How The Age You Retire Affects Your Benefits
You can apply for Social Security retirement benefits once youve turned 62. However, youll receive more money per month if you wait a few years. People who start collecting retirement benefits at 62 will receive 70 percent of their full benefit amount. You can receive 100 percent of your benefit amount if you dont start collecting until full retirement age.
The full retirement age for people born after 1960 is 67. If you were born before 1960, refer to this chart from Social Security to see when youll reach full retirement age.
You can qualify for additional benefits if you have a limited income. Known as Supplemental Security Income , these benefits are for people with limited income who qualify for Social Security because of age or disability.
Reasons Relating To Material Change In Income Or Resources During Six Months Preceding Approval For Assistance
A change in income or resources should be regarded as material only if the amount of the reduction or loss of income is substantial in relation to the need for assistance. A loss of income that is based on need, such as assistance from a public or private agency, is not regarded as a material change in income.
How To Apply Online For Just Medicare
If you are within three months of turning age 65 or older and not ready to start your monthly Social Security benefits yet, you can use our online retirement application to sign up just for Medicare and wait to apply for your retirement or spouses benefits later. It takes less than 10 minutes, and there are no forms to sign and usually no documentation is required.
To find out what documents and information you need to apply, go to the .
You May Like: Does Medicaid Cover Root Canals For Adults
Who Is Eligible For Medicare
Most people enroll in Medicare when they turn 65. You can enroll as early as three months before your 65th birthday or as late as three months after. Youll need to be a United States citizen or have been a permanent legal resident for at least five years. In order to get full coverage, you or your spouse need to meet a work requirement. Meeting the work requirement verifies that youve paid into the system.
State Medicaid Eligibility And Enrollment Policies And Rates Of Medicaid Participation Among Disabled Supplemental Security Income Recipients
In addition to providing income-maintenance payments to eligible participants, the Supplemental Security Income program provides automatic Medicaid enrollment for applicants upon SSI award in most states. Other states require applicants to file a separate Medicaid application. Some use the SSI eligibility criteria for both programs others use Medicaid eligibility rules that are more restrictive. We use matched monthly longitudinal administrative records to test whether automatic enrollment has a positive effect on Medicaid coverage. Using logistic regression with a combination of repeated cross-section and regression discontinuity approaches, we find positive effects of automatic enrollment on Medicaid coverage relative to other policies. The differences are attributable to a discontinuous increase in Medicaid coverage shortly after the final disability determination decision. The time lag arising from the often-lengthy disability determination process reduces the effectiveness of automatic enrollment, which depends critically on timeliness of the final award decision.
The findings and conclusions presented in the Bulletin are those of the authors and do not necessarily represent the views of the Social Security Administration, the Centers for Medicare and Medicaid Services, or any other agency or organizational entity.
You May Like: How To Apply For Women’s Medicaid
Financial Medicaid Eligibility Component
HHSC is responsible for determining if the person meets the criteria specific to CLASS for the financial Medicaid eligibility component. If the person is already eligible for Medicaid through another program under the Texas State Medicaid Plan, the financial Medicaid eligibility component for this waiver has already been met.
When determining financial Medicaid eligibility for CLASS, give special consideration to the following:
I Am About To Turn 65 My Spouse Is 60 And Still Working We Are Both Covered Under Her Employers Health Plan Do I Have To Do Anything With Regard To Medicare This Year
A person with group health coverage through a current employer may be able to delay enrolling in Part A and Part B until that coverage ends, and wont face penalties for enrolling later, but only if the employer has 20 or more employees. If your wifes employer has at least 20 employees, you may want to enroll in Part A but delay enrollment in Part B until your group coverage through your spouses employer plan ends.
If you are already receiving Social Security benefits, you will be automatically enrolled in Part A and Part B when you turn 65. If you do not want to pay a premium for Part B benefits now because you have comparable coverage under your spouses employer plan, you will need to let Social Security know that you want to delay Medicare Part B enrollment. You can contact Social Security about this beginning three months before you turn 65. Otherwise, Medicare will assume you want to enroll in Part B and the monthly premium will be automatically deducted from your Social Security check.
If the employer has fewer than 20 employees, you should sign up for Part A and Part B when youre first eligible or you will face late enrollment penalties.
If you do delay Part B enrollment because you are covered under your wifes plan, remember to sign up for Part B once her coverage ends. That way, youll have continuous coverage and wont face a late enrollment penalty for Part B.
Dont Miss: How Does Geha Work With Medicare
Also Check: Psychiatrist In Nyc That Take Medicaid
Funds Held In Financial Institution Accounts
The Texas Health and Human Services Commission follows 20 CFR §416.1208 regarding the treatment of funds held in financial institution accounts, except the balance of funds in a financial institution account as of 12:01 a.m. on the first day of the month is reduced by the amount of any funds encumbered before that time, including any checks written, that have not yet been processed by the financial institution.
How Soon Before I Turn 65 Can I Sign Up For Medicare
Those collecting Social Security receive Medicare automatically at age 65. For those who arent, its best to enroll in Medicare as soon as possible. Specifically, you should enroll during your Initial Enrollment Period. This is unique to each person and lasts seven full months.
The seven-month window begins on the first day of the month, three months before your 65th birthday. It lasts through your birthday month and ends on the last day of the month, three months after your birthday.
For example, someone whose birthday is June 11 would have an Initial Enrollment Period of March 1 through September 30. Those eligible due to disability have a seven-month window beginning three months before the 25th month of their SSDI payments.
You May Like: How Can I Check The Status Of My Medicaid Application
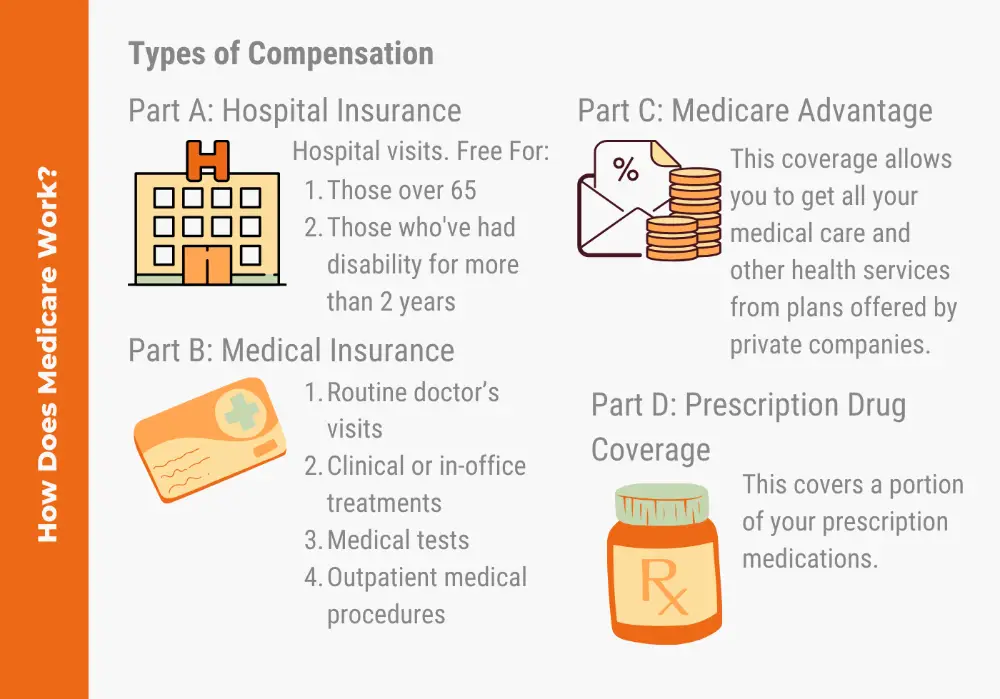
Medicaid And Medicare: An Overview
Both SSA disability programs have health insurance programs associated with them. For SSI it is Medicaid for SSDI it is Medicare which begins two years after the date of eligibility. Establishing eligibility for SSI or SSDI can be key to connecting with Medicaid or Medicare health insurance.
Unmarried Dependent Child Of Veteran/active Duty Member
Eligibility as an unmarried dependent child of a veteran or active duty member ends with the month after the month any of the following occur:
- Loss of dependent status.
- The active duty member separates from the armed forces with a discharge that is not characterized as honorable or that is based on alien status.
- Legal adoption by someone other than the veteran or active duty member of the armed forces or the veteran/active duty member’s spouse.
Also Check: Apply For Sc Medicaid Online
Characteristics Of The Trust
Disbursements for “special needs” or “supplemental needs” or “supplemental care” shall mean nonsupport disbursements and shall not include cash to the beneficiary or payments for food, clothing or shelter. It is not the intention to displace public or private financial assistance that may otherwise be available to any beneficiary. The trustee shall make disbursements only for the supplemental needs as directed by the manager within the manager’s sole discretion. The trust is irrevocable upon acceptance of assets by the trustee. A separate trust subaccount shall be maintained for each beneficiary.
Does Social Security Pay For Medicare
Social Security does not pay for Medicare, but if you receive Social Security payments, your Part B premiums can be deducted from your check. This means that instead of $1,500, for example, youll receive $1,386.40 and your Part B premium will be paid.
Now lets take a look at Medicare and Social Security to understand what these important benefit programs are, how you qualify, and what they mean for you.
Recommended Reading: How Much Do You Have To Earn To Get Medicaid
When Can You Enroll In A Medicare Supplement Insurance Plan
If you have Original Medicare, you may choose to add a Medicare Supplement plan to help pay some of your out-of-pocket costs. More commonly referred to as Medigap, private insurance companies sell Supplement plans.
Although the plans are provided by private insurers, Medicare requires them to be standardized. That means that every Medigap Plan A provides the same benefits, no matter where you buy it. However, costs vary according to the provider you choose.
We always recommend enrolling in a Medicare Supplement plan during you Medigap Open Enrollment Period. This begins the first month you are both aged 65 or older and enrolled in Medicare Part B.
Your Medigap OEP is one of the few times you have guaranteed issue rights, meaning you cannot be denied a Supplement plan or charged a higher rate for it. Outside of your Medigap Open Enrollment Period, your application goes through the medical underwriting process.
Medical underwriting involves answering a variety of health-related questions. This may include:
- Age
Which Statesmake Medicaid Decisions Based On Ssi Standards
Some states use the same eligibility standards as the federalSSI program but insist on making their own Medicaid decisions. In these states,enrollment in Medicaid isn’t automatic when you are approved for SSI, and youmust file a separate application with the state Medicaid agency to get enrolledin the Medicaid program.
These states, called “SSI criteria states,” are:
|
Alaska |
|
Utah |
Also Check: How Do I Add My Newborn To My Medicaid
Med For Home And Community
Prior months’ eligibility and ongoing eligibility for the financial Medicaid eligibility component is contingent upon verification of receipt of waiver services when re-establishing an MED for Home and Community-Based Services waiver services following a denial due for non-receipt of redetermination packet.
Coordinate financial case actions with a waiver case manager.
The following examples are for the financial Medicaid eligibility component for waivers and are not intended to address any situation with continuous Q benefits.
Signed Statement Designating Burial Funds
A signed statement designating resources as set aside for burial must show the:
- value and owner of the resources
- person for whose burial the resources are set aside
- form in which the resources are held and
- date the individual first considered the funds set aside for the burial of the person specified.
Use Form H1252, Designation of Burial Funds, for resources owned by the applicant, recipient or spouse for a signed statement of designation.
Recommended Reading: Who Qualifies For Qmb Medicaid
How Did You Automatically Get Enrolled In Medicare
President/CEO at Healthcare Solutions Direct, LLC, a nationwide insurance agency focused primarily on the retiree health market.
getty
Medicare is a unique type of health insurance because you do not always have to sign up to get it. Once you turn 65, you will become eligible. If you are already collecting social security benefits, you will automatically be enrolled into what is known as Original Medicare. There is nothing you need to do.
The coverage will begin on the first day of the month in which you turn 65 unless you were born on the first of the month. If that is the case, your coverage will begin on the first day of the previous month. You will get alerted to your coverage automatically in the mail by envelope with your Medicare card enclosed. It is mailed out around three months before your 65th birthday.
For many, Original Medicare is far from complete coverage. It is up to you to decide what changes or additions to your healthcare coverage are necessary. If you are still working, it is also up to you to decide whether you would like to continue using the health insurance offered through your employer or not.
With a decade of experience in the healthcare insurance space, I have talked to thousands of Medicare-eligible individuals. In order to make the best decision on what is right for you, you will need a lot of information. This includes an understanding of what each part within Medicare actually covers.
When Can You Enroll In A Medicare Part D Prescription Drug Plan
Original Medicare does not include coverage for prescription medications. To get this coverage, you must enroll in either a Medicare Part D prescription drug plan or an Advantage plan that includes drug coverage. Even if you’re automatically enrolled in Medicare when you turn 65, you must sign up for a Part D plan.
You may enroll in a Part D plan during your Initial Enrollment Period or when you first sign up for Medicare after you leave an employer health plan. If you’re currently enrolled in Medicare, you may also sign up for a prescription drug plan during the Annual Enrollment Period from October 15 to December 7.
Like Medicare Part C, Medicare Part D plans are offered by private insurance companies. And again, prices and coverage vary according to the plan and provider. Use our Find a Plan tool to start comparing Medicare plan options in your area.
Don’t Miss: Does Medicaid Cover A Breast Reduction
Delaying Part B Coverage And Late Enrollment Penalties
You should enroll in Part A when youre first eligible near your 65th birthday, but some people may choose to delay Part B.
If you receive group health insurance at work or through your spouses employer you may be able to delay enrollment in Part B.
But once you stop working or that coverage ends, you must sign up for Part B within eight months. Otherwise, youll face a late enrollment penalty.
If you enroll in Part B after your group health insurance ends, you have options for how to apply.
You can do so online through an application on the Social Security website or by mail.
How to Sign Up for Part B by Mail After Employer Health Insurance Ends
How To Sign Up For Medicare
Some people are automatically enrolled in Original Medicare while others need to sign up on their own. In this guide, we explore the step-by-step process of enrolling in Medicare Part A and Part B as well as Part D drug plans, Medigap policies and Medicare Advantage plans.
On This Page
You May Like: Can You Get Medicare Advantage Without Part B
Recommended Reading: Abortion Clinics In Las Vegas That Accept Medicaid
Overview Of Medicaid Eligibility
Eligibility for Medicaid is determined by both federal and state law, whereby states set individual eligibility criteria within federal minimum standards. This arrangement results in substantial variability in Medicaid eligibility across states. Therefore, the ways that individuals can qualify for Medicaid reflect state policy decisions within broad federal requirements.
In general, individuals qualify for Medicaid coverage by meeting the requirements of a specific eligibility pathway offered by the state.12 Some eligibility groups are mandatory, meaning all states with a Medicaid program must cover them. Other eligibility groups are optional, meaning states may elect to cover them. Within this framework, states may have some discretion to determine certain eligibility criteria for both mandatory and optional eligibility groups. In addition, states may apply to CMS for a waiver of federal law to expand health coverage beyond the mandatory and optional eligibility groups specified in federal statute.
Apply For Medicare Online Through Social Security
To apply online, go to the Social Security web site. Once at the Social Security Web page, a person will see Sign In/Sign Up, and after clicking it, you will choose mySocialSecurity account to continue.
In order to apply for Medicare online, you will first need:
- Your Social Security number
- A valid email address
From the account creation, youll be walked through an email verification process.
After you create your mySocial Security account, you can apply online for Medicare Part A and Part B. This online account will be helpful when updating your address, or replacing a lost Medicare card.
You May Like: How To Cancel Medicaid In Virginia
Eligibility Systems And Payment Systems
Service Authorization System Online identifies the recipient as Service Group 1 and allows vendor payment when:
- an active recipient with coverage Code R enters a nursing facility and
- has a valid medical necessity and facility admission.
The system also automatically assigns a Code 60 , which allows all medications to be paid through the vendor drug benefit.
If the nursing facility stay is temporary and the recipient returns home before being transferred to institutional Medicaid, no action is required. Retroactive coverage code changes are not needed.
