States With The Most And Least Medicaid Coverage
Having reliable and affordable healthcare is more important now than ever as the U.S. faces the COVID-19 pandemic, and as of September 2020, over 70 million individuals were enrolled in Medicaid. President Joe Biden is also looking to expand the program, and is moving to get rid of requirements for people to work in order to receive coverage, which certain states approved during the previous administration.
Regardless of partisan ideas about how expansive Medicaid should be as a whole, its a fact that some states rely on Medicaid coverage more than others do. To find out the states where Medicaid is most prevalent, WalletHub compared the 50 states across 12 key metrics in three overall categories. Our data set ranges from total Medicaid spending per low-income population to adult care quality to the eligibility level of children.
Medicaid Coverage by State
| 50 | 43 |
Note: With the exception of Total Score, all of the columns in the table above depict the relative rank of that state, where a rank of 1 represents the best conditions for that metric category.
What To Do If You Don’t Qualify For Medicaid
If you don’t qualify for Medicaid, you can possibly get subsidized health care through the Obamacare marketplaces during a special enrollment or open enrollment period. Americans who making more than 100% of the FPL qualify for a premium tax credit that can significantly lower the cost of a plan.
Federal open enrollment for 2022 health care plans runs until Jan. 15, 2022, though some state exchanges are open longer. Learn 2022 open enrollments dates by state. Healthcare.gov, the federal exchange, usually opens from November 1 to December 15 each year.
If you can’t find affordable health care on your marketplace during open enrollment, you have a few back-up options.
These include:
Short-term health insurance: Originally designed to prevent short-term health insurance gaps, these plans are cheaper, but much less comprehensive than traditional coverage. They don’t have to cover Obamacare’s 10 essential benefits or pre-existing conditions. Following changes by the Trump administration, short-term health plans can last from three months to potentially three years, though som estates have stricter limits.
Limited benefit plans: These plans cover a very small portion of the costs associated with certain “medical events,” like a doctor’s visit or ambulance ride. Both the number of events and dollar amounts covered are capped.
Option : Change The Aca To Open Up The Exchanges
A fourth idea, Rudowitz says, is to change the law to remove the minimum cutoff for the private health insurance exchanges, since “right now, individuals who are below poverty are not eligible for subsidies in the marketplace.” With this option, states wouldn’t be paying any of the costs, since the federal government pays premium subsidies, Rudowitz says, but “there are issues around beneficiary protections, benefits, out-of-pocket costs.”
What’s next: This idea hasn’t yet been included in any current congressional bills.
Also Check: Does Medicaid Cover Root Canals For Adults
Medicaid And The Covid Pandemic
As noted above in the section about work requirements, the Families First Coronavirus Response Act essentially prevents states from making their eligibility standards any more strict during the COVID emergency period than they were as of the start of 2020.
Section 6008 of the FFCRA provides states with a 6.2 percentage point increase in their federal Medicaid matching funding for the duration of the COVID public health emergency period, as long as the state Medicaid program:
- keeps its eligibility standards no more restrictive than they were at the start of 2020,
- does not raise premiums above the levels they were at in January 2020,
- provides no-cost coverage for COVID testing and treatment,
- does not terminate enrollees coverage for the duration of the COVID emergency period, unless they move out of the state or request that their coverage be terminated.
CMS previously interpreted this last point to mean that in order to receive the increased federal Medicaid funding, a state must keep beneficiaries enrolled in Medicaid, if they were enrolled on or after March 18, 2020, with the same amount, duration, and scope of benefits, and that states could not subject such beneficiaries to any increase in cost-sharing or beneficiary liability for institutional services or other long-term services and supports during this time period.
A Look At Medicaid Programs In Calfornias Neighboring States
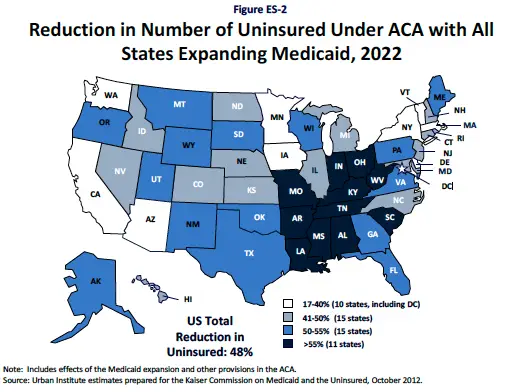
Similarly to California, five states expanded Medicaid access to include low-income adults also. Those states are Illinois, North Dakota, Ohio, Oregon and Pennsylvania. Many of Californias neighboring states also expanded access to their programs, including:
- Oregon: Oregon expanded access to low-income adults but also has programs for normal populations. The state also has medical marijuana and programs to help with substance drug and alcohol abuse.
- Nevada: Nevada expanded access for all households below the 138% FPL threshold.
- Washington: Washington grants access to adults with financial hardships regardless if they have children or other dependents. Income levels vary by household size.
- Arizona: Arizona expanded access to adults whose income levels make them ineligible for other programs, but they must earn less than 133% of the FPL. The program also offers low premiums and coinsurance rates for adults who earn more than 106% of the FPL.
Recommended Reading: How Can I Check The Status Of My Medicaid
How Does Medicaid Expansion Benefit Hospitals
As expected, Medicaid expansion greatly benefits hospitals all over the country. If a patient comes in uninsured and unable to pay, chances are the hospital may never be able to collect on the bill. No matter how efficient the hospitals billing processes may be, a hospital will very rarely receive reimbursement from people who dont have money to pay in the first place. While payment plans may help, enrolling people in those plans still lengthens the reimbursement process. As a result, hospitals may increase their medical charges so that people who can pay more might cover the gap of lost revenue. All of this takes time, effort, and resources, none of which guarantees a win-win solution to offset bad debt effectively.
In addition, rural hospitals in non-expanded states, specifically those in the Midwest and Texas, have also seen a higher rate of closure than rural hospitals in expanded states. Not only that, the loss of rural hospitals is directly associated with a higher rate of mortality and reduced patient satisfaction. Why? Loss of rural hospitals mean that patients in smaller towns have longer distances to the nearest medical facility. In effect, they are more likely to delay care or avoid medical attention, which may lead to worsened symptoms. All in all, this affects not just the hospitals, but the health of small towns in general.
States With The Best Medicaid Benefit Programs
by Adam Johnson| June 16, 2020
Key findings:
- The 14.7% unemployment rate has left many Americans seeking Medicaid benefits.
- Nationally, 21% of people receive Medicaid benefits.
- New York, New Hampshire and Wisconsin were found to provide the best Medicaid programs in the country.
- States with the best Medicaid programs spend 65% more per person than bottom-level states.
- Top-end states fund their Medicaid programs with higher rates of state-provided funding.
- 29% of people in Medicaid expansion states became eligible with expansion under the Affordable Care Act.
As U.S. unemployment rose to 14.7% in April, millions of Americans are seeking unemployment benefits through Medicaid. Medicaid is notoriously underfunded at both the federal and state levels however, some states are capable of providing better Medicaid benefits than others. We here at QuoteWizard analyzed Kaiser Family Foundation data on Medicaid costs and funding to see which states offer the best Medicaid benefits. We evaluated three factors to determine each states capacity to deliver the best Medicaid benefits.
Each ranking factor was analyzed to compile a composite score determining each states overall capacity to provide the best Medicaid benefits.
| Rank |
|---|
Recommended Reading: Does Missouri Medicaid Cover Assisted Living
Nys Medicaid Otc Formulary And Prescription Drug Coverage
The NYS Medicaid formulary is very comprehensive the PDF is 659 pages long! NYS Medicaid providers are expected to select the cheapest option of any drug they prescribe to a New York Medicaid beneficiary. In most cases, this means that the generic form of the drug will be selected. If you notice that your doctor prescribes a brand-name drug, ask and make sure that it is the most affordable option. NYS Medicaid may cover brand-name drugs as well, but generic options are almost always cheaper. Generic drugs usually provide the same benefits as their brand-name counterparts.
In some cases, New York Medicaid may provide reimbursements for over-the-counter products as well. To get that reimbursement, your doctor will need to provide a fiscal order, which is sort of like a prescription for over-the-counter drugs and products.
Work Requirements For States That Have Expanded Medicaid:
Work requirements that were in effect in early 2020 but have since been suspended/withdrawn:
- Michigan 80 hours per month . A federal judge overturned the states Medicaid work requirement in early March 2020, so residents are not currently required to comply with it.
- Utah beneficiaries are exempt from the community engagement requirement as long as theyre working at least 30 hours per week. And there are numerous other exemptions for various populations. But people who werent exempt had to comply with the states community engagement requirements. This involved creating an account on jobs.utah.gov, completing an online evaluation and workshops, and applying for at least 48 jobs within a three-month period.
Medicaid expansion states where new governors withdrew pending work requirements:
Expansion states where work requirements were approved by HHS under the Trump administration but never took effect :
Medicaid expansion states with pending work requirement proposals :
Lawmakers in Louisiana considered several work requirement bills in 2018, but none were enacted. Lawmakers in Pennsylvania passed Medicaid work requirement legislation in 2017 and again in 2018, but Governor Tom Wolf vetoed both bills.
Lawmakers in Alaska considered Medicaid work requirement legislation in 2019, but the measure did not advance to a vote.
Also Check: Does Medicaid Cover Substance Abuse Treatment
Health Plan Report Cards
People across Texas shared their thoughts about their health plan, and rated them, one to five stars, on the services their plan provided.You can compare plans using the overall ratings or by looking at the services that matter the most for you and your family.
You can view the report cards on the Managed Care Report Cards page. Click the program you are enrolled in and find your service area to see plans available to you.
Which Medicaid Plan Is Best In Florida
Each Medicaid plan in Florida comes with the same core benefits which are listed here. You can also compare the performance data for the various plans in your area by using what is known as the Medicaid Health Plan Report Card. You will also have to consider things like the types of services that might be needed along with how many doctor visits that will be necessary, the plan that is accepted by your doctors, the types of doctors you will need, and what extra benefits will meet your needs.
Also Check: How Do I Add My Newborn To My Medicaid
History Of Medicaid Expansion
As noted at the start of this summary, Medicaid was a cornerstone of ACA lawmakers efforts to expand access to healthcare. The idea was that everyone with household incomes up to 133% of the federal poverty level would be able to enroll in Medicaid.
People above that threshold would be eligible for premium tax credits in the exchanges to make their coverage affordable, as long as their income didnt exceed 400% of the poverty level. The idea was that people with income above 400% of the poverty level would be able to afford coverage without subsidies, but that has not proven to be the case. So the American Rescue Plan temporarily eliminated the income cap for subsidy eligibility, and the Build Back Better Act aims to extend that for several more years.
Because Medicaid expansion was expected to be a given in every state, the law was written so that premium subsidies in the exchange are not available to people with incomes below the poverty level. They were supposed to have access to Medicaid instead.
Quality Total Points: 3333
- Adult Care Quality : Full Weight Note: This metric measures performance rates on frequently reported health care quality measures in the CMS Medicaid Adult Core Set.
- Medicaid Denial Rate for In-Network Claims by Healthcare.gov Issuers: Full Weight
- Transparency in Reporting Quality Measures: Full Weight Note: This metric measures the share of voluntarily reported sets of core measures showing the quality of care and health outcomes for adults participating in Medicaid, and children enrolled in Medicaid and the Childrens Health Insurance Program .
Also Check: Medicaid Cost Sharing With Medicare
Medicaid Program Variations By State
States determine their own standards for how to run the program, as long as they follow federal regulations, including who is eligible for services, what services can be covered by Medicaid and how hospitals and doctors will receive payments from Medicaid recipients, among other rules and requirements.
Because states have their own rules they determine eligibility and income requirements. In most state programs, pregnant women, children, seniors and disabled persons are almost always eligible for services. And generally, to be eligible for Medicaid your household income must fall below 138 percent of the federal poverty level .
Who Can Get Medicaid
Many people with low incomes would be unable to afford health insurance without government assistance. This is where Medicaid comes into play. The U.S. Department of Health and Human Services determines the federal poverty level every year, and these values are used to set the eligibility standards for Medicaid.
All states cover certain categories of people, including low-income families, children, pregnant women, the elderly, and people with disabilities. The federal government sets the standard, but individual states can choose to expand coverage beyond these limits, such as to all individuals below a certain income level. States can increase income thresholds to include more people. You can learn more information about what your state program covers on the Medicaid.gov website.
Don’t Miss: How To Get Help With Medicaid
States That Expanded Medicaid 2021
The Affordable Care Act that was enacted in 2010 under former United States President Barack Obama was designed to give more Americans access to affordable healthcare. Under this expansion, households with incomes up to 133% of the federal poverty level would be eligible to receive Medicaid benefits, which provides free healthcare services.
Unfortunately, this isnt universal across all of the states. As of early 2019, a total of 36 states plus Washington, D.C., have received federal funds to expand Medicaid. Additional states are expected to follow suit by the end of 2019. Some states are even working to make changes to the Medicaid program, including buy-in programs and putting lifetime caps in place.
Republican lawmakers pushed for Medicaid work requirements. This means that a person on Medicaid must be working, in school, volunteering, or participating in job training. A total of eight states have received approval from the federal government for work requirements, while other states have put in waivers or may submit them in the future. Work requirements must be approved by the government and vary by state.
As of June 2019, the states that have adopted Medicaid expansion are:
- Alaska
Use The Ny Medicaid Doctors List
The best way to find a doctor in your area who accepts New York Medicaid plans is to use a provider search tool like ZocDoc. You can search by location, name, condition, procedure, or the type of doctor you are looking for. You can also use the official NYS Provider and Health Plan lookup tool to search by health plan, provider, or facility.Back to Top
Don’t Miss: Does Medicaid Cover A Breast Reduction
Virginias Requirements For Medicaid Qualification
Eligibility requirements for Medicaid have to be met before you can qualify for the program. To be eligible for Medicaid in Virginia, you have to belong to one of the designated patient groups. Without this qualification, you will not be eligible for the program. Those medical groups are:
- Children
- Parents or caretakers of relatives
- Adults between the ages of 21 and 64 who suffer from a mental illness
- Other adults who qualify
- Adults between the ages of 18 and 26 who are former foster children
You must also be a resident of Virginia who has a valid state ID. You will also need to provide your Social Security number and have documents proving that you are a US citizen. Aside from these things, if you are a former foster child, suffering from a disability or mental illness, you will need to provide documentation regarding these things.
The ‘complex’ Cost Of Health Care
The study factored in the cost of insurance as well.
Utah has the lowest average monthly insurance premium, followed by Idaho, Massachusetts, Maryland, and Minnesota. Alabama, on the other hand, has the highest premiums with Louisiana, West Virginia, Wyoming, and Vermont rounding out the top five.
The cost of health care and pricing is complex and driven by a number of different market variables, Boyd said. In some areas, there is only one hospital. In some areas, there is only one health care system. Both of these have impacts on the cost of health care and insurance premiums. Also, the disease burden is different in different parts of the country which impacts what the premiums are charged.
Access is extremely important in other ways outside of social programs. For example, despite being the second- and third-most populous states in the nation, both Texas and Florida ranked in the bottom 10 for access, which was surprising to Boyd.
Meanwhile, despite its relatively small population, D.C., ranked 13th overall, stood out in several key areas.
The nations capital has the most hospital beds per capita, the most physicians per capita, and the most dentists per capita. Its also among the top five for the highest percentage of insured children aged 0 to 18 and insured adults aged 19 to 64, and for the lowest percentage of adults with no dental visit in the past year.
READ MORE:
Recommended Reading: Does Medicaid Cover Auto Accidents In Michigan
