Is There Really A $16728 Social Security Bonus
The $16,728 Social Security bonus most retirees completely overlook: If youre like most Americans, youre a few years behind on your retirement savings. Once you learn how to maximize your Social Security benefits, we think you could retire confidently with the peace of mind were all after.4 days ago.
Medicare And Medicaid Reimbursement Rates
Medicaid and Medicare have extensive bargaining power with medical doctors.
Huge discounts can be negotiated for the services received by their clients. That is possible due to the volume of patients covered. It is essentially a mass volume discount that helps them create revenue.
If an individual might get charged $10,000 for the medical procedure, the Medicare reimbursement rate might only be $500. That means the other $9,500 gets written off by the scheme.
It is important to note that the jury may not be told the discount medical bill price under Iowa law. The medical expense often influences how the jury or judge awards for pain and suffering. If they hear that medical damages were only $500, they are more likely to award commensurate damages to the value of $500. That can be detrimental to a person expecting the $10,000 in medical to be paid out.
A personal injury lawyer from Tom Fowler Law can help to bring the claim to court. They can also assist in determining the compensation owed. Unfortunately cost prohibition can occur for legitimate claims because people can easily spend $5,000 to bring the case to court.
How Much Will Medicaid Cost Me
It depends. Every state is different. You will probably not have to pay a monthly premium for Medicaid, but most people do have some out-of-pocket costs.2 Emergency services, family-planning services, pregnancy-related services and preventive care for children are all fully covered with no additional cost to you.
Don’t Miss: Difference Between Medicare And Medicaid Reimbursement
Medicaid Covers 1 In 5 Americans And Serves Diverse Populations
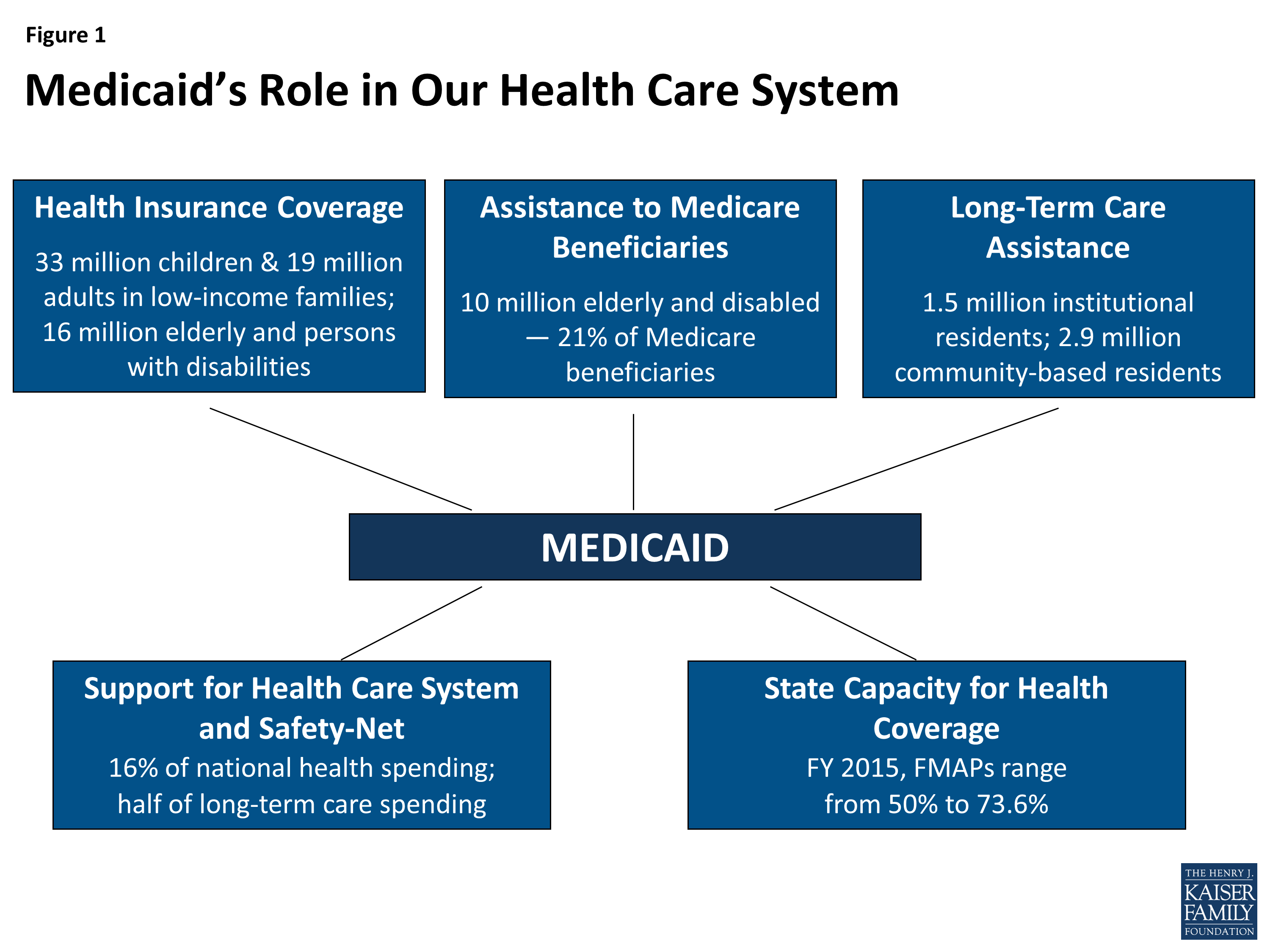
Medicaid provides health and long-term care for millions of Americas poorest and most vulnerable people, acting as a high risk pool for the private insurance market. In FY 2017, Medicaid covered over 75 million low-income Americans. As of February 2019, 37 states have adopted the Medicaid expansion. Data as of FY 2017 show that 12.6 million were newly eligible in the expansion group. Children account for more than four in ten of all Medicaid enrollees, and the elderly and people with disabilities account for about one in four enrollees.
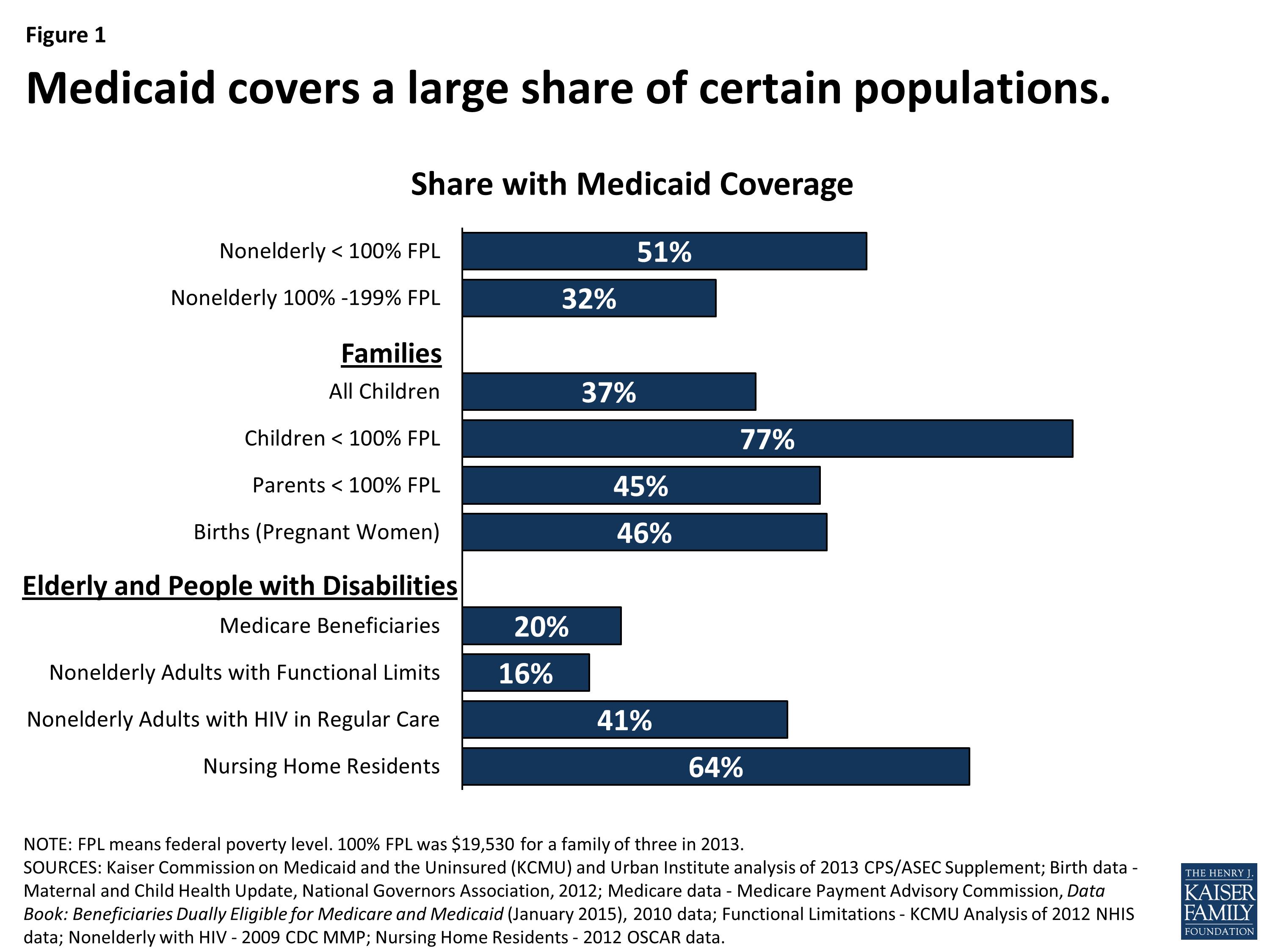
Medicaid plays an especially critical role for certain populations covering: nearly half of all births in the typical state 83% of poor children 48% of children with special health care needs and 45% of nonelderly adults with disabilities and more than six in ten nursing home residents. States can opt to provide Medicaid for children with significant disabilities in higher-income families to fill gaps in private health insurance and limit out-of-pocket financial burden. Medicaid also assists nearly 1 in 5 Medicare beneficiaries with their Medicare premiums and cost-sharing and provides many of them with benefits not covered by Medicare, especially long-term care .
Figure 4: Medicaid plays a key role for selected populations.
Enhanced Federal Medical Assistance Percentages

Enhanced matching rates are similar to FMAP but are taken one step further. They increase the percentage of costs paid by the federal government for certain services. The minimum enhanced FMAP for Fiscal Year 2020 is 76.50. The services covered by enhanced matching rates include but are not limited to:
The Affordable Care Act increased the enhanced FMAP for states from October 1, 2015 through September 30, 2019. It did so by 23 percentage points but did not allow any state to exceed 100%. For Fiscal Year 2020, the enhanced matching rates will be lower. The Healthy Kids Act will allow an increase in the enhanced FMAP by 11.5%, again not to exceed 100% total.
The services covered by enhanced matching rates are seen as valuable because they may help to decrease the burden of healthcare costs in the future. In that way, paying more money upfront is seen as a worthy investment.
Don’t Miss: Dentist In Meridian Ms That Accept Medicaid
How Much Does Medicare Part D Cost In 2022
Medicare Part D is prescription drug coverage. It is provided by Medicare-approved private insurers.
Premium costs vary by plan, state and income, but the average basic monthly premium for a Medicare Part D plan in 2020 was about $43, according to data from the CMS compiled by Policygenius. High-income Medicare beneficiaries are subject to an income-related monthly adjustment amount , meaning if you make more, youll pay more. For 2022 plans, the additional costs will be based on your 2020 income.
Getting Medicare Part D requires enrolling in Original Medicare, so youll pay any of those premiums, too.
The deductibles vary, but no Medicare Part D plan can have a deductible higher than $480 in 2022, up from $445 in 2021.
Copays and coinsurance vary by plan and tier and whether youve hit the Medicare Part D coverage gap, or donut hole. After the insurer has covered a certain amount on prescriptions, they will temporarily limit how much your plan will help pay for prescriptions.
Learn more about Medicare Part D plans and the donut hole here.
What Is The Lowest Income To Qualify For Medicaid
There are 13 states that do not grant Medicaid access to individuals based on income alone.
Of those that do, only Wisconsin uses a limit lower than 138%. An individual in Wisconsin can make no more than the federal poverty level in order to qualify for Medicaid.
Texas has the lowest income limit to qualify on a family basis, at 17% of the FPL. A two-parent household with one child in Texas can make no more than $37,332 and qualify for Medicaid.
Also Check: How To Get Medicaid For Mental Illness
How Can I Lower Medicare Costs
The Medicare Savings Program helps low-income beneficiaries pay Original Medicare premiums, copays, and deductibles. The Medicare Extra Help program assists low-income beneficiaries with prescription drug coverage.
Some Medicare beneficiaries are also eligible for Medicaid, the federal-and-state-funded health insurance program for low-income Americans. Eligibility varies by state you can see our state-by-state guide to Medicaid here to find out if youre eligible, and read more about Medicare vs Medicaid.
Beyond that, cost-saving comes down to finding the best plan and program structure for you. Some people may be looking for different Medicare benefits and more robust coverage than others. As weve discussed, these elections and their costs will vary, depending on whats offered by your state and your income level.
Senior Editor & Disability Insurance Expert
Elissa Suh is a disability insurance expert and a former senior editor at Policygenius, where she also covered wills, trusts, and advance planning. Her work has appeared in MarketWatch, CNBC, PBS, Inverse, The Philadelphia Inquirer, and more.
Questions about this page? Email us at .
32 Old Slip, 30th Fl New York, NY 10005
Check Your States Rules
Check and learn your states requirements concerning maximum assets permitted for Medicaid eligibility.
For more information, contact us at Gentreo.com. We can help you create a simple and affordable health and estate plan, and a safe place to store it.
ww.gentreo.com
Gentreo is not a law firm or a substitute for a law firm, or attorney, or an attorneys advice or recommendations.
Don’t Miss: Moving To Another State Medicaid
How Much Funding Am I Required To Put In A Miller Trust
Typically, there are two primary ways in which you would put your income into a Miller Trust, as well as how much:
- Single applicants must use all of their income to pay their care facility as part of their patient responsibilities.
- Someone who is married and still has a spouse at home will need to divert only a portion of their income to their Miller Trust. The amount will depend on the spouses income.
Essentially, the money you put into your Miller Trust will cover your the costs of your personal care and then ultimately go to the nursing home for a single person. For those who are married, income rules somewhat differ depending on their circumstances.
Read Also: Does New York Presbyterian Hospital Accept Medicaid
Is All Of My Income Taken Into Account When Determining 250% Of The Federal Poverty Level For This Medi
No. This program uses Social Securityâs countable income calculation to determine your income. Additionally, the WDP Program does not count unearned income from private or public disability benefits when determining your countable income.
Important: Medi-Calâs deeming rules apply when a worker has combined household income, for example income from a spouse.
Read Also: How To Apply For Children’s Medicaid In Texas
Often Asked: How Much Money Can You Have In The Bank To Qualify For Medicare
Specified Low-Income Medicare Beneficiary Program A single person can qualify in 2021 with an income up to $1,308 per month. A couple can qualify with a combined income of $1,762 per month. The asset limits are $7,970 for an individual and $11,960 for a couple.
How much money can you have and still get Medicare?
- However, the house you live in and up to one car you own are not counted as assets when it comes to qualifying for a Medicare Savings Program. How much money can you have and still get Medicare? To qualify, your monthly income cannot be higher than $1,357 for an individual or $1,823 for a married couple.
Read Also: Where To Get Braces With Medicaid
Is Repayment Of A Past Medical Lien Required
Anytime Medicaid or Medicare has paid for medical benefits. There is an obligation on both the attorney and client to repay the fees. Of course, the money needs to be recovered from a negligent third party to pay back any expenses.
It is imperative to note that there is no difference between what the settlement money was paid for. An example of this is pain and suffering vs. medical bills. The entire settlement is on the line and the person should protect the settlement.
If they fail to repay Medicare, the government can sue the lawyers for interest plus double damages. That is due to the lawyer knowingly ignoring the lien. The Medicaid lien laws vary in different states, be sure the state can sue the lawyer and client for the interest plus the lien amount.
A requirement from Medicare is that a form is completed and notify them on every personal injury case to check for unpaid medical bills. Any prudent auto accident attorney Des Moines provides handling a case must confirm steps and consider any Medicare liens.
Also Check: How To Change Medicaid Plan Pa
Is There An Asset Limit For Medicare
In 2021, the asset limits for full Extra Help are $9,470 for individuals and $14,960 for couples. This means that you could be eligible for an MSP with assets totaling $7,970 for individuals and $11,960 for couples. MSP limits appear lower than Extra Help limits because they do not automatically include burial funds.
How Do I Apply For Medi
There are different ways to apply for Medi-Cal:
- Online using BenefitsCal. BenefitsCal lets you apply for other programs like CalFresh or CalWORKs at the same time.
- Online using Covered California, an online one-stop shop where you can learn about your public and private coverage options.
- Using a paper application and mailing it in to your local county social services agency.
Note: If you get Supplemental Security Income or used to and now are on SSI 1619, you automatically get Medi-Cal coverage. You do not need to apply for Medi-Cal.
Also Check: Does Medicaid Cover Paragard Iud
Don’t Miss: Emergency Clinics That Take Medicaid
Can Medicaid Take Your Personal Belongings
Elder Law Guides
Most peoples furniture has little or no financial value so it is not considered in determining eligibility for Medicaid. In fact, personal belongings are explicitly excluded as assets for purposes of Medicaid asset limitations, so it can be argued that their transfer cant be penalized.
How Much Money Can A Medicaid Recipient Have In The Bank
Attorney Thomas B. Burton answers the following question:
“How Much Money Can a Medicaid Recipient Have in the Bank?”
Want to know how to protect your home from the nursing home? Download a free copy of my 5 Step Guide on How to Protect Your Home from the Nursing Home Guide!
Subscribe to Burton Law LLCs channel to get notified when we post new videos.
Hello, I’m attorney Thomas Burton and today’s question is the following:
How much money can a Medicaid recipient have in the bank?
So this is a good question, one I see come up frequently. The short answer is you can have no more than $2000 in liquid assets in total and all your bank accounts, when you submit the Medicaid application in order to qualify for Medicaid. Now that’s for a single individual. If you’re married the community spouse can keep a certain amount of assets and that’s going to depend on your total amount of assets.
So work with your attorney to figure out that number but if you’re single person, the answer is it has to be $2000 or less, and for that reason, I don’t recommend you have exactly $2000 in the bank when you submit that Medicaid application. You want to have under that amount because if you’re over it even by $1, you would not qualify to receive Medicaid assistance.
Now one other thing to note, I touched on the house, if you want to have the house, the house won’t stop you from applying for Medicaid but later they will seek estate recovery from the house if it’s in your individual name.
Recommended Reading: State Of Michigan Medicaid Phone Number
Des Virtual Office Services
On April 10, 2020, DES is implementing virtual office services in all locations to continue to better serve our customers and communities in this time of need while protecting the health and safety of our customers and staff. The Department is now directing individuals towards ways to access services virtually, through online options or telephones to the greatest extent possible, and limiting public traffic in lobbies and field offices per CDC public health guidance. Learn more:
Arizona Health Care Cost Containment System is Arizonaâs Medicaid agency that offers health care programs to serve Arizona residents. AHCCCS provides medical insurance coverage to thousands of Arizonans each year. It helps citizens obtain doctors office visits, physical exams, immunizations, prenatal care, hospital care and prescriptions they need.
AHCCCS offers many different medical programs. DES only determines eligibility for the following programs:
Medicaid for adults and children with limited income.
KidsCare for uninsured children under the age of 19 who have income higher than the Medicaid limit.
Eligibility for the Medical Assistance program is based on the following requirements:
Donât Miss: Medicaid Free Cell Phone Application
Funeral And Burial Funds
Generally, Medicaid considers the value of any non-refundable pre-paid funeral plan or burial contract exempt. This includes irrevocable funeral trusts in most states. IFT limits vary, but the cap is typically $15,000 or less per spouse. For example, Nebraska sets a max value of $5,372, whereas New York and Michigan are the only two states that do not consider IFTs of any value exempt for Medicaid purposes. Some states also allow applicants to set aside up to $1,500 in an irrevocable pre-need funeral arrangement and/or a revocable burial fund that is considered an exempt asset.
Read Also: Does Medicaid Pay For Over The Counter Medicine
Also Check: Find Primary Care Doctor Medicaid
Medicaids Benefits For Assisted Living Facility Residents
Assisted living facilities are a housing option for people who can still live independently but who need some assistance. Costs can range from $2,000 to more than $6,000 a month, depending on location. Medicare wont pay for this type of care, but Medicaid might. Almost all state Medicaid programs will cover at least some assisted living costs for eligible residents.
Unlike with nursing home stays, there is no requirement that Medicaid pay for assisted living, and no state Medicaid program can pay directly for a Medicaid recipients room and board in an assisted living facility. But with assisted living costs roughly half those of a semi-private nursing home room, state officials understand that they can save money by offering financial assistance to elderly individuals who are trying to stay out of nursing homes.
Local Elder Law Attorneys in Your City
City, State
As of 2019, 44 states and the District of Columbia provided some level of financial assistance to individuals in assisted living, according to the website Paying for Senior Care, which features a State by State Guide to Medicaid Coverage for Assisted Living Benefits that gives details on each states programs. According to the website, the Medicaid programs of Alabama, Kentucky, Louisiana, Maine, Pennsylvania, and Virginia are the only ones that provide no coverage of assisted living, although non-Medicaid assistance may be available.
Talk With A Senior Living Advisor
Our advisors help 300,000 families each year find the right senior care for their loved ones.
- Respite care and other in-home long term care
- Personal care services
Medicaid also may help cover costs if you cant pay the Medicare co-pay for days 21-100 during a hospitalization, or if you cant pay for long-term care in the skilled nursing facility after rehabilitation is complete.
Also Check: How Do I Get Proof Of Medicaid
Receiving An Inheritance And Medicaid Preservation
Medicaid recipients must constantly maintain assets below $2,000.00. If their assets ever exceed $2,000 at the end of any calendar month, they will no longer be Medicaid-eligible. So, when someone receives a lump sum inheritance from a recently-deceased family member, the lump sum of money can be most unwelcome. This article will explain what happens when a Medicaid recipient receives an inheritance and what the person about to receive an inheritance can do to preserve their Medicaid benefits.
First of all, the time to speak with an experienced medicaid lawyer is now . This allows your medicaid-planning lawyer to provide you a well thought out plan that can be put in place before the inheritance is received to ensure that all players understand what they need to do and provide for a smooth transition and no loss of benefits.
You May Like: Neurologist In Alexandria La That Accept Medicaid
