In The Right Direction
Medicaid expansion coverage is set to begin in Missouri on July 1, 2021. The constitutional amendment, protected from changes by the state legislature, will impact about 230,000 low-income Missourians, according to Von Glahn Missourians like Ledbetter and Altic.
I know its still gonna take some time before I can take advantage of those health care options for Medicaid, Ledbetter said. But its a step in the right direction.
The move will make a huge difference for Altic.
I wouldnt have to worry about whether I can go to the doctor if I have a small earache and wonder if its going to become something way worse, she said.
For Howard, the passage was a sign of hope to bring equal access to voting to the ballot.
There is hope to bring living wages for the working poor, he said. There is hope to bring healthcare as a right and not a privilege. And when we mobilize and organize together around these issues, we can see good things happen.
A senior Trump administration official says Medicare will cover the yet-to-be approved coronavirus vaccine free for older people under a policy change expected to be announced soon
Medicare will cover the yet-to-be approved coronavirus vaccine free for older people under a policy change expected to be announced shortly, a senior Trump administration official said Tuesday.
Compare Medicare Plans Now
Stay tuned, she added.
Compare Medicare Plans Now
View Entire Post
What Is Covered By Medicare Vs Medicaid
Medicare
Depends on the coverage you choose and may include:
- Care and services received as an inpatient in a hospital or skilled nursing facility
- Doctor visits, care and services received as an outpatient and some preventive care
- Prescription drugs
- Medicare Advantage plans: combine Part A and Part B coverage, and often include drug coverage , as wellall in one plan.
Medicaid
Each state creates its own Medicaid program, but has to follow federal guidelines, like the required and optional benefits they include. Some of the benefits Medicaid programs have to include are:
- Care and services received in a hospital or skilled nursing facility
- Care and services received in a federally-qualified health center, rural health clinic or freestanding birth center
- Doctor, nurse midwife, and certified pediatric and family nurse practitioner services
What Is Medicare Supplemental Health Insurance
Medicare is primary health insurance for many Americans over 65 and people with disabilities. However, not everything is covered in Medicare. As a result, you can extend your original Medicare benefits with one of several Medicare supplement possibilities.
A Medicare supplement plan is also known as Medigap. It can help cover some of the costs that Original Medicare doesnt. Medicare supplement insurance helps fill in the gaps that original Medicare misses.
Supplemental Medicare plans are sold by private insurance companies.Such plans can assist with copays, coinsurance, and deductibles. Some plans also help cover medical care when youre abroad.
If you already have original Medicare and you purchase a Medigap policy, Medicare will cover its share of the Medicare-approved share for covered health care fees. Then, your Medigap policy pays its amount.
Remember, Medigap policies dont pay for everything.
Usually, Medigap policies dont cover the following:
- Long-term care
- Private-duty nursing
Recommended Reading: Does Princeton House Accept Medicaid
What Is Medicare Vs Medicaid
Medicare
- A federal health insurance program for people who are:
- 65 or older
- Under 65 with certain disabilities
- Of any age and have End Stage Renal Disease or Amyotrophic Lateral Sclerosis
Medicaid
A joint federal and state program that helps pay health care costs for certain individuals and families with limited income and resources.
Medicaid Eligibility And Costs

The federal and state partnership results in different Medicaid programs for each state. Through the Affordable Care Act , signed into law in 2010, President Barack Obama attempted to expand healthcare coverage to more Americans. As a result, all legal residents and citizens of the United States with incomes 138% below the poverty line qualify for coverage in Medicaid participating states.
While the ACA has worked to expand both federal funding and eligibility for Medicaid, the U.S. Supreme Court ruled that states are not required to participate in the expansion to continue receiving already established levels of Medicaid funding. As a result, many states have chosen not to expand funding levels and eligibility requirements.
Those covered by Medicaid pay nothing for covered services. Unlike Medicare, which is available to nearly every American of 65 years and over, Medicaid has strict eligibility requirements that vary by state.
However, because the program is designed to help the poor, many states have stringent requirements, including income restrictions. For a state-by-state breakdown of eligibility requirements, visit Medicaid.gov and BenefitsCheckUp.org.
Read Also: New Mexico Medicaid Provider Portal
Which Companies Sell Medicare Supplement Insurance In Indiana
Companies must be approved by IDOI in order to sell Medicare Supplement policies. All of the companies listed below have been approved by the state. The plans are labeled with a letter, A through J. Not all companies sell all ten plans. Following each company name and phone number, we have listed the Medicare Supplement plans sold by that company based on the following categories:
- Medicare Supplements for Persons 65 and Older
- Medicare Supplements for Persons Under 65 and Disabled
- Medicare SELECT Insurance Companies
Whats Medicaid Secondary Health Insurance
Now lets cover how Medicaid can serve as secondary health insurance to Medicare.
Medicare is the primary payer for services it covers. These services commonly include visits to the doctors office as well as care in a hospital, at home, or in a skilled nursing facility. When a covered person obtains services from a provider that accepts both Medicare and Medicaid as forms of coverage, Medicaid may cover shared Medicare costs such as copays and coinsurance.
Depending on income, Medicaid may provide cost-sharing help through the Qualified Medicare Beneficiary program. The program may also provide assistance with the cost of prescription drugs or optional coordination of care.
Thats why its important to know whether you are eligible for Medicaid and, if so, to be sure to apply for the program.
Whenever possible, its also important to ask your providers about your coverage and costs before receiving services.
If you currently carry a Medigap policy and are looking for Medicaid to replace it, make sure you understand the ramifications of cancelling that coverage and are fully approved for Medicaid before making any changes.
Read Also: What Is The Income Limit For Arkansas Medicaid
How Do I Find Out About Medicaid Programs In My State
To learn more about Medicaid cost sharing requirements and programs in your state, visit Medicaid.gov and select your state in the State Profiles box on the right.
Youll be linked to your states Medicaid page, which can help answer any questions about Medicaid costs and options in your state.
If you are a Medicare dual eligible individual , looking into Medicare Advantage Plans may be a wise move and a good investment. Call MedicareMall toll-free at 413-1556 and well be glad to help you determine whether Medicare Advantage is right for you.
For further information about Medicaid, visit Medicaid.gov. If youd like information about Medicare supplement plans, Medicare Advantage, or any other aspect of Medicare or senior health insurance, contact a licensed, bonded MedicareMall representative and let us lead you with confidence through the Medicare maze!
If I Have Medicare Or Medicaid Do I Need To Purchase Additional Policies To Supplement It
QUESTION: I was wondering what are people over 65 doing regarding picking plans to supplement Medicare and Medicaid. Can anyone suggest some plans that are good to fill in the gaps? What needs to be purchased to supplement Medicare and Medicaid? Thank you!
-Barbara
ANSWER: Medicaid coverage is quite comprehensive, and beneficiaries do not purchase additional policies to supplement it. Also, since Medicaid is intended for the poor, very few beneficiaries could afford it, anyway. If you are over age 65 and covered by both Medicare and Medicaid, you have one of the best insurance arrangements around. All Medicare eligible services are covered with no, or very small, copayments and deductibles.
If you are enrolled in Medicare but are not eligible for Medicaid, the ACA makes no changes to the way youpurchase a supplement policy. You have the option of either a Medigappolicy or a Medicare Advantage Plan . Medigap policies help pay for Medicare’s coinsurance and deductibles and often for some additional benefits, such as emergencies during foreign travel. However, if you want coverage for prescription drugs, you have to purchase it separately.
Robert I. Field, Ph.D., J.D., M.P.H. is a professor of law at the Earle Mack School of Law and professor of health management and policy at the School of Public Health at Drexel University. He also writes for The Field Clinic blog. Ask Rob your questions about the new healthcare law.
You May Like: Medicaid Funded Home Care Services
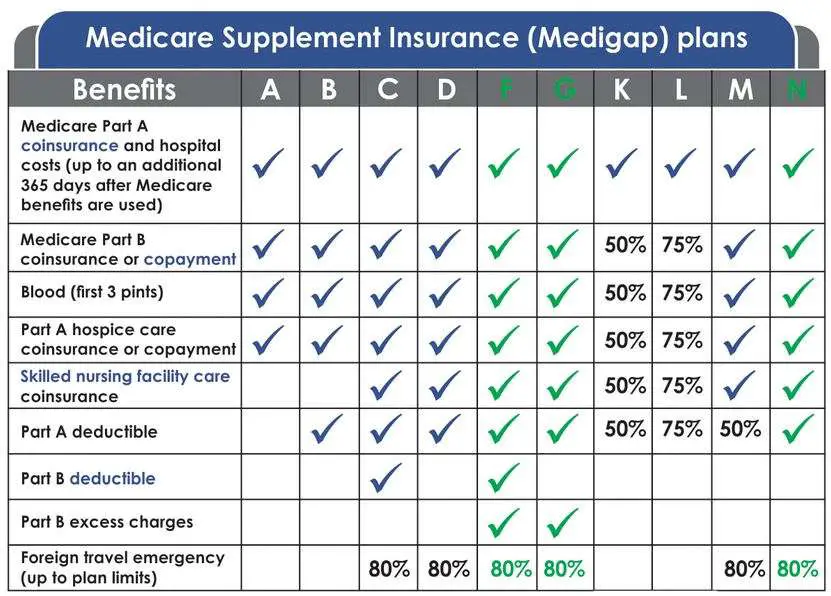
What Does Medicare Supplement Insurance Cover
Medicare Supplement insurance is sold in 12 standard plans. Plans C and F are only available to people who were eligible for Medicare before January 2020.
Every company must sell Plan A, which is the basic plan, or the “core benefit” plan. The standard plans are labeled A through L. Remember, the plans are standardized. So, Plan F from one company will be the same as Plan F from another company. Select the supplement policy which fits your needs, and then purchase that plan from the company which offers the lowest premiums and best customer service. Core Benefits: Included in all plans.
- Pays Part A Hospital copayment
- Pays for an additional 365 days of hospitalization after Medicare benefits end.
- Pays Part B copayment
You will have to pay part of the cost-sharing of some covered services until you meet the annual out-of-pocket limit. Plan K has a $6,220 out-of-pocket limit. Plan L has a $3,110 out-of-pocket limit . Once you meet the annual limit, the plan pays 100% of the Medicare copayments, coinsurance, and deductibles for the rest of the calendar year. These amounts can change each year.
Dropping Your Whole Medigap Policy
You may decide that you want a completely different Medigap policy and not just your old Medigap plan without the prescription drug coverage. Or you may want to move to a Medicare Advantage Plan that provides prescription drug coverage. You may also decide that you want to drop your Medigap policy entirely.
If you want to drop your whole Medigap policy, you must be careful regarding timing. Make sure you understand cancellation and coverage start dates so you arent left without necessary coverage.
Ask questions of your providers to be sure all your needs will be covered before making any changes.
Don’t Miss: If I Have Medicaid Do I Qualify For Food Stamps
Guide To Medicare Supplement
To purchase Medicare Supplement Insurance you must be enrolled in Medicare Part A and Part B. Medicare Supplement Insurance provides coverage for gaps in medical costs not covered by Medicare. Medicare Supplement plans are standardized and offer various benefits to help offset your healthcare cost.
The California Department of Insurance regulates Medicare Supplement policies underwritten by licensed insurance companies. The CDI assists consumers in resolving complaints and disputes concerning premium rates, claims handling, and many other problems with agents or companies. The Consumer Hotline 800-927-4357 is serviced by experienced professionals who will answer your questions, or assist you in filing a complaint.
To find information on Medicare Supplement Insurance, the names of companies authorized to sell it and compare premiums, please visit our Guide to Medicare Supplement page.
How Policies Are Priced
One difference in premiums can arise from how they are “rated.” If you know this, it may help you anticipate what may or may not happen to your premium down the road.
Some policies are “community rated,” which means everyone who buys a particular plan pays the same rate regardless of their age.
Others are based on “attained age,” which means the rate you get at purchase is based on your age and will increase as you get older. Still others use “issue age”: The rate won’t change as you age, but it’s based on your age at the time you purchase the policy .
Premiums also may go up from year to year due to other factors, such as inflation and insurer increases.
It’s worth choosing an insurance company that has a good track record, Gavino said.
“Sometimes new carriers come into the market and have really low rates to entice people but then after a year of claims under their belt, they may have to raise rates significantly,” Gavino said. “I’ve seen it a lot.”
Read Also: What Is The Household Income Limit For Medicaid
When Can I Buy Medigap
After you are signed up for Medicare Part A and Part B, you can look into getting Medigap. The open enrollment period for Medigap automatically starts the first month you have Medicare Part B , as long as you’re at least 65 years old. It is important to purchase Medigap during the open enrollment period, or it might become unavailable to you or overly expensive.
Is Medicare Supplemental Insurance Right For You
Medigap plans are a supplemental insurance option for those already enrolled in original Medicare who are seeking extra financial coverage. When you participate in a Medigap plan, youll receive coverage for specific costs like deductibles, coinsurance, and copayments. But youll still need to cover some out-of-pocket expenses for the services you receive.
Remember, however impressive the terms of Medicare supplemental insurance may be, the plans arent designed to stand alone or replace your regular health insurance.
Supplemental insurance is how it sounds: a supplement. Before signing a policy, make sure that you completely understand the advantages and limitations of the policy. If you dont, its best to perform some more research or reach out to Medicare for more information.
If you cannot afford Medigap or Medicare supplemental insurance, Medicaid may cover those costs that Medicare does not.
Also Check: Find A Neurologist That Takes Medicaid
What Do I Need To Know When Comparing Plans
First, there are no provider networks with Medicare Supplement insurance plans. Plans can be used with any doctor or hospital that accepts Medicare. Second, the basic benefits offered by Plans A, B, C, F, G, K, L and N are the same from every insurance company. However, some companieslike Humanaalso offer additional benefits. Take some time to consider the differences is in the companies, the quality of service and the price.
Organizing For Medicaid Expansion
Missourians mobilized by the thousands to get Medicaid expansion on the ballot this year, a move that will impact 230,000 low-income residents in the coverage gap.
For almost a decade, advocates in Missouri have been lobbying their legislators to expand Medicaid coverage in the red state.
Since the Supreme Court ruled in 2012 that the Medicaid expansion under the Affordable Care Act was optional, 36 states plus Washington, D.C., have adopted and implemented the expansion. In those states where coverage has not been expanded, the decision has come at a devastating cost to Americans who fall into the coverage gap, advocates said.
When the Affordable Care Act was originally passed, folks who were making up to 138% of the federal poverty level were supposed to be on Medicaid. And folks making more than 138% of the federal poverty level would be given subsidies to buy coverage through the exchange or healthcare.gov, Kelly Hall, director of health policy for the Fairness Project, told ABC News.
Because some states havent expanded their Medicaid program, they are creating a problem for people who dont make enough money to get the subsidies on the exchange, but they make too much money to be on their states Medicaid program.
ABC News is examining the coverage gap and expansion of Medicaid as part of its My America video series, which highlights issues that are key to the electorate in the run-up to the 2020 election and spoke to voters and experts about the issue.
Recommended Reading: Does Medicaid Cover Substance Abuse Treatment
Is Medicare The Same Thing As Medicaid
Although they sound similar, Medicare and Medicaid arent the same. The only similarity is that both government programs help cover health care costs for Americans.
Medicaid is designed for people that fall into a certain income bracket while Medicare is for people over the age of 65 or for those that have been on disability for two years, explains Grant Dodge, a broker at Health Benefits Associates Inc., in Reno, Nevada.
Medicaid doesnt have an age requirement, so adults of all ages and dependent children can enroll. In 2021, there were 75.4 million people covered with Medicaid. Medicaid plans are administered by the states but funded jointly by the state and federal government. Medicare is a federal program managed by the United States Centers for Medicare and Medicaid Services . The U.S. Social Security Administration handles Medicare enrollment and premium payments. It has an age requirement unless youve been on disability for 24 months or have specific medical conditions. Once you have both parts of Medicare from the federal government , you can sign up for additional coverage with private insurance carriers to fill in the gaps of Medicare, explains Dodge.
If Your Or Your Spouse’s Employer Has 20 Or More Employees Then The Group Health Plan Pays First And Medicare Pays Second
If the
didn’t pay all of your bill, the doctor or
should send the bill to Medicare for secondary payment. Medicare will pay based on what the group health plan paid, what the group health plan allowed, and what the doctor or health care provider charged on the claim. You’ll have to pay any costs Medicare or the group health plan doesn’t cover.
Employers with 20 or more employees must offer current employees 65 and older the same health benefits, under the same conditions, that they offer employees under 65. If the employer offers coverage to spouses, they must offer the same coverage to spouses 65 and older that they offer to spouses under 65.
Recommended Reading: Who Is Not Eligible For Medicaid
