When To Contact Your State Medicaid Or Chip Agency
Issues to take to your state Medicaid or CHIP agency include:
- You didnt get an enrollment card and arent sure youre covered
- You cant find a doctor who accepts Medicaid or CHIP, or you cant get an appointment
- You want to know if a service or product is covered
- You have a life change that may affect if youre eligible for Medicaid or CHIP like getting a job that increases your income, your dependent reaching an age where they no longer qualify, or getting married or divorced.
FILLING PRESCRIPTIONS IF YOU DON’T HAVE A CARD: If you need to fill a prescription and havent received your enrollment card yet, check if your pharmacy accepts Medicaid, CHIP, or your health plan. If they do, take your eligibility letter and prescription to the pharmacy. Theyll try to fill it using the information in the letter.
If they dont have enough information, most pharmacies can give you enough medicine for 3 days. Call your Medicaid or CHIP agency or health plan for help getting the rest of your medicine.
If your pharmacy doesnt accept Medicaid, CHIP, or your health plan, call the number in your eligibility letter to find a pharmacy you can use. You can usually find this information on the state Medicaid or CHIP agency website too.
Choosing Your Managed Care Organization
Most people are automatically selected for Medicaid managed care coverage. Shortly after you enroll in Medicaid, you will get a letter asking you to choose a Medicaid MCO. Visit the websites below for each to learn more and find one that is right for you. If you dont choose a plan, we will choose one for you. You can change plans up to 90 days from your date of initial enrollment, or during our annual open enrollment period.
A helpful way to enroll in managed care is online through the Medicaid MCO Member Service Website. With help from the MCO Member Service, you can compare plans additional benefits and view plans provider networks. You may want to consider: what services you might need, which health plan is accepted by the doctors you use, which plan was found to meet the highest quality for your health care needs, and which extra benefits are most beneficial to you.
Once you are enrolled with an MCO, you will get a new card in the mail. MCOs send one permanent card when you enroll. Keep this card for as long as you are on the plan. If you need to replace your managed care ID card, please contact your MCO, or use their online member portal. The plan will also send you information on your doctors, health services, and the scope of coverage from your plan.
Choices You Have To Make And Tips For Choosing A Plan
Illinois Client Enrollment Services will mail you an enrollment packet. This packet will include a letter saying by what date you need to choose a health plan. If you do not choose a plan by that date, a health plan and Primary Care Provider will be chosen for you. Once you have picked a PCP and health plan, you will get information about your health plan and your health plan member ID card in the mail. You will use your health plan member ID card to get healthcare services.
Here are some questions to ask yourself that may help you decide which health plan and PCP are right for you.
- Is there a doctor I already like?
- What health plans does my doctor work with?
- Does someone in my family have special needs?
- How far do I want to travel to see my doctor?
- Do I need a doctor who speaks a certain language?
To research the plans and decide which is right for you, go to EnrollHFS.Illinois.Gov for more information. You can also call the plans member services line to learn more about each plan.
For more help choosing a plan and finding a doctor, you can call Illinois Client Enrollment Services at 912-8880 or go online to EnrollHFS.Illinois.Gov.
Read Also: Healthplus Medicaid Provider Phone Number
Q How Can I Find Out If I Can Get Medicaid
A. You can find out if you qualify for Medicaid or other medical assistance and social service programs by speaking with a representative at your local State Service Center. Call Medicaid Customer Relations at 1-800-372-2022 or 255-9500 to be directed to the appropriate office where someone can help you.
Q Who Qualifies For Medicaid

A. Citizenship and Residency – To obtain full Medicaid benefits in Delaware, you must be a Delaware resident and either a U.S. citizen or a legally residing noncitizen. Full coverage for noncitizens which include DACA recipients is dependent on the availability of state funding. However, noncitizens can qualify for coverage for emergencies and labor & delivery services if income requirements are met.
Income Level – Qualifying for Medicaid is also based on need. Household income must be under certain limits as defined by the Federal Poverty Level and is based on family size. For Long Term Care programs, financial resources must also be under a certain amount. There are also specific programs for individuals who meet certain medical or disability tests, or who qualify due to age or pregnancy. To find out more about different Medicaid and other medical assistance programs, visit DMMA Programs & Services.
Recommended Reading: Day Care Covered By Medicaid
Nc Medicaid Managed Care Started July 1 2021
NC Medicaid Managed Care health plans are now active. This means that you will now get care through your health plan. If you have questions about benefits and coverage, call your health plan. You can find the number on your new Medicaid ID card or visit View health plans.
You can also contact the NC Medicaid Ombudsman if you have questions or problems your health plan or provider could not answer. Call 1-877-201-3750 or visit ncmedicaidombudsman.org.
Meetings and events
You can schedule rides to medical appointments. Learn more about transportation services.
Get the free mobile app
To get the app, search for NC Medicaid Managed Care on or the App Store.
Use the app to find and view primary care providers and health plans for you and your family. Learn more about the free mobile app at Get answers.
You May Like: Family Doctors In Charleston Wv That Accept Medicaid
Get Important News & Updates
Sign up for email and/or text notices of Medicaid and other FSSA news, reminders, and other important information. When registering your email, check the category on the drop-down list to receive notices of Medicaid updates check other areas of interest on the drop-down list to receive notices for other types of FSSA updates.
Don’t Miss: Dental Care That Accepts Medicaid
I Would Like To Change My Health Or Dental Plan
Change Health or Dental Plans Online
Log in to the FL Medicaid Member Portal to change your Health or Dental Plan. We will walk you through the process of changing your plan.
Why should you sign up for a FL Medicaid Member Portal account?
- You can check your Medicaid eligibility and enrollment status
- View and update your address
- Request help using secure messaging
- Enroll in a plan or change plans
- File complaint and see what is happening with your complaint
- Go paperless. Choose to only get letters from Medicaid electronically
- Receive email or text message alerts
Other Ways to Change Your Health or Dental Plan
If you are unable to change Health or Dental Plans online at this time, there are several other options available to you.
Recommended Reading: Does Medicaid Cover Glasses In Texas
**which Health Plan Is Available In My County
Not all plans are available in all counties, here is a map of all the health plans by county. **Washtenaw County is part of Region 9 which also includes Livingston, Jackson, Washtenaw, Hillsdale, Lenawee and Monroe counties. Your choices include Aetna Better Health, Blue Cross Complete, McLaren, Meridian, Molina and UnitedHealthcare. Here is a helpful document for choosing your plan Washtenaw County or Livingston County.
Also Check: Does Medicaid Cover Gym Memberships
Choosing A Managed Care Health Plan And Doctor
A health plan is the group of doctors, hospitals, and other providers who work together to coordinate all of your care. A health plan is also called a Managed Care Organization . All of your doctors, hospitals, and providers must be part of the same Health Plan, or MCO.
American Disabilities Act Notice
In accordance with the requirements of the federal Americans with Disabilities Act of 1990 and Section 504 of the Rehabilitation Act of 1973 , UnitedHealthcare Insurance Company provides full and equal access to covered services and does not discriminate against qualified individuals with disabilities on the basis of disability in its services, programs, or activities.
Read Also: Dentist In Meridian Ms That Accept Medicaid
Also Check: Inpatient Rehabs That Take Medicaid
What If Im Eligible For Medicaid But Want To Buy An Insurance Plan In The Marketplace Instead
The income guidelines for an insurance plan through the Marketplace start beyond the income guidelines for Medicaid, so the short answer is no. When you go to the Marketplace website, you will be able to check to see what is available to you. If your estimated income is within Medicaid eligibility, the website will direct you to the Medicaid application process.
When the Affordable Care Act was put into effect, the parameters for Medicaid eligibility were expanded for the sole purpose of making more people eligible for Medicaid and avoiding the need to pay for health insurance.
The initial check is based on the state you live in and the number of people in your household. In short, your household includes the head of the house and all those claimed as tax dependents due to age or disability. Accurately counting the size of your household is crucial in the application process.
Once you enter your household size and state information, you will be provided with a breakdown of what you may qualify for based on your income. For example, if you have a household of 5 people, and you live in Ohio, here is your eligibility breakdown:
| Estimated Income | |
|---|---|
| Youre eligible for a health plan through the Marketplace that provides lower monthly premiums. | |
| More than $113,640 | You are not eligible for any savings programs, but you can still buy health insurance through the marketplace at regular price. |
Q What Medical Services Does Medicaid Cover

A. The Delaware Medicaid program pays for many medical services to keep you healthy and to treat you when you are sick. The major services are:
- Prescriptions
- Inpatient and Outpatient hospital care
- Lab tests
- Dental care
Covered services for the Delaware Healthy Children Program are listed on the DHCP Benefits page.
Read Also: Does Medicaid Pay For Funeral Expenses
Don’t Forget To Renew Each Year
Recertify your Medicaid coverage every 12 months to keep your benefits. Visit the Florida Department of Children and Families to sign up for email reminders.
ENROLLING AND CHOOSING SUNSHINE HEALTH IS EASY
1. Apply for Medicaid. If you are eligible for Florida Medicaid, the Agency for Health Care Administration will send you a letter asking you to choose a plan. Visit the Florida Department of Children and Families website to apply for Florida Medicaid. 2. Receive a letter to choose a plan. 3. Choose a plan. 4. Call a Choice Counselor toll-free at 1-877-711-3662 or visit the Statewide Medicaid Managed Care page online. 5. Receive a welcome packet from your plan.
If You Are Choosing A Health Plan For The First Time:
To keep your primary care provider , choose a health plan your PCP is in. Use these questions to help you choose the best health plan for you:
- Do you want to keep your current provider? Or do you want a new one?
- Does the health plan have the providers, hospitals and specialists you use? To find out, go to Find a provider.
- Does anyone in your family have special health needs?
- What added services does the health plan have? To view each health plans added services, go to View health plans.
Recommended Reading: Does Medicaid Cover Dental Bridges
Do The Worst Case Scenario Math
Some employers offer software that allows workers to upload their claims history from the past year and uses that to recommend a health care plan. I wish that were available to everyone. The closest Ive seen is HealthSherpa, which helps people winnow their ACA marketplace options based on how they generally use health care.
The plan that may have been a good fit for your past claims, though, may not be the best choice for the future especially if you become seriously ill or injured. To protect against worst-case scenarios, you also need to consider the out-of-pocket limits. These are the maximum amounts youd have to pay in addition to your premiums. Out-of-pocket limits typically range from $2,000 to $6,000, although there may be different maximums for in-network versus out-of-network costs, and not all policies have these caps.
Some plans give you only a small break in premiums while exposing you to much larger potential costs, says Alan Silver, senior director of benefits delivery and administration at Willis Towers Watson, a benefits consultant.
Before signing up for any policy, add your annual premiums to the out-of-pocket limit to see the potential costs you could face. If the total scares you, look for a plan with a limit that lets you sleep at night.
This article was written by NerdWallet and was originally published by The Associated Press.
We Know Youre Going To Have Questions
Ohio Medicaids new approach to managed care is based on extensive feedback we received from providers, patients, and other key stakeholders about the way the system was working for them.
It is designed to make access to care simpler, more personal, and more effective. But, we know youll still have questions. Feel free to contact us at with suggestions, questions and guidance on the changes ahead.
For information related to the next generation of managed care, please visit managedcare.medicaid.ohio.gov.
Recommended Reading: Primary Care Doctors In Hammond La That Take Medicaid
How To Choose A Health Plan
When picking a plan, think about the following:
- Are doctors you already use and like covered by the plan?
- How is the plan rated on issues that are important to you and your family?
- What value-added services are available through the plan?
We also provide tools to help you choose the best plan for you and your family.
Q How Long Will My Medicaid Benefits Remain Active
A. Medicaid is based on month to month eligibility. However, your benefits are redetermined on a yearly basis by DMMA to confirm whether you still remain eligible for the program you are receiving. Certain Medicaid programs require you to report changes in your situation within 10 days of the change. One example of a change that must be reported is new employment.
Also Check: How Can I Check The Status Of My Medicaid
Find And View Providers And Health Plans
This website has new tools to help you find and view primary care providers and health plans.
Medicaid and NC Health Choice Provider and Health Plan Lookup ToolYou can use the Medicaid and NC Health Choice Provider and Health Plan Lookup Tool to find a PCP. Our new provider search will help you find the best PCP for you and your family.
To search for a provider, go to Find a provider.
Health Care Option GuideYou can use the Health Care Option Guide to view health plans. It will help you choose the best health plan to meet your health care needs.
Read Also: How To Apply For Medicaid In Houston
Choosing The Right Health Plan For You
Choosing a health plan is a personal decision. While we are confident that all health plans are able to meet your needs, you may want to consider the following points when choosing a plan:
Provider Networks: Each health plan includes a group of health care providers . This is called a “network” of providers. For most health care services, you must use the health care providers who are in your health plan.
Primary or Specialty Medical Providers: When you are enrolled in a managed care program, you will choose a Primary Medical Provider, often called a PMP. Your PMP will work with you and be your primary contact when making medical decisions. Your doctor will also make referrals and help you with prior authorizations for services that are not always covered by Medicaid.
If you already have a doctor or other primary or specialty medical provider, when choosing your health plan, you will want to make sure that provider is part of the health plan’s network. If you do not have one, your health plan will work with you to identify one. To find out if your doctor or other primary medical provider is part of the health plan’s network, you should call the help line listed below.
Locations: You may want to make sure that the plan you choose has providers that are conveniently located for you. This may mean they are near your work or your child’s school, or they may be on a bus line.
Read Also: Michigan Medicaid Waiver Assisted Living
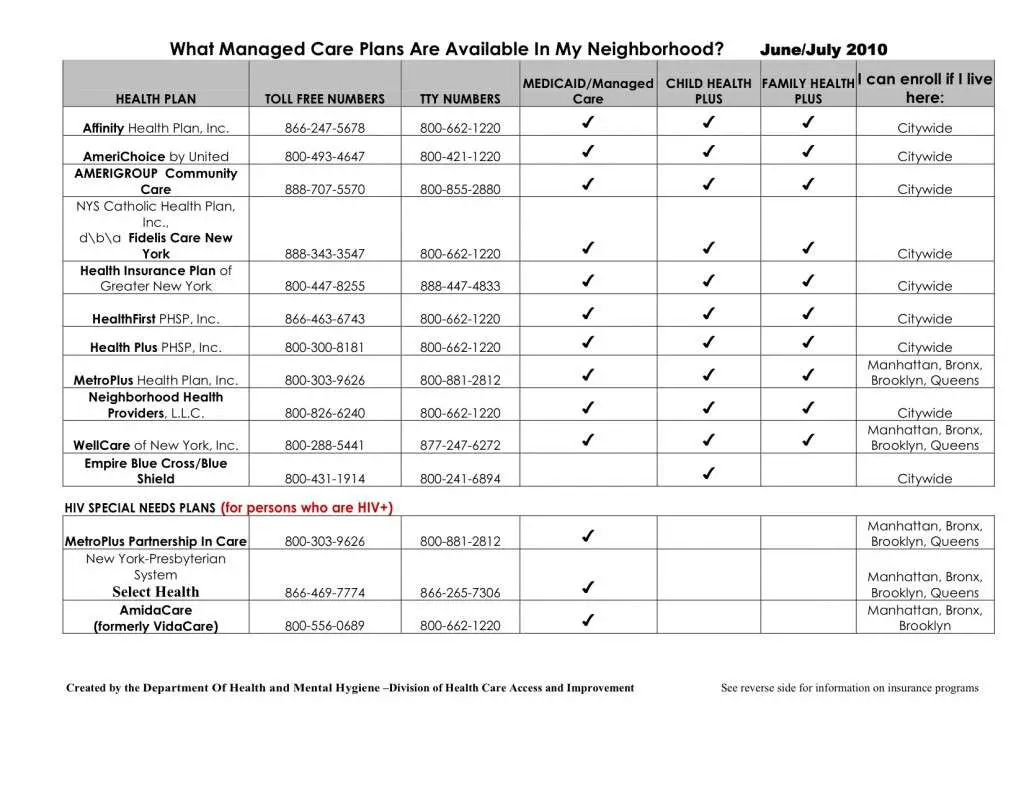
Choosing A Health Plan
To choose the right plan for you and your family, first find out what health plans are available in your county. If you have a doctor you see often, ask that doctor what plans they participate in. Contact the plan to find out what doctors are accepting patients from that plan and ask any other questions you may have. You are entitled to receive certain information about the plan, even if you are not yet enrolled. You may also want to know more about how well the plan provides the services you use most often.
The links below can help you find out what services a managed care plan offers, what managed care organizations are certified in New York and how to pick the best health plan for you and your family.
