Receive Approval For Medicaid
It could take the state 45 days to see if your child/children are eligible for Medicaid coverage. To check on the status of your child/childrens application, visit gateway.ga.gov or call 1-877-423-4746.
Shortly after you are approved for Medicaid or PeachCare for Kids® you will be enrolled into a health plan in Georgia Families. Georgia Families will mail you a welcome letter with information about your health plan. If you do not want the health plan that has been chosen for you, you can change to another health plan. You will have 90 days from the start date of your health plan to change to a new health plan.
After youve been approved for Medicaid, heres what you need to do to select Medicaid with Kaiser Permanente:
If You Currently Have Marketplace Coverage
- If you want to keep your current Marketplace coverage, dont report your pregnancy to the Marketplace. When filling out your application for Marketplace coverage, select the Learn more link when we ask if youre pregnant to read tips to help you best answer this question.
- If you report your pregnancy, you may be found eligible for free or low-cost coverage through Medicaid or the Childrens Health Insurance Program . If you are found eligible for Medicaid or CHIP, your information will be sent to the state agency, and you will not be given the option to keep your Marketplace plan.
- If you keep your Marketplace coverage, be sure to update the application after you give birth to add the baby to the plan or enroll them in coverage through Medicaid or CHIP, if they qualify.
For Members In Medicaid Or Peachcare For Kids
Georgia Families gives you choices for your health care! Choose a health plan and a Primary Care Provider for each member in your family who is in Medicaid or PeachCare for Kids®.
Alert: Due to COVID-19 restrictions, in person visits are not currently available.
As soon as you become a member of Medicaid or PeachCare for Kids® you will be enrolled into a health plan. If you do not want the health plan we chose for you, you can change to another health plan. You will have 90 days from the start date of your health plan to change. You can change your health plan in one of these three ways:
Learn more about:
- Contacts: Georgia Families, Medicaid, PeachCare for Kids®, Family & Children Services offices, health plans
You May Like: United Healthcare Customer Service Medicaid
Who Is Eligible For Medicaid In Georgia
As of April 2020, criteria for enrollment in Georgia Medicaid are set at the following levels for non-disabled adults:
- Children up to age 1 with family income up to 205% of federal poverty level
- Children ages 1-5 with family income up to 149% of FPL
- Children ages 6-18 with family income up to 133% of FPL
- Pregnant women with family income up to 220% of FPL
- Parents of minor children with family income up to 35% of FPL
Preventing Maternal Deaths In Georgia
Comprehensive postpartum care is an important component to preventing maternal mortality. Georgia ranks no. 49 among states for the rate of maternal mortality, defined as deaths related to pregnancy that occurred during or within one year of the pregnancy or birth.
Georgia established a Maternal Mortality Review Committee in 2014 to identify maternal deaths and their causes. The committee found that between 2012 and 2014, 101 mothers died from pregnancy-related causes and about 60 percent of the deaths were preventable.
The committee also found significant evidence of the maternal mortality crisis Black women are facing in Georgia. The maternal mortality rates for Black women in Georgia were three to four times higher than for white women. The committee, as well as House Study Committee on Maternal Mortality and House Study Committee on Infant and Toddler Social and Emotional Health, included the postpartum Medicaid extension in their recommendations to help address the maternal mortality crisis.
Currently no states have implemented the postpartum Medicaid extension, but several states are pursuing the option through Medicaid 1115 waivers. Applying for a waiver is the only way to enact the policy and get federal Medicaid matching funds, unless proposed federal legislation passes to make it a state option.
Read Also: Medicaid Texas Income Limits 2020
Georgia Medicaid Income Limits Summary
We hope this post on Georgia Medicaid Income Limits was helpful to you.
If you have any questions about Medicaid in the state of Georgia, you can ask us in the comments section below.
Help us spread the word! If you found this post on Georgia Medicaid Income Limits helpful, help us spread the word by sharing it using the Share this button below.
Be sure to check out our other articles about Medicaid.
Who Are The Managed Care Organizations
Credentialing Process
DCH is in the process of revising its credentialing process and will begin to announce these changes as they occur. Current plans are to utlize HP to work with an NCQA approved vendor to manage the credentialing process. for details.
Checking Medicaid CMO Eligibility
With the implementation of HB 1234 in 2008, there have been some changes to the way you verify member eligibility. Previously, you would go to the CMOs websites to determine eligibility by plan affiliation however, due to the bill the only acceptable verification of plan affiliation for a member is via the GHP web portal. You may notice that all the CMOs have a link to the GHP web port for plan affiliation verification. You may still utilize the CMO eligibility verification for PCP assignment.
Who is eligible for the Georgia Families Managed Care Program?
Individuals who are eligible to enroll in Georgia Families include low-income families, children, and pregnant women, women eligible for Medicaid due to cervical cancer and PeachCare for Kids to managed care. Aged, Blind and Disabled population are included in the managed care program at this time. Children in foster care must opt out in order to not be transfered to Amerigroups Georgia Family 360.
Recommended Reading: Centers For Medicare And Medicaid Services Login
Online Prenatal Education Classes
The Healthy Mothers, Healthy Babies Coalition of Georgia has an online community called Pickles and Ice Cream Georgia. They host a free, 90 minute online prenatal course for any child-bearing person who is currently pregnant or has given birth within the past 6 months. Learn about pregnancy, baby care, WIC and everything else you need for a happy, healthy pregnancy. You can even earn up to $20 in gift cards for taking part in these classes! Go to picklesandicecreamga.org/events/ to sign up and learn more.
How Do I Get Approved For Pregnancy Medicaid
Hey yall! So today I wanted to give yall a bit of information about Pregnancy medicaid I personally had this for both of my pregnancies. It is a great thing to have when you dont have insurance and also if you do have insurance but have co-pays and just extra bills that you have to pay out of pocket.
Also Check: Dental Places That Accept Medicaid
How Does Medicaid Provide Financial Help To Medicare Beneficiaries In Georgia
Many Medicare beneficiaries receive assistance from Medicaid with Medicare premiums, prescription drug costs, and expenses not covered by Medicare including long-term care.
Our guide to financial assistance for Medicare enrollees in Georgia includes overviews of these programs, including Medicaid nursing home benefits, Extra Help, and eligibility guidelines for assistance.
Benefits Of Medicaid For Pregnant Women
First, you will be given a list of medical providers who accept Medicaid or given a website to look for a provider in your area.
Second, pregnant women are covered for all care related to the pregnancy, delivery and any complications that may occur during pregnancy and up to 60 days postpartum.
Third, as long as you receive care from a Medicaid provider, your health care costs will be submitted through Medicaid and will be covered, in accordance with Medicaid regulations and guidelines.
Finally, Medicaid usually gives Pregnant women priority in determining Medicaid eligibility. Most offices try to qualify a pregnant woman within about 2-4 weeks.
If you need medical treatment before then, talk with your local office about PE Medicaid as explained above.
Don’t Miss: Dentist In Dublin Ga That Accept Medicaid
If You Have Medicaid Or Chip
- If found eligible during your pregnancy, youll be covered for 60 days after you give birth. After 60 days, you may no longer qualify. Your state Medicaid or CHIP agency will notify you if your coverage is ending. You can enroll in a Marketplace plan during this time to avoid a break in coverage.
- If you have Medicaid when you give birth, your newborn is automatically enrolled in Medicaid coverage, and theyll remain eligible for at least a year.
If You May Qualify For Medicaid Or Childrens Health Insurance Program

- Medicaid and CHIP provide free or low-cost health coverage to millions of Americans, including some low-income people, families and children, and pregnant women.
- Eligibility for these programs depends on your household size, income, and citizenship or immigration status. Specific rules and benefits vary by state.
- You can apply for Medicaid or CHIP any time during the year, not just during the annual Open Enrollment Period.
- You can apply 2 ways: Directly through your state agency, or by filling out a Marketplace application and selecting that you want help paying for coverage.
- Learn how to apply for Medicaid and CHIP.
Recommended Reading: How Much Do You Have To Earn To Get Medicaid
Georgia Medicaid Income Limit
The Georgia Medicaid Income Limit is calculated as a percentage of the Federal Poverty Line.
To qualify, you must meet the Georgia Medicaid Income limits listed below.
Here is the Federal Poverty Level for 2021.
| 2021 Federal Poverty Levels for the 48 Contiguous States & D.C. |
| Household Size |
Additionally, to be eligible for Medicaid, you cannot make more than the income guidelines outlined below:
- Children up to age 1 with family income up to 205 percent of FPL
- Any child age 1-5 with a family income up to 149 percent of FPL
- Children ages 6- 18 with family income up to 133 percent of FPL
- CHIP for children with family income up to 247 percent of FPL
- Pregnant women with family income up to 220 percent of FPL
- Parents of minor children with family income up to 32 percent of FPL
- Individuals who are elderly, blind, and disabled with family income up to 74% of the FPL
Pregnancy / Womens Health Medicaid
Presumptive Eligibility Medicaid for Pregnant Women and Womens Health Medicaid
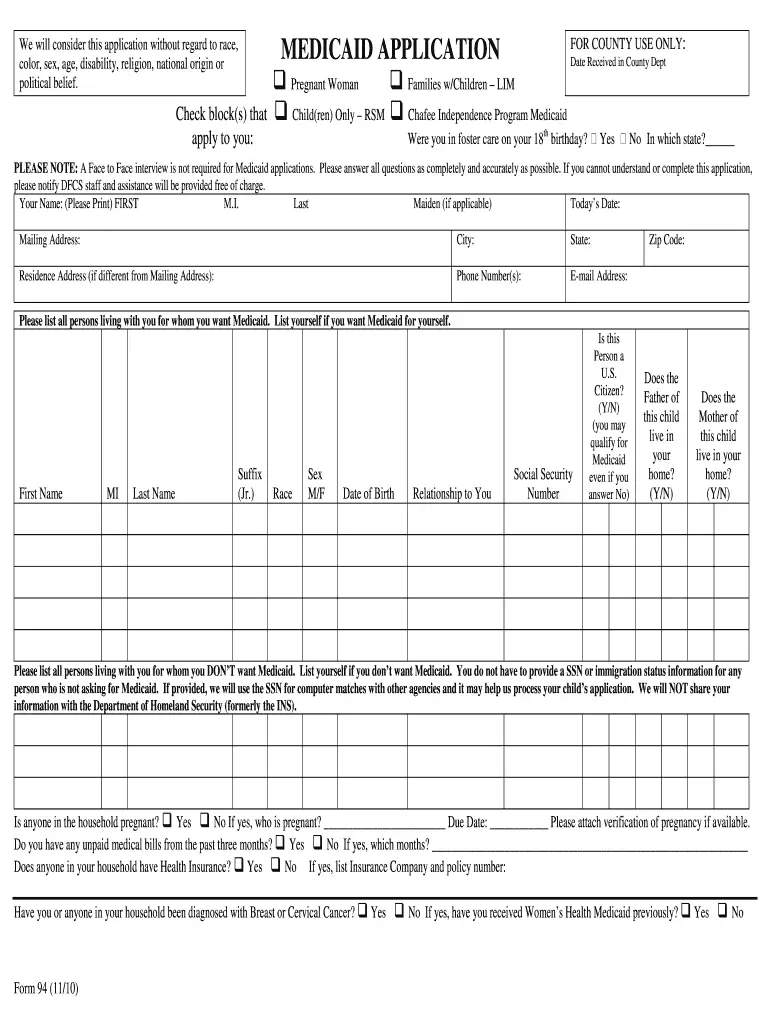
Q. Where do I go to apply for Medicaid?A. There are several ways to apply for Medicaid and other medical assistance programs:
- You can find out if you qualify for Medicaid or other medical assistance and social service programs by speaking with a representative at your local DFCS office. Call the DFCS information line at 877-423-4746 to be directed to the appropriate office where someone can help you. For a list of DFCS locations and address, phone, fax numbers in your county click the following link: www.dfcs.dhr.georgia.gov, click on County Offices, next click on Complete List of All County offices.
- To apply for Medicaid, you can submit a completed signed application online at Georgia Gateway, or you may print a Medicaid application and submit the completed signed application at any local DFCS office, in person, by mail, telephone, fax or email. Click on the following links to complete and print your application.
Don’t Miss: Medicaid And Medicare Supplement Insurance
Early Periodic Screening Diagnostic & Treatment
Early and Periodic Screening, Diagnostic, and Treatment benefit includes a comprehensive array of preventive, diagnostic, and treatment services for Medicaid eligible infants, children and adolescents under age 21, as specified in Section 1905 of the Social Security Act . The EPSDT benefit is also available to PeachCare for Kids® members up to 19 years of age. The EPSDT benefit is designed to assure that children receive early detection and care, so that health problems are averted or diagnosed and treated as early as possible. The goal of the EPSDT benefit is to assure that individual children get the health care they need when they need it.
The EPSDT benefit also covers medically necessary diagnostic services. When a screening examination indicates the need for further evaluation of a childs health, the child should be appropriately referred for diagnosis without delay. States are required to arrange for and cover under the EPSDT benefit any Medicaid covered service listed in Section 1905 of the Act if that treatment or service is determined to be medically necessary to correct or ameliorate defects and physical and mental illnesses or conditions for children through age 20 years of age.
Reviewing your Health Check Record
Billing Tips for Health Check
Health Check Referral Codes
Vision Screening
Georgia Pregnancy Medicaid Income Limit
In addition to the income limit above, you have to also meet the following requirements:
What Does RSM Medicaid Cover?
Right from the Start Medicaid for pregnant women pays for medical care for pregnant women, including labor and delivery, for up to 60 days after they give birth. Benefits include:
- Doctor visits
- Drugs ordered by a doctor
- Labor and delivery
- Rides to the doctor
Read Also: Medicaid How Much Money Can You Make
What Is Georgia Families
Georgia Families® is a partnership between the Georgia Department of Community Health and private care management organizations to provide quality health care services to members of Medicaid and PeachCare for Kids®.
As a new program offering health care for Medicaid and PeachCare members, Georgia Families® offers members better access to care, quality health care providers and health education.
WellCare of Georgia works with Georgia Families®. We help kids, pregnant women and families who have Medicaid.
Georgia Medicaid Expansion Update
Georgia will partially expand Medicaid as of July 2021.
However, it will come with a work requirement and without the ACAs enhanced federal funding that would go along with full expansion.
In November 2019, the state unveiled an 1115 waiver proposal that calls for partial Medicaid expansion, effective in July 2021.
The partial expansion would cover adults age 19-64 with income up to 100 percent of the poverty level, as long as they work at least 80 hours per month.
The work requirement can also be fulfilled via various other community engagement activities, including job training, higher education, or community service.
However, there are time limits on vocational training and job readiness programs.
As of May 2020, 23 percent of people in Georgia did not have health insurance coverage.
Also Check: Medicaid Brooklyn Ny Phone Number
Planning For Healthy Babies
P4HB members need to renew each year. You will get a renewal notice in the mail before the deadline.
To renew:
TTY:
P4HB members renew every 12 months. Youll get a renewal note in the mail before the deadline.
To renew call . Youll need to confirm your income when you renew. You can use pay stubs within 90 days of your renewal deadline.
Need help or your renewal date? Call .
Georgias History With Medicaid Expansion

As of May 2020, 23% of Georgia residents were uninsured the state has the fourth highest uninsured rate in the U.S. Georgia is leaving billions of dollars on the table and over half a million people without Medicaid coverage by passing up federal funding to expand Medicaid.
Two laws designed to make expansion difficult were enacted during the 2014 legislative session. HB 990 prohibits Medicaid expansion without legislative approval , while HB 943 prohibits state and local employees from advocating for Medicaid expansion.
By the spring of 2016, Medicaid expansion began to seem within reach in Georgia, fueled in part by support from hospitals facing severe financial challenges. The state has raised Medicaid reimbursement rates for providers, including OB-GYNs in the state, in an effort to keep providers solvent and able to accept Medicaid patients. And Republican lawmakers began indicating that they might be open to a privatized version of Medicaid expansion, like the model used in Arkansas.
However, there was no real progress on Medicaid expansion in Georgia until the partial expansion proposal was announced in 2019. Governor Brian Kemp, who took office in 2019, has been steadfastly opposed to full Medicaid expansion, although he views the Georgia Pathways program as a conservative compromise aimed at helping people who are working but not able to afford health coverage.
Recommended Reading: Can You Have Insurance And Medicaid
How Do I Apply
Search for the Department of Community Health in your state. Verify that you fit under the income limit for your family size and you can either apply through their website or through the Department of Family and Child Services website. You can apply online or in person but I recommend that you apply in person because you can get your medicaid approved right then and there.
I highly recommend that you are completely 100% honest on your application and that you do not leave anything out. Yes, you can get approved for medicaid if you already have insurance. Basically what happens is your insurance will become your primary insurance and medicaid will be your secondary insurance. So whatever your primary does not pay for, medicaid will cover it. If you have a co-pay for your primary, medicaid will cover it so you will not have to pay for it. You can go to the dentist with medicaid and pay for your prescription medication with it also. I actually got all of my wisdom teeth removed and medicaid paid for it after I delivered my first daughter.
