Medicaid If You Are 18 Or Younger
If you are 18 or younger, you may qualify for income-based Medicaid if your familys income is 211% of the Federal Poverty Guidelines or less . It doesn’t matter how much your family has in resources or whether you have a disability. Note: Income-based Medicaid for children 18 and younger is sometimes called “Healthy Start.”
Check whether your family’s income is low enough for you to get income-based Medicaid:
Your family size:| Income limits for your family: | |
| $13,590 | |
| Income-based Medicaid, adults | |
| Income-based Medicaid, children | |
| Subsidized private plans, reduced fees | |
| Subsidized private plans | — |
If your family’s income is at or below the limit for a program, you may qualify if you meet other program rules.Notes:
|
Note: Some young people with disabilities who don’t get SSI and don’t qualify for income-based Medicaid may still qualify for disability-based Medicaid. If you have any questions about this, talk to a benefits planner.
Have Medicare Questions Call 1
We make our money via compensation from the insurance companies youll encounter on this site, by allowing them to post information about their plans here. But whether you choose one company over another or one plan over another has no effect on the revenue we receive. That means theres no potential for conflict of interest. In other words, the plan you choose doesnt impact our finances, and because of that, we dont have any inclination to promote one option over another. Its all about what works for you, your healthcare needs and your budget.
Health Network Group – PO Box 3199, Winston Salem, NC 27102-3199
Social Security Work Incentives
Dont let concerns about SSI benefits stop you from encouraging your child to find an employment setting that is right for them. Parents of youth with disabilities are very aware of the importance of healthcare for their children. Many have heard that SSI recipients will lose their Medicaid coverage if they earn any money. As a result, some families discourage their young adults from joining the workforce. This is not true. Be aware that the Social Security Administration has Work Incentive programs that allow young adults with disabilities to continue to receive Medicaid coverage while they explore careers or attend postsecondary education or job training.
Make an informed choice. If your son or daughter receives SSI, contact a Work Incentives Planning and Assistance Project in your state to see how they can continue to receive health coverage through Medicaid while they work. WIPA projects are community-based organizations that receive grants from SSA to provide all Social Security and Supplemental Security Income disability beneficiaries with free work incentives planning and assistance.
WIPA services are available in every state, the District of Columbia, and the U.S. Territories of American Samoa, Guam, the Northern Mariana Islands, Puerto Rico, and the Virgin Islands. Call 1-866-968-7842 or 1-866-833-2967 for locations WIPA organizations or see the online SSA service provider directory.
Recommended Reading: Medicaid Indiana Provider Phone Number
Services Covered By Medicaid And Chip
- Regular checkups at the doctor and dentist
- Medicine and vaccines
- Access to medical specialists and mental health care
- Treatment of special health needs and pre-existing conditions
These services are provided by health plans. If your child gets Medicaid or CHIP, you will choose a plan from the ones available in your service area.
Are Children Eligible For Medicare
If you want to qualify for Medicare, children must be disabled and checked through the Social Security Administration. They need to have been receiving social security for their benefits for two years before applying for Medicare. However, if your child has End Stage Renal Disease, which is a kidney condition that needs dialysis every day or a transplant for the affected kidney. Medicare pays for doctors visit and medical services that are provided for those disabilities and conditions that are allowed by Medicare.Quick Facts on Medicare for Kids
- Parents are still responsible for paying Medicare programs
- Some child healthcare programs are free through Medicare. For example, you may be eligible for CHIP or Childrens Health Program
- Even if you have other types of insurance, you can still receive Medicare
Don’t Miss: How To Report Medicaid Fraud
Alternative Healthcare Options For Children
Most kids wont qualify for Medicare. If a child doesnt qualify, you have some other health insurance options. Some common ones include:
- Parents employer or other private health plans. Kids can stay on their parents health coverage until theyre 26 years old. Kids are eligible to stay even if theyre working, married, and not financially dependent on their parents, but coverage ends on their 26th birthday.
- Health Insurance Marketplace plans. Plans you purchase through the Health Insurance Marketplace or your states Health Insurance Exchange follow the same rules as insurance through your employer or other private groups. Youre able to add kids who are under age 26 to any plan you buy.
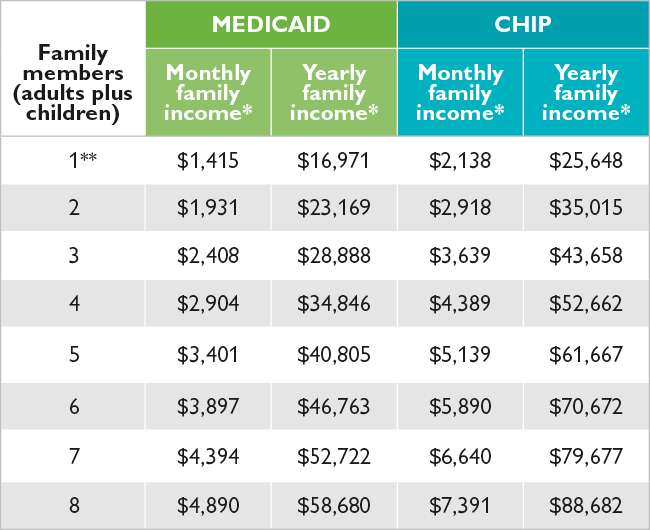
- Childrens Health Insurance Program . CHIP is a national program that works with each states Medicaid office to provide health insurance to kids. Generally, CHIP is intended for families with limited incomes who make too much money to qualify for Medicaid but not enough money to afford private insurance. Income eligibility requirements vary by state and are based on the federal poverty level.
- Medicaid. Families with limited incomes can qualify for health insurance through Medicaid. Every member of your household, including children, will be eligible if you qualify for Medicaid. Eligibility for Medicaid is based on your income and varies by state.
When Does Medicaid End For A Child In California
It depends on their age, eligibility, and income. For children under 18 years of age who are living in California, theyll need to be enrolled in Medi-Cal until they turn 19 years old. They will need to provide parental tax information if they are under 19 and not married. According to the California Department of Health Care Services, Medicaid coverage can end for a child when they turn 19.
Also Check: Iowa Medicaid Breast Pump Coverage
What Is The Medicaid Program
Good health is important to everyone. If you can’t afford to pay for medical care right now, Medicaid can make it possible for you to get the care that you need so that you can get healthy and stay healthy.
Medicaid is available only to certain low-income individuals and families who fit into an eligibility group that is recognized by federal and state law. Medicaid does not pay money to you instead, it sends payments directly to your health care providers. Depending on your state’s rules, you may also be asked to pay a small part of the cost for some medical services. In general, you should apply for Medicaid if you have limited income and resources. You must match one of the descriptions below:
May My Plan Or Health Insurance Coverage Impose Preexisting Condition Exclusions On My Newborn Child Adopted Child Or Child Placed For Adoption
Under HIPAA, as long as you enroll your newborn child, adopted child, or child placed for adoption within 30 days of the birth, adoption, or placement for adoption, your plan or insurance coverage may not impose preexisting condition exclusions on the child. Further, any future plan may not impose a preexisting condition exclusion, provided the child does not incur a significant break in coverage .
Also Check: How To Flip A Newborns Sleep Schedule
Don’t Miss: Does Medicaid Cover Breast Augmentation
Can A Child Qualify For Medicare
Dependent children are eligible for Medicare in certain situations. This is especially the case when a child is severely ill.
- He/she has end-stage renal disease requiring dialysis and currently receiving SSA benefits may qualify for Medicare
- If your child has ESRD that requires regular dialysis or needs a kidney transplant, Medicare eligibility is possible
- A child that has a disability resulting in entitlement from Social Security Disability Insurance payments
Do I Qualify For Medicaid
Medicaid provides free or low-cost health coverage to some low-income people, families and children, pregnant women, the elderly, and people with disabilities. Many states have expanded their Medicaid programs to cover all people below certain income levels. Medicaid qualifications depend partly on whether your state has expanded its program.
Don’t Miss: How To Apply For Medicaid In Las Vegas Nevada
States Where Children Are More At Risk
Children in states with certain characteristics of their Medicaid/CHIP programs are at greater risk of losing their coverage. See Table 1. These include states with separate CHIP programs, states that charge premiums for CHIP coverage , states that do not provide 12 months of continuous coverage for children in Medicaid, and states that process less than half of their renewals using existing data sources. Most states have risk points states where children are at the greatest risk with all five factors are Delaware, Florida, Georgia, Missouri, Nevada, and Texas.
Other impactful practices include ensuring that notices are easy-to-understand and sending reminders via multiple modes of communications when action is required to avoid a loss of coverage. Less is known about these procedures on a state-level basis, so we have not included these factors in identifying states where children may face a higher risk of coverage loss.
However, its important to note that in states with proven enrollment and retention policies but poor administrative procedures, children will face a higher risk of becoming inappropriately disenrolled. Likewise, in states without these key policies but rise to the daunting administrative challenge when the continuous enrollment requirement is lifted, children would face a lower risk.
Utah Chip Experience Raises Red Flags
An instructive lesson about what lies ahead can be imparted from Utahs CHIP program. In 2020, several states received approval from the Center for Medicare and Medicaid Services to impose a disenrollment freeze on its separate CHIP program, in addition to Medicaid. In late 2020, these states, including Utah, were told by CMS that they must lift the CHIP freeze. In Utah, the state was unable to locate many of the families, and 41 percent of children enrolled in CHIP dropped off.15 It is not known how many of these children found other insurance or became uninsured.
The Role of CHIP: States administer their CHIP programs differently states may choose to extend Medicaid coverage under CHIP or establish a separate state program. All children enrolled in Medicaid have been protected by the disenrollment freeze. However, this is not the case for children enrolled in separate CHIP programs, who constitute just over 40 percent of the 6.9 million children enrolled in CHIP.16 As discussed below, two-thirds of states have a separate CHIP program.
All children in Medicaid are at risk of losing coverage for procedural reasons. For those in M-CHIP states, the transition may be smoother if they are successfully redetermined as eligible since these children will retain their Medicaid coverage. However, children in states with separate CHIP programs will be at greater risk when the continuous coverage requirement lifts.
Also Check: Blue Cross Blue Shield Wny Medicaid
Medicaid To Separate Chip Program
In half of the states with separate CHIP programs, a family of three could have an income gain of up to $23,000 and still be eligible for CHIP. The difference in Medicaid and CHIP upper income limits varies considerably across the 34 states. But, even in South Dakota, the state with the smallest difference in income eligibility between Medicaid and CHIP, the household income of a child enrolled in Medicaid would need to increase by more than $5,000 to be over income for CHIP. Thus, a majority of children who lose Medicaid because their families income increased are likely to be eligible for CHIP.
Children with other private health insurance, even those with complex health care needs, are not eligible for CHIP. A key difference between Medicaid and CHIP coverage is an eligibility requirement in CHIP that a child must be uninsured. Children eligible for Medicaid are allowed to have other coverage, such as employer-sponsored insurance, with Medicaid acting as a secondary payor for additional wraparound services that the childs primary insurance does not cover.
Who Is Eligible For Medicaid
You may qualify for free or low-cost care through Medicaid based on income and family size.
In all states, Medicaid provides health coverage for some low-income people, families and children, pregnant women, the elderly, and people with disabilities. In some states the program covers all low-income adults below a certain income level.
- First, find out if your state is expanding Medicaid and learn what that means for you.
- If your state is expanding Medicaid, use this chart to see what you may qualify for based on your income and family size.
Even if you were told you didn’t qualify for Medicaid in the past, you may qualify under the new rules. You can see if you qualify for Medicaid 2 ways:
- Visit your state’s Medicaid website. Use the drop-down menu at the top of this page to pick your state. You can apply right now and find out if you qualify. If you qualify, coverage can begin immediately.
- Fill out an application in the Health Insurance Marketplace. When you finish the application, we’ll tell you which programs you and your family qualify for. If it looks like anyone is eligible for Medicaid and/or CHIP, we’ll let the state agency know so you can enroll.
Read Also: Medicaid Provider Id Number Lookup
Medicaid In New York State
- COVID-19 News and Updates:
- COVID Information for Medicaid Consumers:
- Medicaid Coverage through Your Local Department of Social Services during the Coronavirus Emergency
- Medicaid Telehealth Services During the Coronavirus Emergency
- IRS Form 1095-B Update:
- The 1095-B form for Tax Year 2020 is no longer being mailed automatically.If you need a copy of your 1095-B for Tax Year 2020, you can request it:
South Dakota Medicaid For Individuals In Adult Foster Care Facilities
Individuals in adult foster care homes that meet all eligibility criteria may qualify for South Dakota Medicaid.
Eligibility Requirements
- A person must be 65 years or older. If under age 65, a person must be blind or disabled.
- A person must be a resident of South Dakota and meet certain citizenship requirements of the United States.
- Medical needs of the individual are such that they require a level of care that must be provided in an adult foster care home.
- The applicants monthly income minus allowable deductions must be less than the current state reimbursement rate to an adult foster care home.
- The resource limit is $2,000. Resources include items such as checking and savings accounts and certificates of deposit.
Also Check: Can You Get Medicaid If You Have Insurance
Health Insurance Options For College Students
Medicaid can be a great way for students from limited-income families to obtain health insurance coverage. However, Medicaid eligibility requirements mean that not everyone will qualify for the health plan. There are several health insurance options for students who dont qualify for Medicaid.
Under the Affordable Care Act, students can remain on their parents’ health insurance plans until they are 26 years old. Individuals who currently aren’t covered by their parents plan can be added during enrollment periods.
When seeking health cover under a parents plan, check with the insurance company if there will be an in-network provider if the student is going to college in a different state. Some plans may not cover medical costs at hospitals that are out of their network, which could leave you with a huge out-of-pocket bill.
Being able to stay on your parent’s health insurance plan until you turn 26? That’s a major win. #ThanksObama
At What Age Does Medicaid Stop
Medicaid is a government-sponsored health care program for low-income citizens. The Medicaid program is funded by the federal and state governments, and eligibility varies from state to state. Its generally available to those who meet certain income and asset guidelines, and it provides coverage for low-cost or free medical services.
The age at which Medicaid stops depends on the state in which you live.
Also Check: Annual Income To Qualify For Medicaid
What About The Majority Of Kids Who Will Remain Eligible For Medicaid What Can Be Done To Protect Their Coverage
Recent estimates suggest that almost half of children who lose Medicaid or CHIP re-enroll within twelve months.26 While fluctuating income can result in temporary ineligibility, a significant share of gaps in enrollment are for procedural reasons where children remain eligible but lose coverage. Some families never receive the one and only notice the state sends or are confused about what, if anything, they need to do to retain coverage. These challenges are undoubtedly worse in families for whom English is not the parents primary language and who are less able to access culturally and linguistically competent consumer assistance worsening existing health disparities.27 The gaps in coverage created by churn and administrative barriers inhibit preventive care disrupt management of chronic conditions expose families to large medical bills impact the financial stability of providers serving large numbers of Medicaid enrollees increase administrative costs for states and health plans and undermine efforts to measure the quality of care.
Taking steps to minimize procedural disenrollments, outlined in Figure 3, should be a TOP priority for state and federal policymakers. Discussion on ways states can be better prepared for this mass event follows.
What Exactly Is Covered By Medicaid

Currently, Congress has decided what benefits are going to be provided to patients with autism by way of Medicaid assistance. The federal government does not provide very specific details on this coverage though. Basically, each state will need to determine what type of services are medically necessary for people with autism and then that will be covered. For the most part, this is an umbrella term and anything pertaining to autism will be included. Autism Speaks is a nationwide organization that aims to educate families, patients and the public on autism. Their organization has dedicated much of their time to monitoring all states in the U.S. and ensuring that nothing is being ignored. Medical professionals also have a say in what types of assistance their patients will be eligible to receive based on their diagnosis and their current state of health. For more information, you can visit Autism Speaks.
Recommended Reading: Does Medicaid Cover Swimming Lessons
