Pressure Reducing Support Surfaces
Group 1 support surfaces are generally designed to either replace a standard hospital or home mattress or as an overlay placed on top of a standard hospital or home mattress. Products in this Category include non-powered pressure reducing mattresses, pressure pads and mattress overlays . A Group 1 mattress overlay or mattress is covered if one of the following three criteria is met:
1. The beneficiary is completely immobile- i.e., beneficiary cannot make changes in body position without assistance, or
2. The beneficiary has limited mobility – i.e., beneficiary cannot independently make changes in body position significant enough to alleviate pressure and at least one of the conditions A-D below.
3. The beneficiary has any stage pressure ulcer on the trunk or pelvis and at least one of the conditions A-D below.
A. Impaired nutritional state
g. Education of the beneficiary and caregiver on the prevention and management of pressure ulcers andh. Assessment by a physician, nurse, or other licensed healthcare practitioner at least weekly, andi. Appropriate management of moisture/incontinence.
6. A trained adult caregiver is available to assist the beneficiary with activities of daily living, fluid balance, dry skin care, repositioning, recognition and management of altered mental status, dietary needs, prescribed treatments and management and support of the air-fluidized bed system and its problems such as leakage.
Coverage and Payment Policy
Manufacturer Suggested Retail Price
If the fee schedule states “Code is Manually Priced”, reimbursement is the lower of or the provider’s U& C.
- The provider must keep a copy of the item’s invoice and documented MSRP.
- The documented MSRP must include the name of the provider’s employee that received and documented the MSRP, and the date the MSRP was received.
- Providers may not submit for reimbursement for either state sales tax collection or shipping costs.
- Providers must add the ‘SC’ modifier when using the MSRP for pricing.
- Providers must attach a copy of the MSRP on all claims.
- Providers may manually indicate on the MSRP documentation the actual quantity supplied to the member if it differs from claim total.
State Health Department And Cms Forge Alliance To Improve Care To Dual Eligibles
The Centers for Medicare & Medicaid Services and the New York State Department of Health have established a federal-state partnership to implement the Medicare-Medicaid Alignment Initiative that will better serve individuals eligible for both Medicare and Medicaid.
Under the partnership, DOH and CMS will contract with Fully Integrated Duals Advantage Plans, which are Medicare-Medicaid Plans that provide integrated benefits to people eligible for both Medicare and Medicaid. The FIDA plans oversee the delivery of covered Medicare and Medicaid services for enrollees who reside in New York City and the surrounding counties of Nassau, Suffolk and Westchester. The demonstration will begin July 1, 2014 and continue until December 31, 2017.
The initiative is testing an innovative payment and service delivery model to alleviate health care fragmentation, improve coordination of services for Medicare-Medicaid enrollees, and enhance the quality of care. This demonstration is an important building block in the state’s move to “Care Management for all” in Medicaid.
“We are delighted to partner with CMS to offer access to more coordinated care to Medicare-Medicaid beneficiaries with long-term care needs,” said State Health Commissioner, Nirav R. Shah, MD, MPH. “Providing customized services that address each individual’s medical, behavioral and social needs is critical to improving the health and well-being of this population.”
You May Like: Humana Medicaid Florida Over The Counter
Used And Refurbished Dme And P& o
Supply providers have the option to request used and/or refurbished DME and P& O. Equipment may be donated, passed down from a sibling, or purchased from a DMEPOS provider post refurbishment. Used equipment also includes equipment that has not been previously rented or sold . All used and refurbished equipment requires a PAR.
The DMEPOS provider must guarantee that the equipment provided to the member is in “like new” condition, and that any modifications are made prior to the delivery of the equipment. The cost of repairs or modifications must not exceed the cost of replacement equipment. The provider will maintain a one year limited warranty that covers all necessary parts or repairs. Comparison pricing for new equipment must be included in the PAR documentation. PAR documentation must include the make, model, and serial number of equipment. The Used Equipment modifier must be included on all used and refurbished equipment PARs and claims.
Examples of allowable used or refurbished equipment include but are not limited to:
- Manual Wheelchairs
- Hospital Beds
- Lifts
- Speech Generating Devices
If new equipment is rented to and subsequently purchased by the same member, it would not be considered used. Supplies may not be provided as used.
Unless a part of the Upper Payment Limit, the maximum allowable for used/refurbished equipment is 60% of the equipment’s maximum allowable for purchase.
Clinical Guidelines For Enteral Nutrition

These Guidelines identify the clinical information that the Rhode Island Medical Assistance Program requires to determine medical necessity for Enteral Nutrition products. The Guidelines are based on generally accepted standards of medical practice, review of medical literature, federal and state policies, and laws applicable to Medicaid programs.Enteral Nutrition is defined as supplemental feeding provided via the gastrointestinal tract orally, or through a tube, catheter or stoma distal to the mouth.
Read Also: Assisted Living Facilities In Arkansas That Accept Medicaid
Does Medicare Cover Tens Units
- Does Medicare cover TENS units? Find out if you can receive coverage and what else you need to know about e-stim therapy as part of your ongoing treatment.
While Medicare does cover TENS units, it is usually on a case-by-case basis. Original Medicare and Medicare Advantage plans can cover TENS units when they’re medically necessary.
Before receiving approval for a TENS device, you may need to attempt other treatment options. If it’s established that previous attempts to treat your condition via other means have failed, you and your doctor may be able to receive approval for a TENS unit.
A Commode Is Covered When The Patient Is Incapable Of Utilizing Regular Toilet Facilities
Coverage and Payment Policy
A commode is covered when the beneficiary is physically incapable of utilizing regular toilet facilities. This would occur in the following situations:
An extra wide/heavy duty commode chair is covered for a beneficiary who weighs 300 pounds or more.
A commode chair with detachable arms is covered if the detachable arms feature is necessary to facilitate transferring the beneficiary or if the beneficiary has a body configuration that requires extra width.
Commode chair with seat lift mechanism is covered if the beneficiary has medical necessity for a commode and meets the coverage criteria for a seat lift mechanism.
Duplicate devices for multiple bathrooms are not covered.
Click here for an approved PDF version of the Commode coverage guidelines.
Compression Garment
A compression garment is a custom made or custom fitted support garment fabricated to apply varying degrees of pressure to specific anatomic areas. These garments affect stress on vein walls, muscle pump activity, tissue pressure and circulation. These garments are also used in the treatment of burn patients. The majority of applications do not require custom made garments.
You May Like: Does Missouri Medicaid Cover Assisted Living
Tens For Chronic Low Back Pain
CMS issued a Medicare National Coverage Determination on June 8, 2012 that allows coverage of Transcutaneous Electrical Nerve Stimulation for chronic low back pain only when the patient is enrolled in an approved clinical study within three years after the publication of this decision under coverage with evidence development that meets the criteria outlined below. 1
The results of additional clinical research may potentially provide sufficient evidence to inform future NCDs on the topic. CMS will maintain a list of all approved studies and post that list on this website.
Does Medicare Cover Tens Units For E
There are many conditions that may require e-stim therapy, which requires the use of a TENS unit. If your doctor is using a broader approach that incorporates the use of your device as part of a larger treatment plan, you’re more likely to be approved for coverage. Medicare Advantage plans vary and may have different requirements for coverage but are generally more accepting of TENS unit therapy.
Read Also: Family Doctors In Charleston Wv That Accept Medicaid
Early And Periodic Screening Diagnostic And Treatment
8.280.4.E Other EPSDT Benefits
Other health care services may include other EPSDT benefits if the need for such services is identified. The services are a benefit when they meet the following requirements:
Personal Emergency Response System
Personal Emergency Response System is an electronic device that enables certain individuals at high risk of institutionalization to secure help in an emergency. The individual may also wear a portable “help” button to allow for mobility. The system is connected to the individual’s phone and programmed to signal a response center once a “help” button is activated. Trained professionals staff the response center, as specified by the Center for Adult Health contract standards.
You May Like: What Is The Difference Between Medicare & Medicaid
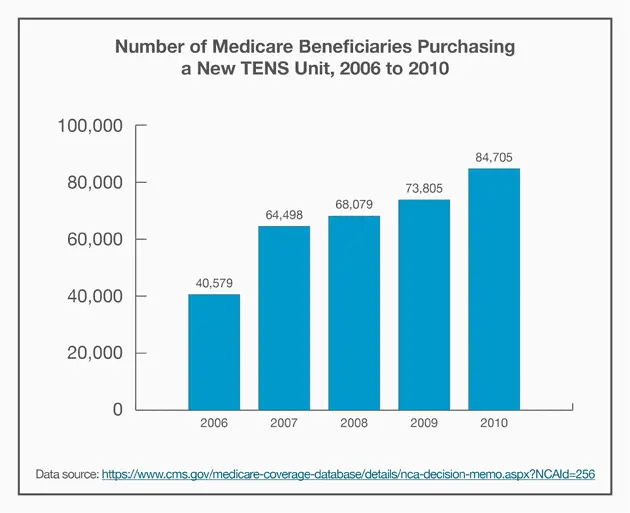
Medicare Will Stop Reimbursing Patients For Tens Unit Purchases
Sunday, July 15th, 2012
Recently, the Center for Medicare Services announced that it will no longer cover TENS unit therapy. Tens unit, which stands for transcutaneous electrical nerve stimulation, is a low-cost and low-risk therapy for alleviating pain.
The memo that was released by CMS stated tens is not reasonable and necessary for the
TENS Unit
treatment of chronic low back pain,. In addition, the memo stated that tens units will only be reimbursed when the patient is part of a randomized, controlled trial looking at the effectiveness of the treatment.
The units are about the size of an iPod and patients can wear them on their belt. The units emit slight electrical impulses to go through foam pads on the skin for the purpose of providing a low risk method of relieving many types of pain. While it has been known for some time that the effectiveness of tens units has been inconclusive, the report a couple years ago from the American Academy of Neurology found the treatment not to be effective.
Interestingly, when most Arizona pain doctors and chiropractors are interviewed they say that their patients get great results from using TENS units. There are plenty of anecdotes of patients seeing excellent results from tens units, for instance at pain management Scottsdale clinics. However, CMS based its decision on formal clinical studies to draw its conclusion.
| 31 |
Palivizumab Article 28 Clinic Reimbursement
Palivizumab is reimbursable to hospital-based and free-standing clinics and is reimbursed under Ambulatory Patient Groups as well as ordered ambulatory for non-clinic patients.
When billing the cost and administration of palivizumab for registered clinic patients under APGs:
- For the immune globulin, use CPT procedure code 90378, respiratory syncytial virus, monoclonal antibody, recombinant, for intramuscular use, 50mg, each. This will group to APG 416, Level III Immunization.
- Submit the valid 11 digit NDC, quantity, and units on the claim.
- For the administration, use CPT 90460 Immunization administration through 18 years via any route of administration, with counseling by a physician or other qualified health care professional: first or only component of each vaccine or toxoid administration. This will group to APG 490 and will not pay at the line level.
- This immunization may be billed as a “stand alone” service even if there are no other procedure codes included on the claim.
When billed ordered ambulatory:
- If a Medicaid enrollee is referred to the Article 28 clinic by their private practitioner, the clinic should bill CPT code 90378 for the immunization as an ordered ambulatory service and report actual acquisition cost . Additionally, providers should bill CPT code 90471 for immunization administration 1 vaccine which will pay $13.23.
Please call the eMedNY Call Center at 343-9000 with billing questions.
Read Also: Aged Blind Disabled Medicaid Nj
Additional Upstate Counties To Be Added To Transportation Carve
To implement the Medicaid Redesign Team’s Transportation Reform Initiative, the Department is phasing in a Medicaid fee-for-service non-emergency medical transportation management program under which transportation services are carved out of the Medicaid managed care benefit package. The first NEMT program for managed care enrollees was implemented in the Hudson Valley Region in January 2012, with additional counties in the Region moving to the NEMT manager in March and September of 2012 , and implementation in New York City in January 2013.
Beginning January 1, 2014, the following transportation services will be carved-out of the managed care benefit package for managed care enrollees in 24 additional counties in the Finger Lakes and Northern New York:
- 1) emergency and non-emergency transportation services for all Medicaid managed care enrollees and
- 2) non-emergency transportation only for Family Health Plus enrollees aged 19 through 20.
The upstate carve-out schedule for transportation of managed care enrollees is provided below:
Members and medical providers in the these counties should be advised to contact Medical Answering Services, LLC , at the county-specific numbers provided on the following page:
Albany County855-360-3549| Staten Island facility fax877-585-8780 |
| Hospital Discharge 877-564-5926 |
Managed care enrollees may use the numbers below to make their own transportation arrangements through LogistiCare or to register a complaint:
It May Take Time To Know If Tens Will Work For You
Keep in mind it may take a number of sessions with your doctor or pain therapist to know if TENS will ease your pain. Your healthcare provider may need to try different types of TENS machines or different settings. This will help you see if youll benefit from TENS. If so, your doctor or therapist will be able to recommend the most effective unit for you to buy and the settings to use.
Also Check: The Phone Number For Medicaid
Additional Low Back Pain Coverage Guidelines
COVERAGE DECISION:
Effective November 1, 2013, for Medicaid fee-for-service beneficiaries, Medicaid Managed Care enrollees and Family Health Plus enrollees, the following procedures are subject to limitation, as they are considered ineffective, or experimental and investigational, for the treatment of chronic low back pain :
- 62290 Injection procedure for discography, each level lumbar
- 72295 Discography, lumbar, radiological supervision and interpretation
Discography for the following conditions is considered not medically necessary:
- Lumbago, low back pain syndrome, lumbalgia, as represented by 2013 ICD-9 code 724.2
- Unspecified backache, vertebrogenic syndrome not otherwise specified, as represented by 2013 ICD-9 code 724.5
The decision to discontinue coverage of lumbar discography for chronic low back pain, or nonspecific LBP, is based on a lack of medical evidence, and the potential for harm. Medicaid will continue to cover discography for other indications, if medically necessary.
DESCRIPTION OF PROCEDURE OR SERVICE:
Practitioners are responsible for ensuring that the codes submitted for reimbursement accurately reflect the service or procedure that was provided. Post payment reviews are conducted by the Office of the Medicaid Inspector General on adjudicated claims. Medical records must be maintained by providers for a period of not less than six years from the date of payment.
Does Medicare Cover Tens Units For Back Pain
Most of the evidence and research about TENS units has been anecdotal in regards to how effective a TENS unit is in the treatment of back pain. For this reason, Medicare may deny coverage on the grounds that your doctor is not exploring other avenues for your treatment. While it’s not impossible to gain approval for a TENS unit, it’s considered a last option.
Also Check: Vermont Medicaid Dental Fee Schedule
User License Agreement And Consent To Monitoring
End User Agreements for Providers
Some of the Provider information contained on the Noridian Medicare web site is copyrighted by the American Medical Association, the American Dental Association, and/or the American Hospital Association. This includes items such as CPT codes, CDT codes, ICD-10 and other UB-04 codes.
Before you can enter the Noridian Medicare site, please read and accept an agreement to abide by the copyright rules regarding the information you find within this site. If you choose not to accept the agreement, you will return to the Noridian Medicare home page.
THE LICENSES GRANTED HEREIN ARE EXPRESSLY CONDITIONED UPON YOUR ACCEPTANCE OF ALL TERMS AND CONDITIONS CONTAINED IN THESE AGREEMENTS. BY CLICKING ABOVE ON THE LINK LABELED “I Accept”, YOU HEREBY ACKNOWLEDGE THAT YOU HAVE READ, UNDERSTOOD AND AGREED TO ALL TERMS AND CONDITIONS SET FORTH IN THESE AGREEMENTS.
IF YOU DO NOT AGREE WITH ALL TERMS AND CONDITIONS SET FORTH HEREIN, CLICK ABOVE ON THE LINK LABELED “I Do Not Accept” AND EXIT FROM THIS COMPUTER SCREEN.
IF YOU ARE ACTING ON BEHALF OF AN ORGANIZATION, YOU REPRESENT THAT YOU ARE AUTHORIZED TO ACT ON BEHALF OF SUCH ORGANIZATION AND THAT YOUR ACCEPTANCE OF THE TERMS OF THESE AGREEMENTS CREATES A LEGALLY ENFORCEABLE OBLIGATION OF THE ORGANIZATION. AS USED HEREIN, “YOU” AND “YOUR” REFER TO YOU AND ANY ORGANIZATION ON BEHALF OF WHICH YOU ARE ACTING.
LICENSE FOR USE OF “PHYSICIANS’ CURRENT PROCEDURAL TERMINOLOGY”, FOURTH EDITION
Consent to Monitoring
