Frequently Asked Questions About Medicaid Expansion
Misconceptions about Medicaid expansion under the Affordable Care Act obscure the fact that the Medicaid program boasts a long track record of proven effectiveness in providing care and assistance to those most in need.
A centerpiece of the Patient Protection and Affordable Care Actoften referred to as Obamacareis the expansion of Medicaid eligibility to people with annual incomes below 138 percent of the federal poverty level, or $26,347 for a family of three and $15,417 for an individual. Despite the fact that the Affordable Care Act was passed into law in 2010 and was subsequently upheld by the U.S. Supreme Court in the summer of 2012, many questions persist about the law, particularly as it relates to Medicaid expansionwhat that expansion actually means, who it will cover, what it will cost, and more.
As we mark the third anniversary of the passage of the Affordable Care Act, it is important not to lose perspective about what Medicaid expansion actually means for the millions of people it will help to insure, as well as the economic benefits it will bring to states and local economies. Here are the 10 questions about Medicaid expansion under the law that are asked most frequently and are too often answered incorrectly.
How To Apply For The Medicaid Expansion
Individuals can also apply by submitting a paper application by telephone toll free 854-4825 or 711 for people with hearing impairments, mail, or in-person at their Human Service Zone office .
If an individual does not qualify for Medicaid, the individual can explore whether he or she may qualify for federal health insurance marketplace coverage at www.healthcare.gov.
Medicaid Expansion Provides More Comprehensive Affordable Coverage For Many Oklahomans
The goal behind the Medicaid program including expanding coverage to low-income residents is to provide accessible health care for people who need it. Due to improved coverage and lower costs, some Oklahomans will move from other insurance plans to Medicaid. This move benefits both the enrollees and the state, as access to more comprehensive and affordable care leads to a more productive, reliable, and healthy workforce for our state.
About 68,000 Oklahomans became eligible for expansion benefits because the Oklahoma Health Care Authority reprocessed their applications to check for expansion eligibility. Of those, somewhere between 23,000 and 38,000 were previously eligible for Insure Oklahoma, the program that allows individuals to purchase health care from the state. For qualifying individuals, the transition to Medicaid coverage will mean access to a health plan without paying monthly premiums. For people making less than 138% of the federal poverty line , Insure Oklahoma premiums made it unaffordable for some low-income workers. Providing more affordable coverage through Medicaid expansion will likely make accessing health care more feasible for many people. As thousands move from Insure Oklahoma to Medicaid expansion, the transition will save the state money through a higher federal matching rate.
You May Like: United Healthcare Medicaid Louisiana Application
Soonercare Income Guidelines For Expansion Adults
| Size of Family |
|---|
Ninety percent of costs for expansion enrollees will be paid by the federal government.
Maximizing federal funding allows the state the ability to:
- Promote integrated care and improve health outcomes, explore reinstating an adult dental benefit in SoonerCare, with a focus on preventive dental services.
- Pursue substance use disorder and serious mental illness waivers to expand access to prevention and treatment services.
- Coordinate with jails and prisons to help former inmates apply for SoonerCare coverage upon release, helping them get access to important behavioral health services immediately, thus reducing the risk of recidivism.
- Help jails and prisons capture additional SoonerCare funding for hospitalizations and surgeries as allowed under federal Medicaid law.
Help Support This Work
Public Integrity doesnt have paywalls and doesnt accept advertising so that our investigative reporting can have the widest possible impact on addressing inequality in the U.S. Our work is possible thanks to support from people like you.
Republish our articles for free, online or in print, under a Creative Commons license.
This work is licensed under a Creative Commons Attribution-NoDerivatives 4.0 International License.
Recommended Reading: Can Medicaid Take Your Pension
For Questions On Services And Other Support Through Dec 31 2021 Contact Sanford Health Plan Member Services
- Toll-Free: 305-5060 / TTY 652-1844
- E-mail:
To get prior approval of health care services, e-mail or call toll-free 276-7214 – Select option 2.
People who have been notified that they qualify for North Dakota Medicaid Expansion coverage, can get plan information at .
Note: Sending an email to this Sanford Health Plan email address is not a secure form of communication. There is some risk that confidential information sent in an email may be misdirected, disclosed to or intercepted by, unauthorized third parties. To protect privacy, members or visitors concerned about security of email communications should call the numbers listed above. If you choose to send an email, you consent and accept the risk of transmitting confidential information via unencrypted email.
For questions on services and other support starting Jan. 1, 2022, contact Blue Cross Blue Shield of North Dakota Member Services.
- Toll-Free: 777-5779 / 711 – This number is now accepting calls from Medicaid Expansion members.
- 711 or 366-6888
- Find a Doctor: www.bcbsnd.com/members/find-a-doctor
If Your Income Is Low And Your State Hasnt Expanded Medicaid
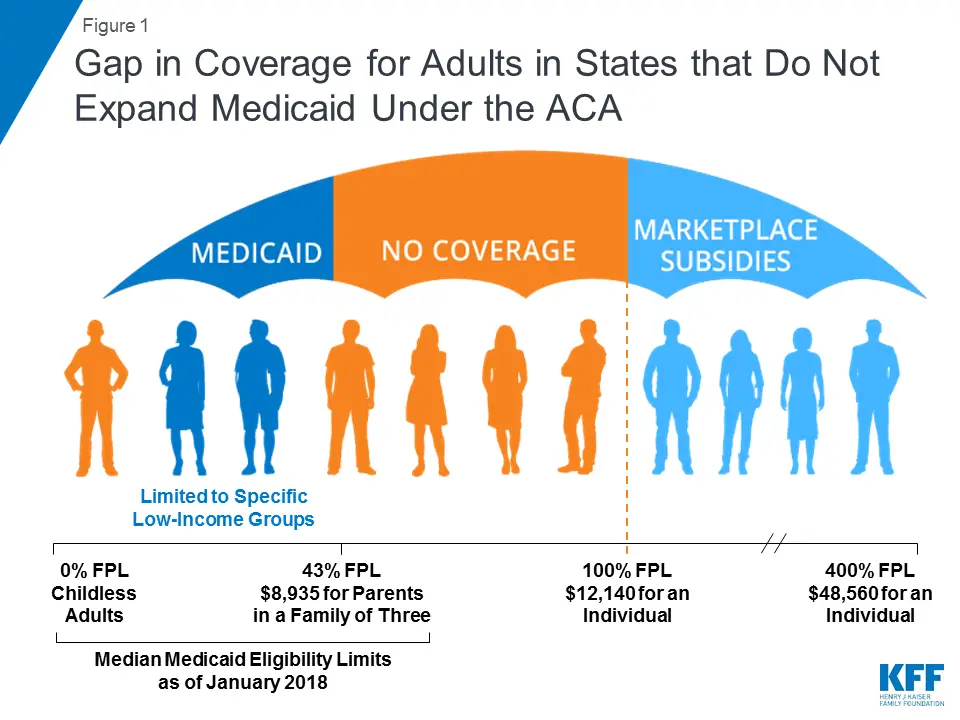
If your state hasnt expanded Medicaid, your income is below the federal poverty level, and you don’t qualify for Medicaid under your state’s current rules, you wont qualify for either health insurance savings program: Medicaid coverage or savings on a private health plan bought through the Marketplace.
- Find out why
-
- When the health care law was passed, it required states to provide Medicaid coverage for all adults 18 to 65 with incomes up to 133% of the federal poverty level, regardless of their age, family status, or health.
- The law also provides premium tax credits for people with incomes between 100% and 400% of the federal poverty level to buy private insurance plans in the Health Insurance Marketplace®.
- The U.S. Supreme Court later ruled that the Medicaid expansion is voluntary with states. As a result, some states havent expanded their Medicaid programs.
- Adults in those states with incomes below 100% of the federal poverty level, and who dont qualify for Medicaid based on disability, age, or other factors, fall into a gap.
- Their incomes are too high to qualify for Medicaid in their states.
- Their incomes are below the range the law set for savings on a Marketplace insurance plan.
-
States are continuing to make coverage decisions. They could expand Medicaid in the future.
Recommended Reading: Iowa Medicaid Customer Service Number
Alternative Policies For Medicaid Expansion Populations
Some states use Section 1115 research and demonstration waivers to test policies not allowed under traditional Medicaid, such as imposing higher cost sharing for some expansion enrollees or placing limitations on certain mandatory benefits.
Specifically, most of the states with these types of demonstrations have implemented beneficiary contributions programs, which involve changes to the premium and cost sharing schedules. Several states restrict retroactive eligibility. A small number of states place limitations on the non-emergency medical transportation benefit. One state, Arkansas, is using premium assistance to purchase plans on the exchange under its demonstration. Although several states planned to implement work and community engagement requirements, such requirements are not currently in effect in any state.
In 2021, CMS notified many of these states that certain elements of their demonstrations are being withdrawn, and that other elements of their demonstrations are under review. As such, it is unclear which elements of these demonstrations will continue.
American Disabilities Act Notice
In accordance with the requirements of the federal Americans with Disabilities Act of 1990 and Section 504 of the Rehabilitation Act of 1973 , UnitedHealthcare Insurance Company provides full and equal access to covered services and does not discriminate against qualified individuals with disabilities on the basis of disability in its services, programs, or activities.
Don’t Miss: Florida Medicaid Gold Card Providers
How Many People Are On Medicaid
According to the Centers for Medicare & Medicaid Services, as of November 2020, here are the number of people enrolled in Medicaid and Chip in the entire United States:
- 78,521,263 individuals were enrolled in Medicaid and CHIP
- 72,204,587 individuals were enrolled in Medicaid
- 6,695,834 individuals were enrolled in CHIP
Read Also: Can Medicaid Be Transferred To Another State
What Does Adult Expansion Medicaid Cover Utah
The federal government covers 90% of the costs for these services, with the state covering the remaining 10%. It is estimated that up to 120,000 Utah adults are eligible for the expansion program.Medicaid Expansion. MAXIMUM INCOME GUIDELINES Family Size Per Month Per Year MAXIMUM INCOME GUIDELINES 1 $1,481.
Recommended Reading: Nursing Homes In Tulsa That Accept Medicaid
Nebraska Medicaid Eligibility And Enrollment
- Are you eligible for Nebraska Medicaid? Find out how to enroll in Medicaid in Nebraska for individual and family coverage and how it differs from other states.
More than 266,000 participants benefit from Nebraska Medicaid each month because they are 65 years of age and older, pregnant, blind or disabled.
Medicaid helps provide families and their children the medically necessary services they need but otherwise cant afford. Caretakers responsible for children 18 years of age and younger are also eligible for state Medicaid benefits.
Nebraska offers a program for residents age 19 through 64 who earn up to 138% of the federal poverty level about $17,000 a year for a single person and $34,000 for a family of four. Coverage includes services like routine doctor visits, hospitalization and prescription drug benefits. In some cases, enrollees may qualify for additional benefits like dental and vision.
Childrens Health Insurance Program

The Childrens Health Insurance Program is a public healthcare program for low-income children who are ineligible for Medicaid. CHIP and Medicaid are related programs, and the former builds on Medicaids coverage of children. States may run CHIP as an extension of Medicaid, as a separate program, or as a combination of both. Like Medicaid, CHIP is financed by both the states and the federal government, and states retain general flexibility in the administration of its benefits.
CHIP is available specifically for children whose families make too much to qualify for Medicaid, meaning they must earn incomes above 138 percent of the federal poverty level, or $33,948 for a family of four in 2017. Upper income limits for eligibility for CHIP vary by state, from 175 percent of the federal poverty level in North Dakota to 405 percent of the FPL in New York. States have greater flexibility in designing their CHIP programs than with Medicaid. For instance, fewer benefits are required to be covered under CHIP. States can also charge a monthly premium and require cost sharing, such as copayments, for some services the total cost of premiums and cost sharing may be no more than 5 percent of a familys annual income. As of January 2017, 14 states charged only premiums to CHIP enrollees, while nine states required only cost sharing. Sixteen states required both premiums and cost sharing. Eleven states did not require either premiums or cost sharing.
You May Like: How Does Medicaid Work In Texas
Medicaid & Braces For Children
Under the EPSDT program, Medicaid provides many benefits to children that are not offered to adults. These services provide dental care, screening, and preventive services to children under 21 years of age in every state. This can include braces! However, the medical necessity of the braces will determine whether Medicaid will cover them. If braces are deemed medically necessary for your child, then Medicaid will cover them. Medical necessity will be determined by a dentist or orthodontist registered with the American Association of Orthodontists.
There are several different reasons why braces might be medically necessary. Cosmetic reasons will not qualify your child for coverage under Medicaid. Your orthodontist will look at your childs records and condition to determine the necessity. Here are some conditions that will usually deem braces medically necessary:
- Cleft palate
- Malocclusion
If your child has any of the medical conditions above, then he or she is likely eligible for orthodontic treatment that will be covered by Medicaid. Medicaid will typically only cover metal braces and not clear or ceramic braces. Once you know that Medicaid will pay for braces, you will need to find an orthodontist who accepts Medicaid.Finding a doctor who accepts Medicaid can be difficult, but you can typically visit the website of your carrier to find an online directory.
Unitedhealthcare Connected For Mycare Ohio
UnitedHealthcare Connected® for MyCare Ohio is a health plan that contracts with both Medicare and Ohio Medicaid to provide benefits of both programs to enrollees. If you have any problem reading or understanding this or any other UnitedHealthcare Connected® for MyCare Ohio information, please contact our Member Services at from 7 a.m. to 8 p.m. Monday through Friday for help at no cost to you.
Si tiene problemas para leer o comprender esta o cualquier otra documentación de UnitedHealthcare Connected® de MyCare Ohio , comuníquese con nuestro Departamento de Servicio al Cliente para obtener información adicional sin costo para usted al de lunes a viernes de 7 a.m. a 8 p.m. .
You May Like: Medicaid Exclusion List By State
Missouri Is The Sixth State To Expand Medicaid Via Ballot Measure
In the last few years, voters in Maine, Idaho, Nebraska, Utah, and Oklahoma have approved similar ballot measures to expand Medicaid. Missouri will be the sixth state to expand Medicaid in this manner.
Its also worth noting that while voters in Utah, Idaho, and Nebraska all approved Medicaid expansion ballot initiatives in 2018, all three states subsequently sought federal approval for Medicaid work requirements , and have imposed various other restrictions and requirements, as opposed to simply expanding Medicaid as called for in their voter-approved ballot initiatives.
But the amendment that voters passed in Missouri prohibits the state from imposing additional eligibility requirements on the expansion population that arent imposed on the rest of the states Medicaid-eligible population. The Biden administration has also notified states that work requirements will no longer be approved, so that would be a non-starter at this point.
Who Is And Who Isnt Gaining Coverage Under Medicaid Expansion
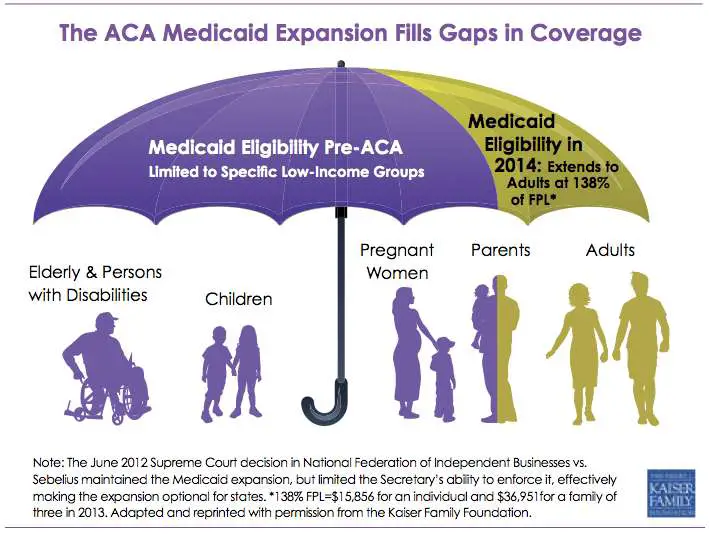
Medicaid, jointly funded by the state and the federal government, requires coverage for certain groups of individuals: low-income children and some of their parents poor pregnant woman certain low-income seniors and some individuals with disabilities who are under the age of 65. Under the Affordable Care Act, Medicaid eligibility will be extended to all individuals with incomes up to 138 percent of the federal poverty level beginning in 2014$26,347 for a family of three and $15,417 for an individual.
Recommended Reading: How To Find Out If I Qualify For Medicaid
What Will Medicaid Expansion Actually Cost States
The federal government is paying for the vast majority of the Medicaid expansion. States dont have to pay any percentage of the cost for the expansion until 2017, at which point the federal government will gradually transition to covering 90 percent of the cost through 2020. Before accounting for state and local government increases in savings and revenues, the nonpartisan Congressional Budget Office estimates that states will increase their Medicaid spending by only 2.8 percent while providing health coverage to 17 million more low-income children and adults between 2014 and 2022.
Some states are acknowledging that they could afford the expansion, but they fear the federal government will cut-and-run at some point, leaving them with a majority of the cost burden. The reality is, however, that there is absolutely no precedent for this. Moreover, if a state is committed to expanding Medicaid, there are ways to address this concern. Both Arizona and Nevada, for example, have adopted the circuit-breaker approach, in which the state will opt-out of the expansion only if the federal governments share of matching funds falls below a certain level.
Does Medicaid Cover Invisalign
No, unfortunately, Medicaid does not cover Invisalign. Medicaid coverage is limited to metal braces only. Metal braces are typically the cheapest option when it comes to orthodontic care. Most health insurance plans or dental insurance plans provide lower benefits for Invisalign and other cosmetically appealing options.
Metal dental braces might not be the most aesthetically appealing option for some people, but those are the only braces that will usually be covered by Medicaid. Some private or group healthcare coverage might still provide benefits for Invisalign or clear braces. However, Medicaid will typically not provide any coverage for those devices. So, if you opt for something other than metal braces, you might be stuck paying the entire cost on your own.
Read Also: Inpatient Drug Rehab Illinois Medicaid
Why Did I Get Denied For Medicaid
Theres a multitude of reasons why someone may get denied for Medicaid coverage. Aside from not meeting the financial or demographic requirements, some common reasons for a denied Medicaid application include:
- Incomplete application or documents
- Failure to respond to a request within a timely manner
- Late filing
- Disability not proven or otherwise not medically qualified
Dont forget that mistakes can be made on behalf of Medicaid, and you have a right to appeal Medicaids decision concerning your coverage. Contact your state Medicaid program for instructions about how to appeal a decision if you are denied benefits.
Can You Have Medicaid And Medicare At The Same Time
Yes, some beneficiaries are eligible for both Medicaid and Medicare. Depending on where you live and your eligibility, you may be able to enroll in a special type of Medicare Advantage plan called a Dual-eligible Medicare Special Needs Plan .
A D-SNP can offer benefits that Original Medicare dont cover, such as dental, hearing, vision and more. All D-SNP plans are required to cover prescription drugs.
To learn more about these special types of plans and to find out if any are available where you live, you can compare plans online or call to speak with a licensed insurance agent.
Recommended Reading: Vermont Medicaid Dental Fee Schedule
