Keeping Health Insurance After Leaving A Job
A federal law called COBRA allows you to stay on your employers health plan for 18 to 36 months after leaving a job. Youll pay both your own monthly premiums and the employers portion, so your cost is likely to be higher than before.
- People with a disability may be able to extend COBRA coverage for an extra 11 months.
- COBRA may also cover young adults who age out of a parents policy when they reach the age limit of 26.
Learn more about COBRA online or call the U.S. Department of Labor at 18664USADOL .
Ketone Urine Test Strips
- This is covered as a durable medical equipment benefit. These are limited to two 100-count boxes a month . DME items are covered with a prescription or order and a certificate of medical necessity from the primary care provider or prescribing provider when presented to a participating DME provider.
- A copay applies to members ages 19 and older. Please refer to the copayment reference guide for a list of current member copays. There is no copay for members who are pregnant or under age 19.
Medicaid And Cgm: Who’s Covered
Karena Yan
Continuous glucose monitoring coverage varies widely by state Medicaid program check out our guide on whos covered and where
In California, a staggering 25% of the population is covered under Medi-Cal and the Childrens Health Insurance Program , which are programs for low-income Americans supported by federal and state governments. We estimate that at least half of these beneficiaries have diabetes, prediabetes, or undiagnosed diabetes. For these individuals, coverage of diabetes drugs and technology dramatically increases their chances of living a life free of complications. Despite this, however, continuous glucose monitors are not covered by Medi-Cal. Moreover, while CGMs are covered under California Childrens Services , a state program for children with certain diseases or health problems, this is limited only to children with multiple co-morbidities and children who are disabled.
CGM is already covered by most private insurance and recently became covered under Part B of Medicare, a federal health insurance program that covers those who are 65 or older or who are disabled. The importance of providing CGM to those who will benefit from it is clearly understood, as acknowledged by Medicares choice to provide coverage. It seems clear that these benefits should be made available to low-income individuals on Medicaid, and many in the advocacy community are working to ensure progress is made on this front.
Recommended Reading: Illinois Nursing Homes That Accept Medicaid
Finding Approved Pharmacies And Suppliers
For supplies to be covered, Medicare requires you to get supplies from participating providers that accept assignment. This means they accept Medicare set payment rates.
If you use a provider that doesnt accept assignment, you will be responsible for all costs. The provider may charge a higher rate than the Medicare accepted rate.
Many supplies such as needles, lancets, and test strips are available at participating pharmacies. Some pharmacies also carry CGMs. You can check with your preferred pharmacy about what supplies they carry and if they accept assignment.
Some diabetic equipment, nutritional therapy, and shoe inserts/special footwear are available through durable medical equipment providers. Youll need prescriptions from your doctor for all supplies and equipment.
Diabetes is a condition in which blood sugar levels are high because the body either doesnt produce enough insulin or doesnt use/produce the insulin effectively , or develops temporary insulin resistance during pregnancy.
Type 2 diabetes is the most common form. Of the 30 million Americans with diabetes, 90 percent have type 2. Twentyfour million people 65 and older have prediabetes .
Risk factors for diabetes can be different for each type, but family history, age, race, and environmental factors may all impact the condition.
Its important to follow your doctors guidance on medications, blood sugar testing, lifestyle, and diet management.
How Does Medicare Cover Diabetes

Different parts of Medicare cover different services and supplies. That said, some things arent covered by Medicare, and in many cases, you will pay a portion of the cost, unless you have another insurance plan that covers it.
Medicare coverage for diabetes would usually be obtained by enrolling in Original Medicare or a Medicare Advantage plan .2
Recommended Reading: Paramount Medicaid Ohio Phone Number
How Does Medicare Part D Cover Diabetes
Medicare Part D is prescription drug coverage. If you joined a Medicare drug plan, youre covered for the following:5
- Insulin: This includes injectable insulin not used with an insulin infusion pump and inhaled insulin.
- Anti-diabetic drugs: Medicare drug plans can cover anti-diabetic drugs to help blood sugar when not controlled by other measures.
- Diabetes supplies: The supplies you use when you inject or inhale insulin may be covered, including syringes, needles, alcohol swabs, gauze and inhaled insulin devices.
The Best Diabetic Supply Companies Of 2022
- Best for Medicare and Medicaid Insurance: Edgepark
- Best Support for Medtronic Users: Medtronic
- Best for Specialized Insulin Pump & Technology: Tandem
- Best for Pediatric Population: Insulet
- Best for Replacements: Dexcom
-
Will review all your insurance options to help save money
-
May not be available to all types of Medicare plans
-
Pump users may be locked into warranties
Why we chose it: Many health professionals and people living with diabetes recommended Byram Healthcare to us for diabetes supplies. Its deliveries are very reliable and because it offers so many products, it may serve as a one-stop-shop for diabetes supplies. Priding itself on convenience, affordability, and choice, Byram Healthcare offers a comprehensive product line of diabetes supplies ranging from diabetes test strips, lancing devices, lancets, control solution, batteries, blood glucose meters, insulin pump supplies, continuous glucose monitor supplies, insulin and pen needles, and more.
Read Also: Does Medicare Or Medicaid Cover Cremation
How Does Medicare Advantage Cover Diabetes
If you have Medicare Advantage, your plan must give you at least the same coverage as Parts A, B and D but there may be different rules. You may have different rights, protections and choices for where to get your care. You may even get extra benefits. For more information on coverage, read your plan materials or contact your plan for information.
There are also Medicare Special Needs plans ,6 which are a type of Medicare Advantage plan that limits membership to people with a specific disease, such as diabetes. Medicare SNPs design their benefits, provider choices, and drug formularies to meet the needs of the group they serve.
Does Medicare Cover Diabetic Supplies
- Medicare Part B covers certain diabetic supplies and preventive screenings.
- Medicare Part D covers oral diabetic medications, injectable insulin, and self-injection supplies.
- Get prescriptions from your doctor for any medication, supply, or service youll want Medicare to cover.
- Check that your pharmacy or device supplier accepts Medicareset payment rates to avoid overpaying.
Diabetes is a metabolic condition that leads to high blood sugar levels. Most people who have diabetes have type 2 diabetes. According to the American Diabetes Association, around 14 million Americans 65 and older have diabetes, some who are undiagnosed.
Older adults with diabetes face unique challenges including hypoglycemia, brain and nervous system problems, and social support issues that require special monitoring to manage risks.
There are many types of diabetic supplies needed for preventive screening, monitoring, and managing the condition. Medicare has several parts that cover different types of supplies and services. Cost and coverage depend on the type of plan.
Also Check: How To Renew Medicaid Colorado
Medicaid And Diabetes Health
As an insurer, Medicaid is dedicated to helping people achieve their health goals. Medicaid has many programs that are geared directly toward specific diseases. The programs are specifically designed to help you with your overall treatment plan and health management. A diabetes health program usually contains information and resources regarding medications, diet, and exercise. Please check with your state run Medicaid program to find out whats available to you as a person living with diabetes.
MedicaidSupplies.com understands that diabetes is a very complex and serious disease. We strive to provide people with valuable information and resources to help make living with diabetes that much easier.
Best For Replacements: Dexcom
-
Reliable continuous glucose monitor that is compatible with many insulin pumps
-
Easy replacement forms can be filled out online
-
Youll need to have other diabetes supplies delivered from a separate company. Dexcom delivers only Dexcom supplies.
Dexcom, a type of Continuous Glucose Monitor , is used to help you check your blood sugars, identify trends, and alert you if your levels are trending high or low. Dexcom provides great flexibility in the delivery of supplies. Simply filling out a form online can determine if you are eligible for the product. And, if you have pharmacy coverage through your insurance, you can get your supplies delivered directly from your pharmacy. If you dont have pharmacy coverage, you can continue to receive supplies from Dexcom or your insurance-designated distributor.
CGM systems like Dexcom take glucose measurements at regular intervals throughout the day and translate them into information to demonstrate trends. These readings are used to help manage diabetes. A Dexcom user told us that in the instance she has a faulty sensor, she deals directly with Dexcom and has no problem getting replacements sent directly to her quickly and easily.
Recommended Reading: How Long Is A Child Eligible For Medicaid
What Do States That Cover Cgm Under Medicaid Have In Common
Medicaid expansion: All of the states that cover CGM for people with both type 1 and type 2 diabetes the states shown in green have also adopted Medicaid expansion.
Diabetes prevalence: While it might be expected that states with the highest diabetes prevalence would also have the greatest investment in diabetes tools, this does not seem to be the case. Among the sixteen states with at least twelve percent of adults with diabetes, only four states cover CGM under Medicaid for people with both type 1 and type 2 diabetes.
Medicaid spending: With the exception of IL and MA, states with the highest Medicaid spending typically do not cover CGM for people with both type 1 and type 2 diabetes. We speculate that this is because coverage for all people with diabetes requires purchasing all of the CGMs, and states may be wary of this high initial cost. However, this approach is not actually cost-effective because the cost of diabetes supplies, such as CGMs, account for only 1.1% of the total cost of diabetes, while the costs of treating complications and lost productivity both expenses that would be reduced with widespread CGM use account for 73.1% of total diabetes costs. Thus, CGMs should not be the focus of cost-cutting efforts.
Do I Qualify For These Benefits
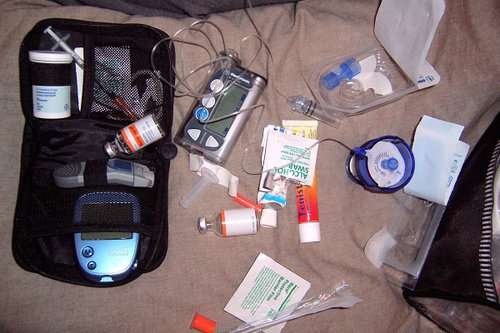
Many diabetic supplies are a covered benefit of Medicare Part B. If you are enrolled, or eligible to enroll, in original Medicare, youll receive coverage for diabetic supplies and services.
Medicare pays the majority of the cost, but you are still responsible for 20 percent. You will also pay for any coinsurance, deductible, and copayment costs.
You can buy a supplemental plan to help offset some of these costs, such as a Medigap plan. Review different plan options to find one that best meets your needs.
For Medicare to cover diabetic supplies, your doctor needs to write prescriptions that explain:
- you have received a diagnosis of diabetes
- any special devices/monitors you need and why
- for special shoes, a podiatrist or other foot specialist has to explain why you need special shoes and provide a prescription
- how often you need to test your blood sugar levels
- number of test strips and lancets you need
New prescriptions are needed each year from your doctor. If you need to monitor your blood sugar more often, your supply limits for each month will need to be increased.
Also Check: What’s The Income Level For Medicaid
Other Useful Information On Diabetic Supplies
- Generally, you pay 20% of Medicare-approved amounts for your supplies, and the Medicare Part B deductible applies.
- Make sure you refill your supplies in a timely manner, and only accept supplies you have requested. Medicare wont pay for supplies you didnt order for example, if a supplier automatically sends you items, you cannot get reimbursed by Medicare.
- You may rent or purchase certain diabetic supplies. For more information, call 1-800-MEDICARE . TTY users call 1-877-486-2048. Customer service representatives are available 24 hours a day, seven days a week.
- Ask if the supplier is a participating supplier in the Medicare program before you get durable medical equipment for diabetes. If the supplier is a participating supplier, he or she must accept assignment. If the supplier is enrolled in Medicare but isnt participating, he or she has the option to accept assignment or not. If a DME supplier doesnt accept Medicare assignment, there is no limit to what you can be charged. You also may have to pay the entire bill at the time you get the DME.
- All Medicare-enrolled pharmacies and suppliers must submit claims for diabetic testing supplies. You cant send in the claim yourself.
Find Plans in your area instantly!
What Health Insurance Plans Cover People With Diabetes
Health insurance helps pay for medical care, including the cost of diabetes care. Your health insurance options are
- private health insurance, which includes group and individual health insurance
- government health insurance, such as Medicare, Medicaid, the Childrens Health Insurance Program , TRICARE, and veterans health care programs
Under current law, health insurance companies cant refuse to cover you or charge you more just because you have a pre-existing conditionthat is, a health problem you had before the date that new health coverage starts.
Changes to insurance rules happen often and may affect your health insurance choices. Learn more or get help with your health insurance questions through
- HealthCare.gov , the federal marketplace, 1-800-318-2596, TTY: 1-855-889-4325
- copayments and deductibles
- health care providersdo your providers participate in the plan, or will you have to change providers or pay more to see your current providers because they are out of network?
Ask for a Summary of Benefits and Coverage, which explains the plan in plain language, including free preventive services. This summary may include a coverage example for managing diabetes.
Read Also: Does Medicaid Pay For Dental Crowns
Which States Have The Best Most Inclusive Medicaid Coverage Of Cgm
State policies that cover CGM through a pharmacy benefit, as opposed to a medical benefit, generally make it easier for people to obtain CGM. Currently, seven states provide CGM through a pharmacy benefit: Illinois, Maine, Ohio, New York, North Carolina, West Virginia, and Wyoming. Of these states, Illinois, Ohio, and West Virginia are the only three that also cover CGM for people with both type 1 and type 2 diabetes, making their policies the most effective and far-reaching of the fifty states.
Getting a CGM through a pharmacy benefit is typically faster, more convenient, and less expensive for the patient. While both pharmacy and medical benefits require a doctors prescription, medical benefits usually require a great deal more paperwork and documentation for the physician. Not only does this create excessive hassle for the doctor, but it also results in additional administrative processing and delays in receiving a CGM for the patient. Thus, while getting a CGM via a pharmacy benefit usually takes a matter of hours or days, it can take up to several weeks to receive one through a medical benefit.
Medicare Free* Meter Pre
6 FREE* METERS packed with every 12 boxes of 50-count CONTOUR®NEXT test strips!
PRE-PACK CONTENTS:
- 12 CONTOUR®NEXT DME Medicare/Medicaid Test Strips 50-count
- 3 CONTOUR®NEXT ONE No-Charge Meters*
- 3 CONTOUR®NEXT EZ No-Charge Meters*
For access to No Charge meters
*These products are provided for evaluation purposes only and may not be charged to any patient and the provider may not submit a claim for reimbursement to Medicare, Medicaid, or other public or private insurer for the sample product. Requires a minimum purchase of 12 boxes of CONTOUR®NEXT 50-count test strips.
Recommended Reading: Can You Get Medicaid At Age 62
How To Learn More And To Apply
Each state’s Medicaid program covers different benefits, and has different rules for eligibility. As a result of the ACA, many states calculate income to determine eligibility in a different way than they did before 2014 and some states offer Medicaid to more people now. So, if someone was previously determined ineligible for Medicaid, he or she should consider reapplying.
The Health Insurance Marketplace in each state offers a single application to determine whether a person is eligible for Medicaid or eligible for help purchasing private health insurance through the Marketplace. For more information on the Health Insurance Marketplaces, visit www.healthcare.gov or call 1-800-318-2596. See our fact sheet on the Health Insurance Marketplaces at www.diabetes.org/HealthInsuranceMarketplaces.
You can also apply for Medicaid through your state’s Medicaid office. A link to your state’s Medicaid office can be found at .
Where Can I Get Free Insulin
Over the last few years, the cost of insulin has skyrocketed. If you are struggling to pay for your insulin, three drug manufacturers may offer immediate prescription assistance: Eli Lilly, Novo Nordisk, and Sanofi. The American Diabetes Association has more information on how to access cheaper insulin through manufacturers.
Also Check: Dentist In Charleston Sc That Accept Medicaid
Get Important News & Updates
Sign up for email and/or text notices of Medicaid and other FSSA news, reminders, and other important information. When registering your email, check the category on the drop-down list to receive notices of Medicaid updates check other areas of interest on the drop-down list to receive notices for other types of FSSA updates.
