Application And Eligibility Procedures
Application Request
Effective immediately, when a women makes an application for Uninsured Womens Health Services, register the application in FAMIS on the Application Request screen. Enter MA in the Program Code field, and WHS in the Sub Program Class field.
On the Application Detail screen, enter the appropriate Benefit Requested code for each listed individual. DO NOT exclude a spouse, if in the home, or the father of any dependent child that is included.
Explore eligibility for UWHS anytime an application for Family Healthcare is received requesting coverage for an age-eligible woman by registering both a FAM and WHS application.
If an Internet application is received for a woman requesting coverage and the woman is not currently receiving benefits but is included on an active Family Healthcare case in FAMIS, explore eligibility for all MO HealthNet programs including UWHS. The application will not be able to be sent to FAMIS as the participant has an active case in FAMIS. The eligibility specialist must print and review the Application Summary that displays on the Document Queue screen in FAMIS. The applicant may wish to add-a-person and/or apply for MO HealthNet for Pregnant Women or Uninsured Womens Health Services program. If an application is needed, register the appropriate requested application in FAMIS.
The MO HealthNet Application for Kids, Pregnant Women and Parents form is the application form used to apply for UWHS.
Control Flow
Coding
No Access To Employer
In addition to being uninsured, the woman cannot have access to employer-sponsored health insurance . Access to insurance available through employment includes group memberships or private company insurance enrollment options offered by the employer. Examples of group memberships that could offer health insurance are a union, professional organization, or trade association.
If the woman or her spouse fails to purchase the health insurance, she is ineligible as long as it is available. It is considered available even though there is a limited open enrollment period for which they need to wait. Affordability limits do not apply to this program.
Can I Get A Ride To My Appointments
If you have an appointment with your healthcare provider and you need a ride, you may be able to get one through Non-Emergency Medical Transportation. To see if you can get a ride, you will need to contact your Managed Care health plan. If you do not have a Managed Care health plan, please call . You will need to call at least 3 days before your appointment to arrange a ride .
Read Also: Dentist Who Accept Medicaid For Braces
Medicare Costing Savings Programs
The purpose of Medicare Costing Savings programs is to assist individuals by paying their Medicare premiums and by making payments to medical providers for coinsurance and deductibles for Medicare services.
The Qualified Medicare Beneficiary program pays for Medicare Part B premiums, coinsurance, and deductibles for those eligible and enrolled in Medicare Part A.
The Specified Low Medicare Beneficiary program provides payment of Medicare Part B premiums only for individuals who would be eligible for the QMB program except for excess income.
The Qualified Individual program provides payment of Medicare Part B premiums only for individuals who would be eligible for the SLMB program except for excess income.
The Qualified Disabled Working Individual program provides payment of Medicare Part A premiums only for individuals meeting income limits.
Medicaid Eligibility In Missouri
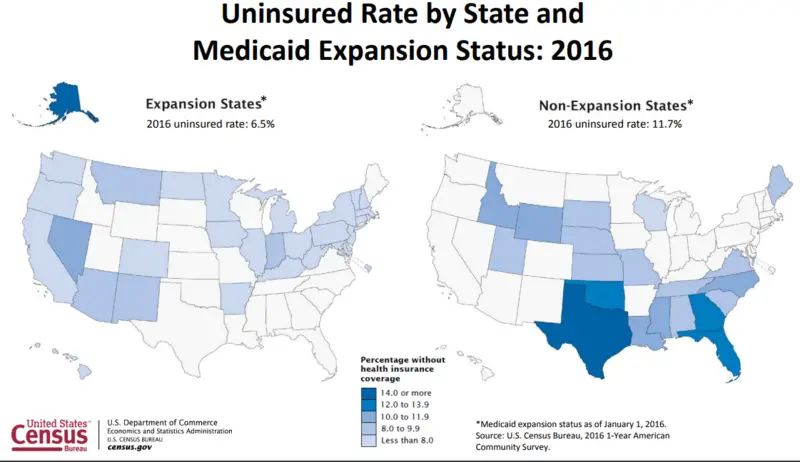
Medicaid is a federal- and state-funded health insurance program that works for low-income individuals, families, and seniors who otherwise wouldnt be able to afford health care coverage. Missouris Medicaid program, which is known as MO HealthNet, runs through the Missouri Department of Social Services.
Recommended Reading: If You Are On Disability Are You Eligible For Medicaid
Missouri Now Uses A Single Application Form To Apply For Medicaid
There are three broad groups which applicants would fall under which determine how best to apply.
Missouri Medicaid Expansion is effective beginning 07/01/2021.
Helpful links for DMH Agencies and Providers:
- The IM-6AR Appointing an Authorized Representative form should be used if the application has already been submitted and the “Appendix C” was not included with the application.
Disabled Application Flow Chart Please review this flow chart if you will be assisting a DMH consumer with the application process.
Uninsured Womens Health Services Program
This program provides MO HealthNet coverage for womens health services to uninsured women ages 18 up to but not including age 55 whose net family income does not exceed 185% of the federal poverty level for their household size. Womens health services are:
- Approved methods of contraception
- Sexually transmitted disease testing and treatment, including pap tests and pelvic exams
- Family planning, counseling, education on various methods of birth control and
- Drugs, supplies, or devices related to the womens health services described above, when they are prescribed by a physician or advanced practice nurse.
You May Like: What Age To Apply For Medicaid
How Much Does Medicaid Cost In Missouri
Most Medicaid plans in Missouri are free. However, some plans such as the plans for seniors and disabled people provide health coverage to people who dont meet the minimum income requirements once their spend down limit for the month is met. Also, the premium SCHIP plans for children have a monthly premium, which is determined based on your familys monthly income.
0 Exploring Uwhs Eligibility For Age Eligible Women When No Longer Eligible For Any Other Mo Healthnet Program
When closing an age-eligible woman in any MHF/MHK/MHABD program, include reviewing eligibility for UWHS in the exparte process if the participant is no longer eligible for any other MO HealthNet program. When a participant is determined ineligible for any Mo HealthNet Program in FAMIS and the participant is female and between the ages of 18-55, FAMIS will automatically register an Uninsured Women’s Health Services application. FAMIS does not register a UWHS application if the Mo HealthNet program that is being closed is in the Legacy system.
NOTE: A woman eligible for EWHS after the 60-day postpartum eligibility for MO HealthNet for Pregnant Women ends is to remain on EWHS as long as she remains eligible. FAMIS explores eligibility for UWHS prior to EWHS ending by registering a UWHS application in the participant’s eleventh month of EWHS coverage. If all information needed to determine eligibility for UWHS is in FAMIS, FAMIS approves or rejects the participant for UWHS and sends the participant an Action notice informing them of the decision on the UWHS application. If additional information is needed to determine eligibility for UWHS the eligibility specialist must complete an eligibility determination and FAMIS sends a Request for Information notice overnight requesting any additional information needed to determine eligibility.
Don’t Miss: Who Can Enroll In Medicaid
How Do You Know If Something Is Wrong With Your Reproductive System
Symptoms of reproductive health problems include bleeding or spotting between periods itching, burning, or irritation genital area pain or discomfort during sex heavy or painful menstrual bleeding severe pelvic/abdominal pain unusual vaginal discharge feeling of fullness in the lower abdomen and frequent.
What Are The Eligibility Requirements For Medicaid In Missouri
The MO HealthNet program covers individuals who meet certain income and resource criteria including:
â Low-income families
â The elderly
â Blind/visually impaired individuals
â Disabled individuals
â Pregnant women
â Newborns and infants
â Uninsured women under the age of 65
The income criteria for eligibility is determined by poverty guidelines set forth by the federal government. Resource criteria typically apply only to the elderly, disabled, and blind individuals. For these applicants, resources such as savings and countable assets can impact eligibility for the program.
Blind and disabled individuals can qualify for Medicaid due to a âphysical or mental impairment, disease, or lossâ that prevents them from working at a job within their skill level for 1 year or longer. Anyone who qualifies for assistance through the federal Supplemental Security Income program is automatically considered eligible for the MO HealthNet program on the basis of disability.
You May Like: Does Medicaid Pay For Lasik Surgery
What Is The Income Limit For Missouri Medicaid
Individuals who qualify for the federal Supplemental Security Income program who are disabled according to the SSI guidelines are eligible for Missouri Medicaid as long as their income doesnât exceed certain levels. For disabled individuals, income should not exceed 85% of the Federal Poverty Level . For blind individuals, income should not exceed 100% of FPL. Some disabled individuals may also qualify to receive MO HealthNet financial assistance to pay for Medicare premiums, deductibles, and copayments.
The elderly can sometimes spend down their incomes or medical expenses in order to meet the Medicaid income requirements in Missouri. âSpending downâ is a term that refers to the amount of medical expenses that a person must pay monthly in order to become eligible for Medicaid coverage. An individual or couple may need to spend down their income so that their net income is equal to or lower than the income eligibility requirement for the Missouri Medicaid program.
âSpending downâ to meet income eligibility requirements may include either of the following:
â Monthly submission of medical expenses to a caseworker
â Monthly payments of the spend down amount to the MO HealthNet Division
MO HealthNet may also provide assistance to some seniors to pay their Medicare premiums, deductibles, and copayments.
More Than 17000 People Had Applied For Expanded Medicaid By Early October Enrollments Being Processed As Of October And Coverage Can Be Backdated To July 1 2021
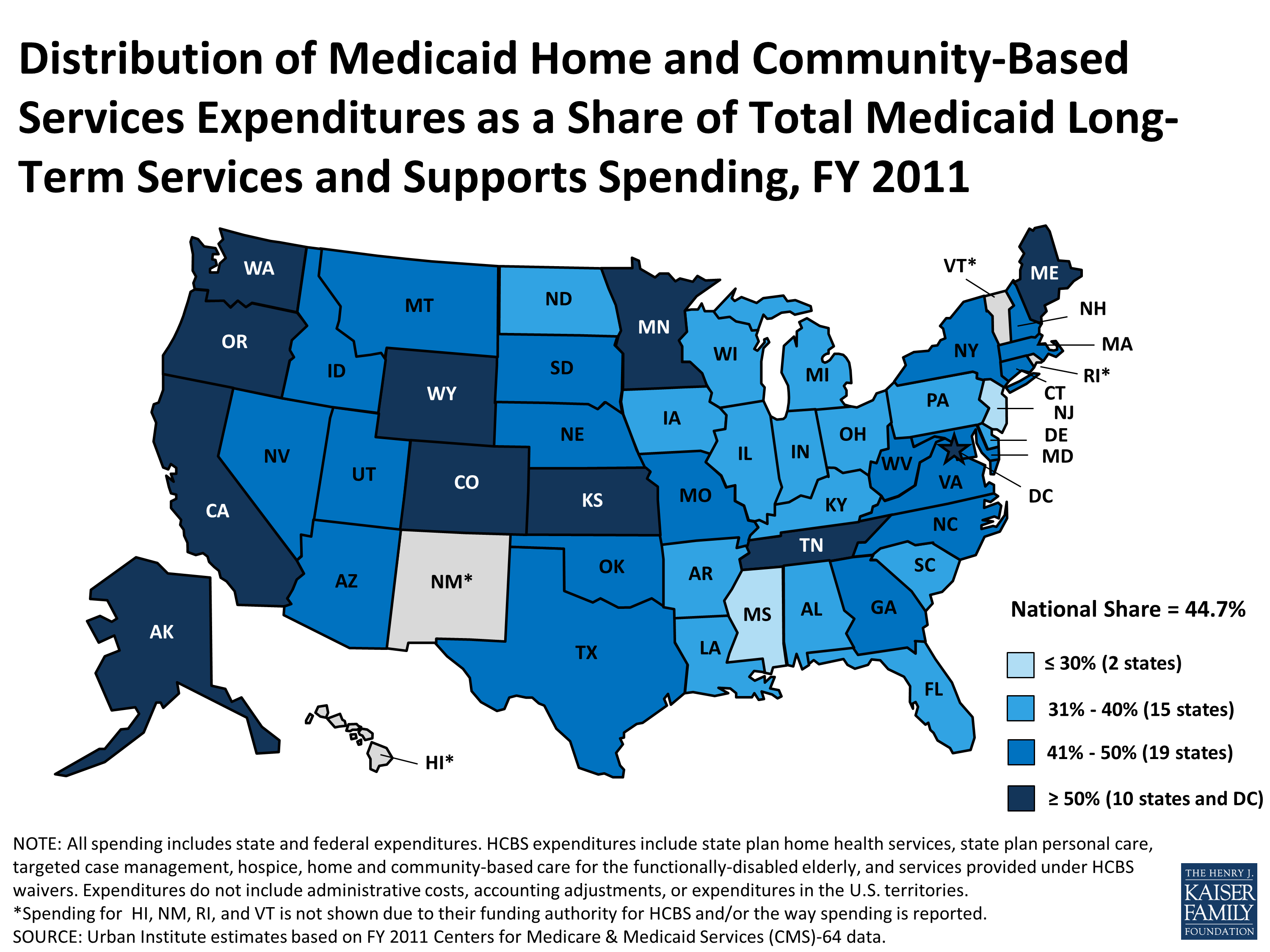
As described below, Missouri had a long and somewhat complicated road to Medicaid expansion. But as of October 2021, Medicaid expansion in the state was fully in effect, and more than 17,000 people had already applied for coverage.
Applications are being accepted for adults under age 65 with household incomes up to 138% of the poverty level. In 2021, that amounts to about $17,774 for a single individual, and $36,570 for a household of four . This is eventually expected to result in 275,000 Missouri residents becoming eligible for MO HealthNet.
The state has clarified that applications submitted by November 1, 2021 can have coverage backdated to July 1, 2021, which is when Medicaid expansion would have taken effect if lawmakers hadnt blocked funding during the spring 2021 legislative session.
The federal government is paying 90% of the cost of Medicaid expansion in Missouri, just as they do in other states that have expanded Medicaid. But since Missouris expanded eligibility rules took effect after the American Rescue Plan was enacted, the state is also receiving an increase of 5 percentage points added to its regular federal matching rate for the traditional Medicaid population, for the next two years .
You May Like: How Do I Get Medicaid
What Is Missouri Medicaid
In Missouri, Medicaid is known as MO HealthNet. The program provides its beneficiaries with an identification card, known as a MO HealthNet Identification Card, which enables them to receive some health care services free of charge. MO HealthNet strives to help aged, blind and disabled persons access quality care, and it also provides coverage for pregnant women, families, uninsured women, women with breast or cervical cancer and children.
Older adults who are enrolled in Medicaid may also be eligible for Missouri Care Options, a Medicaid-funded program that provides home and community-based services for aged, blind and disabled adults.
How To Apply For Medicaid In Missouri
Apply for Medicaid online by visiting the Missouri Department of Social Services’ website or apply in person at your nearest Department of Social Services office. While you cant apply for Medicaid over the phone, you can call the Missouri Department of Social Services at 1-573-751-3221 to check the status of your application.
You May Like: What Home Health Services Are Covered By Medicaid
How Long Will I Get Healthcare Coverage
You can get healthcare coverage through MO HealthNet as long as you are eligible. You will be required to complete an annual review each year you get MO HealthNet to make sure you are still eligible. You should get this form towards the end of your MO HealthNet coverage period. If you do not return your information by the deadline on the form, you may lose your coverage.
NOTE: It is important that you report any changes to your contact information, including your address, so you will get these important letters in the mail. If you do not respond to mail from the FSD, you could lose your benefit.
Missouri Expands Health Services For Uninsured Women
The Centers for Medicare and Medicaid Services has approved the Missouri Department of Social Services’ request to expand women’s health services to uninsured women ages 18-55 with income up to 185 percent of the federal poverty level.
“We are pleased and excited that CMS has given the stamp of approval to expand this program,” said Ian McCaslin, MD, director of the MO HealthNet Division. “MO HealthNet is committed to improving the health status of Missouri’s low income women. That effort begins with improved access to basic preventive services.”
Until now, the women’s health program was only available to uninsured MO HealthNet women for 12 months following the birth of a child.
“Improving access to high quality, affordable healthcare has been a priority for my administration over the last four years,” said Missouri Gov. Matt Blunt. “The approval of our request will help improve the health status of tens of thousands of women in Missouri by providing them with greater access to physical examinations and screenings.”
Blunt said the expanded services would improve access to medical evaluation for women seeking women’s health services. They are patterned after successful public health interventions nationally and focus on engaging patients in increased awareness of underlying health conditions and risk factors.
Also Check: How Do I Renew My Ohio Medicaid Benefits Online
0 Uninsured Women’s Health Services Program
The UWHS program provides women’s health services for uninsured women:
- from age 18 up to but not including age 56
- who are in need of family planning services,
- and have family income up to and including 201% of the federal poverty level for their household size.
NOTE: Women who have been sterilized are not in need of family planning services and are ineligible for the UWHS program.
UWHS coverage is not time limited and is subject to the standard MO HealthNet review and ex-parte processes. The only healthcare services covered by MO HealthNet for UWHS are family planning and family planning related services.
Missouri Is The Sixth State To Expand Medicaid Via Ballot Measure
In the last few years, voters in Maine, Idaho, Nebraska, Utah, and Oklahoma have approved similar ballot measures to expand Medicaid. Missouri will be the sixth state to expand Medicaid in this manner.
Its also worth noting that while voters in Utah, Idaho, and Nebraska all approved Medicaid expansion ballot initiatives in 2018, all three states subsequently sought federal approval for Medicaid work requirements , and have imposed various other restrictions and requirements, as opposed to simply expanding Medicaid as called for in their voter-approved ballot initiatives.
But the amendment that voters passed in Missouri prohibits the state from imposing additional eligibility requirements on the expansion population that arent imposed on the rest of the states Medicaid-eligible population. The Biden administration has also notified states that work requirements will no longer be approved, so that would be a non-starter at this point.
Read Also: Which Medicaid Health Plan Is The Best In Illinois
Ineligible For Any Other Mo Healthnet Program
A woman is ineligible for UWHS if she qualifies for any other MO HealthNet program. Explore eligibility for any Family Healthcare program prior to exploring eligibility for UWHS. If the participant has an active MO HealthNet for Families or MO HealthNet for Kids case, explore eligibility for MO HealthNet for Families prior to exploring eligibility for UWHS by completing an add-a-person application.
If ineligible for MO HealthNet for Families or any other full coverage program, explore eligibility for UWHS by registering a UWHS application and approve for UWHS if eligible on all UWHS eligibility factors. If the woman applies using the IM-SSL application, she is ineligible for MO HealthNet for the Aged, Blind, and Disabled unless she either indicates that she is disabled or receives Social Security disability or SSI benefits.
EXAMPLE: Ms. Johnson meets all eligibility requirements for UWHS, but is receiving Extended Women’s Health Services . Ms. Johnson is not eligible for UWHS as she is currently receiving MO HealthNet benefits under another program.
NOTE: Ms. Johnson should be reviewed for UWHS eligibility prior to closing EWHS.
How To Sign Up For Medicaid
Missouri residents can sign up for Medicaid either online, by phone, through the mail, or in person at a designated Medicaid office. The online application is one of the more popular options for applicants to use, but all three of these application processes are available. Applicants should make sure that they qualify and have the required documents available before starting their Medicaid application.
No matter how you apply for Medicaid, you will need to submit the following documents and information along with your Medicaid application form:
â Proof of United States citizenship
â Proof of Missouri residency
â Income statements
â Social security number
â Current living address
â Phone number
â The number of people in your household
For people who are applying for Medicaid not only for themselves, but also on behalf of their family, they will need to submit the above information for every family member that they are applying for. A separate Medicaid application may need to be completed for each family member as well. If you have questions about applying for yourself and your family members, contact a Medicaid office close to you and ask to speak with an Authorized Representative.
Don’t Miss: Can Medicaid Be Transferred To Another State
