representing you in completing the forms required for funding of Assisted Living or Nursing Home care via Medicaid or Veterans Benefits, and making the changes necessary in your financial structure in order to qualify for that type of funding.
Just filling out the online form wont do this for you if you fail to meet the strict asset and income requirements. You can learn more about this process on our site so stay with us.
Read Also: What’s Better Medicare Or Medicaid
Provider Eligibility And Compliance
Responsible for ensuring the continued eligibility of enrolled providers through research and validation of providers who are excluded from participation in Medicare, Medicaid, or other federally-funded programs documenting justifications for exclusions from Florida Medicaid coordinating with Medicaid Program Integrity and the OGC regarding referrals for legal sanctions monitor provider background screening processes taking appropriate actions when providers have disqualifying offenses participate on the Clearinghouse Advisory Board coordinate with Medicare related to mismatches in provider data between PECOS and the MMIS coordinate requests for onsite reviews with the RPA Onsite Review Desk perform change of ownership reviews, including determining if there is any pending enforcement action by MPI or MFCU, verify accuracy of ownership disclosures, and identify any money owed by the seller or the buyer and participate in an interagency workgroup on provider license compliance.
Even If Youre Not Sure Fill Out The Medicaid Application

The Centers for Medicare & Medicaid Services advises you to complete a Medicaid application even if youre not sure you qualify. Remember that its better for you to apply for Medicaid and be turned down than not to apply at all. A caseworker will review your case to determine whether or not you qualify for Medicaid benefits. Your Medicaid eligibility can change from year to year, so you may want to complete a new Medicaid application each year, even if your application was previously turned down.
Read Also: Is Tenncare And Medicaid The Same Thing
Apply For Medicaid For Aged Or Disabled
Applying online: Individuals can apply for Medicaid electronically. All they have to do is to go to ACCESS Florida website and fill out the application forms there. The entire process can be completed online. You will automatically qualify for Medicaid if you are eligible for SSI. You can apply for SSI using this LINK. However, if you need nursing services, you will have to make sure that you are checking the box that asks for HCBS or Nursing Home on benefit information page. This program will provide services for assisted living so that individuals do not have to be institutionalized.
Applying through fax or mail: You can print application from ACCESS Florida website and mail or fax it to your local customer service center. You can find your nearest local customer service center by clicking here.
How Do I Find My Florida Medicaid Number
Your Florida Medicaid identification number is not listed on your gold card. Your Florida Medicaid number is kept in your Florida Medicaid file.
Any Medicaid provider can use your gold card or health plans membership card to check the Florida Medicaid file to find out if you are eligible for Florida Medicaid services.
You May Like: Medicaid Primary Care Physicians Arkansas
Medicaid For Pregnant Women
Pregnant women will be able to enjoy benefits through presumptive eligibility. Presumptive Eligibility for Pregnant Women provides Medicaid to pregnant women in emergency who may need instant parental care. Women with income less than 185% of federal poverty level can qualify to receive Medicaid through PEPW. Simplified Eligibility for Pregnant Women is another way to get qualified for full Medicaid cover. Pregnant women qualifying for PEPW can then apply for SEPW and get full coverage which would not be available with PEPW.
Eligibility For Medicaid Services
Recipient eligibility for Medicaid is determined by the:
- Department of Children and Families, Office of Economic Self Sufficiency – The Department of Children and Families determines eligibility for low-income children and family programs and the institutional care program.
- Social Security Administration – The Social Security Administration determines eligibility for the Supplemental Security Income program.
Each program has its own income and asset requirements.
Information about Medicaid eligibility criteria for the aged, blind and disabled, and children and family programs can be obtained from the Department of Children and Families Web site or the DCF region / circuit office closest to you.
You May Like: Emergency Clinics That Take Medicaid
Medicaid For The Aged Or Disabled
Any Florida resident who is eligible for Supplemental Security Income is also automatically eligible for Medicaid. There is no need for a separate ACCESS Florida application unless nursing home services are needed.
There are many SSI-Related Medicaid programs and coverage groups, each with different financial and disability requirements. For information on what coverage these programs provide and to find out which coverage group you fit into, read the Florida Department of Children and Families SSI-Related Medicaid Programs Fact Sheet, which you can find here:
Emergency Medical Assistance For Non
- Individual must have Medical Assistance basis of eligibility
- Individual must have a genuine medical emergency
- Individual must be a resident of Florida
Medical emergency purposes for EMA can include:
- Chronic medical condition which can place individual’s health in dangerous condition if left unattended
- Chronic medical condition which can cause impairment to the body if left unattended
- Chronic medical condition which can cause some body organs to dysfunction if left unattended
- Individual has a sudden onset of conditions that can result in acute symptoms
Don’t Miss: Medicaid Phone Number Denver Colorado
Followed By A Face To Face Meeting
This meeting can take place at your home, at the nursing home, or one of our offices located throughout the state and is an opportunity for you to meet a Medicaid Eligbility, Inc. representative in person. At this meeting, we will review the applicants finances in greater detail, including assets and income specifics, and accurately assess your familys overall financial situation.
Apply For Medicaid For Pregnant Women
You can apply for Medicaid for pregnant women in three different ways
- Presumptively Eligible Pregnant Women : This coverage is only available at local clinics and it is only temporary. However, when a pregnant woman qualifies for PEPW, her application is automatically sent to DCF, who will determine eligibility for ongoing Medicaid determination.
- Simplified Eligibility for Pregnant Women : Pregnant women can get full coverage by applying through one page application. You will be required to print application so that you can mail it to ACCESS. You can also fax or return the application in person at an ACCESS office. You can .
- ACCESS application: You can apply for Medicaid benefits through regular process. Regular Medicaid provides benefits for pregnant women. You can apply through THIS link.
- You can apply for Medicaid for Pregnant Women electronically or by using this link to request application by mail or fax.
Read Also: Medicaid Provider Id Number Lookup
Medicaid For Children Only
If families have income below the income limit for their children under the age of 19, they can apply for Medicaid benefits for their children. However, parents can only apply for Medicaid for their children when they are living with them. Caretakers can also apply for Medicaid benefits for children.
Children meeting the eligibility for Medicaid program can also apply for Child Health Check-up Program. Once a child enrolls in this program, he or she will receive regular health checkup along with dental screening and immunizations. Children enrolling in this program will also be able to receive other medical services necessary for proper child health.
Families receiving Medicaid benefits will stop receiving such benefits when their last child turns 18 years of age. For children between 18 and 21, Medicaid benefits are only limited to the child and not to the family.
A child born to a woman with Medicaid eligibility will automatically start receiving benefits under Medicaid for next thirteen months. The Presumptive Eligibility for Newborns begins from the date of birth.
