What You Might Pay Out Of Pocket Costs For
If you have treatment as a public patient at a public hospital you do not pay anything for your medical treatments.
Costs for many private treatments are also fully covered by Medicare and private health insurers. However, you may have to pay out of pocket costs if you have medical treatment as a private patient in a private or public hospital. This can include costs for:
- doctors or other health care providers
- hospital charges like accommodation and theatre fees
You might also have to pay out of pocket costs for medical services:
- outside a hospital, for example for appointments or diagnostic tests
- at a private hospital accident and emergency department
If Your Income Is Low And Your State Hasnt Expanded Medicaid
If your state hasnt expanded Medicaid, your income is below the federal poverty level, and you don’t qualify for Medicaid under your state’s current rules, you wont qualify for either health insurance savings program: Medicaid coverage or savings on a private health plan bought through the Marketplace.
- Find out why
-
- When the health care law was passed, it required states to provide Medicaid coverage for all adults 18 to 65 with incomes up to 133% of the federal poverty level, regardless of their age, family status, or health.
- The law also provides premium tax credits for people with incomes between 100% and 400% of the federal poverty level to buy private insurance plans in the Health Insurance Marketplace®.
- The U.S. Supreme Court later ruled that the Medicaid expansion is voluntary with states. As a result, some states havent expanded their Medicaid programs.
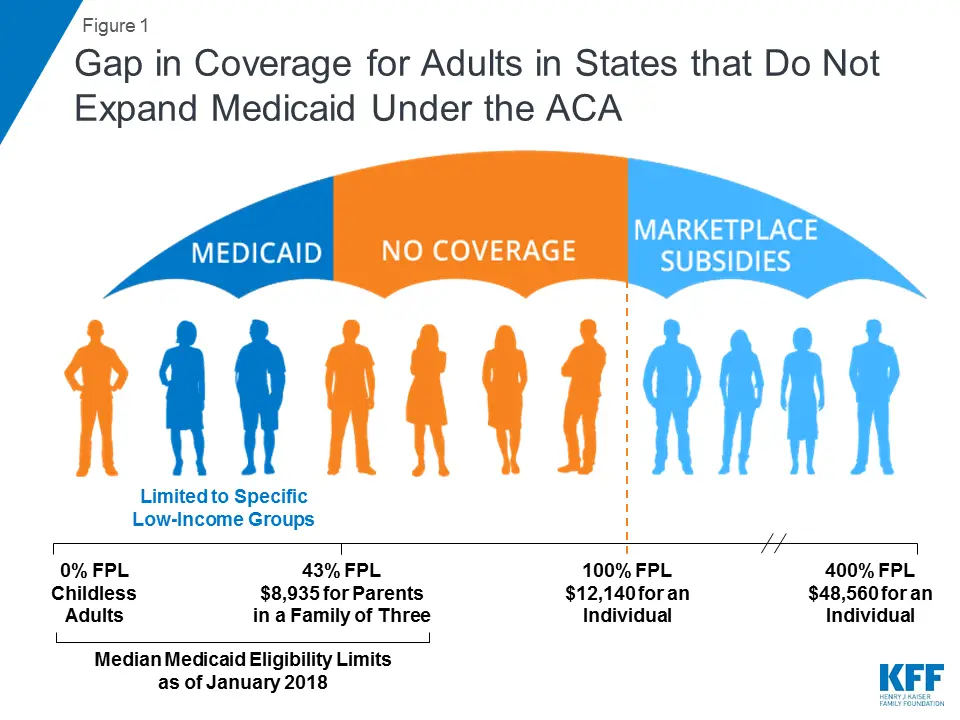
- Adults in those states with incomes below 100% of the federal poverty level, and who dont qualify for Medicaid based on disability, age, or other factors, fall into a gap.
- Their incomes are too high to qualify for Medicaid in their states.
- Their incomes are below the range the law set for savings on a Marketplace insurance plan.
-
States are continuing to make coverage decisions. They could expand Medicaid in the future.
What Out Of Pocket Costs You Might Pay
Any out of pocket costs you pay will vary depending on:
- how much you are charged
- whether you have treatment in hospital or outside hospital
- whether your treatment is covered by Medicare and how much Medicare pays
- if you are treated at a hospital, whether you are a public or private patient
- whether you have private cover for the treatment and if so, your level of cover
Doctors fees can only be covered by private health insurance for treatment in hospital. Different insurers might pay a different amount for the same service. Talk to your doctor, hospital and health insurer about:
- what your costs might be
- when you must pay them
The Medical Costs Finder helps you understand the cost of common medical procedures provided by specialists in Australia.
Don’t Miss: Qualify For Medicaid Washington State
Making Medicaid Adult Coverage All Or Nothing For States
A fourth proposal for expanding Medicaid is less about financing than control over coverage, and is modeled on the legislation passed to create the Medicare drug benefit. It would give states a choice: cover all low-income adults, or none. If they decline, then the federal government would assume responsibility for covering non-disabled, non-elderly adults in both pre-ACA and the ACA expansion eligibility groups. A state not implementing the Medicaid expansion would no longer receive federal matching payments for adults with dependent children . Instead, CMS would operate a federal Medicaid program for those adults. Since all non-expansion states use HealthCare.gov for eligibility determinations for premium tax credits, CMS would use this system for eligibility determinations for this Medicaid-like program. The programs benefits would be determined as previously described for the option in which federal Medicaid is offered in cities and counties. Enrollees would also have the same rights as Medicaid enrollees .
Expansion Is Optional And Some States Continue To Say No
But in 2012, the Supreme Court, while upholding the rest of the ACA, struck down the Medicaid expansion requirement, leaving it up to each state to decide whether or not to participate. As of late 2021, 38 states plus the District of Columbia had expanded Medicaid.
There are still 12 states where Medicaid eligibility has not been expanded under the ACA, although Wisconsin has a unique situation and does not have a coverage gap . So there is still a coverage gap in 13 states: Alabama, Florida, Georgia, Kansas, Mississippi, North Carolina, South Carolina, South Dakota, Tennessee, Texas, and Wyoming.
But Medicaid expansion continues to slowly spread across the remaining states, as we knew it would. Voters in Oklahoma and Missouri approved Medicaid expansion ballot measures in 2020, so Medicaid expansion just took effect in those two states in 2021.
Don’t Miss: Will Medicaid Pay For Gastric Bypass
Doctor And Other Fees For Private Patients
As a private patient in a public or private hospital, you might have to pay for doctors and other health providers such as:
- surgeons
- other specialists
- medical imaging, pathology or other diagnostic test services
If you have private hospital insurance cover for the medical service, your insurer must pay at least the remaining 25% of the MBS fee.
Doctors and other health providers often charge more than the MBS fee for medical services you receive as a private patient in a hospital. This is called the gap. You may have to pay the gap out of your own pocket unless the doctor has a gap arrangement with your insurer and charges you under that arrangement. Many doctors and insurers use gap arrangements to remove or reduce your gap payment.
The Basics Of Medicaid
The Medicaid program provides eligible beneficiaries with low-cost or free health insurance. Administered by state governments, with federal guidelines and funding, the program helps tens of millions of people with limited ability to pay get necessary healthcare services. Each state has its own rules for who qualifies and what benefits are offered, but all use federal guidelines for care, coverage and eligibility of applicants.
The amount Medicaid participants are asked to pay for their health services is largely determined by their ability to pay. Enrollees with very limited means often pay no premiums or co-payments for the services Medicaid provides. Those with some income or assets usually have a share of cost that must be paid before Medicaid coverage kicks in. Some people have more income and/or assets than the pre-ACA Medicaid maximum. Before 2010, these relatively low-income people could be denied Medicaid coverage despite the cost of private insurance being too high for them to pay.
You May Like: How Does Emergency Medicaid Work
Medicaid Expansion Helps Address Health Disparities
Extending health coverage to more low-income people is an important way to reduce health disparities between people of color and others in the United States. An analysis by the Kaiser Family Foundation found that the Medicaid expansion particularly affects people of color, given that they are more likely to lack health insurance and also to have low incomes. In states that have not adopted the Medicaid expansion, poor adults with incomes below the federal poverty level fall into a coverage gap because they remain ineligible for Medicaid but earn too little to qualify for premium tax credits for qualified health plans in the Marketplace. As a result, they are likely to remain uninsured. More than one-quarter of uninsured adults who would be eligible for Medicaid if all states expanded are people of color. The Kaiser analysis also found that the coverage gap in states not expanding Medicaid disproportionately impacts poor, uninsured African-American adults since they are likely to reside in the southern region of the country, where most states have not implemented the Medicaid expansion.
CMS is offering links/charts for informational purposes only, facts should not be construed as an endorsement of the organization’s programs or activities
The Coverage Gap: No Realistic Access To Health Insurance
The coverage gap exists because the ACAs premium tax credits are only available for people with a household income of at least 100% of FPL, up to 400% of FPL. .
Premium subsidies are not available below 100% of FPL, because when the ACA was written, Medicaid expansion was an integral part of the law: It was assumed that subsidies would not be needed below 100% of FPL, since Medicaid would be available instead.
So in states that are not expanding Medicaid, virtually all non-disabled childless adults with incomes below 100% of FPL, as well as a large number of parents with incomes below 100% of FPL, are not eligible for any financial assistance to help them afford health insurance. Premium subsidies are not available to them through the exchange/marketplace, and they dont qualify for Medicaid unless they meet the stringent existing guidelines.
According to Kaiser Family Foundation data, there are about 2.2 million people in the coverage gap across the 11 states that have not expanded Medicaid.
The majority of the people in the coverage gap are in Texas, North Carolina, Florida, and Georgia more than 1.6 million of the people in the coverage gap are in those four states.
You May Like: Arkansas Long Term Care Medicaid Application
Impact On Medicare Beneficiaries
| This section needs to be . The reason given is: it does not reflect benefit changes following passage of the Patient Protection and Affordable Care Act of 2010. Please help update this article to reflect recent events or newly available information. |
The U.S. Department of Health and Human Services estimates that more than a quarter of Part D participants stop following their prescribed regimen of drugs when they hit the doughnut hole.
Every Part D plan sponsor must offer at least one basic Part D plan. They may also offer enhanced plans that provide additional benefits. For 2008, the percentage of stand-alone Part D plans offering some form of coverage within the doughnut hole rose to 29 percent, up from 15 percent in 2006. The percentage of Medicare Advantage/Part D plans plans offering some form of coverage in the coverage gap is 51 percent, up from 28 percent in 2006. The most common forms of gap coverage cover generic drugs only.
Among Medicare Part D enrollees in 2007 who were not eligible for the low-income subsidies, 26 percent had spending high enough to reach the coverage gap. Fifteen percent of those reaching the coverage gap had spending high enough to reach the catastrophic coverage level. Enrollees reaching the coverage gap stayed in the gap for just over four months on average.
| 25% | 25% |
As of January 1, 2020, the coverage gap has closed.
Allowing Cities Or Counties To Expand Medicaid
Another option to expand Medicaid would be to bypass state governors and legislatures, instead allowing local jurisdictions to implement the Medicaid expansion within their borders. To take this option, local towns, cities, or counties would need to secure what would have otherwise been their states share of the total costs of the expansion of Medicaid in their jurisdictions. They would also need to work with the Centers for Medicare and Medicaid Services to set up eligibility systems for their areas, using the HealthCare.gov website. Several of the same states targeted for Medicaid expansion already allow HealthCare.gov to determine Medicaid as well as Marketplace eligibility for people applying for health care coverage through the website. CMS also already reviews Medicaid managed care rates for currently eligible people in most of these states it could use this information to leverage these rates for coverage for the city or countys adult population. CMS would adopt benefits consistent with those offered to similarly situated Medicaid enrollees in the state, within the ACAs guidelines for alternative benefit plans. The proposal would provide to this federally run Medicaid program the same rebates for prescription drugs that state-run Medicaid programs receive.
Recommended Reading: Chiropractors That Accept Medicaid In Louisiana
What Is The Medicare Coverage Gap
The coverage gap is also known as the donut hole for Part D prescriptions. Most Medicare plans have a coverage gap, but sometimes in select areas, there are plans available that cover more than the standard amount. If you find a plan that includes gap coverage, its likely to have a higher monthly premium.
How Does The Medicaid Gap Work

Below are some quick points to illustrate the gap between those who qualify for subsidies and those who qualify for affordable health insurance due to .
- If a person falls below the cut-off, they may fall in the Medicaid Gap if: Their state didnt expand Medicaid to at least 100% of the Federal Poverty Guidelines.
- In some states Medicaid eligibility can be as low as 50% FPL and other factors such as gender and pregnancy can affect eligibility.
- In most states CHIP covers most low-income children, so the Medicaid gap mainly affects adults.
See information on states that expanded Medicaid.
Don’t Miss: I Am On Disability Can I Get Medicaid
Closing The Medicaid Coverage Gap Will Improve Health And Well
Closing the Medicaid coverage gap would provide health coverage for over 2.2 million low-income Americans who are currently ineligible for any federal health insurance supports. These families live in the 11 states where Republican state officials have refused to accept generous federal funding to expand their state Medicaid programs to cover the larger low-income population offered coverage under the Affordable Care Act .
This expansion would narrow racial gaps in health access while also delivering benefits to a broad and diverse low-income population. Analyses of recent and historical coverage expansions for low-income families show that the policy saves lives, improves peoples health, supports local hospital systems and is a strong investment in long-run socioeconomic well-being.Read the full brief here.
Increasing Federal Funding For The Medicaid Expansion
A straightforward approach to encouraging the remaining states to expand Medicaid is to increase federal financial support for doing so. In his fiscal year 2017 budget, President Obama proposed to provide states that newly expand Medicaid the same higher federal matching rate and six-year phase-down as those that expanded in 2014 .23 Senators Warner and Kaine introduced this proposal, called the SAME Act .24 The Congressional Budget Office projected that this policy would cost $31 billion over ten years.25 Congress could also vary increased federal financial incentives, such as extending the number of years that a newly expanding state gets 100 percent federal funding, or increasing the federal matching rate for such states from 90 percent to 95 percent, for example, for some extended length of time or in perpetuity.
Also Check: What Does Medicaid For Adults Cover
Closing Medicaid Coverage Gap Would Help Diverse Group And Narrow Racial Disparities
The 2.2 million uninsured adults with incomes below the poverty line who were caught in the Medicaid coverage gap in 2019 are a varied group theyre essential workers, parents caring for children, older and younger adults, and diverse in terms of race and ethnicity but they all have something in common. They live in states that have failed to adopt the Affordable Care Acts Medicaid expansion, even with significant federal financial incentives, leaving this group with no pathway to affordable coverage.
States that havent implemented expansion should do so, and to account for states that wont, Congress should act on calls from Senators Warnock and Ossoff and over 60 civil rights and other organizations to close the coverage gap by creating a federal fallback.
Extending health insurance to people in the coverage gap squarely benefits people with incomes below the poverty line who are uninsured and lack any access to affordable coverage.Extending health insurance to people in the coverage gap squarely benefits people with incomes below the poverty line who are uninsured and lack any access to affordable coverage. Some 60 percent of people in the gap in 2019 were people of color, reflecting long-standing racial and ethnic disparities in health care access that coverage extensions would do much to address.
What Are Gap Payments
A gap payment is an out-of-pocket expense you have to pay when you receive medical treatment that costs more than what you can claim back from Medicare or your private health insurance. Regardless of whether youre a public or private patient, Medicare will subsidise some of the cost.
Lets go into a bit more detail. When you are treated in a hospital, there is a scheduled fee charged as outlined in the Medicare Benefit Schedule for each different Medicare Item Number. Medicare and private health insurance cover 100% of this scheduled fee, as well as the cost of your accommodation and theatre fees, provided youre treated in a hospital that has an agreement with your Health Fund.
The medical gap is the amount above the scheduled fee that your specialist charges.
Take a hospital admission for heart surgery, for example. Youll notice in the graph above that Medicare covers part of your fee, and so does your private health insurance policy . In fact, if your doctor onlycharged the scheduled fee for your treatment, you might pay nothing!
In the example above though, this doctor charges more than the standard scheduled fee, and you need to pay the gap to make up the difference.
Also Check: Does Medicare Medicaid Pay For Dentures
Death In Dallas: One Familys Experience In The Medicaid Gap
By Ashley Lopez, KUTSeptember 30, 2021
We encourage organizations to republish our content, free of charge. Heres what we ask:
You must credit us as the original publisher, with a hyperlink to our khn.org site. If possible, please include the original author and Kaiser Health News in the byline. Please preserve the hyperlinks in the story.
Have questions? Let us know at
