Which Medicaid Plan Is Best In Virginia
The best Medicaid plan will be different from person to person based on their specific needs. There are a variety of plans to choose from. Not all of them are available in all areas, so check to see which ones are available to you before choosing one. You might also want to check with your doctors to see which plans they accept if you dont want to have to change doctors.
Requesting A Medicaid Hearing
The notice must also provide instructions on how to appeal the decision made by the Medicaid agency. In some states, the first step in the Medicaid appeal process is an administrative hearing, commonly known as a âfair hearing.â Other states, however, provide for a local âevidentiary hearing,â which may then be appealed through the fair hearing process. The notice should tell you how to request a hearing.
You may request a hearing whenever either your application for Medicaid has been denied or your existing Medicaid benefits have been reduced or terminated, and you believe the state Medicaid agency is mistaken in its analysis. You may also be able to request a hearing to dispute other aspects of the decision, such as a decision about how much you must contribute to the cost of your care or the amount of your benefit. The request for a hearing should be filed promptly since there is always a deadline for making such a request. In addition, when existing Medicaid benefits are improperly decreased or terminated, you may want to request that your benefits continue during the appeal process. Such a request, often referred to as a request for âaid paid pending appeal,â must be made within 10 days of the date on the denial or termination/reduction notice. As a cautionary note, however, you may be asked to repay these continued payments if you ultimately lose the appeal.
Children’s Health Insurance Program Health Plans
Children in CHIP get services through a medical plan in their area. Some CHIP plans also offer services to mothers who are pregnant. This is called CHIP perinatal coverage.
You can find the CHIP health plans in your area by using the Find Your Medical Plan search tool. You can see how well some CHIP health plans perform by looking at the CHIP health plan report cards.
To learn more about CHIP, visit the CHIP and Children’s Medicaid website.
You May Like: How To Obtain A Medicaid Provider Number
What If I Don’t Want My Medicaid Doctors And Providers To See My Health Information Through This Website
You can “opt out” of sharing. “Opt-out” means that you choose not to share your health information. To opt out, go to and then:
You can also opt out by calling 800-252-8263. If you opt out, we won’t share your health information with Medicaid doctors or other providers.
How Can I Change My Address And Phone Number

You can change your address and phone number by visiting YourTexasBenefits.com. You can also make changes by phone.
Phone
Important: You must report changes to your case within 10 days of the change.
Note:
- If you get Social Security benefits or Supplemental Security Income, you must contact them first to update your information. If your address isn’t correct in the Social Security system, the wrong address will show up in our system too. Call the Social Security office at 800-772-1213 to correct your address. After that, visit YourTexasBenefits.com or call 2-1-1 or 877-541-7905 to correct your address.
- We won’t send you another Your Texas Benefits Medicaid card unless you ask us to send you a new card to replace one that has been damaged, lost or stolen.
Recommended Reading: Apply For Medicaid Health Insurance
An Overview Of Medicaid Eligibility And Benefits
Jason DelCollo, DO, is board-certified in family medicine and on the faculty of Philadelphia College of Osteopathic Medicine.
Shereen Lehman, MS, is a healthcare journalist and fact checker. She has co-authored two books for the popular Dummies Series .
Covering more than 64.5 million Americans, Medicaid is the largest health insurance provider in the United States. The program, created under the Social Security Act Amendments of 1965, is available to low-income individuals in the fifty states, the District of Columbia, and U.S. territories. It is a collaboration between federal and state governments to provide coverage for basic health care.
Understanding how it works can help you to make the most of its benefits.
Which Medicaid Plan Would Be Best In Indiana
Indiana Medicaid has several different plans that provide coverage for certain groups of people. There is the Hoosier Healthwise which is for children up to the age of 19 and for pregnant women. The Hoosier Care Connect is for those individuals that have reached the age of 65 and older, also for the blind and disabled. Then there is the Healthy Indiana Plan which is available for all eligible adults between the ages of 19 and 64. To learn more about these main plans and others that are available go to the Indiana Government website and find the plan you need most.
Recommended Reading: Medicaid Data Warehouse New York
Q If I Have Private Health Insurance Can I Be Eligible For Medicaid
A. It depends. If your income is low, and you have minor children, you and your children can have private health insurance and still be eligible for Medicaid. Certain Medicaid qualifying programs require that you not have any other health insurance in order for you to get Medicaid. If you have both private health insurance and Medicaid, you should show both your Medicaid card and your private health insurance card to your medical provider each time you receive services.
How To Apply For Medicaid In In Virginia
If you want to apply for Virginia Medicaid, you will have to fill out an application and have the necessary documentation regarding your identity along with proof of income. If you are applying for your family or household, you will need the same documents for each member you are including.
Virginia Medicaid Application To download an application for Medicaid in Virginia, simply click here and download the application for the category you are applying for.
If you would like to apply for Medicaid online, you can do so through the Cover Virginia website. If you apply this way, you might still need to mail in documentation regarding residence, citizenship, and income. Once you have applied online, you will be able to check the status of your application using your Social Security Number and your login information. Medicaid forms shouldnt take any longer than 30 days to be fully processed.
Some people might prefer to apply in person and this can easily be done at the Department of Social Services office in your county. Once you get the application, fill it out completely and make sure that you have all of the necessary documentation with you. This will help to speed the process along. You can get the application in the Department of Social Services office or you can call them and have one sent to you in the mail.
Don’t Miss: Nursing Homes In Huntsville Al That Take Medicaid
Who Qualifies For Medicaid
Medicaid qualification is different in every state. You must be a resident of the state in which you are applying for benefits and must be a U.S. citizen or otherwise qualified non-citizen such as a lawful permanent resident.
Federal law requires every state to provide Medicaid to the following mandatory eligibility groups that meet certain income and asset requirements:
As you can see from the federal guidelines, the only reference to age is in regards to children. Each state governs its own Medicare program in adherence to federal regulations. Some states may have an age requirement in order to qualify for its Medicaid program while other states may not.
You can find your states Medicaid eligibility requirements to learn more.
Q Where Do I Go To Apply For Medicaid
A. There are several ways to apply for Medicaid and other medical assistance programs:
- On the internet, you can use ASSIST to check your eligibility for several different assistance programs by completing a self-screening questionnaire. ASSIST then allows you to apply online.
- You may also print an Application for Health Insurance/Medicaid. The application form is also available in Spanish/en Español.
- By phone, you can contact Medicaid Customer Relations at 1-800-372-2022 or 255-9500 to be directed to the Division of Social Services office closest to where you live. DSS staff members will help you find out more about eligibility for Medicaid and other assistance programs. Then the appropriate information and application forms will be mailed to you. Complete, sign and date the application form in ink and mail it to the address provided.
- For Long Term Care applications, please call the Long Term Care Medicaid Unit listed for the county where you live.
Don’t Miss: What Does Medicaid For Adults Cover
Choosing A Different Mycare Ohio Plan
If you end your membership in our plan by choosing a different MyCare Ohio plan:
- If you request to switch to a different MyCare Ohio plan before the last five days of a month, your membership will end on the last day of that same month. Your new coverage in the different MyCare Ohio plan will begin the first day of the next month. For example, if you make a request on January 18, your coverage in the new plan will begin February 1.
- If you request to switch to a different MyCare Ohio plan on one of the last five days of a month, your membership will end on the last day of the following month. Your new coverage in the different MyCare Ohio plan will begin the first day of the month after that. For example, if we get your request on January 30, your coverage in the new Plan will begin March 1.
How Do I Know If My Child Is Due For A Texas Health Steps Checkup
Texas Health Steps will send you a letter when it’s time for your child’s medical and dental checkups. You can also visit YourTexasBenefits.com or call the number below to find out if your child is due for a checkup.
Phone
Don’t Miss: How To Switch Medicaid Plans Ohio
Unemployment Insurance Claims In 2021
With the pandemic and general shutdown of the economy that took place in 2020 and 2021, tens of millions of Americans found themselves suddenly out of work. For many of them, this was the first time they needed to file for unemployment benefits, which are distributed by states to help the jobless.
The procedure for filing for unemployment varies by state, since each of the 53 unemployment systems in the United States and its territories has somewhat different rules. The process is generally time-consuming and difficult for first-time filers. For many people, a first-round rejection of claims forces an appeal that can last weeks or months. When an award is finally made, the funds can come as a welcome relief.
How To Stop Calworks Benefits
Under the CalWorks program, a low-income adult can receive cash assistance for up to 60 months. Children can receive benefits beyond the 60-month limit. If you no longer meet the eligibility requirements for CalWorks due to a change in your income or household circumstances, you can withdraw your request for benefits. Once you cancel your benefits, you will not be eligible to request a hearing. However, you can reapply for benefits at any time.
Compose a letter expressing your desire to stop receiving CalWorks benefits. On the letter, include your name. You can also include the names of other individuals in the home for whom you are receiving benefits.
Take or mail the letter to your local California Department of Social Services branch.
Complete the “CW 89 Application Withdrawal Request” provided by your caseworker. Completing this form is not a requirement. It is optional. On the form, you can state your reason for canceling your benefits. A copy of the CW 89 will be placed in your file.
You’ll receive a “CW 10 Notice of Withdrawn Application.” This notice will be mailed to you by your caseworker, confirming that your request to cancel benefits has been processed.
Also Check: Does Medicaid Pay For Hospice Room And Board
Supplemental Security Income Appeals
Supplemental Security Income is a federal cash assistance program. To be eligible for SSI, you must be disabled as defined by the Social Security Administration , and you also must meet the programâs income and asset guidelines. In most states, eligibility for SSI means automatic eligibility for Medicaid. Applications for SSI must be submitted to the SSA.
Q Who Qualifies For Medicaid
A. Citizenship and Residency – To obtain full Medicaid benefits in Delaware, you must be a Delaware resident and either a U.S. citizen or a legally residing noncitizen. Full coverage for noncitizens which include DACA recipients is dependent on the availability of state funding. However, noncitizens can qualify for coverage for emergencies and labor & delivery services if income requirements are met.
Income Level – Qualifying for Medicaid is also based on need. Household income must be under certain limits as defined by the Federal Poverty Level and is based on family size. For Long Term Care programs, financial resources must also be under a certain amount. There are also specific programs for individuals who meet certain medical or disability tests, or who qualify due to age or pregnancy. To find out more about different Medicaid and other medical assistance programs, visit DMMA Programs & Services.
Recommended Reading: How To Get Medicaid Certified
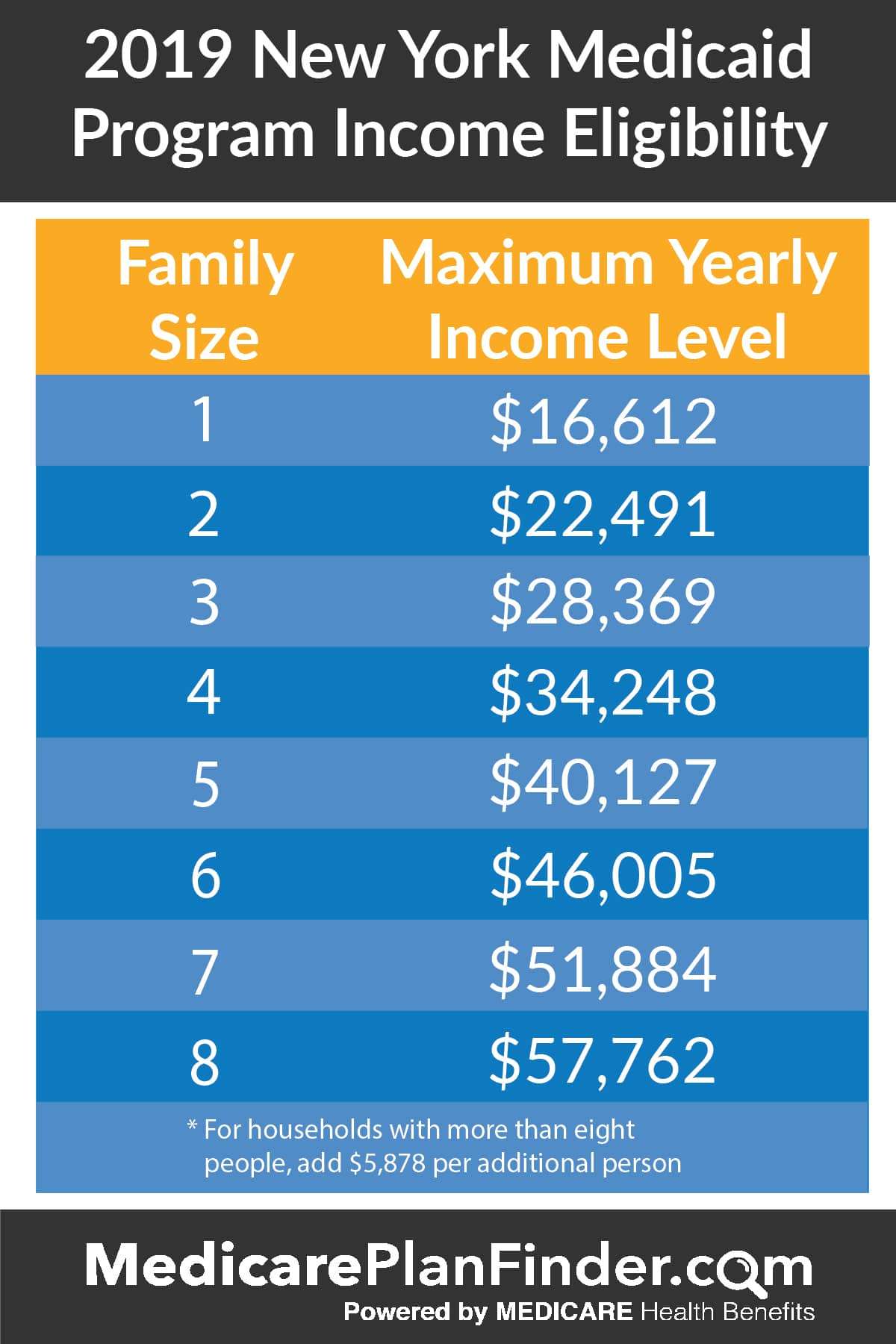
Q How Much Income Can I Receive And Still Be Eligible For Medicaid
A. Income is money that you get from working, or money that someone gives you, or checks that you receive, such as a Social Security check, unemployment benefits, child support, retirement benefits, or sick pay. Whether your income level qualifies you or your family for Medicaid depends on the size of your family and the Medicaid program for which you are applying.
Income limits are set each year by the federal government to define the Federal Poverty Level for different family sizes. In general, if your household income is at or below the current 100% Federal Poverty Level for your household size, your family is likely to be eligible for Medicaid. Children from age 1 to under age 6 can qualify for Medicaid benefits when household income is at or below 133% of the Federal Poverty Level. Pregnant women and infants under age 1 qualify for Medicaid with family income at or below the 200% Federal Poverty Level, and pregnant women count as 2 family members.
See our tables of income limits for applying for DMMA programs to find out where your family income is, in relation to these income benchmarks.
Medical assistance programs other than Medicaid have different income level requirements. For example, uninsured children under age 19 who live in families with incomes at or below the 200% Federal Poverty Level are eligible for low cost health insurance under the Delaware Healthy Children Program.
Q How Long Will My Medicaid Benefits Remain Active
A. Medicaid is based on month to month eligibility. However, your benefits are redetermined on a yearly basis by DMMA to confirm whether you still remain eligible for the program you are receiving. Certain Medicaid programs require you to report changes in your situation within 10 days of the change. One example of a change that must be reported is new employment.
You May Like: Is My Medicaid Still Active
When We Must End Your Membership
CareSource must end your membership in the plan if any of the following happen:
- If you do not stay eligible and enrolled in Medicare and Medicaid
- If you move out of our service area
We may not end your membership for any reason related to your health.
For a complete list of situations where we must end your membership in the plan, see your member handbook, chapter 10. You can find this document on the Plan Documents page.
Member Services: , 8 a.m. to 8 p.m., Monday Friday.
Virginias Requirements For Medicaid Qualification
Eligibility requirements for Medicaid have to be met before you can qualify for the program. To be eligible for Medicaid in Virginia, you have to belong to one of the designated patient groups. Without this qualification, you will not be eligible for the program. Those medical groups are:
- Children
- Parents or caretakers of relatives
- Adults between the ages of 21 and 64 who suffer from a mental illness
- Other adults who qualify
- Adults between the ages of 18 and 26 who are former foster children
You must also be a resident of Virginia who has a valid state ID. You will also need to provide your Social Security number and have documents proving that you are a US citizen. Aside from these things, if you are a former foster child, suffering from a disability or mental illness, you will need to provide documentation regarding these things.
Also Check: Psychiatrist In Nyc That Take Medicaid
