What Services Are Available Through This Program
- Physical exams which may include a pap smear, breast exam, and STD testing
- Family planning counseling and pregnancy test
- Birth control supplies including condoms
- Colposcopies and treatment for STDs which are limited to a six week period after a family planning exam, counseling visit, or supply visit
- Related pharmaceuticals and laboratory test
Please noteAll Services are CONFIDENTIAL
Will My Insurance Cover My Iud
It has been well-established that long-acting and reversible methods of contraception like IUDs and the implant are a good option for many women. They provide the most effective coverage of all available contraceptive methods available, with failure rates of less than one percent they can last up to a decade and they can be easily removed when a women decides to become pregnant. There are also significant public health implications associated with an increased use of these methods, including decreased rates of unintended pregnancy, teen births, and abortions. Clinicians and public health advocates are increasingly recognizing the benefits, and efforts are underway across Northeast Ohio to educate women about the benefits of IUDs and the implant. However, despite some growth, these methods remain underutilized. More work is necessary to increase access and to understand the challenges women face when receiving family planning services.
We decided to do some quick research to find out how a woman could identify her covered contraceptive benefits. There was good news . However, in some cases, finding the answers proved more difficult than youd think.
Can we make this easier?
Is my product covered?
Healthcare providers can play a role.
There are other significant barriers to access.
Progress has been made.
Barrier, hormonal and implant methods, as well as emergency contraception, sterilization, and patient education and counseling.
Like this post?
Ny Medicaid Ehr Incentive Program Update
The NY Medicaid Electronic Health Records Incentive Program provides financial incentives to eligible professionals and hospitals to promote the transition to EHRs. Providers who practice using EHRs are in the forefront of improving quality, reducing costs and addressing health disparities. Since December 2011, over $784 million in incentive funds have been distributed within 24,999 payments to New York State Medicaid providers.
Also Check: Medicaid Data Warehouse New York
License For Use Of Current Dental Terminology
End User License Agreement:These materials contain Current Dental Terminology , copyright © 2021 American Dental Association . All rights reserved. CDT is a trademark of the ADA.
The license granted herein is expressly conditioned upon your acceptance of all terms and conditions contained in this agreement. By clicking below on the button labeled I accept, you hereby acknowledge that you have read, understood and agreed to all terms and conditions set forth in this agreement.
If you do not agree with all terms and conditions set forth herein, click below on the button labeled I do not accept and exit from this computer screen.
If you are acting on behalf of an organization, you represent that you are authorized to act on behalf of such organization and that your acceptance of the terms of this agreement creates a legally enforceable obligation of the organization. As used herein, you and your refer to you and any organization on behalf of which you are acting.
Does An Iud Help Prevent Stds
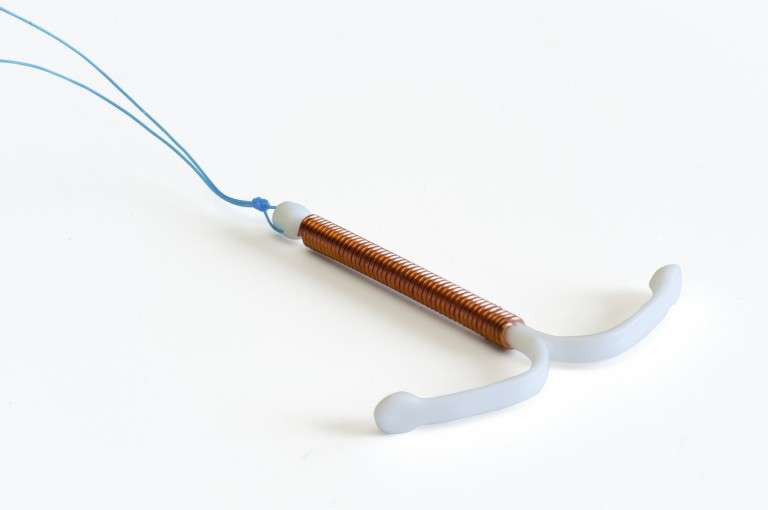
No. The IUD does not protect against sexually transmitted diseases . Couples who are having sex must always use condoms along with the IUD to protect against STDs.
A doctor or nurse practitioner will check to be sure a woman doesn’t have any STDs before putting in an IUD. Getting an IUD put in while she has an STD could lead to pelvic inflammatory disease .
Abstinence is the only method that always prevents pregnancy and STDs.
Also Check: Missouri Medicaid For College Students
How Much Will Birth Control Cost If I Have Medicare
Medicare Advantage and Medicare Part D prescription drug plans are offered by private insurance companies. Their costs vary according to the plan you choose and the coverage it provides.
The chart below contains some examples of common birth control medications and devices, and what your costs may be after youve met your annual deductible and paid the plan premium.
| Birth control method |
|---|
How Much Does It Cost
The cost of an IUD can vary depending on the health insurance plan and the type of IUD. Many health insurance plans cover the costs, and family planning clinics may charge less, particularly for teens and young adults.
Because an IUD lasts for many years, the cost works out to about the same as monthly birth control methods, such as the Pill or ring.
You May Like: How Can I Print My Medicaid Card
Information Notice To Couples With An Institutionalized Spouse
- “Information Notice to Couples with an Institutionalized Spouse” is available as a PDF.
- Additionally, the form Request for Assessment should be printed and distributed.
Medicaid is an assistance program that may help pay for the costs of your or your spouse’s institutional care, home and community based waiver services, or enrollment in a managed long term care plan. The institutionalized spouse is considered medically needy if his/her resources are at or below a certain level and the monthly income after certain deductions is less than the cost of care in the facility.
Federal and State laws require that spousal impoverishment rules be used to determine an institutionalized spouse’s eligibility for Medicaid. These rules protect some of the income and resources of the couple for the community spouse.
Note: Spousal impoverishment rules do not apply to an institutionalized spouse who is eligible under the Modified Adjusted Gross Income rules.
If you or your spouse are:
Does Medicare Cover Iud Australia
The hormonal IUD is covered by a healthcare card in Australia. It costs around $6 if you are a health care card holder and around $37 if you do not have a healthcare card. If you do not have a Medicare card it will be more expensive. The copper IUD is not covered by a healthcare card and may cost around $120.
Also Check: Qualified Health Plan Vs Medicaid
No Insurance Bayer May Be Able To Help
The Bayer US Patient Assistance Foundation is a charitable organization that helps eligible patients get Bayer prescription medicines at no cost. Please contact the program at MondayFriday, 8:30 AM5:00 PM ET, or visit the foundation website for information to see if you may qualify for assistance.
If you have Medicaid
All Medicaid programs are required to cover family planning services without cost-sharing. State coverage decisions and patient out-of-pocket costs can vary. Most Medicaid patients have no out-of-pocket expense for the Mirena IUD.
Is Contraception Covered By Medicare
Original Medicare does not cover birth control, although Medicare Part D and Medicare Advantage plans offer coverage depending on certain conditions. While Medicare primarily covers people aged 65 years and older, younger people with certain conditions or disabilities are also eligible for coverage.
Read Also: Does Medicaid Cover Long Term Care Facilities
Ama Disclaimer Of Warranties And Liabilities
CPT is provided as is without warranty of any kind, either expressed or implied, including but not limited to, the implied warranties of merchantability and fitness for a particular purpose. AMA warrants that due to the nature of CPT, it does not manipulate or process dates, therefore there is no Year 2000 issue with CPT. AMA disclaims responsibility for any errors in CPT that may arise as a result of CPT being used in conjunction with any software and/or hardware system that is not Year 2000 compliant. No fee schedules, basic unit, relative values or related listings are included in CPT. The AMA does not directly or indirectly practice medicine or dispense medical services. The responsibility for the content of this file/product is with CMS and no endorsement by the AMA is intended or implied. The AMA disclaims responsibility for any consequences or liability attributable to or related to any use, non-use, or interpretation of information contained or not contained in this file/product. This Agreement will terminate upon notice if you violate its terms. The AMA is a third party beneficiary to this Agreement.
Does Medicaid Cover Weight Loss Programs
There is a misconception that weight loss pills are mandatory Medicaid benefits, but Medicaid programs provide the benefit in part because weight loss medicines are not mandatory. Some prescription drugs are covered in Medicaid, whether its helping to control your weight or any other condition including heart disease.
Don’t Miss: How To Cancel Medicaid In Virginia
Medicaid Breast Cancer Surgery Centers
Research shows that five-year survival increases for women who have their breast cancer surgery performed at high-volume facilities and by high-volume surgeons. Therefore, it is the policy of New York State Department of Health that Medicaid recipients receive mastectomy and lumpectomy procedures associated with a breast cancer diagnosis, at high-volume facilities defined as averaging 30 or more all-payer surgeries annually over a three-year period. Low-volume facilities will not be reimbursed for breast cancer surgeries provided to Medicaid recipients. This policy is part of an ongoing effort to reform New York State Medicaid and to ensure the purchase of cost-effective, high-quality health care and better outcomes for its recipients.
The Department has completed its ninth annual review of all-payer breast cancer surgical volumes for 2013 through 2015 using the Statewide Planning and Research Cooperative System database. Seventy-three low-volume hospitals and ambulatory surgery centers throughout New York State were identified. These facilities have been notified of the restriction effective April 1, 2017. The policy does not restrict a facility’s ability to provide diagnostic or excisional biopsies and post-surgical care for Medicaid patients. Other facilities in the same region as the restricted facilities have met or exceeded the volume threshold and Medicaid patients who require breast cancer surgery should be directed to those providers.
How To Check If Your Insurance Will Cover Mirena
You may be able to get Mirena with no out-of-pocket cost.
Follow these steps to check:
*Please note: Other product-related costs may apply.
If you need help understanding your insurance coverage, visit CoverHer.org.
Recommended Reading: Does Medicaid Cover Glasses In Texas
Attention Care At Home Waiver Iii Iv And Vi Case Management Providers: New Billing Guidance Effective For Dates Of Service Beginning April 1 2017
Effective January 20, 2017, the Centers for Medicare and Medicaid Services approved the consolidation of the Care at Home III, IV, and VI waivers into the “Office for People With Developmental Disabilities Care at Home Waiver.” The new waiver will continue to serve medically fragile children under the age of eighteen who have a developmental disability and live at home with their parent or legal guardian. The purpose of the consolidation is to streamline and strengthen New York State’s administrative oversight and reporting mechanisms for these waiver programs.
Children who are currently enrolled under the CAH III, CAH IV or CAH VI Waivers, and who continued to meet eligibility requirements as of January 20, 2017 are automatically included in the new consolidated waiver. There will be no disruption in services for children served under the OPWDD Care at Home Waiver.
Effective for dates of service beginning April 1, 2017, all CAH case management services must be billed using the following rate codes, regardless of which waiver the child was enrolled in prior to April 1, 2017:
Rate CodeMedicare Website Privacy Policyprivacy Policy
Thank you for visiting www.medicarebenefits.com website , which is owned and operated by Medicare Benefits Solutions, herein after referred to as Medicare Benefits “We” or “Our”, which is a brand operated by Health Compare Insurance Services Inc. Your privacy is important to us. To better protect your privacy, We are providing this notice explaining Our online information policies and practices. By visiting this Websites, you are consenting to the practices described in this privacy policy.
Effective Date of This Privacy Policy This privacy policy is effective October 1, 2009.
Categories of Personally Identifiable Information We Collect. Medicare Benefits will receive and store information about you and your dependents such as name, address, gender, Social Security Number, age and answers to medical questions whenever this information is provided through these Websites. We may also obtain information about you from third parties such as your employer or insurance brokers who may utilize these Websites to do such things as request a quote for health insurance coverage or manage account activity online.
Log FilesThese Websites records the IP or internet protocol address of users who log on to facilitate use of these Websites. IP addresses are not linked to personally identifiable information.
Also Check: Assisted Living Facilities That Take Medicaid
How Much Is A Copper Iud Without Insurance
There are two types of IUD one uses copper and the other, progestin and the copper IUD is popular among women who want a non-hormonal form of birth control. Typical costs: For patients not covered by insurance, an IUD typically costs between $175 and $600 for the device, insertion and a follow-up appointment.
How Much Does Medicaid Cost In Nevada
NV Medicaid cost estimates vary depending on the individual and services sought. The estimate Medicaid costs discussed below do not apply to pregnant women or members who are 18 years of age or under. Pregnant women are eligible for free health services up to their post-partum period.
How much is Medicaid? The Medicaid cost estimates for copayments range from zero to a few hundred dollars depending on the service required. The majority of copays are less than $30, with basic services only costing a few dollars. However, copays can be revised from time to time, as plans and costs are evaluated regularly.
Some Medicaid coverage programs like preventive health services, emergency services, and family planning services are free of cost. Your Medicaid cost estimates in NV can change depending on any number of events.
For example, a change in income level or family size may entitle a recipient to pay less copay. Inform your Medicaid coverage health plan of any changes that can affect your benefits as soon as possible. Download our informative guide to learn more about Medicaid coverage and costs.
Read Also: Dentist In Salt Lake City That Accept Medicaid
Contribution From Community Spouse
The amount of money that we will request as a contribution from the community spouse will be based on his/her income and the number of certain individuals in the community depending on that income. We will request a contribution from a community spouse of 25% of the amount his/her otherwise available income that exceeds the minimum monthly maintenance needs allowance plus any family member allowance. If the community spouse feels that he/she cannot contribute the amount requested, he/she has the right to schedule a conference with the local department of social services to try to reach an agreement about the amount he/she is able to pay.
Pursuant to Section 366 of the Social Services Law, Medicaid MUST be provided to the institutionalized spouse, if the community spouse fails or refuses to contribute his/her income towards the institutionalized spouse’s cost of care. However, if the community spouse fails or refuses to make his/her income available as requested, then the Department, at its option, may refer the matter to court for a review of the spouse’s actual ability to pay.
Where Can I Get Services

Services are available at any eligible Apple Health provider.
Condoms and spermicides are available at pharmacies without a prescription.
Emergency Contraception is available at any eligible Apple Health provider or directly from a pharmacist. For more information, visit the Emergency Contraception website.
You May Like: How To Apply For Medicaid In Dc
What Is The Family Planning Program
This program allows men and women to get family planning services only. This program is a form of limited insurance coverage. If you are able to enroll in the FPP, most of your basic family planning services will be paid for. However, it does not meet the Affordable Care Act requirements for a minimum essential benefits plan.
What Do Family Planning Services Cost
There is no cost for family planning services, including office visits and drugs/devices. You do not have to pay a co-payment for family planning services.
Where can you go for family planning services?
You can go to any Health First Colorado provider who offers family planning services, such as:
-
An ob/gyn or gynecologist
-
A nurse practitioner or other advanced practice nurse
-
A family planning clinic
-
Your regular doctor or primary care provider
You do not need a referral from your primary care provider in order to get family planning services. You can choose to see any Health First Colorado family planning provider even if you are in a managed care plan and the provider you want to see is out-of-network. For help finding a family planning provider, please see the Find a Doctor page or call the Member Contact Center.
Program Contact:
Don’t Miss: Nursing Homes That Accept Medicaid
