Medicaids Requirement For Weight Loss Surgery
Medicaids requirements for weight loss surgery coverage are a little different as compared to other insurance plans. Typically, this is because Medicaid is unique in who they cover and how they cover their patients.
You need to meet a number of specific requirements in order to qualify for weight loss surgery through Medicaid, and you also need to be free from any medical issues that would prevent you from having surgery. If you pass these two tests, then Medicaid will generally pay for your weight loss surgery.
How Long Does Medicaid Pay For Weight Loss Drugs
Some of the restrictions placed upon Medicaid coverage of weight-loss prescriptions are to be expected, while others are interesting. For example, Georgia covers Xenical, but only for persons aged 12-21 and only for one year. Rhode Island covers any weight-loss drug but for only 3 months with prior authorization.
State Insurance Law Analysis
We reviewed state laws and regulations for private insurance in both the individual and small-group markets for statutory provisions that expressly prohibit or regulate medical insurers’ medical underwriting or eligibility exclusion practices where obesity or health status is used as an independent risk factor and statutory provisions mandating coverage of obesity-related treatments. The 2004 CMS policy change allowed obesity to be considered a medical condition, and, thus, considered under the term health status.
We conducted a state-by-state document review of state insurance laws and regulations obtained via Internet search of the following websites: each state’s Department of Insurance, National Association of Health Underwriters, Georgetown University Health Policy Institute, National Association of Insurance Commissioners, and legal searches of state insurance codes from Westlaw and Lexis Nexis®. We searched state legislature websites for relevant enrolled legislation that had not yet been compiled into the official state code.
Key words included obesity, weight loss, bariatric surgery, mandated coverage, nutritional counseling, morbid obesity, gastric bypass, underwriting, risk factors for underwriting, exclusions, and preexisting conditions.
Read Also: Michigan Pregnancy Medicaid Income Limits
Types Of Weight Loss Surgery Medicare Does Not Cover
Medical does not cover weight loss procedures for which there is insufficient evidence to confirm that they are reasonable and necessary. These include the surgeries below, some of which have caused safety concerns:
- Open and laparoscopic vertical banded gastroplasty: This combination of stapling the stomach and inserting a band creates a very small stomach.
- Open and laparoscopic sleeve gastrectomy: This procedure involves the removal of most of the stomach.
- Open adjustable gastric banding: This procedure is similar to the laparoscopic version, except that surgeons perform it through a large cut in the abdomen.
- Gastric balloon surgery: Surgeons insert a device into the stomach to reduce its capacity.
- Intestinal bypass: This surgery bypasses much of the small intestine.
It is difficult to estimate the portion of this amount that a person must pay out of pocket, as it is not possible to determine the necessary services in advance. Original Medicare, which comprises Part A and Part B, provides coverage for those who meet the eligibility requirements, but deductibles, coinsurance, and copayments still apply.
The total expenses will depend on the type of surgery and several other factors, including:
- whether an individual has met their deductibles
- whether a person has surgery-related problems
- if procedures take place on an inpatient or outpatient basis
In general, a person with original Medicare may expect the following costs in 2021:
State Regulation Of Insurers’ Obesity

About 68% of Americans obtain health-care benefits through private health insurance plans, many of which are regulated at the state level. Some states require insurers to offer specific health benefits or access to certain types of providers. Other state regulations affect the rating rules that insurers use to set premiums or to evaluate people for coverage through medical underwriting.
Privately insured people are overwhelmingly insured in the employer-based group market, with only 6% of insured people covered through the individual market. In the small-group market, we found that 41 states and the District of Columbia either explicitly or implicitly allow insurers to use health status or obesity as an independent factor in determining rates. Only nine states require small-group health plans to use a community or an adjusted community rating, where the premiums would be based on the expected claims of the community, not the individual employer group. These findings are consistent with the consumer information available from the National Association of Health Underwriters.
Thus, in most states, an employer’s health insurance premiums can be affected by the weight of his or her employees. Obesity carries high health-care costs thus, as obesity rates rise, increasing health insurance premiums may lead employers to drop health insurance coverage, increase premiums and cost-sharing for employees, or lower wages for workers.
You May Like: Does Medicaid Cover Glasses In Texas
Start Working With A Top Doctor As Soon As Possible
Top doctors will help you navigate the various procedure choices, pre-surgery steps, financing, and insurance options.
- As a first step, many doctors offer a free initial consultation to give you a better understanding of what to expect.
- Many will also provide a free insurance check to help you figure out how much insurance will cover, and, if necessary, appeal any denials or find additional financing. Most insurance companies require you to complete a medically supervised diet and exercise program before they will approve your surgery, so your doctor will set this up for you if you havent done so already.
- Your doctor will also push you towards new habits that will be essential to long-term success after surgery. Many doctors will recommend that you attend support group meetings so you can listen to feedback from actual patients.
Find a Doctor Essential Checklist: 3 to 6 Months Out
Medicare And Weight Loss Surgery
Medicare covers weight loss surgery in many cases, including roux en y gastric bypass, duodenal switch, and lap band surgery. Any other weight loss procedures are deemed experimental and will not be covered by Medicare. Some of these might include a gastric balloon, intestinal bypass, or liposuction.
However, you must meet specific coverage requirement, including:
- Body mass index of 35 or greater
- Passed psychological evaluation
- An illness that is directly related to obesity
- Documented evidence of obesity for the last five consecutive years
- Proof of medically supervised weight loss program completion or nutritional counseling
- A physicians letter supporting or recommending weight loss surgery
- Normal screening tests that prove that there are no other medical issues that are causing your obesity
Medicare looks at each case uniquely. You must be able to provide the scientific facts of your obesity, in addition to the documentation that youve met the other Medicare requirements. It may take a few months to get all of these things in order and to get an answer from Medicare to see if you have been approved.
You May Like: How Can I Check The Status Of My Medicaid
Food & Drink: Your 14
Improving your food choices and lifestyle habits will be the most important change after the procedure. The gastric balloon provides a great opportunity to jumpstart a longer-term diet and exercise program. However, since it is not a permanent solution , many patients wisely use this time to change long-term habits.
Your surgeons dietitian or nutritionist, and sometimes a personal trainer, will help get you on track for long-term success. Here is what your diet transition will look like:
| Timeframe |
|---|
|
About a week after surgery, you will switch to a pureed food diet. Your doctor will work with you regarding the exact timing and what foods you should be eating. This diet will likely consist of pureed lean protein foods, such as fish, poultry, eggs, cheese, or dairy and soy products. These should always be accompanied by high ratios of pureed fruits and vegetables. |
After your balloon is removed, your surgeon will discuss options such as continuing your new diet and exercise regimen, replacing your balloon with a new one, or potentially transitioning to a more permanent type of weight loss surgery.
Does Medicare Cover Bariatric Surgery
Does medicare cover bariatric surgery? Do they cover gastric sleeve surgery? Is there a co-pay?
According to Medicare, they do cover bariatric surgeries as long as the patient applying for approval fits their requirements. Their requirements include the patient having a body mass index over 35 and at least one co-morbidity related to obesity. Comorbidity is a disease that is a result of ones obesity. These co-morbidities can include: Type II Diabetes, high blood pressure, high cholesterol, obstructive sleep apnea, soft tissue infections, depression, stroke or risk of stroke, GERD and Gallbladder Disease, just to name a few.
The patient must also have documentation in their medical records confirming they have tried to lose weight in the last 12 months without success. If all of these things apply to this patient, they are eligible for coverage.Medicare Approved Surgery Types
Read Also: Is Wisdom Teeth Removal Covered By Medicaid
Bariatric Surgery For The Treatment Of Idiopathic Intracranial Hypertension
Levin and colleagues stated that IIH occurs most frequently in young, obese women. Gastric bypass surgery has been used to treat morbid obesity and its co-morbidities, and IIH has recently been considered among these indications. These investigators presented a case report of a 29-year old female with a maximum BMI of 50.3 and a 5-year history of severe headaches and moderate papilledema due to IIH. She also developed migraine headaches. After a waxing and waning course and various medical treatments, the patient underwent laparoscopic Roux-en-Y gastric bypass surgery with anterior repair of hiatal hernia. Dramatic improvement in IIH headaches occurred by 4 months post-procedure and was maintained at 1 year, when she reached her weight plateau with a BMI of 35. Pre-surgery migraines persisted. This added to the small number of case reports and retrospective analyses of the successful treatment of IIH with gastric bypass surgery, and brought this data from the surgical literature into the neurological domain. It offered insight into an early time course for symptom resolution, and explored the impact of weight-loss surgery on migraine headaches. The authors concluded that this treatment modality should be further investigated prospectively to analyze the rate of headache improvement with weight loss, the amount of weight loss needed for clinical improvement, and the possible correlation with improvement in papilledema.
Conversion Of Sleeve Gastrectomy To Roux
Langer and colleagues noted that due to excellent weight loss success in the short-time follow-up, sleeve gastrectomy has gained popularity as the sole and definitive bariatric procedure. In the long-term follow-up, WL failure and intractable severe reflux can necessitate further surgical intervention. These investigators carried out a retrospective analysis of laparoscopic conversions from SG to Roux-en-Y gastric bypass to assess the efficacy for reflux relief and WL success 8 out of 73 patients underwent conversion to RYGB for severe reflux or weight regain after a median interval of 33 months following laparoscopic SG . In 1 of the patients, a banded gastric bypass was performed. In both groups, conversion to RYGB was successful, as proton pump inhibitor medication could be discontinued in all patients presenting with severe reflux, and a significant WL could be achieved in the patients with WR within a median follow-up of 33 months. Post-operative complications were observed in only 1 patient as leakage at the gastrojejunostomy was successfully treated by temporary stent placement. The authors concluded that conversion to RYGB was an effective treatment for WR or intractable reflux symptoms following SG. Therefore, SG could be performed, intended as the sole and definitive bariatric intervention, with conversion from SG to RYGB as an exit strategy for these complications.
You May Like: Blue Cross Blue Shield Medicaid Dental Providers
Cigna Requirement For Weight Loss Surgery
Cigna Requirement for Weight Loss Surgery
Most of the insurance policies offered by Cigna do cover weight loss surgical procedures, but there are some benefit plans that specifically exclude it. If you are not sure whether or not your particular plan includes surgical procedures for weight loss, make sure that you contact Cigna directly to find out.
All of the following requirements and criteria for weight loss surgery under Cigna health insurance plans also apply to Great West Healthcare, a provider that Cigna recently merged with.
Requirements for Pre-Approval of Weight Loss Surgery with Cigna
Unless you have a policy that specifically excludes weight loss surgery, surgery is going to be covered provided that you meet specific criteria set forth by Cigna. These requirements include all of the following:
- You need to be at least 18 years old,
- You need to have reached your expected skeletal growth,
- You need to have documented evidence of a BMI exceeding 40, or
- You need to have documented evidence of a BMI exceeding 35 with a significant comorbidity. Qualifying comorbidities include:
- Type 2 diabetes,
- Pulmonary hypertension,
- Obstructive sleep apnea.
What Weight Loss Procedures Does Cigna Cover?
The procedures that Cigna generally covers will include all of the following.
- Natural Orifice Surgery
Other Considerations
Remember that excess body weight is defined as the weight that you need to lose, not your total body weight.
Resources:
Important Things To Know
For Medicaid to cover your weight loss surgery, you must have your procedure at a Center for Excellence . These facilities have a level of excellence that makes them successful at performing these procedures. If you have any specific questions about your Medicaid coverage and whether or not weight loss surgery is an option for you, contact them directly. Yes, your surgeon is an excellent source of information, but you are responsible for making sure there is no surprises post-op regarding out of pocket costs and overall coverage.
- Editor
Read Also: How To Obtain A Medicaid Provider Number
Exercise: 25 Hours Per Week Spread Out Over 2 To 4 Days
Exercise is almost as important as your diet when it comes to long-term success:
- Patients who exercise regularly lose more weight over the long-term
- Physical and mental health benefits are incredible
How much exercise do you need to for noticeable results?
While no studies exist for the gastric balloon procedure, one study of gastric bypass patients found that 2.5 hours per week resulted in 5.7% greater excess weight loss 00501-1/abstract” rel=”nofollow”> 16).
To help you stay on track, block out time to exercise at the same times on the same days of the week.
Also, spread your 2.5 hours per week out over 3 or 4 days . This will make it less intimidating to get started each day and will help you build endurance.
Exercise Types
There should be 3 main goals of your exercise routine:
- Endurance walking, stationary bike, and especially swimming
- Flexibility a good stretching routine. Yoga is best since it incorporates proper breathing and uses your own body weight to build strength
- Strength exercise balls, weights, and yoga
Prophylactic Mesh Placement For Prevention Of Incisional Hernia After Open Bariatric Surgery
In a systematic review and meta-analysis, Dasari and colleagues examined if mesh prevents post-operative incisional hernia in open and laparoscopic bariatric surgery patients. A total of 7 studies met inclusion criteria. These investigators abstracted data regarding post-operative IH development, surgical site infection, and seroma or wound leakage and performed a meta-analysis. The prophylactic mesh group had significantly decreased odds of developing IH than the standard closure group . No included studies evaluated outcomes after prophylactic mesh during laparoscopic bariatric surgery. The authors concluded that prophylactic mesh during open bariatric surgery appeared to be beneficial in reducing post-operative IH without significant increasing the odds of surgical site infection or seroma or wound leakage. Moreover, they stated that higher quality studies, including those in laparoscopic patients, and cost-utility analysis, are needed to support routine use of this intervention.
Read Also: Therapist That Accept Medicaid Nyc
Medicaid For Weight Loss Surgery
When it comes to using Medicaid for weight loss surgery, things get a little tricky. Why do you want to undergo weight loss surgery? Obvious reasons aside, your insurance company is going to want to see that you have done everything possible to take care of your weight, before undergoing weight loss surgery. You need to build a case for your insurance company that shows them you have a life-threatening disease that needs to be addressed to continue living a full and happy life. Start gathering your medical history. Have you tried other weight loss methods with no success? Your insurance will want a list of tried and failed methods. Read our Writing a Medical Referral Letter Blog.
Many insurance companies will require that you have proof that you have been clinically obese for at least 5 years before you can undergo surgery. Most insurance companies will also except a letter of medical necessity from a bariatric surgeon, such as Western Bariatric Institute. Visit our Steps to Surgery to see how we prepare our patients for surgery and what you will need to do to get started with our bariatric surgery program.
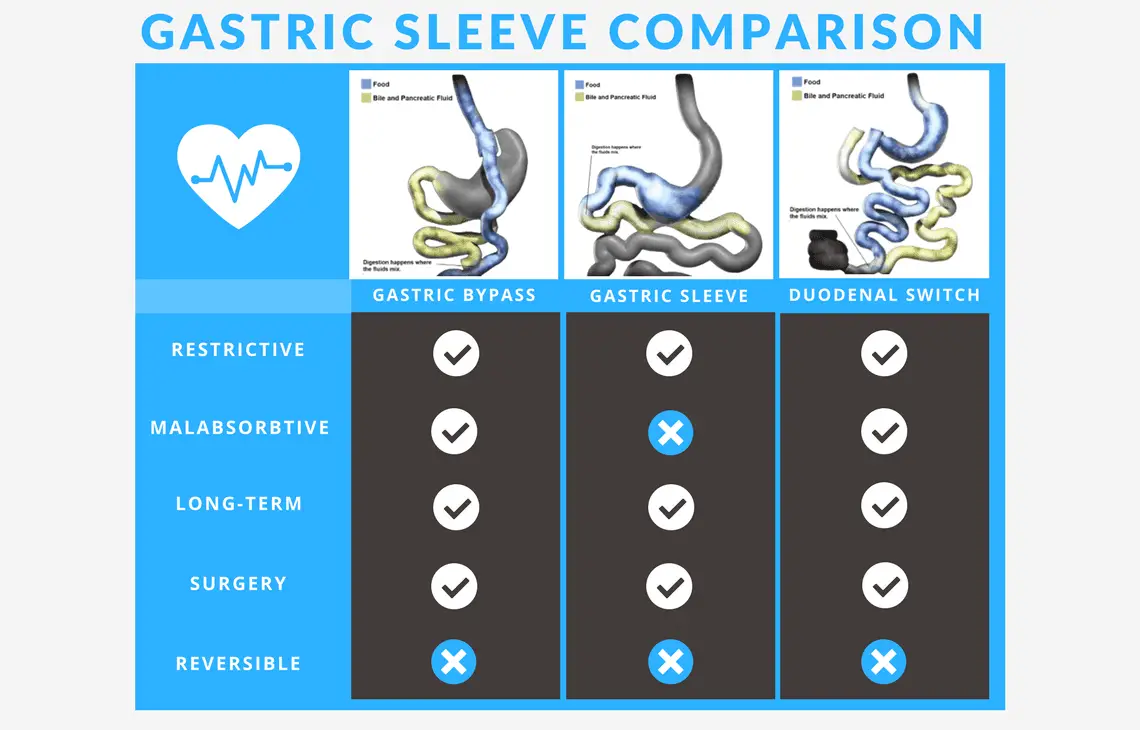
Malabsorptive + Restrictive Approach
Some procedures are both malabsorptive and restrictive. These include biliopancreatic diversion with duodenal switch and roux-en-Y gastric bypass.
Biliopancreatic diversion with duodenal switch involves removing a portion of the stomach.
Roux-en-Y gastric bypass reduces the stomachs size to a small, gastric pouch that is usually about 30 mL in size.
Medicare doesnt cover some treatment and surgical approaches related to weight loss. Treatments that may not be covered include:
- gastric balloon
- open or laparoscopic sleeve gastrectomy
- open or laparoscopic vertical banded gastrectomy
- supplemented fasting to treat obesity
- treatments for obesity alone
Medicare also doesnt usually cover new or experimental procedures. Coverage decisions are based on rigorous scientific data, which must prove that any new procedures are safe and effective, as well as medically necessary for its beneficiaries.
If youre not sure if Medicare will cover a weight loss procedure, contact Medicare directly or your plan provider to determine if its covered and how much it will cost.
Medicare will cover weight loss surgeries if your doctor recommends the procedure based on medical necessity. There are certain criteria that you need to meet to prove the procedure is medically necessary, such as:
Your doctor may also have additional requirements for surgery. Because weight loss surgery is a life-changing process, you may be required to participate in counseling sessions and/or psychiatric evaluations.
Recommended Reading: Dentist In Lafayette That Accept Medicaid
