Supportive Services Through The Older Americans Act
The Older Americans Act provides federal funding for a range of home- and community-based services throughout the country. Although they are not intended to provide funds to seniors directly, these services and resources can be a welcome time and cost savings to supplement the expense of providing in-home care. The OAA established a nationwide network of Area Agencies on Aging public or private non-profit agencies designated to address the needs and concerns of all older persons at regional and local levels. Contact your local Area Agency on Aging for a list of supportive senior services offered in your community.
How To Qualify In Florida
To qualify, one must meet the following criteria:
- If you are under the care of an attending physician and have a physicians order for home health services
- If a medical condition or disability that substantially limits your ability to perform everyday living activities
- Require services that can be safely, effectively, and efficiently provided in the home or other authorized setting
- If you are certified homebound by your doctor/nurse
Is Medicaid Home Health Care Available In My State
- Medicaid beneficiaries can get home health care services if they are ill, injured, disabled or meet other qualifications. Learn about your state’s rules.
Medicaid is a U.S. government program that provides healthcare coverage to children and adults who meet eligibility requirements. Both the federal government and individual states fund the program together. The federal government requires that states offer Medicaid coverage to certain mandatory groups:
- Low-income families
- Supplemental Security Income beneficiaries
- Certain individuals with disabilities
- Other groups
States may add beneficiary classes to these eligible groups. Individual states also determine which services are covered and how beneficiaries can access healthcare services. Because of this setup, medical programs vary significantly from one state to another. That includes coverage for Medicaid home health care services.
Don’t Miss: Assisted Living Facilities In Arkansas That Accept Medicaid
Who Is Eligible For A Health Home
Health Homes are for people with Medicaid who:
- Have two or more chronic conditions
- Have one chronic condition and are at risk for a second
- Have one serious and persistent mental health condition
Chronic conditions listed in the statute include mental health, substance abuse, asthma, diabetes, heart disease, and being overweight. Additional chronic conditions, such as HIV/AIDS, may be considered by CMS for approval.
- States can target health home services geographically
- States cannot exclude people with both Medicaid and Medicare from health home services
When Does Medicare Not Cover In

In most cases, Medicare doesnt cover these types of in-home health care.
- Home health aides, when the only care you need is custodial. That means you need help bathing, dressing, and/or using the bathroom.
- In-home meals
- Round-the-clock care
- Homemaker services, like cleaning, laundry, and shopping. If these services arent in your care plan, and theyre the only care you need, theyre generally not covered.
Its important to know that just because your doctor might recommend home health care, Medicare doesnt automatically cover it. It depends on your situation.
Also Check: Can You Have Va Benefits And Medicaid
Who Is Eligible To Receive Home Health Services
In order to receive home health services, consumers must be eligible for Medicaid with some requirements:
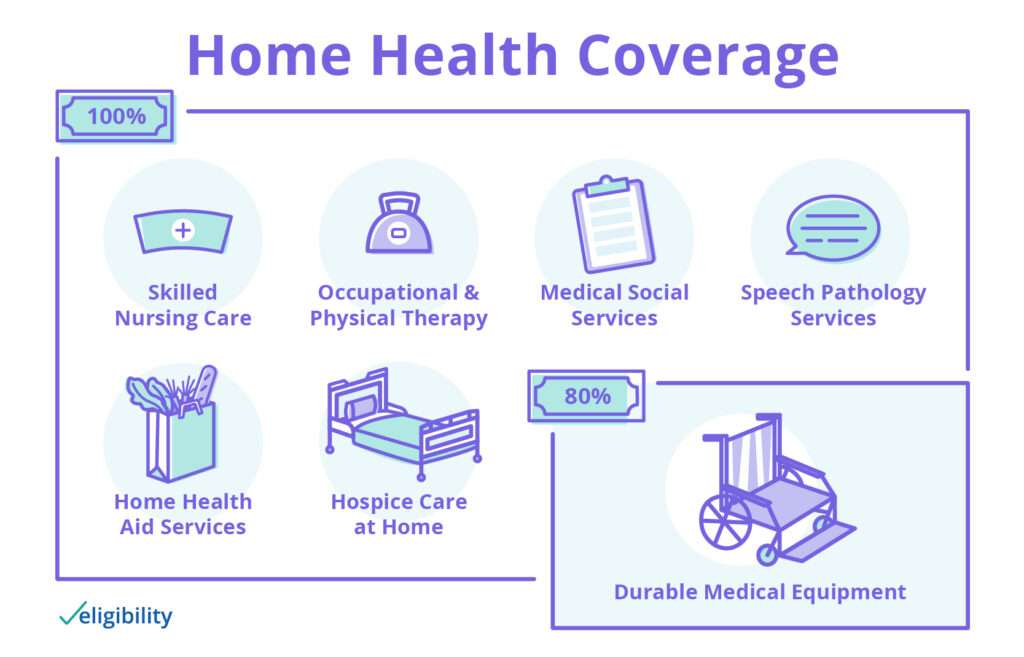
Home Health Coverage Eligibility
All people with Part A and/or Part B who meet all of these conditions are covered:
- Your doctor must consistently update your medical needs. Because covered services must be considered medically necessary, your needs must be current and checked up on to see if your needs have increased, decreased, or stayed the same.
- A doctor must certify that you need one or more of these:
- Intermittent skilled nursing care
- occupational therapy services, speech-language pathology, physical therapy
So, the takeaway for coverage for home health services is that a doctor must certify your homebound condition.
Don’t Miss: Apply For Emergency Medicaid Utah
How To Get Medicaid Coverage For Care At Home
Traditionally, Medicaid has paid for long-term care in a nursing home, but because most individuals would rather be cared for at home and home care is cheaper, all 50 states now have Medicaid programs that offer at least some home care. In some states, even family members can get paid for providing care at home.
Medicaid is a joint federal-state program that provides health insurance coverage to low-income children, seniors, and people with disabilities. In addition, it covers care in a nursing home for those who qualify. Medicaid home care services are typically provided through home- and community-based services “waiver” programs to individuals who need a high level of care, but who would like to remain at home.
Local Elder Law Attorneys in Your City
City, State
Medicaid’s home care programs are state-run, and each state has different rules about how to qualify. Because Medicaid is available only to low-income individuals, each state sets its own asset and income limits. For example, in 2021, in New York an applicant must have income that is lower than $884 a month and fewer than $15,900 in assets to qualify. But Minnesota’s income limit is $2,382 and its asset limit is $3,000, while Connecticut’s income limit is also $2,250 but its asset limit is just $1,600.
States also vary widely in what services they provide. Some services that Medicaid may pay for include the following:
- In-home health care
- Minor modifications to the home to make it accessible
- Medical equipment
Do Medicare Advantage Plans Cover In
Medicare Advantage plans provide your Medicare Part A and Part B coverage. Instead of getting Part A and Part B through the federal government directly, you get them through a private insurance company that contracts with Medicare.
So, your in-home health care benefits will be at least the same as what Medicare Part A and Part B offer . Medicare Advantage plans may have annual deductibles, and may charge coinsurance or copayments for these services. Medicare Advantage plans have out-of-pocket maximum amounts, which protect you from unlimited health-care spending.
Youll need to keep paying your Medicare Part B premium when you have a Medicare Advantage plan.
Want to learn more about Medicare Advantage plans? Its easy to take a look at the plans in your area and see what benefits they offer besides Medicare Part A and Part B coverage. Just type your zip code in the box on this page, and you can compare Medicare Advantage plans at your convenience.
New To Medicare?
Becoming eligible for Medicare can be daunting. But don’t worry, we’re here to help you understand Medicare in 15 minutes or less.
Read Also: Centers For Medicare And Medicaid Services Login
Family And Caregiver Assistance
Recently recognized as one of the most important care programs for maintaining stability in a home living environment. This program includes respite care, short term relief for primary caregivers. Qualifying for this program shouldnt be a problem as it is included in almost every Medicaid sponsored relief program, in almost all states.
Enrolling In An Aetna Medicare Advantage Plan
Not all of the benefits outlined above may be available with all plans in every location. Compare Aetna Medicare Advantage plans online to find out exactly what benefits are available from plans offered where you live, and compare the costs of your different Aetna plan options.
You can also connect with a licensed insurance agent for help exploring Aetna Medicare Advantage plans in your area that may offer similar or additional home health care benefits.
Read Also: How Much Does Medicaid Cover For Nursing Home
Does Medicaid Cover Home Care
Medicaid is a bit less black and white than Medicare because it is administered by the states. Therefore, the state you live in determines which home care services are covered and what eligibility requirements you must meet. In general, you can expect that if you qualify for Medicaid in your state, some level of home care will be covered.
Did You Know: In some states, family members can be paid by Medicaid for providing personal care to their aging loved one.2
To find out whether you are eligible for Medicaid home care and which services are available to you, find your state’s Medicaid profile on Medicaid’s Home & Community Based Services page. Then, contact your state’s Medicaid department directly.
Using Life Insurance To Pay For Home Care
There are a few ways that seniors who have life insurance policies can use them to pay for home care. Options include taking a loan from the policys cash value or surrendering the policy entirely in exchange for the cash value.
Some policies may feature an accelerated death benefit rider, which is a cash advance that is subtracted from the death benefit amount the beneficiary receives upon the death of the policy holder. The owner of the policy must be terminally ill with a limited life expectancy or be deemed unable to perform basic activities of daily living . The policy is not surrendered at the time of the cash advance, so the policy holder must continue to pay the premiums to guarantee the beneficiary receives what remains of the original death benefit. The insurance company will require physicians statements and medical records attesting to the illness or loss of function before they will pay out any early benefits.
You May Like: Anthem Medicaid Ky Dental Providers
What Are Home And Community Based Services
Home and Community Based Services allow Medicaid recipients to receive necessary services in their own homes or as part of their existing community. Eligibility for HCBS depends on the state youre applying in, but its generally based on whether the recipient would otherwise need care in an institutional setting, like a nursing home.
Many seniors are reluctant to move into nursing homes, especially if theyre currently living in a senior community or if they expect their health problems to improve over time. For these individuals, in-home care including necessary medical care and help with day-to-day tasks is often preferable.
Virginia’s Medicaid Waiver Programs
Virginia’s Commonwealth Coordinated Care Plus Waiver, a combination of the waivers formerly known as the Elderly and Disabled with Consumer Direction Waiver and the Technology Assisted Waiver Waiver, helps seniors and disabled individuals receive long-term care services in the community.
The CCC Plus Waiver program provides care in the home and community, rather than in a nursing or other specialized care facility, to those who require a hospital or nursing home level of care. To eligible individuals who are 65 or older or disabled, and certain others who are functionally dependent and have medical nursing needs, the CCC Plus Waiver program offers services like adult day health care, respite care, personal care, medication monitoring, private-duty nursing, environmental modification, assistive technology, emergency response systems, and case management for those who live at home. Depending on your income, you may have to pay a portion of the cost of your services under this program. In this program, you can choose to either have an agency hire and supervise your personal care attendants, or you can choose to hire and supervise your own. If you choose the “consumer-directed” model, the state will assign a services facilitator to help you coordinate your own care.
Other waiver Programs are available for Virginians with intellectual or developmental disabilities. For more information about those, contact your local Community Services Board.
You May Like: Alabama Medicaid Application For Child
Medigap Coverage Of Home Care Services
Also known as Medicare Supplement Insurance, Medigap is additional policy coverage that works alongside Original Medicare benefits . The supplemental policy is purchased from a private company to pay for the gaps in costs not covered by Medicare, such as copays and deductibles. Neither Medicare nor Medigap policies are designed to pay for long-term care, so their coverage for in-home services is typically limited to medically necessary care over the short term. If a senior does not meet Medicares requirements for home health care coverage, then a Medigap plan will not minimize out-of-pocket costs for these services.
Read: Take the Confusion Out of Buying Medicare Supplemental Insurance
Using Va Health Benefits To Pay For Home Care
The Veterans Health Administration Standard Medical Benefits Package may be used to provide various levels of home care services as an alternative to nursing home care and as a way of delivering respite care for veterans and their family caregivers. The VAs Skilled Home Health Care Services , Homemaker and Home Health Aide Services , and Home-Based Primary Care programs are available to all veterans who meet eligibility requirements for standard benefits, although some additional conditions may apply.
Read:Understanding the VA Home Care Program
Don’t Miss: Vision Care That Accepts Medicaid
What Are Private Duty Nursing Services And How Are They Different From Home Health Services
Private Duty Nursing Services are Medicaid State Plan skilled nursing services that are provided on a continuous basis to Medicaid clients of any age in their home.
Home Health Services are Medicaid State Plan services that are provided on a part-time and intermittent basis to Medicaid clients of any age. Home Health services include home health nursing, home health aide, and skilled therapies .
How Does Medicaid Coordinate With Other Insurance
Medicaid acts as the payer of last resort when a beneficiary has an employer-based or other private commercial insurance plan. This means Medicaid will be the last plan to contribute to a medical bill and may pick up copayments and coinsurances in similar fashion to how Medicaid works with Medicare.
Recommended Reading: Dentist In Montgomery Al That Accept Medicaid
Types Of Programs Covered By Medicaid
As of October 2021, the services that are covered by Medicaid/Medicare for individuals living at home or in a facility extends beyond simple home health care services like companionship or light house-keeping. Medicare/Medicaid covers a variety of services, and the services offered are personalized for the patient and are delivered on an as-needed basis the list of services is long & updates frequently, make sure to stay on top of it by checking out Medicares official home health services page here.
Using Income And Savings To Pay For Home Care
Most families pay out of pocket for in-home care services. Possible sources used to cover private pay home care expenses might include individual retirement accounts , health savings accounts , pensions, investments, annuities, real estate and Social Security benefits. Although seniors may be hesitant to use their hard-earned savings or liquidate assets, it is important to consider that properly spending down almost all assets is required to qualify for Medicaid. By and large, elder care needs grow over time and higher levels of long-term care are increasingly expensive. Unless an aging loved one has amassed significant savings, it is important to consider the possibility that they may outlive their funds and need to apply for Medicaid when creating a long-term financial plan.
Read: Spending Down for Medicaid: One Caregivers Personal Journey
Also Check: Dentists In Logan Utah That Accept Medicaid
Does Aetna Cover Home Health Care
- Aetna Medicare Advantage plans can cover home health care such as physical therapy, skilled nursing care, home meal delivery, non-emergency transportation and more. Learn about other Aetna Medicare plan benefits and find out how you can compare plans online and enroll.
Many home health care services and items can be covered by an Aetna Medicare Advantage plan, allowing plan members to continue living safely and comfortably in their own home or in a nursing home or assisted living facility.
What Are Home Health Services
Home Health Services are Medicaid State Plan services provided on a part-time and intermittent basis to Medicaid consumers of any age. Home health services include home health nursing, home health aide, and skilled therapies . The only provider of home health services is a Medicare Certified Home Health Agency .
The medical necessity for home health services must be certified by the consumer’s qualifying treating physician. A face-to face encounter with the consumer and the physician, advanced practice nurse in collaboration with the physician, or a physician assistant under the supervision of the physician is required for certification of medical necessity. A face-to-face encounter must be conducted within the 90 days prior to the home health care start-of-care date, or within 30 days following the start-of-care date, inclusive of the start-of-care date.
Recommended Reading: How Can I Check The Status Of My Medicaid
Learn More About Medicare
Join our email series to receive your free Medicare guide and the latest information about Medicare and Medicare Advantage.
For services covered by both Medicare and Medicaid, Medicare pays first and Medicaid serves as the secondary payer. That means Medicare will pick up the bill first and pay its share before handing it off to Medicaid. Copayments and coinsurances that are left remaining after Medicare applies its coverage will be picked up by Medicaid.
Dual-eligible beneficiaries can expect to pay little to nothing out of their own pocket after Medicaid has picked up its share of the cost.
There are also some additional ways in which Medicaid beneficiaries can save money on care with Medicares help.
- Dual-eligible beneficiaries are often automatically enrolled in a Medicare Savings Program , which covers the Medicare Part B premium and may offer additional services.
- Dual-eligible beneficiaries also generally receive Extra Help, which provides assistance with Medicare Part D drug costs.
- There are certain types of Medicare Advantage plans known as Dual-eligible Special Needs Plans that are custom built to accommodate the specific needs of those on both Medicare and Medicaid.
