Does Iowa Help With My Medicare Premiums
Many Medicare beneficiaries who struggle to afford the cost of Medicare coverage are eligible for help through a Medicare Savings Program . This program pays for Medicare Part B premiums, Medicare Part A and B cost-sharing, and in some cases Part A premiums.
- Qualified Medicare Beneficiary : QMB pays for Part A and B cost sharing as well as Part B premiums. QMB will also pay Part A premiums if a beneficiary owes them. The income limits for QMB are $1,083 a month if single or $1,457 a month if married.
- Specified Low-income Medicare Beneficiary : SLMB pays for Part B premiums. The income limit for SLMB is up to $1,296 a month if single or $1,744 a month if married.
- Expanded Specified Low-income Medicare Beneficiary : E-SLMB pays for Part B premiums for beneficiaries with income up to $1,456 a month if single or $1,960 a month if married.
- Qualified Disabled Working Persons : QDWP pays Part A premiums owed by certain disabled beneficiaries who have returned to work. Few beneficiaries enroll in QDWP due to other Medicaid benefits available to disabled workers. The income limit is $2,126 a month if living alone and $2,873 a month if living with one other person.
MSP asset limits: Iowa uses the federal asset limits for QMB, SLMB and QI: $7,860 if single and $11,800 if married. The QDWI asset limit is $4,000 if single and $6,000 if living with others.
How Do I Apply For Medicaid For My Child
In Iowa, Medicaid funding is administered by managed care organizations however the Department of Human Services determines eligibility and manages applications. You can apply for any program for your child by visiting your local DHS office. You can find the nearest office by visiting the DHS website.
If you have any questions while you are completing the Medicaid application, you can call the DHS Help Center at .
You May Like: What Is The Difference Between Medicare & Medicaid
Where Can Medicare Beneficiaries Get Help In Iowa
Iowas SHIP-SMP
Free-of-charge Medicare enrollment help and counseling is available by contacting Iowas SHIP-SMP at 1-800-351-4664. This is the States Health Insurance Assistance Program. The programs website lists the SHIP-SMP offices in each county.
Elder Law Attorneys
Elder law attorneys can assist individuals in accessing Medicaid long-term care benefits. Search for a local elder care attorney on the National Academy of Elder Law Attorneys website.
Area Agencies on Aging
Iowas Area Agencies on Aging provide information and services about the assistance programs available to older adults and people with disabilities.
You May Like: Dentists In Grand Island Ne That Accept Medicaid
Iowa Medicaid Asset Limits 2019
Individuals in Iowa are allowed to keep $2,000 when they apply to Medicaid for long term care. If they are over this amount, they must spend down on care. It is important to note, that individuals are not allowed to give gifts of any amount for a period of 5 years prior to applying to Medicaid. If an individualâs assets are more than $2,000, they should learn about Medicaid Planning strategies. This asset limit only applies to assets that are considered countable assets. Some examples of countable assets include savings accounts, bank accounts, retirement accounts and a second home. If you have multiple assets and are looking to access Medicaid, it may make sense to speak with a Medicaid Planner or Elder Law attorney in Iowa.
Couples that both require Medicaid for long term care in Iowa are allowed to keep $3,000 in assets. If there is one spouse that requires care, and one that does not, the spouse that does not receive care is referred to as the Community Spouse. The Community spouse is allowed to keep 50% of their assets up to $123,600 in countable assets which is known as the Community Spouse Resource Allowance. The Community Spouse is allowed to keep 100% of their marital assets up to $24,720 .
Also Check: How To Obtain Medicaid In Florida
Medicaid For Kids With Special Needs
Medicaid for Kids with Special Needs is a special kind of Medicaid for children with special needs due to a disability . A child may often qualify for MKSN while they are on the waiting list for a waiver however a child does not have to be on a waiver waiting list to qualify. It is based on the number of people who live in your home and your monthly income.
To qualify for MKSN you child must be:
- Under the age of 19
- Income Eligible. Your family income must be no more than 300 percent of the federal poverty level of your family size.
- A U.S. citizen.
Medicaid for Kids with Special Needs gives the same Medicaid insurance coverage you will have while on a waiver. You can apply at your local DHS office or by calling .
Read Also: Nys Medicaid Rate Private Duty Nursing
If The Medicaid Applicant Is Married
For Medicaid applicants for long-term care who are married, the healthy spouse is referred to as the community spouse.
The income of the healthy spouse living in the community is not counted in determining the applicants eligibility.
Only income in the applicants name is counted in determining his or her eligibility.
Therefore, even if the community spouse is still working and earning income, he or she will not have to contribute to the cost of caring for his or her spouse in a nursing home if the spouse is covered by Medicaid.
Unitedhealthcare Plan Of The River Valley Inc
UnitedHealthcare has three plans for Iowa Medicaid recipients. The UnitedHealthcare Dual Complete HMO SNP is for people who have both Medicare and Medicaid, the UnitedHealthcare Community Plan Hawki is for those under 19, and the UnitedHealthcare Community Plan IA Health Link is for adults and families. Aside from the great health benefits these plans provide, the IA Health Link plan includes:
- Text4baby health and safety tips for expecting new mothers
You May Like: How Much Does It Cost For Medicaid
How Medicaid Spend Down Program Works
Some applicants for Medicaid have too much income and/or assets to qualify for benefits initially, but they also do not have enough money to pay for the care they need out of pocket without eventually running out of money.
Under rules established by the federal government, states have the option to establish a medically needy program for individuals with significant health needs whose income is too high to otherwise qualify for benefits under other eligibility groups.
Under this program, most states allow individuals to spend down their excess income on their care until they reach the states income limit.
They can spend down their excess income on eligible medical expenses, which may include Medicare premiums, to a predetermined amount in order to qualify for benefits.
Essentially, this is called the medically needy pathway to Medicaid eligibility.
Therefore, if your state has implemented a medically needy pathway to Medicaid eligibility, heres what you need to know:
Your medical costs can be taken into account when determining whether your income makes you eligible for Medicaid.
Medicaid Payment For Nursing Home Care
Many people rely on Medicaid, also known as Title 19, to pay for their nursing home care or in-home services under the Medicaid Elderly Waiver program. Medicaid is a needs-based program for people who cannot afford the care they need. The financial eligibility rules for nursing home Medicaid and the Elderly Waiver are the same. In general, people are financially eligible for Medicaid for nursing home care if their income in 2021 is $2,382 or less per month and their nonexempt resources are $2,000 or less. In some instances, people with incomes above $2,382 per month may be eligible for Medicaid if they can establish a medical assistance income trust, also known as a Miller Trust. All non-exempt resources count toward the $2,000 limit. Exempt resources that do not affect your eligibility include a car, homestead, household goods, and prepaid funeral plans.
Medicaid eligibility is much more complicated for married people. The Medicaid program allowsthe spouse who lives outside of the nursing home to have more than $2,000 in resources withoutdisqualifying the spouse who lives in the nursing home from receiving Medicaid. The community spouses income does not count toward the $2,382 income limit. In addition, if the community spouses monthly income is less than $3,260 then part or nearly all the income from the spouse in the nursing home may be kept by the community spouse.
Recommended Reading: How To Apply For Pregnancy Medicaid In Nc
Medicaid Eligibility Income Chart By State Updated Jul 2022
The table below shows Medicaids monthly income limits by state for seniors. Income is not the only eligibility factor for Medicaid long term care there is also an asset limit and level of care requirements. Additionally, there are state-specific details. Click on the state name below to see that states complete Medicaid eligibility criteria.
The maximum income limits change dependent on the marital status of the applicant, whether a spouse is also applying for Medicaid, and the type of Medicaid for which they are applying. Nursing home Medicaid may have a different income limit than home and community based Medicaid services, and both of those may differ from the Aged, Blind and Disabled income limits.
Exceeding the income limits does not mean an individual cannot qualify for Medicaid. Most states have multiple pathways to Medicaid eligibility, such as a medically needy pathway. Furthermore, many states allow the use of Miller Trusts or Qualified Income Trusts to help person who cannot afford their care costs to become Medicaid eligible. There are also Medicaid planning professionals that employ other complicated techniques to help persons become eligible. Finally, candidates can take advantage of spousal protection laws that allow income to be allocated to a non-applicant spouse.
| Medicaid Eligibility Income Chart Updated July 2022 |
| State |
How To Apply For Medicaid
Enter your zip code to get started.
There are three corresponding programs that provide you Medicaid services: Medicaid Fee for Service , Healthy and Well Kids in Iowa and IA Health link. Each one of these programs continues to provide health care services to a certain group of people and it covers kids under age 1, children from age 1 to 6, children from 6 to 18 years old, pregnant women, aged, blind and people with certain disabilities. The State of Iowa also provides health care benefits to American Indians and Alaskan Natives. To read more about the programs available, click here.
Hawk-I is a program that specifically provides health care programs for the kids and children under age 18. To get your kid covered, low-income families can pay as low as $40/month or don’t play at all. To get the complete details about the Hawk-I, you can click here.
Recommended Reading: What Does Anthem Medicaid Cover
What Does Iowa Medicaid Cover
Iowa Medicaid is designed with three main coverage groups: IA Health Link, Medicaid Fee-for-Service and HAWKI. Most Iowa Medicaid beneficiaries participate in the IA Health Link managed care program, where they access medical services from a large network of providers of their choice across the state.
The Iowa Health and Wellness Plan is offered under the IA Health Link program and provides comprehensive medical care at low or no cost to residents between the ages of 19 and 64. Eligibility is based on household income. All Iowa Health and Wellness Plan members receive medical care for free if they choose to participate in the Healthy Behaviors program. Some beneficiaries are served through the Medicaid Fee-for-Service system where their medical care providers are paid separately for each treatment, such as a doctors visit, test or procedure.
Children in Iowa receive health care from the Childrens Health Insurance Program also known as the Healthy and Well Kids in Iowa Program . Iowa provides comprehensive health coverage for uninsured children of working families who cannot afford medically necessary care.
No family in Iowa pays more than $40 a month for the service, and many families pay zero. Most of the applicants who qualify for HAWKI program in Iowa are in one of these groups:
Prescription Coverage And The Pdl
The IA Medicaid program covers most prescription drugs . Your doctor is expected to always select generic prescriptions from the prescription drug list. If for some reason a generic version is not available, or if your doctor prefers another drug, he or she will need to get prior approval from the Medicaid program before issuing the prescription.
You May Like: Florida Medicaid Waiver For Developmental Disability
Income Limits In Iowa For Medicaid
In Iowa the individual receiving Medicaid cannot have income over $2,250. If their income is over that amount, they will need to do some Medicaid Planning to create eligibility. One strategy that works well is a Miller Trust . If an individual is married, the spouse’s income does not typically count towards the income cap, but it is important to maximize income protection via the Monthly Needs Allowance rules. The maximum amount of income the Medicaid office allows a community spouse to keep in Iowa is $3,090. All of an individual’s monthly income must go towards their cost of care, which can include medical bills, prescriptions and other health care costs, aside from $50 which is for a personal needs allowance. The income limits are based as a percentage of the Supplemental Security Income defined by the Social Security Administration’s Federal Poverty Levels and change every year.
Meeting Program Income Requirements
In order to receive help from many services offered by community action, you have to meet income requirements, based on the Federal Poverty Level. The requirement level for each program may be different. Look at the chart below to get an idea of what your income eligibility may be. Your local Community Action Agency will work with you to determine your eligibility for various programs and services. Find your local agency.
Donât Miss: Who Gets Medicaid In Florida
Read Also: Does Nc Medicaid Cover Chiropractic
What Is The Iowa Medicaid Program
Iowa Medicaid is offering its Health Home program for Medicaid recipients with particular chronic diseases.
Members must have one chronic condition and be at risk for a second condition, such as high blood pressure, being overweight, having heart disease, having diabetes, having asthma, abusing drugs, or having mental health issues.
Children At Home Program
The Children at Home Program is a program that can help you and your family receive services and supports you think are necessary in helping your child remain at home. It also can help you receive the services and supports that are not available in other programs.
Eligibility for the Children at Home Program is for families who meet all of the following conditions:
- The family resides in Iowa
- The family includes an individual with a disability, which is defined as an individual who is less than 22 years of age and meets the definition of a developmental disability
- The family expresses an intent for the individual with a disability to remain living in the familys home
- The familys net taxable income is the most recently completed tax year is less than $60,000
If you have any questions about this program or want to apply for assistance, please contact the Iowa Family Support Network.
Read Also: Can Someone Have Both Medicare And Medicaid
Who Is Eligible For The Iowa Medicaid Program
Medicaid is a system of income-based health insurance. You must meet particular eligibility standards and a minimum income level to be eligible for Medicaid coverage. A few of these fundamental requirements are as follows:
- A young person under 21
- A parent who shares a home with a minor
- An expectant mother
- A female patient in need of therapy for cervical or breast cancer
- An elderly individual
- A person who meets the criteria for disability as defined by Social Security
- A person aged 19 to 64 with an annual income of less than 133 percent of the federal poverty level
- A citizen of the United States and a resident of Iowa
You must fall under one of the following thresholds for household income to qualify:
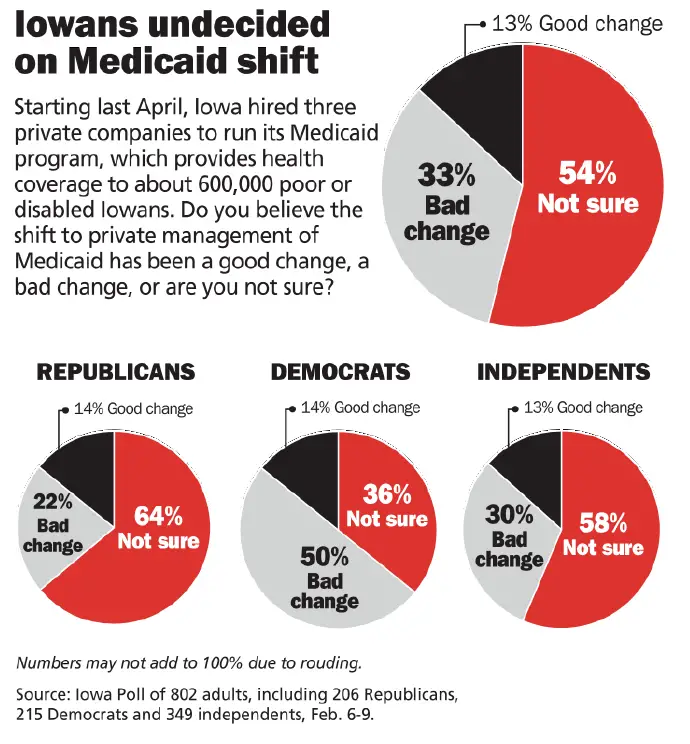
Medicaid Eligibility Expansion In Iowa Without A Waiver But With Managed Care
In July 2015, Iowa officials announced that they were abandoning their Medicaid demonstration waiver, and would instead implement Medicaid expansion as called for in the ACA, but with a Medicaid Modernization managed care waiver instead, switching Iowa Medicaid enrollees to a Medicaid managed care system .
560,000 Iowa Medicaid beneficiaries were scheduled to transition to the Medicaid managed care system as of January 1, 2016. The Medicaid enrollees were supposed to select a managed care program by mid-December, but many enrollees were having trouble determining which managed care programs included their doctors and hospitals. As a result, the federal government delayed Iowas switch to Medicaid managed care until March 1, 2016. The federal government ultimately gave the go-ahead for the switch on February 23, but added an extra month to allow enrollees, MCO carriers, and providers time to make the change. The Medicaid managed care system in Iowa took effect April 1, 2016.
Eligibility for coverage under Iowas Medicaid expansion was unchanged Medicaid coverage continued to be available to Iowa residents with household income up to 138% of the poverty level. But enrollees with incomes between 101% and 138% of the poverty level were no longer enrolled in private exchange plans as of 2016. Instead, they are enrolled in a private Medicaid managed care program, just like the rest of the Medicaid population in Iowa.
Also Check: Is Invisalign Covered By Medicaid
