Types Of Medicaid Plans Including Dental
The type of Medicaid that you have could impact whether it pays for dental work for adults. Each state offers a variety of plans designed for different groups of low-income individuals.
In addition to the straight or regular program, you could enroll in unique plans for pregnant women, dual-eligible Medicare recipients, and individuals deemed medically needy.
Unitedhealthcare Dual Complete Plans
Plans are insured through UnitedHealthcare Insurance Company or one of its affiliated companies, a Medicare Advantage organization with a Medicare contract and a contract with the State Medicaid Program. Enrollment in the plan depends on the plans contract renewal with Medicare. This plan is available to anyone who has both Medical Assistance from the State and Medicare. This information is not a complete description of benefits. Call TTY 711 for more information. Limitations, co-payments, and restrictions may apply. Benefits, premiums and/or co-payments/co-insurance may change on January 1 of each year.
Medicaid And Former Foster Youth
For young adults formerly in foster care, there are special provisions. Medicaid is available until age 26 for those who:
- exit foster care at age 18
- were on Medicaid while in foster care
- are not eligible for other Medicaid coverage
No income is counted towards eligibility, and the young adult is eligible even if they have another offer of coverage through an employer. Children who were adopted or placed in guardianship at age 18 are not eligible for Medicaid under the former foster care coverage group.
Read Also: Medicaid And Medicare Supplement Insurance
Lenses Covered By Medicaid
If you need new glasses through Medicaid, it is important to be aware of which types of lenses are covered. Regular single vision lenses are covered by Medicaid, for near and distance vision correction.
If you need bifocals or trifocals, Medicaid will also usually cover the cost. It will generally cover the cost of one pair of bifocals or trifocals, or two pairs of single vision glasses.
Lenses that are not covered by Medicaid include:
- Oversized lenses.
- Progressive multifocals.
- Transition lenses.
If you would like to have any of the above lenses, you can still get them with your Medicaid coverage. You will just have to pay the difference in cost for such specialty lenses.
Additionally, contact lenses are not typically covered by Medicaid. If you want contacts, you will probably have to pay for them out of pocket or with a different supplemental insurance plan. In some cases, contact lenses are covered, but only when they are deemed to be medically necessary.
Does Medicare Cover Gym Membership
For older adults who have Medicare instead of or in addition to Medicaid, gym membership may be available through that plan. Although Original Medicare doesnt cover fitness center membership, some Medicare Advantage plans may offer gym membership as part of their plan benefits.
Medicare Advantage, also known as Part C, is provided by private health insurance companies that cover all the benefits offered by Original Medicare and can offer extra benefits to clients. Many include gym membership as part of these extras.
Medicare Advantage plans generally reimburse memberships up to a certain amount of money. This may cover the full amount of a membership, or there may be a gap. Some companies only cover a certain percentage of the costs, so make sure to check your plan carefully. Plans marketed to members of senior organizations, such as Medicare Advantage plans offered by AARP, often include these types of incentives to encourage seniors to stay active.
Recommended Reading: Medicaid Provider Id Number Lookup
Texas Medicaid Wellness Program
The Texas Medicaid Wellness Program is a special health program for people who get Medicaid and have long-lasting or serious health conditions. These conditions can include asthma, diabetes, congestive heart failure, coronary artery disease, chronic obstructive pulmonary disease , and others.
People in this program can get help any time of day or night with:
- Getting an answer to a health question.
- Finding a main doctor.
- Managing their health between doctor visits.
- Learning more about their health conditions.
- Knowing how to take their medicines.
- Picking the best medical care for their health.
Learn more about the Wellness Program.
Children’s Health Insurance Program Health Plans
Children in CHIP get services through a medical plan in their area. Some CHIP plans also offer services to mothers who are pregnant. This is called CHIP perinatal coverage.
You can find the CHIP health plans in your area by using the Find Your Medical Plan search tool. You can see how well some CHIP health plans perform by looking at the CHIP health plan report cards.
To learn more about CHIP, visit the CHIP and Children’s Medicaid website.
Recommended Reading: Pediatricians In Austin Tx That Accept Medicaid
Are There Different Vaccines For Medicaid
No. Medicaid vaccines are the same as youd receive through any other program or form of insurance. And Medicaid-covered vaccines are always administered by qualified professionals such as pharmacists and healthcare workers. This also applies to COVID-19 vaccines. At the height of the pandemic, some mass vaccination sites also brought in active-duty troops from the National Guard to give shots, and they were also qualified to do so.
Does Medicaid Cover Glasses In Louisiana
All Medicaid recipients. Examinations and treatment of eye conditions, including examinations for vision correction, refraction error. Regular eyeglasses when they meet a certain minimum strength requirement. If the recipient has both Medicare and Medicaid, some vision related services may be covered.
Don’t Miss: How Do You Know If You Still Have Medicaid
Medicaid Offers Additional Mental Health Support
Medicaid is the single largest payer for mental health services in the United States. While they didnt always include therapy as a benefit and limitations do still exist, Medicaid now covers this and a myriad of other substance use, mental health, and behavioral health services.
If youre enrolled in a Medicaid plan, some of your covered services may include:
- Psychological testing and evaluation
- Social work services
- Case management for chronic mental illness
Other services like tobacco use cessation, mental health skill-building, and peer support should also be covered. If youre experiencing mental health concerns or battling a substance use disorder, its important to seek professional care and get the diagnosis and treatment you need.
If you or a loved one are struggling with substance use or addiction, contact the Substance Abuse and Mental Health Services Administration National Helpline at 1-800-662-4357 for information on support and treatment facilities in your area.
For more mental health resources, see our National Helpline Database.
Who Qualifies For Medicaid
Medicaid is a federal entitlement program that offers guaranteed coverage to all qualifying residents. Certain individuals, including low-income families, pregnant women and adults who are blind or disabled, are included in mandatory eligibility groups. States may also offer optional coverage to individuals who are categorically needy. This includes seniors who receive home- and community-based services, are on hospice, live in a nursing home or are in poor health. Because each state operates its own Medicaid program within the federal framework, income limits and medical eligibility requirements vary by state.
Financial Eligibility for Medicaid
At least 42 states have adopted the optional Special Income Level standard for Institutional Medicaid. Under the special income rule, individuals who are expected to need nursing home care for at least 30 days can earn up to 300% of the Supplemental Security Income Federal Benefit Rate. For 2021, the limit is $2,382 per month, and it typically doubles for couples applying jointly.
A handful of states, including Tennessee, Washington and Wyoming, set the income limit as low as $794, which is 100% of the FBR. Other states, such as California, Hawaii and Kansas, require seniors to use all or nearly all of their income for institutional long-term care before Medicaid kicks in. Fortunately, there are other ways for individuals who have substantial medical needs to qualify for Medicaid.
Asset Limits and Exemptions
- Investments
You May Like: Dermatologist In Lake Charles That Accept Medicaid
Q If I Have Private Health Insurance Can I Be Eligible For Medicaid
A. It depends. If your income is low, and you have minor children, you and your children can have private health insurance and still be eligible for Medicaid. Certain Medicaid qualifying programs require that you not have any other health insurance in order for you to get Medicaid. If you have both private health insurance and Medicaid, you should show both your Medicaid card and your private health insurance card to your medical provider each time you receive services.
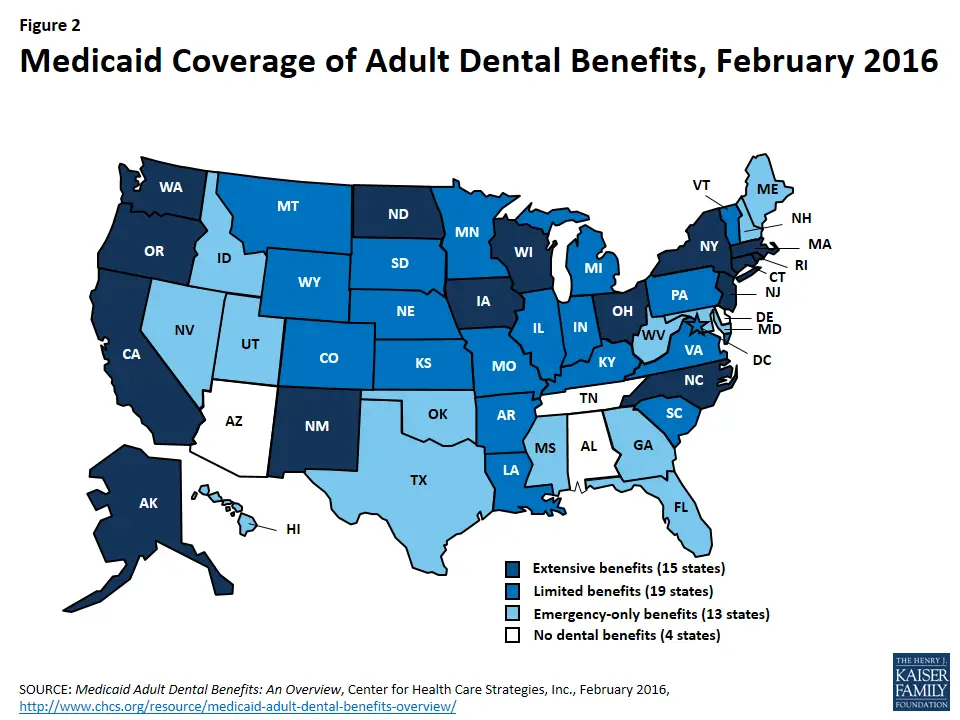
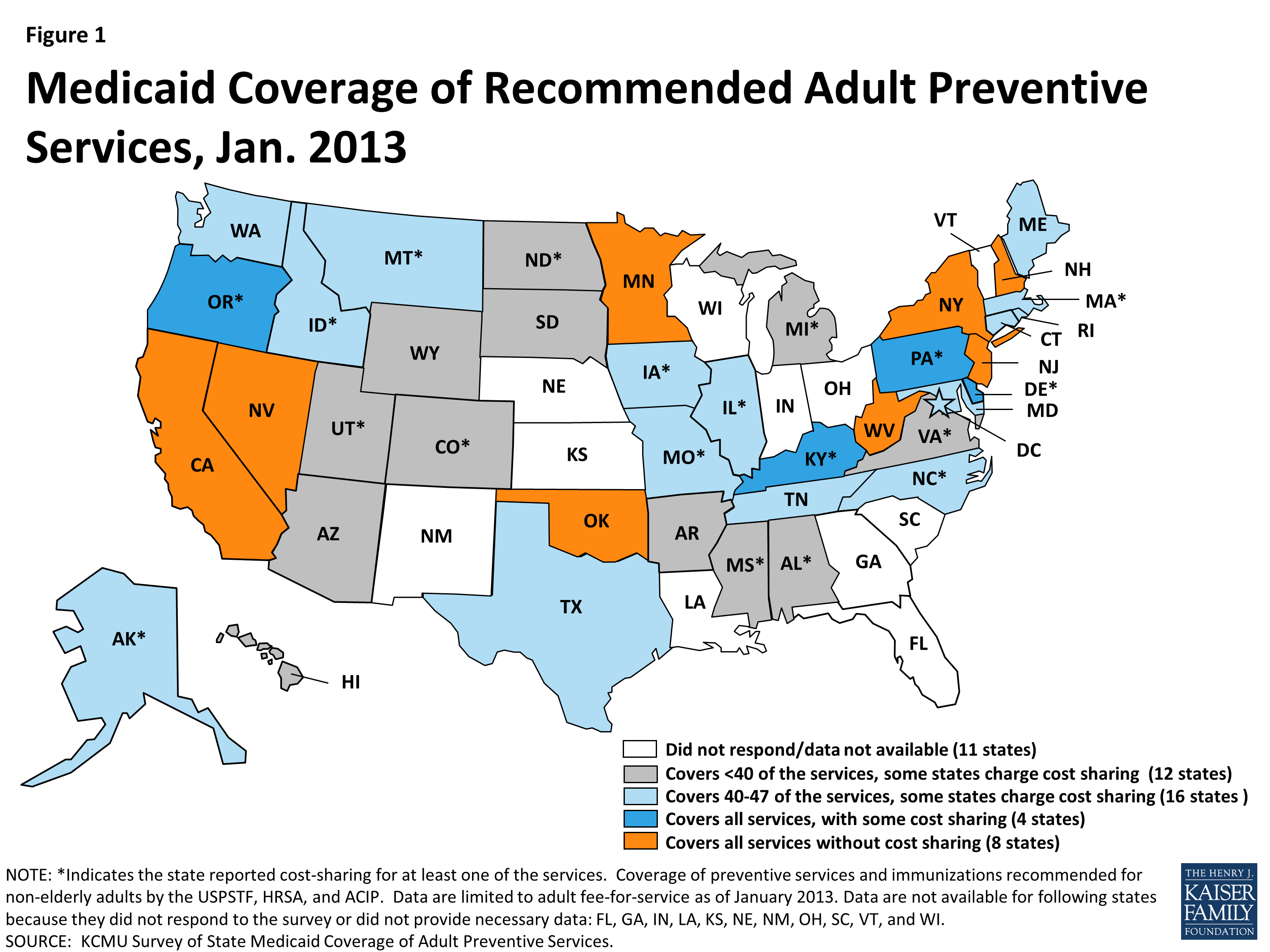
How Much Regional Difference Is There Between States As To Whether Medicaid Covers Adult Vaccines
It varies, but most states cover at least one of the recommended adult vaccines. Some only cover flu vaccines for adults.
Coverage varies widely depending where you live. Among the majority of states that offer at least some coverage, it can range from coverage for both kids and adults to an age limit that caps out at 19 or 20 years old.
So, in some areas, older Americans looking for a shingles vaccine might find it difficult to get coverage. That can be problematic given that Shingrix, the CDC-recommended shingles vaccine, costs about $200 a dose out of pocket and requires two doses. Its now also approved for use in immunocompromised adults.
Recommended Reading: What Does It Take To Get Medicaid
Which Eyewear Providers Accept Medicaid Cover
The first step to finding a physician or eyewear provider who accepts Medicaid is to look at your Medicaid insurance card. On the card, youll find the contacts and web address of the agency that manages your Medicaid plan.
Visit the agencys webpage to find the online directory of physicians and eyewear providers that accept Medicaid insurance plans. When you enter your location and the name of your plan, the website will generate a list of eyewear providers near you who accept Medicaid.
You can also use the Medicaid Benefits database provided by KFF .
This database can help you understand the eye services covered by your Medicaid plan and the limitations to these services that exist in the state you live in. However, specific Medicaid plan details should still be confirmed by the agency that manages your Medicaid plan.
Most Medicaid Enrollees Get Care Through Private Managed Care Plans
Over two-thirds of Medicaid beneficiaries are enrolled in private managed care plans that contract with states to provide comprehensive services, and others receive their care in the fee-for-service system . Managed care plans are responsible for ensuring access to Medicaid services through their networks of providers and are at financial risk for their costs. In the past, states limited managed care to children and families, but they are increasingly expanding managed care to individuals with complex needs. Close to half the states now cover long-term services and supports through risk-based managed care arrangements. Most states are engaged in a variety of delivery system and payment reforms to control costs and improve quality including implementation of patient-centered medical homes, better integration of physical and behavioral health care, and development of value-based purchasing approaches that tie Medicaid provider payments to health outcomes and other performance metrics. Community health centers are a key source of primary care, and safety-net hospitals, including public hospitals and academic medical centers, provide a lot of emergency and inpatient hospital care for Medicaid enrollees.
Figure 6: Over two-thirds of all Medicaid beneficiaries receive their care in comprehensive risk-based MCOs.
Don’t Miss: How To Get Medicaid In Colorado
When Medicaid Covers Braces For Adults
When does Medicaid cover braces for adults over age 21? This publically-funded program has a dual nature leading to two different answers because coverage varies by state especially for orthodontia.
- Finding a local orthodontist that accepts Medicaid often proves challenging due to the low reimbursement rates and the complex web of rules
- Free braces programs for adults might prove a more viable option if you live in a region that does not support orthodontia
- Expect benefits only for the least costly treatment alternative for any oral care problem
| 1 |
Does Medicaid Cover Dental In Ky
The Kentucky Medicaid DentalMedicaidMedicaid does coverdental
Will medicaid pay for dentures in ky?
Coverage for Dental Services in Kentucky In Kentucky, qualifying adults over the age of 21 may only be eligible to receive routine or emergency dental services through Medicaid. Dentures do not typically qualify under routine or emergency oral care.
does Medicaid cover immediate dentures?MedicaiddenturesdenturesMedicaid doesdentures
Contents
Don’t Miss: Does Sc Medicaid Cover Weight Loss Surgery
Medicaid Facilitates Access To Care
A large body of research shows that Medicaid beneficiaries have far better access to care than the uninsured and are less likely to postpone or go without needed care due to cost. Moreover, rates of access to care and satisfaction with care among Medicaid enrollees are comparable to rates for people with private insurance . Medicaid coverage of low-income pregnant women and children has contributed to dramatic in the U.S. A growing body of research indicates that Medicaid eligibility during childhood is associated with reduced teen mortality, improved long-run educational attainment, reduced disability, and lower rates of hospitalization and emergency department visits in later life. Benefits also include second-order fiscal effects such as increased tax collections due to higher earnings in adulthood. Research findings show that state Medicaid expansions to adults are associated with increased access to care, improved self-reported health, and reduced mortality among adults.
Figure 7: Nationally, Medicaid is comparable to private insurance for access to care the uninsured fare far less well.
Medicaid Is The Nations Public Health Insurance Program For People With Low Income
Medicaid is the nations public health insurance program for people with low income. The Medicaid program covers 1 in 5 Americans, including many with complex and costly needs for care. The program is the principal source of long-term care coverage for Americans. The vast majority of Medicaid enrollees lack access to other affordable health insurance. Medicaid covers a broad array of health services and limits enrollee out-of-pocket costs. Medicaid finances nearly a fifth of all personal health care spending in the U.S., providing significant financing for hospitals, community health centers, physicians, nursing homes, and jobs in the health care sector. Title XIX of the Social Security Act and a large body of federal regulations govern the program, defining federal Medicaid requirements and state options and authorities. The Centers for Medicare and Medicaid Services within the Department of Health and Human Services is responsible for implementing Medicaid .
Figure 1: Medicaid plays a central role in our health care system.
You May Like: Anthem Blue Cross Medicaid Nevada
Does Florida Medicaid Cover Permanent Dentures
The Medicaid program often covers preventive dental care for adults. Regular oral exams, cleanings, and X-rays are some of the preventive services available. In these four states, preventive care is combined with emergency services, but there is no additional restorative or major treatment except in Florida, where dentures are covered.
Who Does Medicaid Provide Vision Coverage For
Federal law requires that vision care be provided through Medicaid to children and adults under the age of 21. Regular well visits that include vision screenings help to reduce the occurrence of eye conditions later in life. The idea is that prevention is the best way to keep costs down overall.
There are no federal regulations, however, that require Medicaid to provide vision care for adults over the age of 21. Standard vision coverage options are offered by each state, though the specific services can vary greatly. Its important to confirm the specifics of coverage with your state.
Optometry services and eyeglasses are optional benefits under Medicaid. Optional medical services may come with a small copay for the individual. Again, the amount will vary by state.
In order to qualify for Medicaid coverage, you must meet certain requirements. You can qualify for Medicaid based on the following factors:
- Income
- State residency
If you have questions regarding your eligibility status, you can contact Medicaid directly.
As of October 2019, over 71 million people were enrolled in Medicaid across the country. Over 35 million of those individuals were children enrolled in Medicaids Childrens Health Insurance Program .
Medicaid provides affordable and essential health care services to individuals and families who may otherwise not be able to afford it.
Recommended Reading: Medicaid Requirements For Gastric Sleeve
Does Medicaid Cover Diapers
When it’s deemed medically necessary, Medicaid does cover the cost of diapers for adults. For adults and seniors, these needs generally fall under Home and Community-Based Services waivers, which provide additional services and supplies for older adults and those living with disabilities.
A doctor’s prescription is typically required to receive coverage for diapers. This prescription will determine how many diapers the beneficiary is eligible for each month.
When it comes to diapers for young children, Medicaid will typically provide a diaper allowance for children under age four, provided they’re medically necessary.
Does Medicaid Cover Glasses Overview
Federal laws do not require state Medicaid programs to pay for glasses. As a result, most states provide eyewear as an optional benefit. However, there are many instances whereby Medicaid programs pay for the cost of new glasses.
For instance, Medicaid pays for glasses for kids and young adults. Medicaid will also cover glasses for adults of any age if they are considered to be medically necessary by a physician.
Note that if you qualify for new glasses under Medicaid, you will be limited to the types of lenses you can pick.
For instance, Medicaid will pay for standard single vision lenses, but you will incur out-of-pocket costs if you decide to go for premium lenses.
To find out which eye clinics accept Medicaid as payment for new glasses, you should contact your local Medicaid office.
Most agencies offer online directories to help you find eyewear providers near you that accept Medicaid.
Read Also: How Does Someone Get Medicaid
