What To Do If You Don’t Qualify For Medicaid
If you don’t qualify for Medicaid, you can possibly get subsidized health care through the Obamacare marketplaces during a special enrollment or open enrollment period. Americans who making more than 100% of the FPL qualify for a premium tax credit that can significantly lower the cost of a plan.
Federal open enrollment for 2022 health care plans runs until Jan. 15, 2022, though some state exchanges are open longer. Learn 2022 open enrollments dates by state. Healthcare.gov, the federal exchange, usually opens from November 1 to December 15 each year.
If you can’t find affordable health care on your marketplace during open enrollment, you have a few back-up options.
These include:
Short-term health insurance: Originally designed to prevent short-term health insurance gaps, these plans are cheaper, but much less comprehensive than traditional coverage. They don’t have to cover Obamacare’s 10 essential benefits or pre-existing conditions. Following changes by the Trump administration, short-term health plans can last from three months to potentially three years, though som estates have stricter limits.
Limited benefit plans: These plans cover a very small portion of the costs associated with certain “medical events,” like a doctor’s visit or ambulance ride. Both the number of events and dollar amounts covered are capped.
Prescription discount cards: While these cards won’t help you pay for inpatient or outpatient care, they do help you get medication at discounted rates.
When Does Medicaid End For A Child In Nys
The New York State Department of Health website states that Medicaid coverage for children ends at age 18. However, there are exceptions: If you have an Individual or Family Plan through your employer, then Medicaid will continue until you reach 26 years old if you qualify for Supplemental Security Income , Medicaid continues until you become 21 years old.
How To Apply For Medicaid
If youre eligible for Medicaid, you can apply all year round through your state’s Medicaid website or HealthCare.gov, the federal health insurance marketplace. If you apply for Medicaid through Healthcare.gov and it looks like you qualify, the federal government will notify your state agency, which will contact you about enrollment. States also generally let you print out paper applications you can mail, fax or return directly to your local government office.
To complete your Medicaid application, you will likely need to provide documentation that you meet your state’s requirements. This documentation may include:
-
Your birth certificate or driver’s license to serve as proof of age and citizenship
-
Recent pay stubs or tax returns to serve as proof of income
-
Copies of bank statements
-
Proof of address, which could include a lease, utility bill statements or a copy of your mortgage
-
Medical records to serve as proof of disability
States have 45 days to process your Medicaid application. They have 90 days if eligibility is tied to a disability . Processing can take longer if applicants do not supply all of the required documentation. If you don’t qualify for Medicaid, you might be able to get subsidized health insurance through Healthcare.gov. However, only certain life events allow you to apply for a marketplace health care plan outside of open enrollment, which takes place from Nov. 1 to Jan. 15.
Get your finances right, one money move at a time. Sign up for our free ebook.
Read Also: How Can I Check The Status Of My Medicaid
Does My Parents’ Income Affect My Medicaid
Your parents’ income may affect your eligibility to receive Medicaid if:
- You live with them, or
- They could claim as you a dependent on their taxes
If you’re under 19, your parents’ income will affect your Medicaid eligibility as long as you live together. If you’re 19 or older, your parents’ income will affect your Medicaid if they claim you as a dependent on their taxes.
In most cases, Medicaid income eligibility is determined by your Modified Adjusted Gross Income . MAGI is calculated from household size and total household income.
Your MAGI must be less than a set amount to qualify for Medicaid. Using MAGI allows people with larger households to have higher household incomes and still qualify for Medicaid. Income limits are different in every state. For example, in Texas, a three-person household can have a total income of $43,481. In Colorado, the income limit is $29,207.
If your parents are considered part of your household, they will impact your Medicaid eligibility. Although your parents will increase your household size, living together may prevent you from receiving Medicaid if their incomes are too high.
How Much Is The Federal Poverty Level

The federal poverty level in 2021 is equal to an income of $12,880 per year for an individual adult, plus $4,540 for each additional household member. Alaska and Hawaii have different benchmarks because of their differing costs of living.
|
Number of people in home |
48 states and Washington D.C. |
Alaska |
|---|
Also Check: How Do I Find My Medicaid Number Online
What Is The Supplemental Nutrition Assistance Program Snap
Eligibility for SNAP
- The gross monthly income must be equal to or fall under 130 percent of the national poverty line, about $25,400 a year or $2,116 a month for a household of three for 2014. The elderly or disabled are not required to meet this limit to receive food stamps for seniors.
- Monthly net income, applied for specific items like childcare and housing cost, must be equal or fall below the poverty line of $19,600 a year, or $1,626 a month for a household of three for the year 2014.
- The assets for each household must fall below certain amounts: households without the disabled or elderly must not own assets above the value of $2,000, and those with disabled or elderly family members must not own assets above the value $3,250.
How Can People Apply for SNAP?How Much Does SNAP Cost?How Efficient and Effective is SNAP?Additional References
Can A Non Citizen Get Medicare
Specifically, you will qualify for Medicare even if you are not a U.S. citizen if you qualify to receive or currently receive Social Security retirement benefits, Railroad Retirement Benefits , or Social Security Disability Insurance . In any of these cases, you will qualify for premium-free Part A.
You May Like: Louisiana Medicaid Provider Enrollment Portal
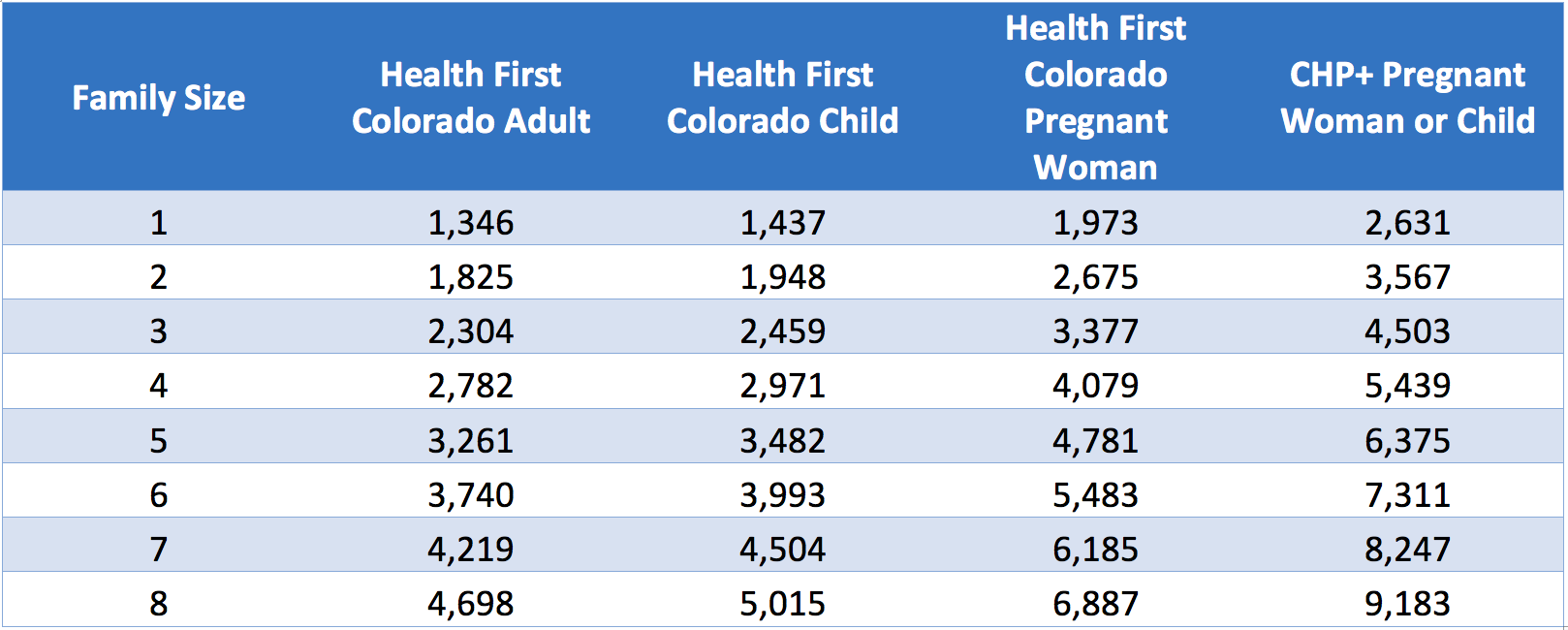
See If You Can Sign Up For Child Health Plan Plus
Who Qualifies?
- Children age 18 and under and pregnant women age 19 and over
- Applicants with household income under 260% of the Federal Poverty Level . See the CHP+ Income Chart for details
- Lawfully present children and pregnant women with no five-year waiting period
- Children and pregnant people not eligible for Health First Colorado
- Children and pregnant people who do not have other health insurance
| Family Size |
When Does Medicaid End For A Child
Do you know? When does Medicaid end for a child? If not, this article is for you! Medical assistance for children, unlike Medicare coverage for seniors, is not permanent. One of the most important things to know about Medicaid for kids is when it will end. Medicaid coverage for children lasts until the child turns 18 years old, or until they are no longer a full-time student. The Medicaid coverage will then be converted into an affordable health insurance plan that can be purchased in the marketplace with help from government subsidies.
Don’t Miss: How To Apply For Pregnancy Medicaid In Nc
Signing Up For Medicaid When Youre Unemployed
If you have recently found yourself unemployed, you could be eligible for Medicaid. Most states applications include a box you can check if you have lost your former income from work, which alerts the program workers that your past income figures might not be an accurate guide to your present eligibility. To be on the safe side, you should let your intake worker know about your employment status at the time you submit the application, or you can tell a worker about your situation during the initial telephone interview.
The intake worker you speak with may require some kind of verification that you are unemployed before approving the application. This may be done over the phone or by submitting a written statement from your former employer that indicates you no longer work for them.
Unlike an unemployment insurance claim, the specific reason your employment ended is not relevant to your application for Medicaid, and so you could potentially be approved for health coverage even if you have been denied unemployment compensation.
Can I Get Medicaid If I Live With My Parents
- Find out when you can get Medicaid if you live with your parents. Learn how tax filing status, household income and household size affect Medicaid benefits.
Many adults share a home with their parents. These living arrangements can be convenient and sometimes even necessary for families. Sharing a home can help you save money or care for aging parents. However, living with other people can impact the availability of some benefits. Medicaid for children and teenagers is also affected by how much their parents earn. Regardless of your age, you may be wondering if you can get Medicaid while living with your parents.
Don’t Miss: Medicaid Health And Human Services
Health Insurance Discount Cards
Health insurance discount cards give members access to negotiated low-cost healthcare. They’re not insurance plans but rather an option you might want to explore as a last resort.
You’ll pay a small monthly fee and get a discounted rate on your services when you go to a doctor or hospital. You’ll still end up paying all your medical costs, but at least you’ll pay less.
Interactions Between Snap And Medicaid At Renewal

Prior to the ACA, many states conducted joint renewals for SNAP and Medicaid. They often had households return a single renewal form along with supporting information and evaluated continued eligibility for both programs. States now find it more challenging to conduct joint renewals because the renewal processes differ in key areas:
- In SNAP, households lose eligibility at the end of their certification period unless they reapply and re-establish eligibility. The household must provide information showing that it still meets the eligibility requirements and submit a signed application form.
- In contrast, Medicaid approaches renewals from the perspective that the participant is likely still eligible, and the state agency uses available data to confirm ongoing eligibility or call eligibility into question. Many participants dont have to return a form to renew their coverage.
Although the ACA widened the differences between Medicaid and SNAP in this area, it also provided an impetus for greater integration. Medicaid regulations now specify SNAP as a data source that states can use for Medicaid eligibility determinations. Further, the ACAs enhanced funding for integrated technology systems recognizes the overlap between these programs and the significant opportunity to modernize states overall benefit delivery systems. As states modify their eligibility systems, they can expand coordination between Medicaid and SNAP.
Also Check: How To Get Approved For Medicaid In Florida
Read Also: Am I Eligible For Medicaid In Ohio
Taking Advantage Of Magi
The Affordable Care Act simplified Medicare eligibility and enrollment for millions of Americans. Using MAGI for eligibility simplified the application process. The administrative burden of confirming assets was put to the wayside. Unfortunately, it also gave wealthy people the opportunity to take advantage of taxpayer dollars.
This loophole occurs because the majority of Americans now qualify for Medicaid through MAGI, which unless you are seeking long-term nursing home care no longer uses the asset test. People who are asset rich, particularly those who have investments or real estate properties, can still technically meet MAGI criteria.
Someone could own a home worth $850,000, a Lamborghini, a second vehicle, hundreds of acres of farmland, and still technically be eligible for Medicaid.
These Americans would be considered wealthy by any standards but by sheltering their net worth under the current tax laws, they would be legally eligible for Medicaid or subsidized plans through the Health Insurance Marketplace. This is the case even when they could easily dip into their assets to pay for health insurance.
If the intent is to provide health care to the most financially needy, MAGI Medicaid may need to consider how it addresses this loophole. The GOP is currently looking to repeal Obamacare which would, in effect, put an end to MAGI Medicaid altogether.
Can The Unemployed Get Medicaid
People who have lost their jobs, for whatever reason, may be eligible for health coverage through Medicaid. Medicaid provides basic health insurance for tens of millions of Americans with a limited ability to pay. Unemployed workers who have lost their income may be able to sign up for the healthcare services Medicaid provides, even if they were not eligible for coverage while employed.
Losing a job can be difficult, regardless of the reason. Apart from the loss of your former stable income, you might find yourself without the health insurance you counted on to protect yourself and your family. Many people who find themselves out of work wonder how they can keep their families covered until a new job comes along. Fortunately, Medicaid offers basic health services to people with medical needs and financial limits that make it difficult to pay. Not everyone is eligible for coverage, however, and your former income could complicate your income verification during the application process.
You May Like: Is Medical Marijuana Covered By Medicaid
When Does Medicaid End For A Child In The United States
The Medicaid program is a federal and state partnership that provides health coverage to eligible low-income children, pregnant women, parents, and people with disabilities. The Affordable Care Act established a Medicaid expansion to cover all adults with incomes up to 138% of the federal poverty level.
Children can remain covered until they turn 19 years old or until they become disabled or pregnant.
Do I Have To Be A Us Citizen To Get Medi
No. U.S. Citizenship and immigration status is not a condition of eligibility.
Assuming all eligibility requirements are met, U.S. citizens, and individuals with Satisfactory Immigration status are entitled to receive full-scope Medi-Cal benefits.
Additionally, undocumented eligible adults will have access to Emergency and Pregnancy-related services.
Furthermore, in the state of California, all eligible children are entitled to receive full-scope Medi-Cal benefits, regardless of immigration status.
Recommended Reading: How To Report Medicaid Fraud
How Do You Calculate Your Medicaid Income Eligibility
Follow these steps to calculate whether or not your income may qualify you for Medicaid:
- Find the FPL for your household using the chart above
- Multiply that number by your states Medicaid income limit found below, and then divide by 100
For example, if there are two people living in your household and you live in Arizona, you would multiply $17,420 by 138 and then divide by 100. That equals $24,039.60.
You may also multiply $17,420 by 1.38.
When Does Medicaid End For A Child In Virginia
There are many situations when people may need Medicaid to help with medical costs. Perhaps the most common situation involves children who are eligible for Medicaid if they have a household income below the federal poverty level. A child will no longer be eligible for Medicaid in Virginia if they exceed these limits. The Virginia Medicaid program will continue coverage until the child turns 19 years old.
Don’t Miss: Dentists In Grand Island Ne That Accept Medicaid
Maximum Monthly Amounts On Food Stamps
There is a maximum monthly allotment based on the size of the household. When determining your benefit allotment, they will take your net monthly income and multiply it by 30%. That number will then be subtracted from the maximum monthly allotment. The remaining amount is the total monthly allotment you will receive based on your application. This amount may change if your income or household size changes.
SNAP benefits are a specific money amount provided to recipients each month to go towards nutritional foods. Recipients are provided with an electronic benefits transfer card, and money is added to the card each month. You can check your balance by phone, and any unused funds at the end of the month remain on the card to be used to following month. Once allocated, benefits will not expire.
Benefits can be used to buy food and drinks at most grocery stores, convenient stores, gas stations, pharmacies that sell food, and farmers markets. Benefits cannot be used to buy alcohol, tobacco, medicine, hot food, food meant to be eaten in the store, or any non-food items.
Other Help For The Unemployed
Medicaid is not the only resource you might be eligible for if you have lost a job. Apart from your states unemployment compensation program, you could benefit from a range of support services intended to help financially struggling people get by until another job opens up. Programs you might consider looking into include:
- SSI/SSDI
- SNAP, also called food stamps
- TANF, also called cash aid or welfare
- WIC nutritional support for young children
- County or state job placement assistance or retraining services
- Emergency food or housing vouchers
- Low-Income Housing Assistance, formerly called Section 8
Fortunately, many of these programs are administered by the same health and human services office that takes your Medicaid application. If you are recently out of work, speak with a worker in this office about the various programs you may qualify for. Often, approval for Medicaid or another low-income support program makes you automatically eligible for other programs with similar enrollment criteria.
Read Also: Pediatricians In Amarillo Tx That Accept Medicaid
The Food Stamp Program And Income
Next, we turn to the contribution of FSP benefits to household income. For this purpose we continue separate analysis by age and further differentiate between recipients living alone or with spouses only and SSI recipients living with others. Table 3 provides a sense of the reliability of estimates for various subgroups by reporting sample sizes and the estimated number of SSI recipients for various subgroups in 2004. Some of the subgroups are so small that the results are meaningless. However for subgroup samples that are large, results can be viewed with considerable confidence.
Table 3. SSI recipients in food stamp recipient households, by living arrangements and benefits, fiscal year 2004| SSI recipient characteristic |
|---|
| NOTES: SSI = Supplemental Security Income OASDI = Old-Age, Survivors, and Disability Insurance. |
| a. Too few observations for meaningful calculations. |
| SSI recipient |
|---|
| NOTE: SSI = Supplemental Security Income. |
| a. Too few observations for meaningful calculations. |
| SSI recipient characteristic |
|---|
