Income Guidelines For Children’s Medicaid
Your income is the money you get paid before taxes are taken out. Find your family size on the table below. If your monthly income is the same or less, your child might get Children’s Medicaid.
| Family Members | Monthly Family Income |
|---|
| For each additional person, add: | $761 |
*A family of one might be a child who does not live with a parent or other relative.
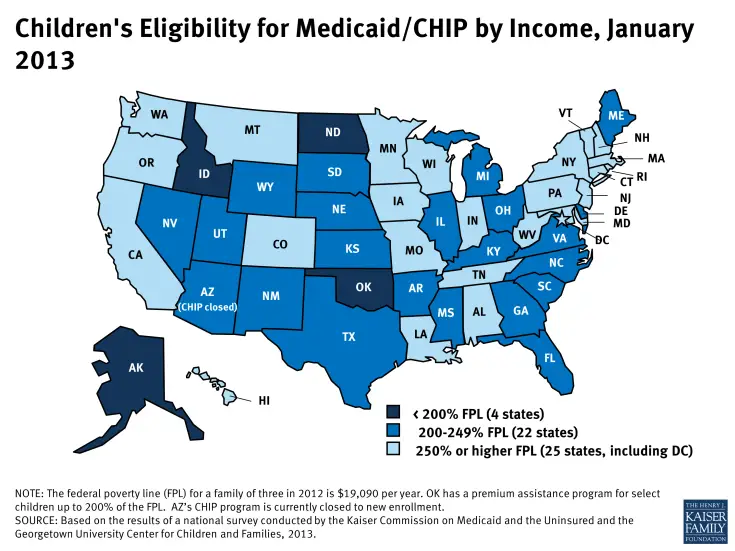
Can I Get Medicaid For My Children
Yes, if your income is not too high. Medicaid and The Children’s Health Insurance Program provide low cost coverage to millions of families with children. Income requirements vary by state. In all but two states, children who live in four-person households with incomes up to $52,400 qualify for either Medicaid or CHIP. Eighteen states and DC will cover children in families of four who earn even up to $78,600, although sometimes families at the higher eligibility levels may need to pay more for the coverage.
If you have a baby while you’re on Medicaid, your baby will automatically be enrolled in Medicaid for their first year.
South Dakota Medicaid For Youth Formerly In Foster Care
The Former Foster Care Medical Program provides extended medical coverage for youth age 18 to 26 that are leaving State foster care after their 18th birthday. Referrals for this program are normally generated by the Division of Child Protection Services staff. You may also call 877.999.5612 for further information.
Eligibility Requirements
- The youth must have been in foster care under the responsibility of the State of South Dakota on his/her 18th birthday.
- The youth must be a resident of South Dakota.
- There is no resource or income limit.
- Eligibility continues from the month the youth is no longer under the responsibility of the State until the end of the month in which the youth attains age 26 if s/he meets all other eligibility requirements.
Don’t Miss: Dual Enrollment Medicare And Medicaid
Medicaid Coverage Improves Families Access To Care Health And Financial Security
A large and growing body of research shows Medicaid expansion has improved access to medical care and health for parents and other adults with low incomes. In Arkansas and Kentucky, parents and other adults with low incomes saw significant gains in access to care and improvements in self-reported health compared to those in Texas, which hasnt expanded Medicaid. And mental health outcomes improved among parents who gained Medicaid coverage through pre-ACA increases in state eligibility limits.
Improved parental access to care and health is important to their children because childrens health and development depends in part on their parents health and well-being. Childrens relationships with their parents can influence their brain structure and function, such as by mitigating the negative effects of trauma, poverty, or other adverse childhood experiences. For example, maternal depression can negatively affect childrens cognitive and social-emotional development as well as their educational and employment outcomes.
Research also confirms that coverage gains for parents, and the associated gains for children, improve childrens access to care. For example, a 2017 study found that children are 29 percentage points more likely to have an annual well-child visit if their parents are enrolled in Medicaid.
Applying For Apple Health Coverage
You have many options to apply for Apple Health coverage. Visit our Apply for or renew coverage webpage to learn more.
When youre ready to apply, youll need:
- Your household monthly income.
- The Social Security numbers and dates of birth for each member of your household.
- Your immigration information, if that applies to you.
You May Like: Does Uc Health Accept Medicaid
Can I Get Medicaid And Medicare At The Same Time
You may in some situations. Medicare is a health insurance program for:
- People ages 65 and older
- People younger than age 65 who are disabled
- People with end-stage kidney disease
With Medicare, you have to pay monthly premiums and other costs, such as copays and deductibles, when you go for medical care. If you are on Medicare and have a limited income, you may qualify for help from Medicaid to pay the costs of Medicare. If you have both Medicaid and Medicare, you may hear people refer to you as being dually eligible.
What If Im Turned Down By Medicaid
- You may be able to buy a private health plan through the Marketplace instead for the 2018 plan year in the fall. You may qualify for savings based on your income through a premium tax credit and savings on out-of-pocket costs.
- If you don’t qualify for either Marketplace or Medicaid savings, you still have options. Learn more here.
Recommended Reading: When Did Medicaid Expansion Start
What Is The Medicaid Program
Good health is important to everyone. If you can’t afford to pay for medical care right now, Medicaid can make it possible for you to get the care that you need so that you can get healthy and stay healthy.
Medicaid is available only to certain low-income individuals and families who fit into an eligibility group that is recognized by federal and state law. Medicaid does not pay money to you instead, it sends payments directly to your health care providers. Depending on your state’s rules, you may also be asked to pay a small part of the cost for some medical services. In general, you should apply for Medicaid if you have limited income and resources. You must match one of the descriptions below:
Why Implement Continuous Eligibility
Children who have health insurance continuously throughout the year are more likely to be in better health. Guaranteeing ongoing coverage ensures that children can receive appropriate preventive and primary care as well as treatment for any health issues that arise. Stable coverage also enables doctors to develop relationships with children and their parents and to track their health and development. Additionally, eliminating the cycling on and off of coverage during the year reduces state time and money wasted on unnecessary paperwork and preventable care needs.
You May Like: Medicaid Brooklyn Ny Phone Number
Q How Long Will My Medicaid Benefits Remain Active
A. Medicaid is based on month to month eligibility. However, your benefits are redetermined on a yearly basis by DMMA to confirm whether you still remain eligible for the program you are receiving. Certain Medicaid programs require you to report changes in your situation within 10 days of the change. One example of a change that must be reported is new employment.
Learn More About Medicare
Join our email series to receive your free Medicare guide and the latest information about Medicare and Medicare Advantage.
Another type of Medicaid program is Early and Periodic Screening, Diagnostic, and Treatment . This program is available to individuals under the age of 21 who live in households that meet certain financial criteria. This type of Medicaid also has an age restriction and could therefore also be considered age-based.
ABD and EPSDT are required by federal law to be included in all state Medicaid programs. But as long as certain federal requirements are met, state Medicaid programs are free to offer their own Medicaid benefits and eligibility guidelines to people who might not otherwise be eligible for these two programs. Age may or may not play a role, depending on where you live.
For example, Medicaid in North Carolina is only available to those age 65 and over or 21 and under unless you are pregnant, are responsible for a child age 18 and under, disabled or require long-term care.
But in North Dakota, Medicaid is available to all low-income adults, regardless of age.
It could be said that Medicaid is age-based in some states and for some programs, but it is not universally age-based.
Read Also: Vermont Medicaid Dental Fee Schedule
Q If I Have Private Health Insurance Can I Be Eligible For Medicaid
A. It depends. If your income is low, and you have minor children, you and your children can have private health insurance and still be eligible for Medicaid. Certain Medicaid qualifying programs require that you not have any other health insurance in order for you to get Medicaid. If you have both private health insurance and Medicaid, you should show both your Medicaid card and your private health insurance card to your medical provider each time you receive services.
Social Security Work Incentives
Dont let concerns about SSI benefits stop you from encouraging your child to find an employment setting that is right for them. Parents of youth with disabilities are very aware of the importance of healthcare for their children. Many have heard that SSI recipients will lose their Medicaid coverage if they earn any money. As a result, some families discourage their young adults from joining the workforce. This is not true. Be aware that the Social Security Administration has Work Incentive programs that allow young adults with disabilities to continue to receive Medicaid coverage while they explore careers or attend postsecondary education or job training.
Make an informed choice. If your son or daughter receives SSI, contact a Work Incentives Planning and Assistance Project in your state to see how they can continue to receive health coverage through Medicaid while they work. WIPA projects are community-based organizations that receive grants from SSA to provide all Social Security and Supplemental Security Income disability beneficiaries with free work incentives planning and assistance.
WIPA services are available in every state, the District of Columbia, and the U.S. Territories of American Samoa, Guam, the Northern Mariana Islands, Puerto Rico, and the Virgin Islands. Call 1-866-968-7842 or 1-866-833-2967 for locations WIPA organizations or see the online SSA service provider directory.
Recommended Reading: Guidelines To Qualify For Medicaid
Home And Community Based Waivers
Home and Community Based Services Waivers are Medicaid programs that provide services in the home for persons who would otherwise require institutional care in a hospital or nursing facility. Without waiver services being delivered in the community, some young adults might not be able to live at home or receive needed supports in the workplace.
Can I Get Medicaid
States have different rules to decide who’s eligible for Medicaid. You may be eligible if:
You’re disabled. Your state may let you use Medicaid no matter how much money you make in a year. In other states, a disabled person may only qualify for Medicaid when their income falls below a cutoff level.
You already get Supplemental Security Income . In the majority of states, SSI eligibility automatically qualifies you for Medicaid unless your state uses more strict criteria. Those states are commonly called 209 states.
You don’t make much money during a year. The rules are different in each state.
Check with your state’s Medicaid office to get the exact income requirements. You can also find out if you qualify by going online at www.healthcare.gov.
Some states have expanded their Medicaid program to allow more people to qualify. In those states, the income rules have loosened for adults without children. Other states have chosen not to expand Medicaid.
If your state has expanded Medicaid under the Affordable Care Act:
You’re eligible if:
- You’re single, don’t have children, and make less than $17,609 a year.
- You have a family of three and make less than $29,974 a year.
If your state has NOT expanded Medicaid:
In Alaska and Hawaii, youâre able to make a slightly higher income than in other states and still qualify. Your state Medicaid office can help you with the specific income limits based on how many people are in your family.
Recommended Reading: Child Behavioral Therapist That Accept Medicaid
Do I Qualify For Medicaid
Medicaid provides free or low-cost health coverage to some low-income people, families and children, pregnant women, the elderly, and people with disabilities. Many states have expanded their Medicaid programs to cover all people below certain income levels. Medicaid qualifications depend partly on whether your state has expanded its program.
Who Qualifies For Medicaid
Medicaid qualification is different in every state. You must be a resident of the state in which you are applying for benefits and must be a U.S. citizen or otherwise qualified non-citizen such as a lawful permanent resident.
Federal law requires every state to provide Medicaid to the following mandatory eligibility groups that meet certain income and asset requirements:
As you can see from the federal guidelines, the only reference to age is in regards to children. Each state governs its own Medicare program in adherence to federal regulations. Some states may have an age requirement in order to qualify for its Medicaid program while other states may not.
You can find your states Medicaid eligibility requirements to learn more.
Also Check: Does Medicaid Cover A Breast Reduction
Provider Responsibility To Screen For Vfc Eligibility
Screening to determine a childs eligibility to receive vaccines through the VFC Program and documentation of the screening results must take place with each immunization visit. The patient eligibility screening record provides a means of recording parent responses to VFC eligibility questions. The parent, guardian or provider may complete this form. Verification of parent/guardian responses is not required. To maximize efficiency, providers may elect to incorporate these screening questions into an existing form however, any revision must include the core screening information listed on the CDC-developed form and be approved by the state Immunization Program. Patient eligibility screening records should be maintained on file for a minimum of 3 years after service to the patient has been completed unless state law/policy establishes a longer archival period.
What Does Medicaid Cover
In each state, Medicaid must cover:
- Birth control medicine and devices
- Care at rural and federally qualified health clinics
- Care at many childbirth centers
- Care from a pediatrician or family nurse practitioner
- Early Periodic Screening, Diagnostic, and Treatment Services , which includes an array of services for children and adolescents
- Doctor’s fees
- Nurse midwife care during pregnancy and childbirth
- Preventive care and immunizations for children under age 21
- Quit-smoking programs
- Transportation to medical care
Many states offer more care, such as checkups and cancer screening tests for adults, physical therapy, and occupational therapy.
Read Also: Does Medicaid Cover Gastric Balloon
Elderly Individuals Who Would Require Nursing Home Care If Not For Special Services Performed In Their Home
Elderly individuals living independently in their own homes may be eligible for South Dakota Medicaid.
Eligibility Requirements
- A person must be in need of nursing facility care.
- A person must not be a resident of a hospital, nursing facility or an intermediate care facility for the mentally retarded.
- A person must be a resident of South Dakota and meet certain citizenship requirements of the United States.
- The monthly income limit is 300 percent of the SSI Standard Benefit Amount.
- The resource limit is $2,000. Resources include items such as checking or savings accounts and certificates of deposit.
to the standard Medicaid covered services
Homemaker Services: Teaching and providing home management skills, promoting self-care, making beds, changing linens, washing dishes, laundry work, floor care and housecleaning. Providing meal preparation, shopping and menu planning. Providing non-South Dakota Medicaid in mobility, personal comfort and grooming of the individual. Arranging for transportation.
Private Duty Nursing: Nursing services provided by a licensed nursing professional for recipients with chronic and stable conditions who require more individual and continuous care than is available from a part-time or intermittent nursing service.
Adult Day Care: Services providing out-of-home structured health and social services on a regularly scheduled basis and in daytime settings.
Quadriplegics Who Would Require Nursing Home Care If Not For Special Services Performed In Their Home
Individuals with quadriplegia living independently in their own homes may be eligible for South Dakota Medicaid. Individuals who are eligible are entitled to full South Dakota Medicaid coverage.
Eligibility Requirements
- A person must be age 18 or older and have quadriplegia.
- The income limit can be up to $2,382 month.
- The resource limit is $2,000. Resources include items such as checking and savings accounts and certificates of deposit.
Recommended Reading: How Can I Check The Status Of My Medicaid
South Dakota Medicaid For Certain Newborns
South Dakota children born to women eligible for South Dakota Medicaid are also eligible for South Dakota Medicaid.
Eligibility Requirements
- The child must be born to a woman eligible for and receiving South Dakota Medicaid on the date of the childs birth.
- There is no resource or income limit.
- Coverage continues from the month of birth until the end of the month in which the child turns one year of age as long as the child continues to live in South Dakota.
Colorado Indigent Care Program
The Colorado Indigent Care Program provides discounted health care services to low income people and families. CICP is not a health insurance program. Services vary by providers.
Who Qualifies?
You must be 18 and olderYou must be at or below 250% of the Federal Poverty Level You must be lawfully present in the United States and a legal resident of ColoradoYou cannot be eligible for Health First Colorado or Child Health Plan Plus
Top Benefits:
Discounted health care services provided by participating Colorado hospitals and clinicsNo premium costsYou are allowed to have primary health insurance or have MedicareCICP ratings are good for a full year, see program information page for exceptions
Co-pay Costs:
| Program Information Page |
Recommended Reading: How Much Does Medicaid Pay For Family Caregivers
Lawfully Residing Targeted Low
States have the option to provide CHIP and Medicaid coverage to children and pregnant women who are lawfully residing in the United States and are otherwise eligible for coverage, including those within their first five years of having certain legal status. If states do not adopt this option, federal law requires a 5-year waiting period before many legal immigrants are permitted to enroll in Medicaid and CHIP. Learn more about providing health coverage to lawfully residing children and pregnant women at 2107 of the Social Security Act, and in SHO# 10-006 . A list of states providing Medicaid and CHIP coverage to lawfully residing children and/or pregnant women.
