How Can I Report Medicaid Fraud
If you suspect a person or a doctor, clinic, hospital, home health service or any other kind of medical provider is committing Medicaid fraud or abuse, report it.
Check The Status Of An Application
The Division of Family Resources provides tools to strengthen families through services that focus on prevention, early intervention, self-sufficiency, family support, and preservation.
You can check the status of your application online by clicking on your county of residence or by calling 1-800-403-0864. You will need to have your case number to check the status of your application.
Please remember that your application must be completed and all required documentation submitted before DFR can begin processing your application.
Pursuant to HIPAA and other applicable federal regulations, DFR is committed to respecting the privacy of each client. For that reason, DFR will not share or disclose information about your case without a signed release. You may download the DFR online.
Not Enrolled To Medicaid Heres How To Apply
If you have not yet enrolled yourself and/or your family, there are multiple methods you can use to enroll in Medicaid. Your first option is to enroll yourself and/or your family by going online and filling out an application for yourself and/or your family at the Health Insurance Marketplace. There you can follow the steps to create an account and provide your information such as whether or not you have a disability, your income level, and enroll any minor dependent children you have in health coverage programs such as the Childrens Health Insurance Program, otherwise known as CHIP.
Another method you can use to enroll in the Medicaid program is to directly contact your states Medicaid agency. You can find the agency contact information you need by visiting the Healthcare website. Scroll down to the state in which you reside, and you will be taken to the website of your local Medicaid agency. There you will be provided with telephone numbers for your local Medicaid agency which you can call during normal business hours in order to check if you and/or your family qualify for Medicaid.
You May Like: Children’s Medical Services Medicaid Florida
How Do I Find Out My Medicaid Application Status
Medicaid is a federally-funded health insurance program for low-income families that is administered by each state. The income requirements and types of coverage you get depend on state laws, but there are federal minimums that every state has to meet to qualify for funding. Each year, low-income families apply for Medicaid services that will allow them to get the health care they need. The application process can sometimes take a while, but there are ways to check the progress of your application.
Wait For The Letter
When your state Medicaid office receives your application, it will send out a letter that will give you a date you can expect coverage to start. At some point before that date, you should get insurance cards in the mail and a confirmation of the effective date. If you dont mind waiting, then you will get your application status mailed to you.
Look Online
These days, most states have an online application process set up for Medicaid that makes the process much easier. When you submit your application online, the website will create an account for you. If you ever want to check the status of your application, then you can just log into your online account and check.
Go To Your Medicaid Office
Medicaid Offers A Full Range Of Health Services For Eligible Persons Including:
- All regular medical checkups and needed follow-up care.
- Immunizations.
- Medical equipment and appliances .
- Lab tests and x-rays.
- Eye care and eye glasses.
- Emergency care.
- Emergency ambulance transportation to a hospital.
- Hospital stays.
For some pregnant women, services may be limited to perinatal care if their incomes are too high to qualify for full Medicaid coverage.
For children birth to 21 years old, Medicaid offers the Child/Teen Health Program , which provides the services listed above for all Medicaid recipients. C/THP places an emphasis on preventive care and treatment. For example, Medicaid requires that all children be screened with a blood lead test at one and two years of age. C/THP is available from fee-for-service healthcare providers. Also, all managed care plans must offer C/THP to Medicaid recipients under 21 years of age who are enrolled in their plan.
Child Health Plus and Family Health Plus provide services to eligible children and adults, respectively, through managed care plans.
Read Also: Https Portal Mmis Arkansas Gov Ar Medicaid Member
Illinoiss Requirements For Medicaid Qualification
The state of Illinois sets particular requirements for enrollees to qualify for the Medicaid program. First, certain income standards must get met if residents in the area hope to qualify. What was once given to children and pregnant women is now available for women and men as well, as long as they meet the criteria. Those who fall far above the poverty level cannot receive this state insurance. If you would like to find out if you should apply, use the Check If I Should Apply button on the Application for Benefits Eligibility website. It asks questions regarding your family size, age, gender, taxes, health coverage through work, medical needs, and more.
Medicaid Is The Nations Public Health Insurance Program For People With Low Income
Medicaid is the nations public health insurance program for people with low income. The Medicaid program covers 1 in 5 Americans, including many with complex and costly needs for care. The program is the principal source of long-term care coverage for Americans. The vast majority of Medicaid enrollees lack access to other affordable health insurance. Medicaid covers a broad array of health services and limits enrollee out-of-pocket costs. Medicaid finances nearly a fifth of all personal health care spending in the U.S., providing significant financing for hospitals, community health centers, physicians, nursing homes, and jobs in the health care sector. Title XIX of the Social Security Act and a large body of federal regulations govern the program, defining federal Medicaid requirements and state options and authorities. The Centers for Medicare and Medicaid Services within the Department of Health and Human Services is responsible for implementing Medicaid .
Figure 1: Medicaid plays a central role in our health care system.
Don’t Miss: Hearing Aids Covered By Medicaid
How To Find Out If My Medicaid Is Active
If you have limited financial resources, you should consider Medicaid, the federal-state partnership program. Currently, this affordable health insurance for individuals provides healthcare coverage for 20 percent of Americans, thus helping them cover some of their medical costs. One of its major benefits is that, unlike Medicare, it offers coverage for personal care services and nursing home care, which you or your loved ones may need on a long-term basis but cannot afford.
Read More: What Is Comprehensive Medical Insurance?
Affordable Care Act Subsidized Plans After Medicaid
Special Enrollment Status: If you lose your Medicaid health coverage, a Special Enrollment Period opens up for you. During an , you can obtain full-featured health insurance known as an Affordable Care Act plan.
The SEP is only a 60-day window, so you have to act quickly. Tools like HealthCare.com help you determine which plan is best for your needs and budget.
Without a Special Enrollment Period, you can enroll in a health plan only during the annual Open Enrollment Period, which generally lasts from November 1 through January 15. Once the window closes, you will be unable to enroll in healthcare coverage until the next open enrollment period.
For example, if your Medicaid is canceled as of March 1, you will have 60 days to enroll in a health plan through Obamacare. If you dont enroll by the end of that 60-day window, you will have to wait until the next open enrollment period, and the coverage would not be effective until January 1 of the following year.
If you know when your Medicaid plan ends, you can sign up in advance. Health insurance plans are generally effective the first day of the following month after you apply, but a new application may take some time to process.
ACA Discounts for Low and Moderate Incomes: The cost of health insurance premiums can be intimidating, but help is available. Depending on your income level, you might receive a subsidy for ACA coverage.
Read Also: How To Become A Medicaid Provider In Texas
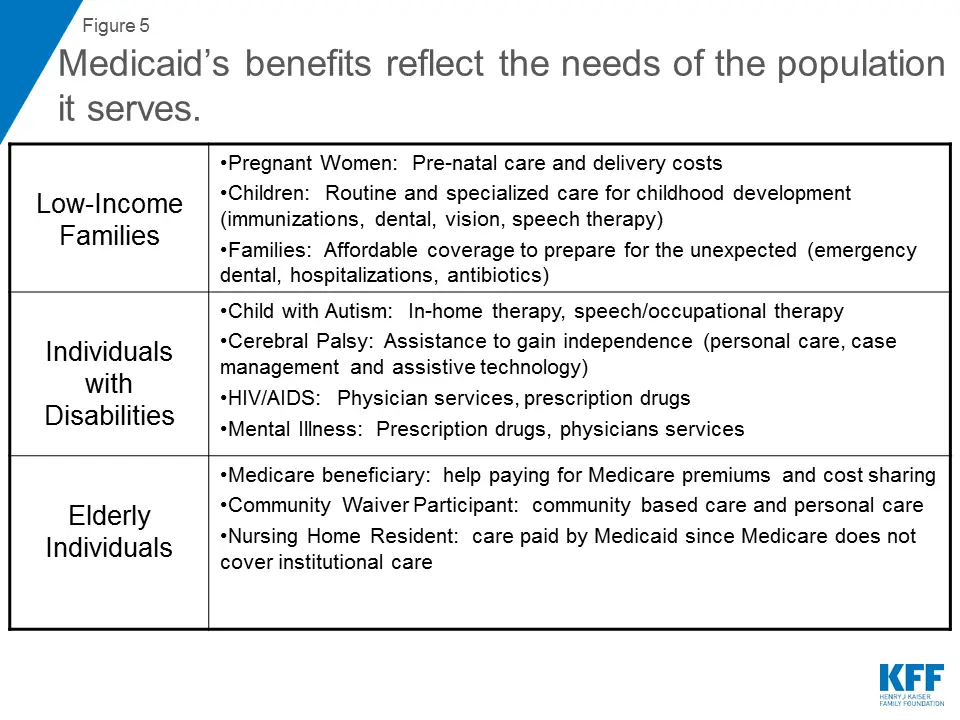
Medicaid Covers 1 In 5 Americans And Serves Diverse Populations
Medicaid provides health and long-term care for millions of Americas poorest and most vulnerable people, acting as a high risk pool for the private insurance market. In FY 2017, Medicaid covered over 75 million low-income Americans. As of February 2019, 37 states have adopted the Medicaid expansion. Data as of FY 2017 show that 12.6 million were newly eligible in the expansion group. Children account for more than four in ten of all Medicaid enrollees, and the elderly and people with disabilities account for about one in four enrollees.
Medicaid plays an especially critical role for certain populations covering: nearly half of all births in the typical state 83% of poor children 48% of children with special health care needs and 45% of nonelderly adults with disabilities and more than six in ten nursing home residents. States can opt to provide Medicaid for children with significant disabilities in higher-income families to fill gaps in private health insurance and limit out-of-pocket financial burden. Medicaid also assists nearly 1 in 5 Medicare beneficiaries with their Medicare premiums and cost-sharing and provides many of them with benefits not covered by Medicare, especially long-term care .
Figure 4: Medicaid plays a key role for selected populations.
How Do I Know If I Qualify For Nemt Reimbursement
In order for you to be reimbursed for your travel you must be on a medical assistance program that provides Medicaid travel coverage.
Travel must be to the closest medical facility or medical provider capable of providing the necessary services. The service must be a Medicaid covered service that is provided by a medical provider who is enrolled in SD Medicaid.
Don’t Miss: Select Health Medicaid Provider Portal
New York Medicaid Eligibility
New Yorkers who apply for Medicaid benefits must have income that is determined at or below poverty level. In addition, the state will consider your application if you have high medical bills or receive Supplemental Security Income.
Which Medicaid plan is best in New York?
In many cases, Medicaid will cover most of the costs of your healthcare, though in New York, the program may require you to pay co-payments for some services. You will also be required to select a Managed Care Health Plan that includes doctors in your region or offices you already visit regularly.
You can apply for New York Medicaid benefits through several state agencies.
New York Medicaid Application:
North Carolina Medicaid Eligibility
Beyond the standard financial requirement, North Carolina looks at several factors in determining whether your application for benefits will be accepted. These include family size, need for long-term care, ability level, and if you receive Medicare.
Which Medicaid plan is best in North Carolina?
North Carolina provides different levels of coverage based on the above-mentioned factors, as well as other benefits for children and pregnant women. What coverage you qualify for depends on your level of medical and financial need.
Youll need to submit an online application to the Department of Health and Human Services.
North Carolina Medicaid Application:
Read Also: Does Medicaid Cover Circumcision In Florida
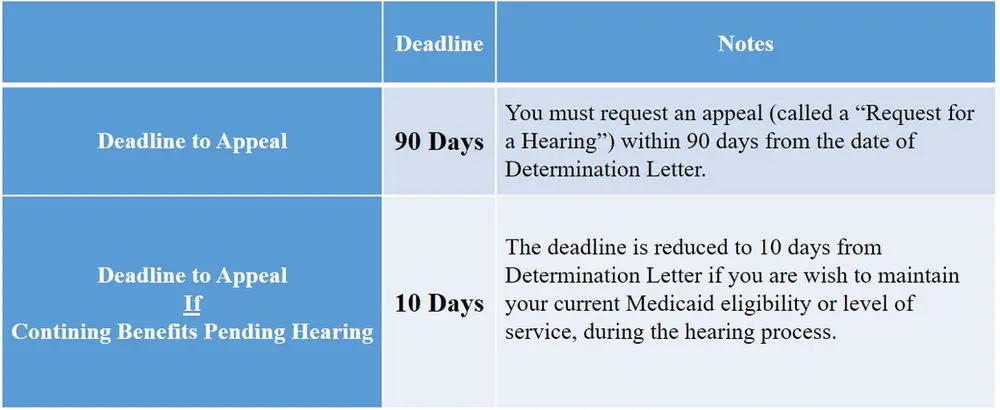
Review Your Options And Stay Covered
Losing Medicaid coverage can be very scary and shocking at first, especially if you have ongoing health issues.
If you are dealing with losing Medicaid, remember that it is not the end of the road. You have multiple options. Keep both your healthcare needs and budget in mind when making a decision about how to move forward. And if you end up at the hospital without insurance coverage, there are options even in that situation.
No matter what path you choose to follow once youre denied Medicaid or you are dropped from Medicaid, the most important thing to do is to obtain some type of coverage. The physical and financial safety that you get from having health insurance can end up being well worth any cost.
Will Medicaid Provide Payment For A Family Member Who Needs Nursing Home Care
Louisiana’s Medicaid Program provides payment for special long term care support services, as well as full Medicaid health coverage, to eligible people who, because of their medical condition, require assistance with activities of daily living . Long-term care supports may be provided either in a facility or in an individual’s own home or in the community. Visit Medicaid Long-Term Care.
Recommended Reading: How Do Elderly Qualify For Medicaid
How To Find Out If Your Medicaid Is Active
If you did not follow any of the above steps to apply for Medicaid in the past, the chances are that you dont have an account in the first place. And in your case, you would need to register from scratch.
However, if you applied for healthcare coverage via your state Medicaid agency or through the Healthcare Insurance Marketplace in the past, it is all a matter of determining whether your Medicaid is still active.
Below are the tips you can implement to find out your status.
South Carolina Medicaid Eligibility
South Carolina refers to its Medicaid program as Healthy Connections. In most cases, your eligibility is determined based on income and any assets you have available to you . Certain health situations can also make you eligible.
Which Medicaid plan is best in South Carolina?
Health Connections offers many coverage options, which are based on you or your familys particular health needs. These vary from coverage for pregnant women and infants to disabled workers and women with some cancers. After applying, youll learn what programs or coverage levels you qualify for.
You can apply for the Healthy Connections program by submitting an online application, over the phone, or in person.
South Carolina Medicaid Application:
You May Like: How To Qualify For Medicaid
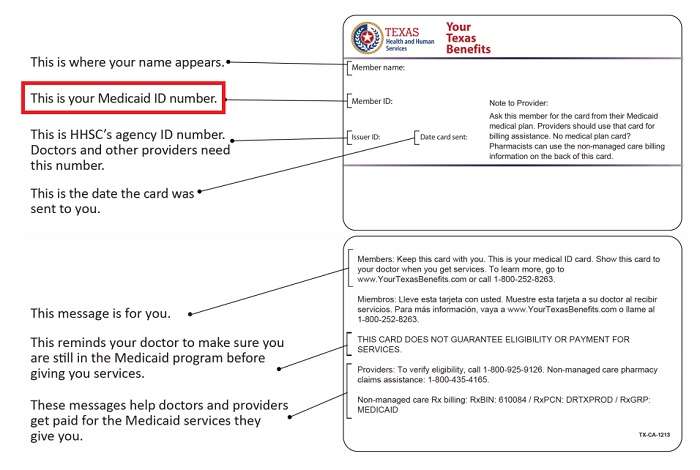
Confirming Medicaid Coverage For Beneficiaries Providers And Pharmacies Should Always Use Nctracks To Confirm Eligibility
NC Medicaid has received reports of confusion in the field by providers and pharmacies when members do not present an ID card or when presented with a Medicaid member ID card that differs from the data shown in the NCTracks system.
To mitigate any confusion associated with newly issued Medicaid Managed Care member ID cards, providers and pharmacies should always use NCTracks Recipient Eligibility Verification/Response to confirm eligibility and not rely solely on the information shown on a Member ID Card.
Health plans are required to generate an identification card for each Member enrolled in their health plan that contains the Members North Carolina Medicaid or NC Health Choice Identification number. Some health plans also include their health plan member ID as well. However, member ID cards are not required to provide service, and this includes pharmacies as well. Therefore, members should not be turned away due to the lack of a Member ID card in their possession.
Follow these steps when an NC Medicaid or NC Health Choice member presents at your office:
Additionally, the health plan will honor existing and active prior authorizations on file with the North Carolina Medicaid or NC Health Choice program for services covered by the health plan for the first 90 days after launch or until the end of the authorization period, whichever occurs first.
Important Terms For Medicaid Qualification
Modified Adjusted Gross Income is your total gross income. This includes income from employment, other benefits, child support, alimony, interest, foreign income, etc. All your income sources are included.
Federal Poverty Level is the line designated by the Department of Health and Human Services to determine who is living in poverty.
Recommended Reading: How Much Can You Make And Qualify For Medicaid
Qualifying For Different Types Of Coverage
Medicare is a federal insurance program that helps pay medical bills from a fund to which users have contributed. It covers people 65 and older, people younger than 65 with certain disabilities and patients with end-stage kidney disease and other conditions requiring dialysis. Participants usually pay part of the cost.
Medicaid is an assistance program provided jointly by federal and state agencies. It helps with medical expenses for eligible people with limited income and resources.
There are different rules for each state, but in most states, you may be eligible for Medicaid if you are under certain income levels and/or are:
- 65 and older
- A parent or adult caring for a child
- An adult with dependent children
- An eligible immigrant
Participants usually pay nothing for covered medical costs, although they may sometimes be responsible for a small copayment or cost share.
Also Check: Find A Neurologist That Takes Medicaid
Can I Get Medicaid For My Children
Yes, if your income is not too high. Medicaid and The Childrens Health Insurance Program provide low cost coverage to millions of families with children. Income requirements vary by state. In all but two states, children who live in four-person households with incomes up to $52,400 qualify for either Medicaid or CHIP. Eighteen states and DC will cover children in families of four who earn even up to $78,600, although sometimes families at the higher eligibility levels may need to pay more for the coverage.
If you have a baby while youre on Medicaid, your baby will automatically be enrolled in Medicaid for their first year.
You May Like: Is Obamacare And Medicaid The Same Thing
Also Check: Does Medicaid Cover Breast Augmentation
