Do I Qualify For Medicaid
Medicaid provides free or low-cost health coverage to some low-income people, families and children, pregnant women, the elderly, and people with disabilities. Many states have expanded their Medicaid programs to cover all people below certain income levels. Medicaid qualifications depend partly on whether your state has expanded its program.
Newly Eligible For Medicaid Choose First Choice
If Healthy Connections determines you are eligible, and you are new to Medicaid, you need to choose a health plan or one will be assigned to you. South Carolina Healthy Connections Choices manages the health plan selection process. Learn more about Healthy Connections Choices and enrolling in First Choice. Or, go to the Healthy Connections Choices website to pick a plan.
Learn About Requirements For Medicaid In South Carolina
Medicaid eligibility requirements in South Carolina provide a path for low-income families and other needy individuals to get assistance in the form of health care coverage. Understanding how to qualify for Medicaid makes it possible for applicants to take advantage of the program, which is known as Healthy Connections in South Carolina. The process to qualify for Medicaid is established in part by the federal government, which works in tandem with the state to fund and operate Medicaid for the population. The benefits of Medicaid are numerous, but for individuals or families to take advantage of the system, they must meet several provisions that include legal status in the country, income levels and more. Learn more about SC Medicaid benefits eligibility guidelines by reading through the information provided on this web page.
Who qualifies for Medicaid in South Carolina?
The Medicaid eligible groups listed above are just some examples of those who may qualify for Medicaid benefits. Medicaid eligibility requirements were expanded under the Affordable Care Act Medicaid expansion. However, South Carolina has yet to accept the Medicaid expansion guidelines outlined in the ACA.
What are the requirements for Medicaid in South Carolina?
- Candidates must fall within any established income thresholds.
- Candidates must provide proof of permanent residency in South Carolina.
- Candidates must provide proof of citizenship or legal immigration status.
Read Also: Https Portal Mmis Arkansas Gov Ar Medicaid Member
How Do I Apply For Medicare In South Carolina
Most people are automatically enrolled in Medicare Part A, but youll have to enroll in Part B. You can at your local Social Security office, the Social Security website, or by calling 1-800-772-1213 . If you are a Railroad Retirement Board member, call the RRB directly to apply for Medicare in South Carolina at 1-877-772-5772 . If you want more coverage than A and B, those plans are offered by private insurance companies. Our agents can help you if you want Medicare Advantage instead of Original Medicare.
What Services Are Covered
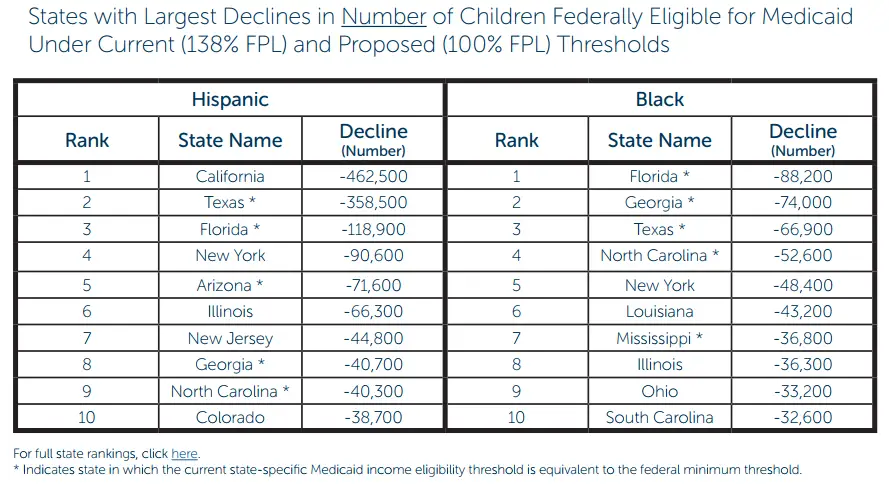
There are certain services that Medicaid must cover. States can choose to cover more services. The federal law does not require states to provide additional services under Medicaid though.
In addition, if a child is diagnosed with a medical condition, she has the right to treatment under the Medicaid EPSDT program.
Read Also: What Is The Medicaid Gap
What Does South Carolina Medicare Cost
While your costs may be different based on the plan options you choose, the Part A and Part B costs are standardized. If you worked and paid your Medicare taxes for at least 39 quarters , you can qualify for premium-free Part A. If, however, you only worked and paid your Medicare taxes for 30-39 quarters , youll have to pay $240 per month in 2019. If you paid Medicare taxes for even less than 30 quarters, youll have to pay $437 per month. Most Medicare Part A beneficiaries will face coinsurance for hospital stays. In 2019, the cost is $341 per day for the first 90 days, and then $682 per day.
The 2019 standard premium for Part B is $135.50 per month, but that amount can change based on your income. The standard deductible is $185 per year.
Am I Eligible For Wic
Need help? If you have difficulty understanding English or have a disability, free language assistance or other aids and services are available upon request. Please contact your local WIC clinic.
WIC is a free program that provides healthy foods and nutrition and health services to South Carolina families who qualify. WIC is for all types of families.
If you are a father, mother, grandparent, foster parent, or other legal guardian of a child under 5, you can apply for WIC for your child.
If you currently receive Medicaid, TANF, or SNAP, you already meet the income eligibility requirements.
To qualify for WIC services, participants must:
- Be a child under 5, a new mom, or a pregnant or breastfeeding mom
- Live in South Carolina
Don’t Miss: Not Reporting Marriage To Medicaid
What Does South Carolina Medicare Cover
Original Medicare in SC includes Part A, hospital coverage, and Part B, medical coverage. Part A provides coverage for hospital, nursing home, hospice, and home health services. Part B provides coverage for preventative doctor visits, emergency transportation, x-rays and labs, mental health, and durable medical equipment. Once you have A and B, youll need to add a form of prescription drug coverage. You can do this through a prescription drug plan or through a Medicare Advantage or Medicare Supplement plan that includes prescription drug coverage.
Helping You Stay Healthy Is Important To Us
We cover all medically necessary Medicaid-covered services for our Humana Healthy Horizons in South Carolina members. These services should:
- Meet your medical needs as ordered by your healthcare provider
- Help you achieve age-appropriate growth and development
- Help you attain, maintain, or regain functional capacity
Your includes a full list of your benefits and information about what your medical plan covers.
Read Also: What Type Of Health Insurance Is Medicaid
Can I Have Medicare And Medicaid In Sc
If you qualify for Medicare in South Carolina but also meet the income requirements for SC Medicaid, you can get benefits from both programs. If you qualify for a DSNP , you can enroll in a Medicare Advantage plan during almost any time of the year instead of waiting for the Annual Enrollment Period to come around every fall. Your DSNP can make your Medicare coverage more affordable by covering your premiums, deductibles, and/or coinsurance and co-payments.
Other Scdhhhs Programs For Families Enrolled In Medicaid
The HIPP Program was created to assist families of Medicaid beneficiaries with the cost of health insurance that covers the client. The goal is to help beneficiaries maintain their private insurance to ensure Medicaid payment as a last resort. Private plans pay first for medical services and Medicaid is secondary. A program brochure, questions and answers , and the referral form are available on the website. The referral form must be printed, completed and submitted to the address on the form.
Also Check: Mosquito Repellent Covered By Medicaid
Why Choose Humana Healthy Horizons
We designed Humana Healthy Horizons to provide you with the care and support you need so you have more time to focus on what you love. Now more than ever, your health and healthcare coverage are important. Humana Healthy Horizons makes available to South Carolina Medicaid members access to the high-quality you want and extras you need.
We have easy ways for you to find a doctor or a specialist. We can send your medicines to your home, so you dont have to go to a pharmacy. And along with your medical care, you get:
- Behavioral and emotional health coverage
- Hearing, prescription, and vision coverage
- Digital tools to help you manage your health care
Here are some things you should know about Medicaid enrollment in South Carolina:
Medicare Savings In South Carolina

Looking for South Carolina Medicare savings? We can help you figure out if youre eligible for any cost savings. We can help you set up a free appointment with an agent in your area who can come to your home and help you sort through your options.
If youre looking for a way to save money on your premiums, copayments, and coinsurance, get in touch with us at Medicare Plan Finder. We can help you find out if you are eligible for cost savings.
To get started, give us a call at 833-GET-ENROLLED .
Read Also: How Does A Person Get On Medicaid
Where Do I Look For Help With Healthcare
Various programs may provide assistance depending on the situation. Several state programs may be able to provide services based on area of need. Grant opportunities can help pay for care not included in state programs and not covered by insurance. The programs listed here may provide health care assistance, either by providing health care or through financial assistance.
Who Can Get Medicaid
- No matter your state, you may qualify for Medicaid based on your income, household size, disability, family status, and other factors. But if your state has expanded Medicaid coverage, you can qualify based on your income alone.
- Enter your household size and state. We’ll tell you who is eligible for Medicaid, if your state expanded and if you qualify for Medicaid based only on your income.
- If you think you have Medicaid eligibility, you can create an account and fill out a Marketplace application. If it looks like anyone in your household qualifies for Medicaid or CHIP, we’ll send your information to your state agency. They’ll contact you about enrollment. You can apply any time of year.
- If you don’t qualify for Medicaid, we’ll tell you if you qualify for financial help to buy a Marketplace health plan instead.
Read Also: Can You Get Medicaid If You Have Health Insurance
South Carolina Has Not Accepted Federal Medicaid Expansion
- 1,159,844 Number of South Carolinians covered by Medicaid/CHIP as of May 2021
- 345,000 Number of additional South Carolina residents who would be covered if the state accepted expansion
- 105,000 Number of people who have NO realistic access to health insurance without Medicaid expansion
- $2.2 billion Federal money Wyoming is leaving on the table in 2022 by not expanding Medicaid
How To Apply For Medicaid In South Carolina
Medicaid candidates can learn how to apply for Medicaid in South Carolina in order to understand what the process entails. Applicants can discover what a Medicaid application will require, including forms of documentation and information. South Carolina offers several ways to submit a Medicaid application form, from applying online to manually submitting the form. Understanding where to apply for Medicaid is also important, especially with the different options that are offered for South Carolina residents. Applying for Medicaid benefits does not need to be a lengthy or time-consuming process. With just some basic understanding of how a petitioner can apply for Medicaid in SC, the application process will be much smoother than anticipated. To find out more about the Medicaid application process, plus information regarding how to appeal a denial for eligibility, continue reviewing the sections below.
Where do you sign up for Medicaid in South Carolina?
Information Required on the Medicaid Application Form in South Carolina
- Residency status within South Carolina.
- Citizenship or legal non-citizen status in the United States.
- Household income.
Read Also: Does Medicaid Cover Prenatal Care
Medicaid Eligibility Income Chart By State Updated Jul 2022
The table below shows Medicaids monthly income limits by state for seniors. Income is not the only eligibility factor for Medicaid long term care there is also an asset limit and level of care requirements. Additionally, there are state-specific details. Click on the state name below to see that states complete Medicaid eligibility criteria.
The maximum income limits change dependent on the marital status of the applicant, whether a spouse is also applying for Medicaid, and the type of Medicaid for which they are applying. Nursing home Medicaid may have a different income limit than home and community based Medicaid services, and both of those may differ from the Aged, Blind and Disabled income limits.
Exceeding the income limits does not mean an individual cannot qualify for Medicaid. Most states have multiple pathways to Medicaid eligibility, such as a medically needy pathway. Furthermore, many states allow the use of Miller Trusts or Qualified Income Trusts to help person who cannot afford their care costs to become Medicaid eligible. There are also Medicaid planning professionals that employ other complicated techniques to help persons become eligible. Finally, candidates can take advantage of spousal protection laws that allow income to be allocated to a non-applicant spouse.
| Medicaid Eligibility Income Chart Updated July 2022 |
| State |
Medicaid Asset Rules In South Carolina
The general Medicaid eligibility rule is that a person cant have more than $2,000 in countable assets. If you are trying to become eligible for Medicaid to pay long-term care costs, you may need to spend down your assets or use other strategies to qualify.
Exempt Assets
Fortunately, some assets may not be counted for Medicaid purposes. The spouse of a nursing home resident is permitted a higher allowance of assets, and other assets are exempt.
Some personal possessions, one vehicle, and the primary residence may be exempt from the Medicaid asset calculation. However, there are some complex rules that apply, so ask your elder law attorney exactly how these will apply to your case.
If you have countable assets that exceed the $2,000 threshold, you may think that you could just gift them to your kids, but Medicaid has rules about transfers that include severe penalties.
Five-Year Penalty Period
Starting the day you apply to Medicaid, there is a five-year look-back period on any asset transfers you make. If you give away assets and dont receive fair value, you will be penalized.
The penalty is calculated based on the value of the transferred assets and leads to a ban for a certain period of time. If you transfer valuable assets, you could be ineligible for Medicaid for several months or even years.
Income and Estate Recovery
Read Also: Oral Surgeons That Take Medicaid In Michigan
Using Your Healthy Connections Plan
Q. What medical services does Medicaid cover? A. Within certain limits, Medicaid will pay for services that are medically necessary. Examples of services that may be covered include doctor visits, medications, hospital visits, and many other medical services.
If you have any questions about what is covered, to view a chart that shows each health plan and what they cover. You can also contact Healthy Connections toll-free at 1-888-549-0820.
Q. How long will my Medicaid benefits remain active? A. Eligibility for most Healthy Connections programs lasts for 1 year. After 1 year, South Carolina Health and Human Services will review your case annually.
Q. I was enrolled in S.C. Healthy Connections Choices and now am told I must choose between health plans. What should I do? A. The Healthy Connections Choices website offers comprehensive information on its health plans. Members may utilize a Quick Start Guide, search for doctors, compare plans, and more. Please visit S.C. Healthy Connections Choices for more information.
Q. Do I need to tell South Carolina Healthy Connections when I move or change jobs? A. Yes. If you have any changes to your income, resources, living arrangements, address or anything else that might affect your eligibility you must report these changes to Healthy Connections right away at 1-888-549-0820.
Q. What if my Medicaid card is lost or stolen? A. Report a lost or stolen card to Healthy Connections immediately at 1-888-549-0820.
What Is The Coverage Gap
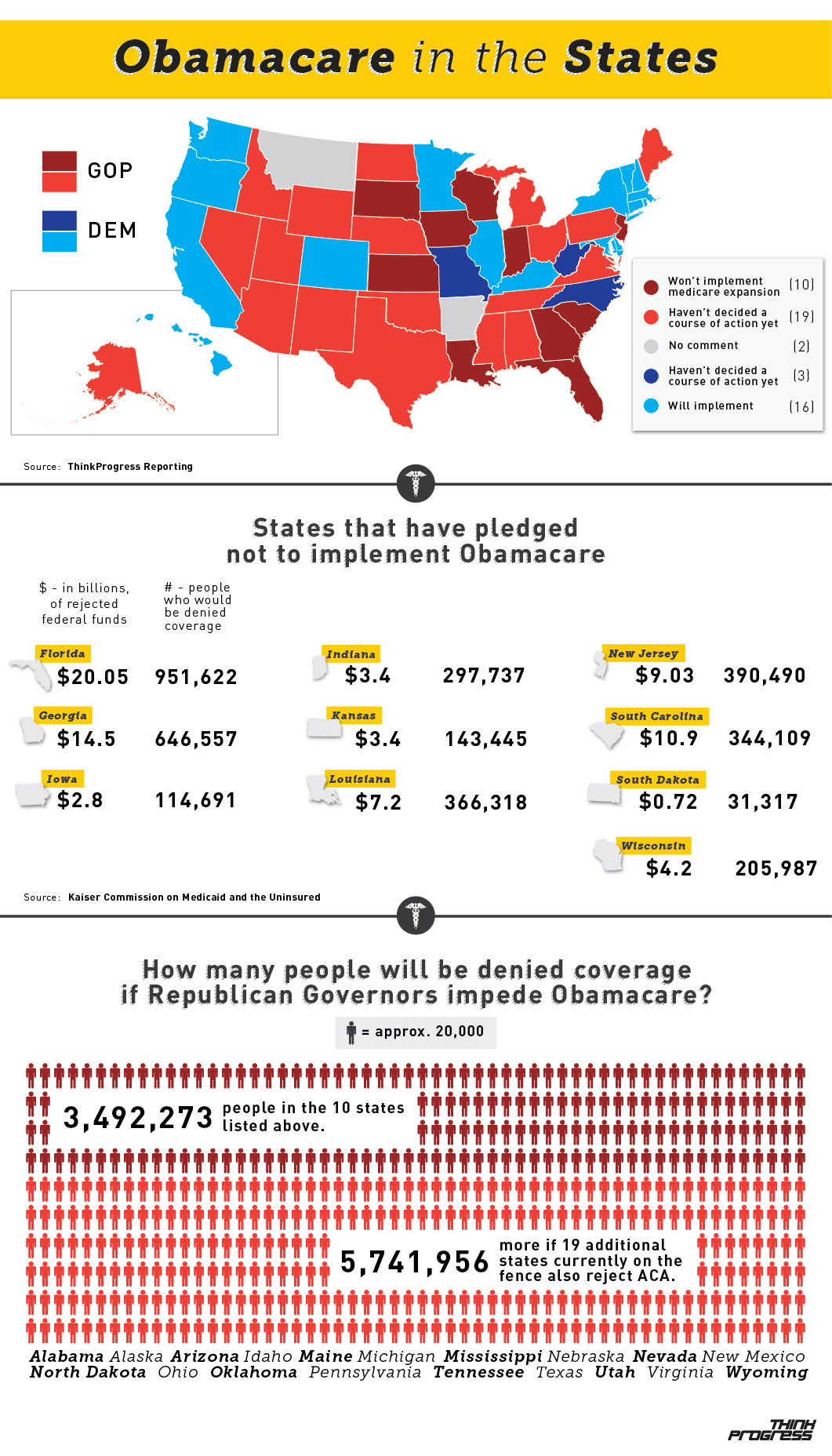
We do have a coverage gap because our state refuses to expand Medicaid. If you are an adult without children or disability, but have low income, you may fall in what is known as the coverage gap. Adults in the coverage gap fall between two zones. On the one hand, they do not make enough money to buy coverage through the Affordable Care Act health insurance marketplace. On the other hand, they also do not meet the minimum requirements for Medicaid under South Carolinas current program.
If we expanded Medicaid, the federal government would pay 90% of your coverage. South Carolina would only have to pay 10% of your coverage. If you were covered, you could get your medicine and doctor visits needed to stay healthy and able to work.
Also Check: Does Idaho Medicaid Cover Vision
How Medicaid Eligibility Is Determined
Income eligibility is determined by your modified adjusted gross income , which is your taxable income, plus certain deductions. Those deductions include non-taxable Social Security benefits, individual retirement contributions and tax-exempt interest. For most people, MAGI is identical or very close to your adjusted taxable income, which you can find on your tax return. Specific income requirements in dollars rise alongside the size of your household.
Our guide focuses on each states major programs for adults. Most are only available to state residents, U.S. citizens, permanent residents or legal immigrants .
Looking for insurance for a child? Check out our guide to the Children’s Health Insurance Program .
Choosing A Medicaid Health Plan
Healthy Connections Choices the health plan selection website for South Carolina Healthy Connections Choices. South Carolina Healthy Connections Choices is a program that helps eligible Medicaid members enroll in health plans.
1-877-552-4642
Watch video clips and find materials that help you choose a health plan and doctor. Find meetings in your area to learn more about the health plans.
Also Check: When Does Medicaid Enrollment Start
District Of Columbia Medicaid
Eligibility overview: Washington, D.C., has one of the most generous Medicaid programs in the U.S., covering adults with household incomes up to 215% of the FPL as part of its expansion program. It also has programs for pregnant, parent/caretaker, elderly, disabled and child residents.
Income requirements: The expansion covers adults without dependents who make up to $2,082 a month when applying on their own. Elderly, blind or disabled D.C. residents are eligible if they make up to 100% of the FPL, or $1,073.33 per month for one individual, and have resources below $4,000 for one person. D.C. also covers pregnant women with incomes up to 319% of the FPL, or $4,703.40 monthly for a two-person household, and parents/caretakers with incomes up to 216% of the FPL.
How to apply for Washington, D.C. Medicaid: You can apply online at DC Health Link or by visiting your closest Income Maintenance Administration Service Center.
Other notable programs: Long-term care and nursing home care services Spend Down, a Medicaid program for people who exceed income limits, but have high medical bills Emergency Medicaid for people who cant qualify for standard Medicaid due to citizenship/immigration status.
