Medicaid Benefits And Ssi
If you already get Supplemental Security Income in SSA, the regional area office will automatically register you in Medicaid. If you apply and are eligible for TANF , then you will most likely receive expedited aid with your Medicaid application. In certain states, you may automatically get Medicaid. If you do not already have SSI benefits or Social Security Disability Insurance from Social Security, you could concurrently apply for Medicaid because of your limited fiscal resources and/or a severe medical or health condition or handicap.
Medicaid differs considerably from personal medical insurance. Medicaid may restrict your ability to visit exactly the exact same medical and healthcare providers which you used previously. Recent limitations on the Medicaid program can limit your accessibility to specific medical providers. The state agency which accepts Medicaid applications also receives applications for both cash assistance as well as the SNAP! Food stamps app.
View Or Download Our Free Guide
While we are not affiliated with the government in any way, our private company engaged writers to research the Medicaid program and compiled a guide and the following answers to frequently asked questions. Our goal is to help you get the benefits that you need by providing useful information on the process.
Our free Medicaid Guide is filled with helpful information about how to apply, program eligibility and how to get in touch with local offices. You can view or download our free guide here.
Read Also: Tolls Dc To Ny
We Also Encourage You To Download Our Take On Obtaining Medicaid For Home Care:
Please Note: Information provided herein is for convenience purposes. Nothing on this page or website constitutes legal advice, and we recommend that you verify all information on your own and seek legal counsel where appropriate. Please see full disclaimer at the bottom of this page.
When it comes to Medicaid in NY State, the first thing that one needs to determine is the applicants budgeting category. People in different age groups and circumstances are subject to different eligibility rules, and the services available in each category may also vary. In this section we will be discussing eligibility and services for the aged, blind, and disabled. This category includes people who are 65 and above, certified blind by the Commission for the Blind and Visually Handicapped, and certified disabled by Social Security or NY State . There are three levels of Medicaid for this category:
- Community Medicaid
Get help applying for Medicaid for home care
What is Covered by Community Medicaid?
While Medicaid covers prescription drugs, people with Medicare will not have their prescription drugs paid for by Medicaid directly. Rather, Medicaid will pay Medicare to provide a free Medicare Part D prescription drug plan for these beneficiaries. Click here to learn more about this.
Community Medicaid with Long-Term Care provides everything that Community Medicaid does with the addition of community based long-term care services such as home care, adult day care, and assisted living .
Also Check: Dentist Who Accept Medicare And Medicaid
New York Waiver Factsheet
NY Long Term Home Health Care Program
Provides respite, assistive technology, community transitional services, congregate and home delivered meals, environmental mods, home and community support services, home maintenance, medical social services, moving assistance, nutritional counseling/education services, respiratory therapy, social day care transportation, social day care for aged individuals ages 65 â no max age and physically disabled ages 0 64
Donât Miss: Where Is The Wax Museum In New York
The Way To Create An Signature For A Pdf Document In Google Chrome
The guidelines below will help you create an signature for signing new york medicaid application in Chrome:
Once youve finished putting your signature on your medicaid application ny pdf, decide what you want to do next download it or share the file with other people. The signNow extension gives you a selection of features for a better signing experience.
Recommended Reading: Does Medicaid Cover Clinical Trials
Eligibility Requirements For New York Medicaid Benefits
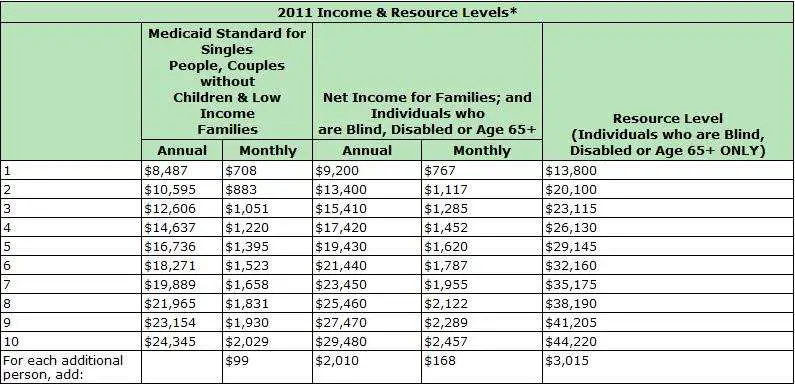
In order for New York seniors to be eligible for Medicaid services, they must meet certain financial eligibility requirements. First of all, an individual must be disabled or 65 years of age or older at the time of application.
There are additional requirements for New York Institutional Medicaid. In order for an individual to be eligible to receive New York Institutional Medicaid benefits, he or she must be under the appropriate asset limit set by Medicaid. Those limits are currently as follows:
- Single person $15,150
- Couple $22,200
In the event that only one spouse is seeking admission to a facility, the community spouse will be able to retain at least $74,820or a maximum of one-half of the couples joint liquid assets up to a maximum of $123,600. In the event the assets are over $123,600,there may be other rules that apply.
In Medicaid terminology, the snapshot date refers to the first day of the month on which one spouse goes to a facility, and the assessment of the couples joint liquid assets occurs from this date.
The Way To Create An Signature For A Pdf Document Online
Follow the step-by-step instructions below to design your new york medicaid application:
After that, your medicaid application ny pdf is ready. All you have to do is download it or send it via email. signNow makes signing easier and more convenient since it offers users a number of additional features like Merge Documents, Invite to Sign, Add Fields, and so on. And because of its cross-platform nature, signNow can be used on any device, desktop computer or mobile phone, regardless of the operating system.
Also Check: How Do I Get A Free Medicaid Phone
New York Medicaid Application
As of June 2015, the average monthly enrollment in the New York Medicaid program reached 6,441,902. The state of New York chose to make its own health benefits exchange situated at the NY State of Health website. Before the execution of the Affordable Care Act, New York was ahead of the medical insurance market concerning coverage for residents.
The health benefits market was created in 2012 by Governor Andrew Cuomo. Prior to the beginning of the state-funded market, the country ran Family Health Plus. This strategy was aimed toward providing health insurance coverage for low income adults residing in the state of New York. The state has expanded its Medicaid program since its beginning, covering hundreds of thousands more New Yorkers as a result.
Whats Covered Under Medicaid
Whos Covered Under Medicaid
- Adults who receive incomes of around 138 percent of the federal poverty level are eligible to receive Medicaid coverage.
- Pregnant women and babies whose household income doesnt exceed 218 percentage of the federal poverty level are eligible for coverage under the program.
- For kids in New York, CHIP is another program which allows participation for children whose family income doesnt exceed 400 percent of the federal poverty level.
After the Medicaid Application
Eligible parties will be given a letter telling them of the acceptance or rejection for New York Medicaid coverage.
Hearings on the Application Procedure
PO Box 1930
General Eligibility Requirements For 2021
Most long term care applicants will be either disabled, aged 65+, or have diagnosed blindness. As such, they will be subject to the Non-Magi standard, essentially the pre-affordable care act standard.
3. Income Limitations if single, the applicants income must be no higher than $825.00 per month .
- There is a personal needs allowance of $50.00 per month, which is not factored into the total income, for the person receiving long term care services.
4. Asset Limitations Medicaid divides assets into two categories: Exempt and Available. Exempt assets are specifically designated under the rules, and ownership of an exempt asset by the applicant will not result in a denial of benefits. If an asset is not listed as exempt then it needs to be liquidated and applied toward the costs of nursing home care before the applicant can receive Medicaid benefits. The state has a look back period of 5 years with a penalty for people who sell assets below fair market price, transfer assets to others, or give money and property away.
Exempt Assets in 2021 for an applicant in New York include:
i. $15,150 or less in cash/non-exempt assets if single. If the assets exceed the limit on the first of the month the applicant is ineligible for the entire month. If married and both spouses reside in a nursing home, the asset allowance for a couple is $22,200.00.
iii. One car, no equity amount specified.
iv. An irrevocable funeral trust, no amount specified.
Spousal Rules for 2021:
Read Also: Tens Unit Covered By Medicaid
How To Apply If In Ny City:
If you are in New York City, you can easily obtain applications from Human Resources Administration. You can also request information and applications on phone by calling at 718 557 1399.
NOTE: If you need any further assistance, you can call helpline at 693-6765.
Other requirements for applying
In order to apply for Medicaid, you will need to provide
- Proof of age
- Proof of citizenship
- If someone above 65 years of age, disabled or blind lives with you, you will need to provide proof of your income and resources
- Proof of your residence
- If you have any other insurance, you’ll be required to provide its proof and information about it
Medicaid Benefits
Medicaid provides a comprehensive coverage for various health services including
- Inpatient and outpatient services
- Home health care through approved agencies
- Access to smoking cessation agents
- Lab facilities and access to tests
- Eye, dental and mental health services
- Prescription drugs, medical supplies, and necessary medical equipment
- Transportation services
Medicaid Cancer Treatment Program
The Medicaid Cancer Treatment Program for breast and/or cervical cancer or colorectal and/or prostate cancer provides full Medicaid coverage for individuals whose income is higher than the Medicaid medically needy income levels. See below, Additional Medicaid Benefits, Medicaid Cancer Treatment Program.
Recommended Reading: Children’s Medical Services Medicaid Florida
Governor Pushed Back Against Gop Efforts To Repeal The Aca
In January 2017, as President Trump was poised to take office and it was clear that GOP lawmakers were going to push hard for ACA repeal, New York Governor Andrew Cuomo, announced that 2.7 million people were at risk of losing Medicaid coverage in New York if the ACA was repealed and not replaced with something equally robust, and that the state budget impact would be $3.7 billion.
Although most of the New Yorks Medicaid enrollees were already eligible under the states pre-2014 guidelines, the state estimated that several million Medicaid enrollees would have lost coverage if the ACA had been repealed. Thats because the state was using 1115 waivers to expand coverage eligibility in the years prior to ACA implementation, and the federal government was splitting the cost with the state as called for in the waivers.
But those waivers expired after Medicaid expansion was implemented. If the ACAs Medicaid expansion had been repealed, eligibility would have reverted to much lower thresholds: parents with dependent children would have been covered with income up to 94 percent of the poverty level , and childless adults wouldnt have been eligible at all. The state would have been allowed to spend their own money to extend those guidelines, but it would have been fiscally challenging without the federal match.
Medicaid expansion in New York
How To Apply For Medicaid
You can request an application for Medicaid by phone, by mail or in person through your local department of social services . VNSNY CHOICE representatives can help you understand if you are eligible, and then guide you through every step of the application process.
You can also complete the application yourself by going online to the ACCESS NY Health Care website and following the instructions at: . Applications and assistance in filling them out can also be obtained by calling New York Health Options at . You will need:
- Proof of age, like a birth certificate
- Proof of citizenship or alien status*
- Four weeks of recent paycheck stubs
- Proof of your income from sources like Social Security, Supplemental Security Income , Veterans benefits, retirement, Unemployment Insurance Benefits , Child Support payments
- If you or anyone who lives with you is 65 years old or older, certified blind, or certified disabled, you need to give information on bank accounts, insurance policies and other resources
- Proof of where you live, like a rent receipt, landlord statement, mortgage statement, or envelope from mail you received recently
- Insurance benefit card or the policy
- Medicare Benefit Card
New York State Medicaid information: www.health.ny.gov/health_care/medicaid/. * Medicaid coverage is available, regardless of alien status, if you are pregnant or require treatment for an emergency medical condition .
Read Also: What Eye Center Accept Medicaid
How To Apply For Medicaid In Ny
Millions of people all across the United States rely on Medicaid for their health coverage. The program is designed for low-income adults, people with disabilities, and older adults, among others.
Medicaid is sponsored by the government to provide coverage to low-income patients who arenât able to afford medical care otherwise. It is run jointly by both the state and federal governments.
If you live in New York, this article will be an easy to understand guide covering all you need to know about Medicaid in NY.
We will discuss eligibility requirements, what proof you need, the benefits you can receive if eligible, and more.
Medicaid Offers A Full Range Of Health Services For Eligible Persons Including:
- All regular medical checkups and needed follow-up care.
- Immunizations.
- Medical equipment and appliances .
- Lab tests and x-rays.
- Eye care and eye glasses.
- Emergency care.
- Emergency ambulance transportation to a hospital.
- Hospital stays.
For some pregnant women, services may be limited to perinatal care if their incomes are too high to qualify for full Medicaid coverage.
For children birth to 21 years old, Medicaid offers the Child/Teen Health Program , which provides the services listed above for all Medicaid recipients. C/THP places an emphasis on preventive care and treatment. For example, Medicaid requires that all children be screened with a blood lead test at one and two years of age. C/THP is available from fee-for-service healthcare providers. Also, all managed care plans must offer C/THP to Medicaid recipients under 21 years of age who are enrolled in their plan.
Child Health Plus and Family Health Plus provide services to eligible children and adults, respectively, through managed care plans.
Don’t Miss: Does Medicaid Cover Substance Abuse Treatment
How To Apply For Ny Medicaid
You may apply for Medicaid in the following ways:
- Enrollment Assistors offer free personalized help.
- To speak with the Marketplace Customer Service Center call 355-5777
- Through a Managed Care Organization
- Call the Medicaid Helpline 541-2831
- Through your Local Department of Social Services Office
Where you apply for Medicaid will depend on your category of eligibility. Certain applicants may apply through NY State of Health while others may need to apply through their Local Department of Social Service . No matter where you start, representatives will help make sure you are able to apply in the correct location. For more information on determining your category of eligibility and where you should apply read on.
NY State of Health determines eligibility using Modified Adjusted Gross Income Rules. In general, income is counted with the same rules as the Internal Revenue Service with minor variations. Individuals who are part of the MAGI eligibility groups listed below should apply with NY State of Health.
- Adults 19-64 years of age and not eligible for Medicare,
- Children 1 – 18 years of age
- Infants ,
- Pregnant Individuals,
- Parents and Caretaker Relatives of any age
Individuals who are part of the non-MAGI eligibility groups listed below should apply with their Local Department of Social Services .
Other factors that may affect your eligibility include:
- State Residency
- Family or Household size
- Income
Medicaid Application for Non-MAGI Eligibility Group
Supplement A
What Proofs Will You Have To Bring To Apply For Medicaid
The evidence you need will vary depending on your age, medical conditions, and a few other factors.
These are some general requirements to give you an idea of what is needed.
Your case worker will let you know if there are any specific requirements for your application. Contact your local Medicaid office for more details.
Here is a list of the documents that you will need when applying for Medicaid in NY.
Also Check: Not Reporting Marriage To Medicaid
Institution For Mental Disease In Lieu Of Service Benefit
Institution for Mental Disease In Lieu of Service Benefit information
-
PDF 39.88KB â Last Updated: 11/12/2020
Notice:
New York State Department of Health has stated Medicaid recipients should receive breast cancer surgery services at high volume facilities .
See the listing of low-volume facilities that will not be reimbursed for breast cancer surgeries provided to Medicaid recipients.
This policy does not affect a facilityâs ability to provide diagnostic or excisional biopsies, and postsurgical care for Medicaid patients.
Clinical Practice Guidelines
UnitedHealthcare Community Plan has practice guidelines that help providers make healthcare decisions. These guidelines come from nationally recognized sources. UnitedHealthcare Community Plan has practice guidelines for preventive health and other health conditions.
View the entire list of guidelines or call our Member Services at 1-800-493-4647 to request a printed copy.
-
PDF 2.36MB â Last Updated: 10/13/2021
Summer
-
PDF 1.97MB â Last Updated: 07/06/2021
Spring
-
PDF 6.45MB â Last Updated: 03/18/2021
Winter
Determine How You Will Submit Claims To Emedny
Providers are given several options for submitting claims to eMedNY
Option 1: HIPAA Compliant Claim Formats Submitted Directly to eMedNY
Option 2: Medicaidâs Electronic Provider Assisted Claim Entry System web-based application
- Claims: Professional Institutional and Dental
- Claim Status Requests**
- Prior Approval Requests
- Eligibility Verification
*Real-time means that the claims are processed instantaneously and the provider can view the status of a real-time claim within seconds. There is no need to wait for a remittance statement to be mailed to find out about the status of submitted claims. **The status of claims submitted via the ePACES batch feature is generally available within 24 hours. To enroll in ePACES:
Option 3 Paper Claim Forms
Read Also: Dentist That Take Medicaid For Adults In Monroe La
