Wellcare Of North Carolina To Partner With Behavioral Health Plans
- Medium
- Large
Centene subsidiary WellCare of North Carolina has partnered with the state’s selected behavioral health plans to assist in care coordination, according to an Aug. 2 news release.
The state’s Department of Health and Human Services on July 26 announced the selection of seven organizations to serve as behavioral health and developmental disability tailored plans, effective July 1, 2022. The plans will serve individuals with mental illnesses, substance use disorders, developmental disabilities and traumatic brain injuries.
WellCare will contract with its local management entities and managed care organizations to facilitate care to the health plans’ patients, Centene stated.
What Is A Standard Plan
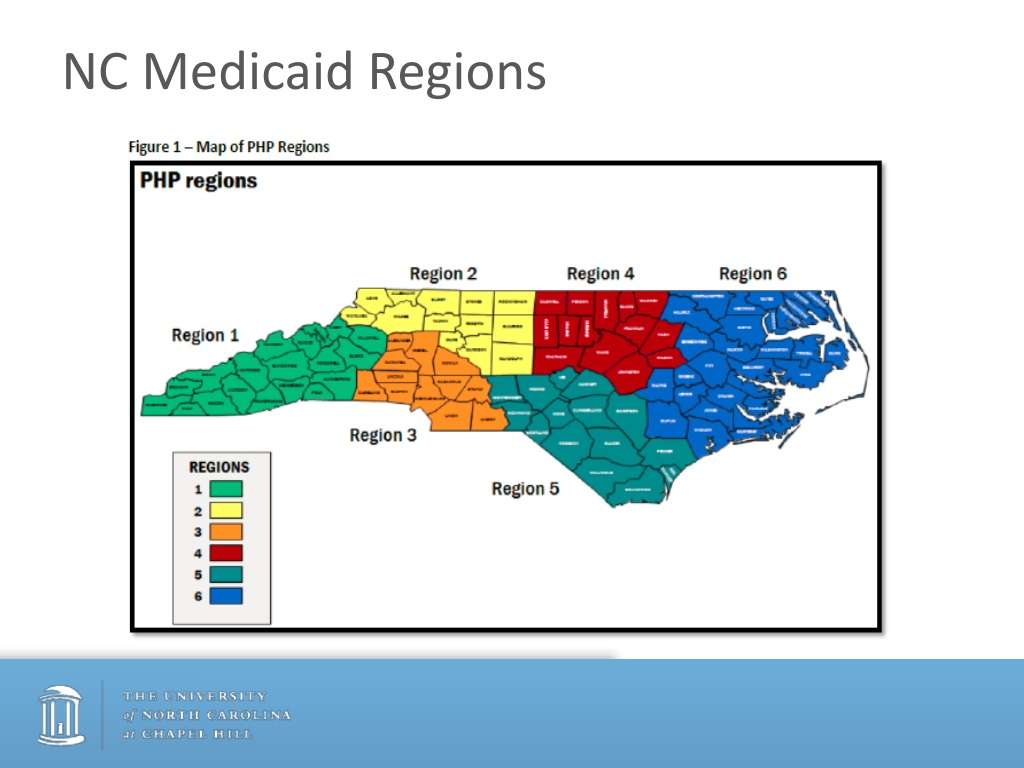
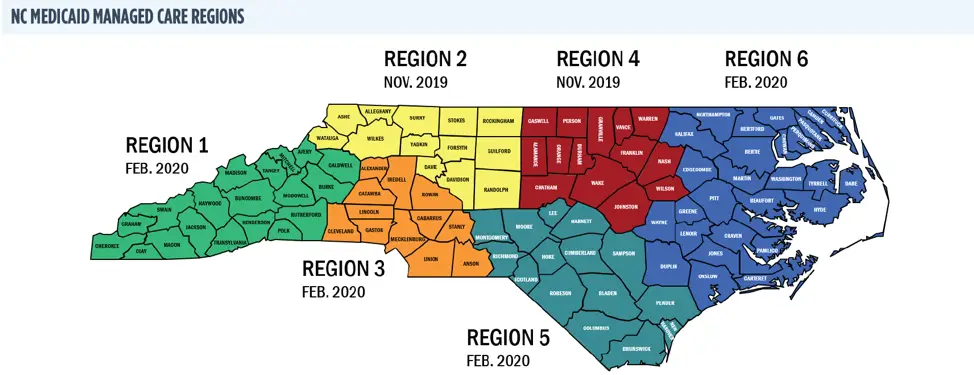
There are six health plan contracts, five prepaid health plans and one primary care case management entity, to deliver Standard Plan Medicaid services starting July 1, 2021, to eligible North Carolina beneficiaries.
AmeriHealth Caritas of North Carolina Prepaid Health Plan StatewideBlue Cross and Blue Shield of North Carolina Prepaid Health Plan StatewideUnitedHealthcare of North Carolina Prepaid Health Plan StatewideWellCare of North Carolina Prepaid Health Plan, StatewideCarolina Complete Health, Inc. Prepaid Health Plan, Regions 3, 4 and 5Eastern Band of Cherokee Indians Tribal Option Primary Care Case Management managed by the Cherokee Indian Hospital Authority. For federally recognized Tribal members and others eligible for services through the federal Indian Health Service agency.
North Carolina Medicaid Good Faith Contracting Policy
May 19, 2021
WellCare NC Medicaid Good Faith Contracting Policy
1. The network will be developed, filed, and maintained to meet the Departments availability, accessibility, and quality goals and requirements in accordance with state regulations, accrediting bodies, and company guidelines.
2. During the initial development of the network, WellCare will proactively reach out to providers with an offer to contract in writing. WellCare will use the Departments historical claims payment file to send contracts to all providers actively seeking Medicaid eligibility, as well as all hospital systems, AMH certified providers, essential providers, key provider groups and all other required provider types. Follow up activities after written offers are made will take place within 10 business days, either by phone or email to ascertain interest and answer questions. All offers and follow up activities will be documented in WellCares contract management system and will include date of initial offer and any follow up performed by phone or email.
3. If WellCare receives a direct inquiry for a contract, either in writing or via telephone,WellCare will engage in contract negotiations by offering the provider a contract. WellCare will negotiate, regardless of provider or PHP affiliation, to contract with providers in writing and all offers shall include the required standard provisions as required by the state of North Carolina.
Recommended Reading: The Phone Number For Medicaid
Choosing A Provider Or Pharmacy
WellCare of North Carolina is a managed care plan. This means that you will need to use doctors and other providers that are part of the plan’s network.
We regularly add new providers to our network. You can download a copy of our latest Provider Directory from this web page. Or, you can use our online Find a Provider/Pharmacy tool for the most up-to-date listings.
We look forward to serving you!
Wellcare Medicaid Provider Trainings
WellCare Medicaid Provider Training sessions are available for you to meet your Provider Relations Representative, register for our WellCare Provider Portal, and provide an overview of WellCare provider support for the transformation from Medicaid Fee-for-Service to Medicaid Managed Care.
Webinar invitations will be sent to each Provider via Email. Face to face meetings will introduce your assigned Provider Relations Representative and provide an orientation to the training modules on the WellCare provider portal.
If you have any questions about the WellCare Medicaid Provider Training sessions, please feel free to Email .
| Training Topic |
|---|
Don’t Miss: Humana Medicaid Florida Over The Counter
Welcome To Wellcare Of North Carolina
Thank you for choosing WellCare of North Carolina. We are happy to serve you and your family, and to provide you with the quality healthcare services you deserve.
This website will help you learn how to work with WellCare of North Carolina. It will also help you to get the most out of your healthcare benefits.
But remember, our Member Services representatives are just a phone call away. They are dedicated to helping you get access to the right care. So, don’t hesitate to pick up the phone and give us a call if you have questions about your plan. You can call us toll-free at 1-866-799-5318 . We’re here for you MondaySaturday, 7 a.m. to 6 p.m.
Wellcare Of North Carolina
Welcome to the WellCare of North Carolina page. Here you can download policies and procedures specific to both ordering providers and imaging facilities. These include quick reference guides and information designed to assist you in using the RadMD Website to obtain and check authorizations.
Any services requested that are listed on the IFSP form will be redirected back to Medicaid Direct for children less than 3 years of age. NIA will not process these requests.
If you have any questions about the NIA Program, please contact your dedicated NIA Provider Relations Manager, Priscilla Singleton.
Radiology Benefits Management
RadMD Documents
RadMD is our user-friendly, real-time tool that provides you with instant access to the high-tech imaging authorization and supporting information you need. Whether submitting imaging exam requests or checking the status of a prior authorization request, you will find RadMD to be an efficient, easy-to-navigate resource.
Search for resources by solution below:
Recorded General Trainings
We have a series of training videos that discuss the components of requesting a prior authorization request. Click here to access these videos.
Recorded RadMD Demos
Need additional help using RadMD? Click here to access a series of RadMD demos that demonstrate how to properly submit a prior authorization request.
Clinical Guidelines
Clinical Training Modules
You May Like: Will Medicaid Pay For Portable Oxygen Concentrator
How To Access Coverage In The Event Of A Disaster Or Local Emergency
In the event of an emergency or natural disaster, WellCare is committed to helping you continue to access care easily. In a time of crisis, we will:
- Allow Part A and Part B and supplemental Part C plan benefits to be furnished at specified non-contracted facilities , be furnished at Medicare certified facilities)
- Waive in full, requirements for gatekeeper referrals where applicable
- Temporarily reduce plan-approved out-of-network cost-sharing to in-network cost sharing amounts
- Waive the 30-day notification requirement to enrollees as long as all the changes benefit the enrollee
- Allow you to fill medications sooner than usual to ensure you have what you need during the emergency
These actions will be in effect through the emergency declaration period. Disasters/Emergencies may be declared by the U.S. Government, the Federal Emergency Management Agency , or the Governor of any state.
Typically, the source which declares the disaster will clarify when the disaster or emergency is over. If however, the disaster or emergency timeframe has not been closed 30 days from the initial declaration, and if the Centers for Medicare & Medicaid Services has not indicated an end date to the disaster or emergency, we will resume normal operations 30 days from the initial declaration.
WellCare also offers Special Needs Plans to qualifying individuals. To enroll in a Special Needs Plan, please contact us for more information.
Nc Medicaid Is Changing
As of 1 Sept 2021 Sandhills Pediatrics is participating with Medicaid Health Plans Carolina Complete Health, Wellcare and NC Medicaid Direct.
Comparison website between Carolina Complete Health and Wellcare
This new system of paying for healthcare for NC Medicaid and NC Health Choice beneficiaries in NC started 1 July 2021.
IF you have received a letter saying you are signed up with AmeriHealth Caritas, Healthy Blue, or United HealthCare Community Plan, and would like to still see Sandhills Pediatrics, THEN please call the enrollment broker 1-833-870-5500 and ask to switch to Carolina Complete Health or Wellcare. . You will still be able to see us regardless of what plan is on your card until 30 November 2021) BUT best to get this fixed ASAP while you are thinking about it!
If your plan is Carolina Complete Health or Wellcare and your Primary Care Provider is someone other than Sandhills Pediatrics and you us to be your childs doctor, please call them and tell them you want to switch PCPs.
- Carolina Complete Health 833-552-3876 and follow the prompts for member services
- Wellcare 866-799-5318
You can also contact the enrollment broker to pick a plan at:
- 833-870-5500 Hours of operation: 7 a.m. to 8 p.m., Monday through Sunday
Our group NPI is 111-499-8150
Our central office address is: 195 W ILLINOIS AVESOUTHERN PINES, NC 28387-5808
Our primary care doctors are:
- LINDSEY BELLAMY, DO
Comparison website between Carolina Complete Health and Wellcare
Anything Else?
Also Check: Does Medicaid Cover Root Canals For Adults
Wellcare Of North Carolina Announces Count On Me Covid
Program Offers $50 Walmart Gift Cards to Medicaid Members Who Get Vaccinated
RALEIGH, N.C., Dec. 20, 2021 /PRNewswire/ — As the holidays near, along with the first detection of the omicron variant in North Carolina, WellCare of North Carolina is launching a COVID-19 vaccine member incentive program to encourage its Medicaid members to get vaccinated. WellCare Medicaid members ages 5 and older who get fully vaccinated between Sept. 1, 2021 and June 30, 2022 are eligible to receive the incentive a $50 Walmart gift card.
“As we enter the holiday season and continue to see increasing COVID-19 transmission rates, it’s critical that all North Carolinians get vaccinated,” said Dr. Matt Oettinger, Vice President of Population of Health for WellCare of North Carolina. WellCare’s member incentive program will help increase rates of vaccination among our members, decrease COVID-19 infections in our communities, and help everyone in our state have a healthy holiday season and New Year.
WellCare is also outreaching to its members in care management to help increase access to vaccines. Medicaid Members with multiple chronic conditions often require care managers who can assist them with appointment scheduling, medication adherence, home safety assessments, and other supports, as needed. Care managers are also actively working to ensure members have access to the COVID-19 vaccine and other needed supports.
Behavioral Health Crisis Line
If you are experiencing a behavioral or mental health crisis, please call . Carolina Complete Health has clinicians available to speak with you 24 hours a day, seven days a week. They can connect you to the support you need to help you feel better. If you are in danger or need immediate medical attention, please call 911.
Don’t Miss: How Do I Add My Newborn To My Medicaid
Extra Support To Manage Your Health
Managing your health care alone can be hard. If you need extra support to get and stay healthy, we can help. As a member of WellCare of North Carolina, you may have a Care Manager on your health care team. A Care Manager is a specially trained health professional. They work with you and your doctors to make sure you get the right care when and where you need it.
Your Care Manager can:
- Coordinate your appointments and help arrange for transportation to and from your doctor
- Support you in reaching your goals to better manage your ongoing health conditions
- Answer questions about what your medicines do and how to take them
- Follow up with your doctors or specialists about your care
- Connect you to helpful resources in your community
- Help you continue to receive the care you need if you switch health plans or doctors
WellCare of North Carolina can also connect you to a Care Manager who specializes in supporting:
- People who need access to services like nursing home care or personal care services to help manage daily activities of living like eating or bathing and household tasks
- Pregnant women with certain health issues such as diabetes or other concerns such as wanting help to quit smoking
- Children from birth to age 5 who may live in stressful situations or have certain health conditions or disabilities
Keep Kids Fit And Healthy
What is the first thing your kids do when they come home from school? Do they grab a snack and head for the TV or computer?
Eating too much and not being active can make kids too heavy. In the last 20 years, the rate of overweight kids has doubled. About 15% of kids ages 6-19 weigh too much. That means that nearly one out of every five kids is too heavy.
Recommended Reading: Is Wisdom Teeth Removal Covered By Medicaid
Ambetter Of North Carolina
Ambetter of North Carolina Inc. is Centenes Health Insurance Marketplace product in North Carolina. Ambetter exists to improve the health of its beneficiaries through focused, compassionate and coordinated care. Our approach is based on the core belief that quality healthcare is best delivered locally.
- Health Insurance Marketplace
Dagiti Serbisio Ti Parmasia
WellCare of North Carolina Will Pay for the Drugs that Medicaid Requires You to Have.
It is also important to know that WellCare of North Carolina uses a Preferred Drug List .
- The PDL is a list of drugs that we prefer your doctor use
- The drugs on the PDL are organized by brand and generic name
- Quantity, gender and age limits are also provided
- Some drugs require step therapy – the use of other drugs first before they will be approved. These are noted with an “ST”
- Some of these drugs require a review and are noted with a “PA” .
Find a drug by searching our online tool or viewing/printing a PDL
The NC Medicaid Preferred Drug List allows NC Medicaid to obtain better prices for covered outpatient drugs through supplemental rebates. The PDL was authorized by the NC General Assembly Session Law 2009-451, Sections 10.66-.
- Prescribers are encouraged to write prescriptions for preferred products.
- Prescribers may continue to write prescriptions for drugs not on the PDL.
- If a prescriber deems that the patients clinical status necessitates therapy with a non-preferred drug, the prescriber will be responsible for initiating a prior authorization request.
- Prior authorization requirements may be added to additional drugs in the future.
Also Check: Does Medicaid Cover Long Term Care Facilities
What Is A Tailored Plan
North Carolina will launch specialized managed care plans, called BH I/DD Tailored Plans, starting in 2021. These plans are designed for those with significant behavioral health needs and intellectual/developmental disabilities . BH I/DD Tailored Plans will also serve other special populations, including Innovations and traumatic brain injury waiver enrollees and waitlist members. Often this is called the high risk population.
Alliance Health was awarded a contract to operate a BH I/DD Tailored Plan beginning July 1, 2022.
What Is Changing
North Carolinas Medicaid program is changing. It will go from a state-run program to a managed care model. Managed care models are designed to better manage costs, use and quality of health care services. The new program will include 5 new Medicaid health plans, called Prepaid Health Plans .
Under the new Medicaid Managed Care program, most but not all NC Medicaid and NC Health Choice patients will need to:
- Pick 1 of the 5 new health plans
- Choose a Primary Care Provider and the office address you see them at
All of the plans offer the same basic health care benefits and services. However, the doctors and hospitals included in each health plan may be different. The health plans also offer different non health care related services.
Also Check: Is Medical Marijuana Covered By Medicaid
