Medicare Part A Premiums
Most people will pay nothing for Medicare Part A. Your Part A coverage is free as long as youre eligible for Social Security or Railroad Retirement Board benefits.
You can also get premium-free Part A coverage even if youre not ready to receive Social Security retirement benefits yet. So, if youre 65 years old and not ready to retire, you can still take advantage of Medicare coverage.
Part A does have a yearly deductible. In 2022, the deductible is $1,556. Youll need to spend this amount before your Part A coverage takes over.
How Is The Federal Poverty Level Used In Health Care
The federal poverty level is used to determine eligibility for Medicaid and CHIP to determine eligibility for ACA premium tax credits and cost-sharing reductions and eligibility for Medicare Savings Programs .
Medicaid and CHIP:
- In states that have expanded Medicaid, Americans under the age of 65 will qualify for Medicaid if they earn up to 138% of the federal poverty level.
- In states that havent expanded Medicaid, the eligibility guidelines are stricter, with much lower income limits for parents and coverage generally not available at all to non-disabled childless adults, regardless of how low their income is. This creates a coverage gap that exists in a dozen states as of 2021.
- For people who are disabled or 65+, Medicaid eligibility also depends on assets .
- CHIP eligibility is also based on the federal poverty level, but the specific thresholds vary from one state to another.
- For Medicaid and CHIP eligibility determinations, the current years federal poverty level numbers are used .
Premium tax credits:
Cost-sharing reductions:
| If more than 8 in household / family, add $4,480 per additional person. | If more than 8 in household / family, add $5,600 per additional person. | If more than 8 in household / family, add $5,150 per additional person. |
Maximums And Deductibles On Hsa
The maximum and deductible requirements for HSA qualifying plans are not the same as maximums and deductibles on health plans in general. Below are the HSA limits for 2022.
Minimum Deductible for HSA Eligibility 2022
- $1,400 for self-only coverage
- $2,800 for family coverage
NOTE: It is $2,800 for embedded individual deductible NOTE: The minimum deductible, which is the minimum deductible your High Deductible Health Plan must have after cost assistance.
Maximum Out-of-Pocket Limit for HSA Eligibility 2022
- $7,050 for self-only coverage
- $14,100 for family coverage
NOTE: The maximum out-of-pocket is the highest maximum a plan can have to qualify for an HSA. TIP: The maximums are slightly lower on HSA compatible plans than they are in general on health plans. This has to do with the fact that the rates are raised by different mechanisms. The difference allows for non-HSA compatible high deductible plans. Thus, if you want an HSA, make sure your plan is HSA Eligible.
HSA Contribution Limit for 2022
- $3,650 for self-only coverage
- $7,300 for family coverage
NOTE: 55 plus can contribute an extra $1,000. TIP: See Revenue Procedure 2021-25 for final HSA levels.
Recommended Reading: How To Obtain A Medicaid Provider Number
What Services Does Medicaid Cover
Medicaid covers more than 60 percent of all nursing home residents and roughly 50 percent of costs for long-term care services and supports.
Federal rules require state Medicaid programs to cover certain mandatory services, such as hospital and physician care, laboratory and X-ray services, home health services, and nursing facility services for adults. States are also required to provide a more comprehensive set of services, known as the Early and Periodic Screening, Diagnostic, and Treatment benefit, for children under age 21.
States can and all do cover certain additional services as well. All states cover prescription drugs, and most cover other common optional benefits include dental care, vision services, hearing aids, and personal care services for frail seniors and people with disabilities. These services, though considered optional because states are not required to provide them, are critical to meeting the health needs of Medicaid beneficiaries.
About three-quarters of all Medicaid spending on services pays for acute-care services such as hospital care, physician services, and prescription drugs the rest pays for nursing home and other long-term care services and supports. Medicaid covers more than 60 percent of all nursing home residents and roughly 50 percent of costs for long-term care services and supports.
How Much Does Medicaid Cost? How Is It Financed?
The 2021 Federal Poverty Guidelines Used In 2022
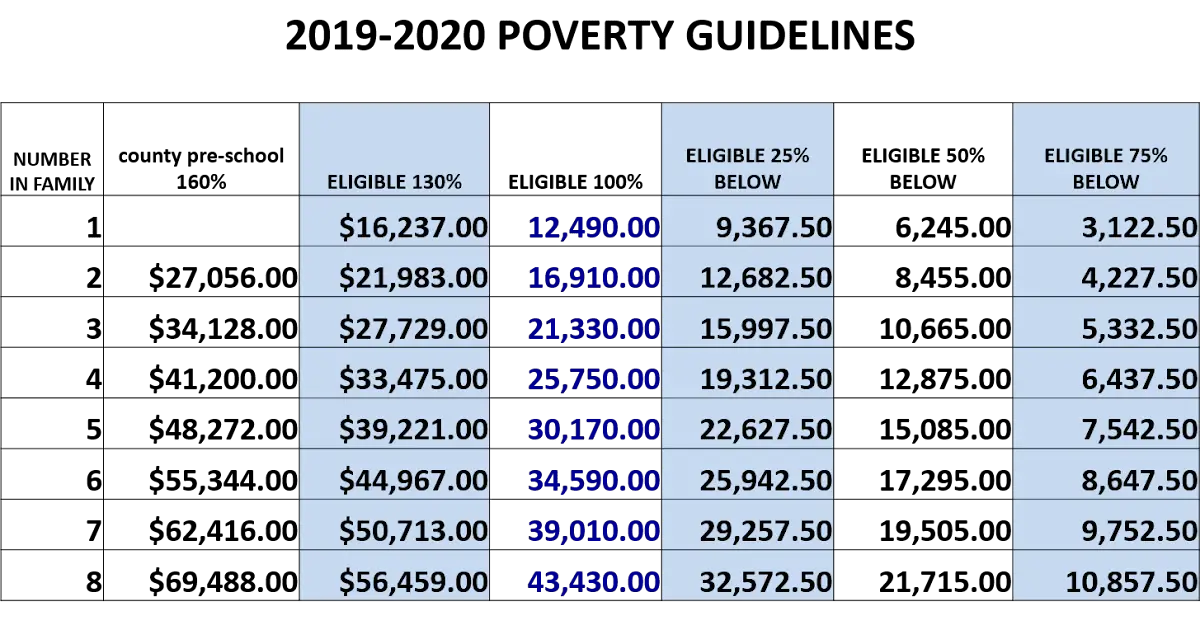
Below are the 2021 Federal Poverty Guidelines that went into effect in early 2021 .
These guidelines are the key to all cost assistance under the Affordable Care Act. Specifically, these guidelines are used for:
- Medicaid/CHIP between late Jan 2021 Jan 2022 after the poverty level guidelines are published.
- 2022 marketplace cost assistance on all marketplace health plans held in 2022 and purchased during open enrollment for 2022 .
- For special enrollment in 2022.
- For ACA taxes for the 2022 calendar year filed in 2023.
NOTE: Our federal poverty guideline list has the 100% poverty level, 138% Medicaid expansion threshold, the 250% CSR subsidy threshold, and the 400% premium tax credit thresholds so you can at a glance see what assistance you qualify for. Please note that for Medicaid Expansion if you make under 138% you qualify, for CSR it is between 100% 250%, and for tax credits, it is between 100% and 400%. See details on subsidies under the ACA.
TIP: For mobile and smaller screen sizes, drag the table below to scroll and see the different poverty levels.
| 2021 POVERTY GUIDELINES FOR THE 48 CONTIGUOUS STATES AND THE DISTRICT OF COLUMBIA |
|---|
| Persons in Family/Household |
Recommended Reading: Does Medicaid Cover Gastric Bypass In Michigan
South Carolina Medicaid Expansion Update
Medicaid has not been expanded in South Carolina.
It is estimated that about 312,000 additional people would be covered if the state accepted Medicaid expansion under the ACA.
However, the state has received federal approval for a Medicaid work requirement that will apply to low-income parents.
Additionally, a separate waiver extends Medicaid eligibility to low-income parents earning up to 100% of the poverty level .
Furthermore, this waiver applies to low-income adults who are chronically homeless, in need of substance abuse treatment, or involved with the justice system.
Who Is Eligible For Medicaid In California
To receive Medi-Cal benefits in California, you must be a U.S. citizen, a state resident of California, a permanent U.S. resident, a legal alien or a U.S. national. You are eligible to receive benefits if you are:
- Over the age of 65
- Blind or disabled
- In a nursing or intermediate care home
- Under the age of 21
- A refugee living in the U.S. temporarily
As a parent or guardian relative of a child who is under the age of 21, you may be eligible for Medicaid assistance if youre taking care of the child because the parents:
- Have died
- Do not live with the child
- Are incapacitated
- Are not employed
You may also qualify for Medi-Cal benefits if you are already enrolled and receiving benefits from one or more of the following programs:
- CalFresh also known as the Supplemental Nutrition Assistance Program
- Supplemental Security Income / State Supplementary Payment
- CalWorks also known as Temporary Assistance to Needy Families
- Refugee Assistance
- Foster Care or Adoption Assistance Program
You May Like: How To Obtain Medicaid In Florida
A Caseworker At The Department Of Social Services Will Assess Your Individual Situation And Discuss Eligibility Requirements
Contact your local department of social services . Apply at johnston county dss at 714 north street smithfield nc 27577. Starting march 15, 2021, there is a new way to get medicaid health care. fmap = federal medical assistance percentage. There are many different medicaid programs, and the eligibility. And people who are determine your eligibility for this benefit. County departments of social services conduct eligibility determinations. In 2021, north carolina will begin the transition to a medicaid managed care model. Applications can be completed by:. All the programs have income limits and some have resource limits. You may apply at the department of social services. This section presents information for women who are uninsured, women who may qualify for medicaid insurance, and women who are currently insured with . A caseworker at the department of social services will assess your individual situation and discuss eligibility requirements.
Option 1 Apply Online
You can apply online through the MI Bridges Portal as shown in the image below.
If you have an account, you can log in or create your MI Bridges Account. to be taken to the website.
The video below, by the Michigan HHS does a great job of explaining how to apply online for benefits with MI Bridges.
We highly recommend you watch it if you are applying online for Michigan Medicaid.
You May Like: Amerigroup Medicaid Texas Breast Pump
How Many People Are On Medicaid
According to the Centers for Medicare & Medicaid Services, as of November 2020, here are the number of people enrolled in Medicaid and Chip in the entire United States:
- 78,521,263 individuals were enrolled in Medicaid and CHIP
- 72,204,587 individuals were enrolled in Medicaid
- 6,695,834 individuals were enrolled in CHIP
Obamacare Pros And Cons List
The ACA, ObamaCare, doesnt create insurance it regulates private insurance to ensure you get more rights and protections. In doing this, it helps tens of millions get access to high-quality affordable health insurance. Of course, health care reform has both financial and private costs. Below are just a few of ObamaCares pros and cons: Pros: ObamaCare contains many benefits, especially for low and middle-income families and small businesses. This includes tax credits for health insurance premiums and out-of-pocket cost assistance based on income, the expansion of Medicaid to low-income adults, letting children stay on their parents plan until 26, the mandate for large employers to cover employees, the expansion of consumer protections like guaranteed coverage for pre-existing conditions and the elimination of gender discrimination, and more. Cons: ObamaCare contains some obstacles for high earners, those who had been healthy and paid low rates in the past, larger firms that didnt insure their employees before the law, and certain sectors of the healthcare industry. After all, ObamaCare contains some new taxes and regulations, and this means more costs for some demographics . Here is a more complete list of ObamaCare pros and cons:
Recommended Reading: Pediatricians In Amarillo Tx That Accept Medicaid
How Do I Know If I Qualify For Medicaid Services
If youre unsure whether you meet the Medicaid qualifications and income requirements, you can use a Medicaid calculator. Simply enter your information, including your state/zip code, income, household size and the number of adults and children you want to enroll.
Health For California is here to help you determine your Medi-Cal eligibility. Our free agents are always available to answer your question. If you want to enroll yourself or your family in Medi-Cal, get your free quote today.
Not sure how Obamacare affects your health care plans in California? Learn how the ACA works in California, including benefits, costs and enrollment.
This Section Presents Information For Women Who Are Uninsured Women Who May Qualify For Medicaid Insurance And Women Who Are Currently Insured With
Applications can be completed by:. This section presents information for women who are uninsured, women who may qualify for medicaid insurance, and women who are currently insured with . You may apply at the department of social services. And people who are determine your eligibility for this benefit. Contact your local department of social services . There are many different medicaid programs, and the eligibility. Income and resource limits vary depending on the medicaid program and eligibility. The process of making an application for medicaid can be . County departments of social services conduct eligibility determinations. Starting march 15, 2021, there is a new way to get medicaid health care. In 2021, north carolina will begin the transition to a medicaid managed care model. A caseworker at the department of social services will assess your individual situation and discuss eligibility requirements. Your medicaid eligibility is not changing, but the organization that .
This section presents information for women who are uninsured, women who may qualify for medicaid insurance, and women who are currently insured with . Your medicaid eligibility is not changing, but the organization that . All the programs have income limits and some have resource limits. Applications can be completed by:. In 2021, north carolina will begin the transition to a medicaid managed care model.
Also Check: Washington State Medicaid Residency Requirements
What Is The Lowest Income To Qualify For Medicaid
There are 13 states that do not grant Medicaid access to individuals based on income alone.
Of those that do, only Wisconsin uses a limit lower than 138%. An individual in Wisconsin can make no more than the federal poverty level in order to qualify for Medicaid.
Texas has the lowest income limit to qualify on a family basis, at 17% of the FPL. A two-parent household with one child in Texas can make no more than $37,332 and qualify for Medicaid.
How To Enroll In Medicaid
You or members of your family may qualify for Medicaid through Maryland Health Connection to receive free or low-cost health care. Enrollment in Medicaid and the Maryland Childrens Health Program is available any time of year.
Are you eligible for Medicaid?
Look up your income and household size below to see if you may qualify. If youre pregnant or have children, you may earn more and still qualify.
| You may be eligible for Medicaid if your monthly income is up to approximately: | |
|---|---|
| If your household size is this | Adults |
Effective February 1, 2021 *Premium cost is per family / household each month
What does Medicaid cover?
Your managed care organization covers doctor visits, pregnancy care, prescription drugs, hospital and emergency services, and more, at no cost.
How do you enroll in Medicaid or MCHP?
1. Apply
Apply via our mobile app: Apple or AndroidApply over the phone 1-855-642-8572.
Learn who to include in your household, how to calculate your household income and what documents youll need.
2. Check for available help
Get answers and advice on all of your health coverage options before you select your plan. Search for free, local help.
3. Send verification documents as needed
You will receive a notice if we need documents to complete your application.
4. Choose a doctor and a Managed Care Organization
Ask your doctors which MCOs they accept or use the MCO search tool.
5. Pay your bill
- What is Medicaid & How Do I Apply?
- Enrolling in Medicaid
Read Also: Does Medicaid Cover Substance Abuse Treatment
In 2021 North Carolina Will Begin The Transition To A Medicaid Managed Care Model
Children under the age of 19 who do not qualify for medicaid may qualify for nc health choice . There are many different medicaid programs, and the eligibility. Apply at johnston county dss at 714 north street smithfield nc 27577. You may apply at the department of social services. County departments of social services conduct eligibility determinations. And people who are determine your eligibility for this benefit. The process of making an application for medicaid can be . North carolina health choice offers health coverage for children whose. All the programs have income limits and some have resource limits. Starting march 15, 2021, there is a new way to get medicaid health care. Your medicaid eligibility is not changing, but the organization that . Applications can be completed by:. fmap = federal medical assistance percentage.
There are many different medicaid programs, and the eligibility. fmap = federal medical assistance percentage. The process of making an application for medicaid can be . Income and resource limits vary depending on the medicaid program and eligibility. Starting march 15, 2021, there is a new way to get medicaid health care.
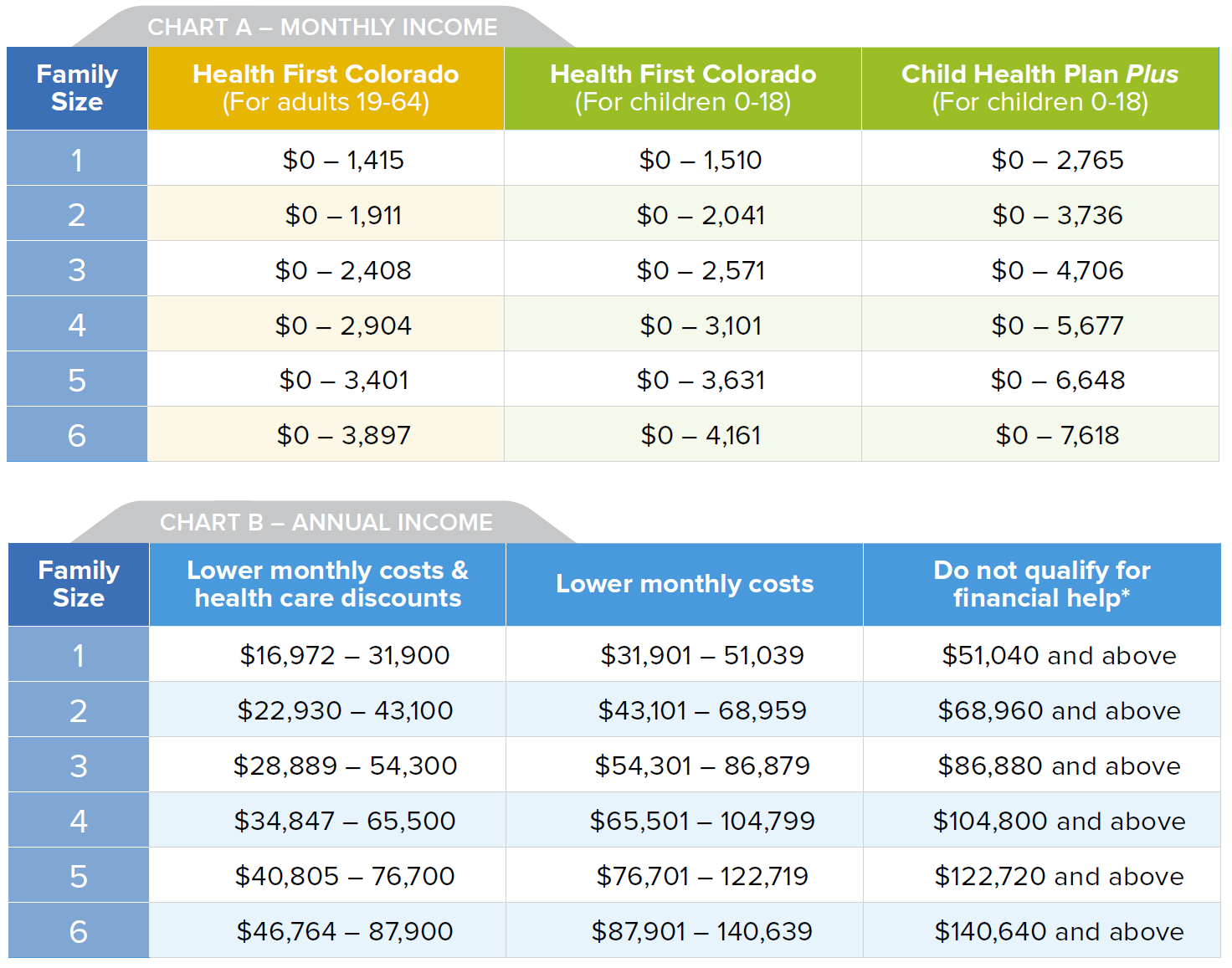
See If You Can Sign Up For Health First Colorado
You may qualify for Health First Colorado if you meet the monthly income guidelines:
| Family Size |
Can I still sign up for a plan through Connect for Health Colorado if I qualify for Health First Colorado?
- Yes. You can still purchase a private health insurance plan at full price if you qualify for Health First Colorado.
- NOTE: If you qualify for Health First Colorado or CHP+, you will not qualify for financial help to lower the cost of your health insurance plan through Connect for Health Colorado. You will pay full price for your health insurance plan.
I applied through Connect for Health Colorado and was told that my application was sent to Health First Colorado. Whats next?
- Watch your mail or email. You will get a notification from the State of Colorado with your application results. You will also receive a letter or email if more information is needed to complete the process.
- You may also check the results of your application through your PEAK account.
- If you do not have a PEAK account, you can create one at Colorado.gov/PEAK.
- You can use your Connect for Health Colorado log-in and password information to sign into PEAK.
- You can also use PEAK to manage your Health First Colorado or CHP+ benefits, print benefit cards, report changes and more.
Don’t Miss: Psychiatrist In Nyc That Take Medicaid
South Carolina Medicaid Income Limit
The South Carolina Medicaid Income Limit is calculated as a percentage of the Federal Poverty Line.
To qualify, you must meet the South Carolina Medicaid Income limits listed below.
Here is the Federal Poverty Level for 2021.
| 2021 Federal Poverty Levels for the 48 Contiguous States & D.C. |
| Household Size |
Additionally, to be eligible for Medicaid, you cannot make more than the income guidelines outlined below:
- Children up to age 1 with family income up to 208 percent of FPL
- Any child age 1-5 with a family income up to 208 percent of FPL
- Children ages 6- 18 with family income up to 208 percent of FPL
- CHIP for children with family income up to 208 percent of FPL
- Pregnant women with family income up to 194 percent of FPL
- Parents of minor children with family income up to 95 percent of FPL
- Individuals who are elderly, blind, and disabled with family income up to 100% of the FPL
