Spending Down To Become Eligible As Medically Needy
A person spends down his or her excess income to the states medically needy limit by incurring medical expenses, such as doctor visits, prescription drugs, or anything else the state considers to be medical or remedial care. It is important to understand that the person does not actually have to pay an expense for it to count as an incurred expense. The person only has to incur the obligation to pay the expense.
The medical expenses the person has incurred are then subtracted from his or her income. If the remaining income does not exceed the states income limit, the person is eligible as medically needy.
The medically needy income limit varies considerably from state to state. In most of the states that cover the medically needy, the income limit for an individual is less than $500 a month.
As an example of how this works, Mr. George has income of $1,000, which is too high to qualify for Medicaid in his state unless he can qualify as medically needy. His state has a medically needy income limit of $400 a month. That means Mr. George has a spenddown liability, or spenddown amount, of $600, which is the difference between his income and the states income limit.
For a person with high income, the spenddown liability can be considerable. But, a person receiving long-term care services, particularly as an inpatient in a nursing home, can incur enough expenses very quickly because nursing home care is very expensive.
How Do You Calculate Your Medicaid Income Eligibility
Follow these steps to calculate whether or not your income may qualify you for Medicaid:
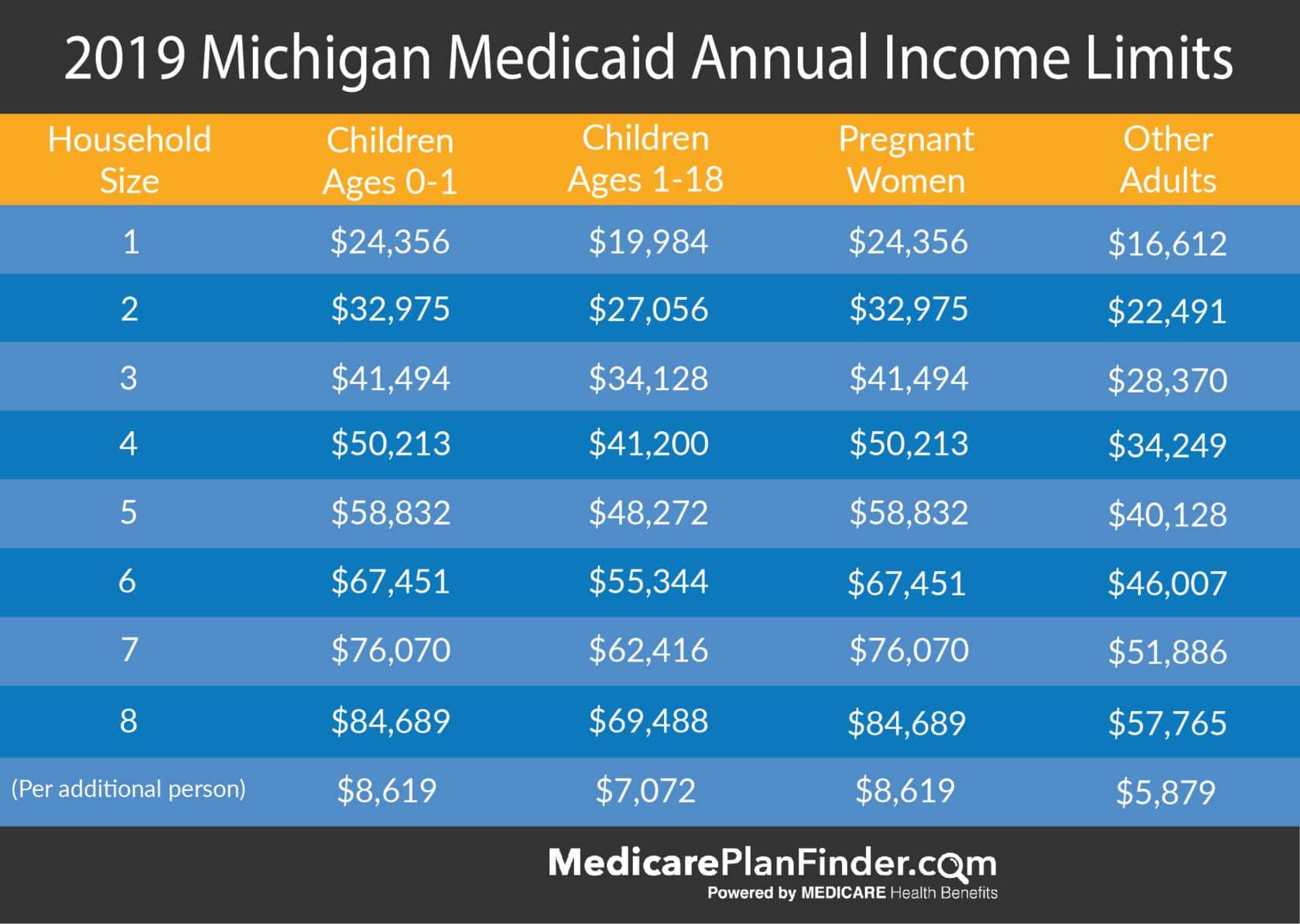
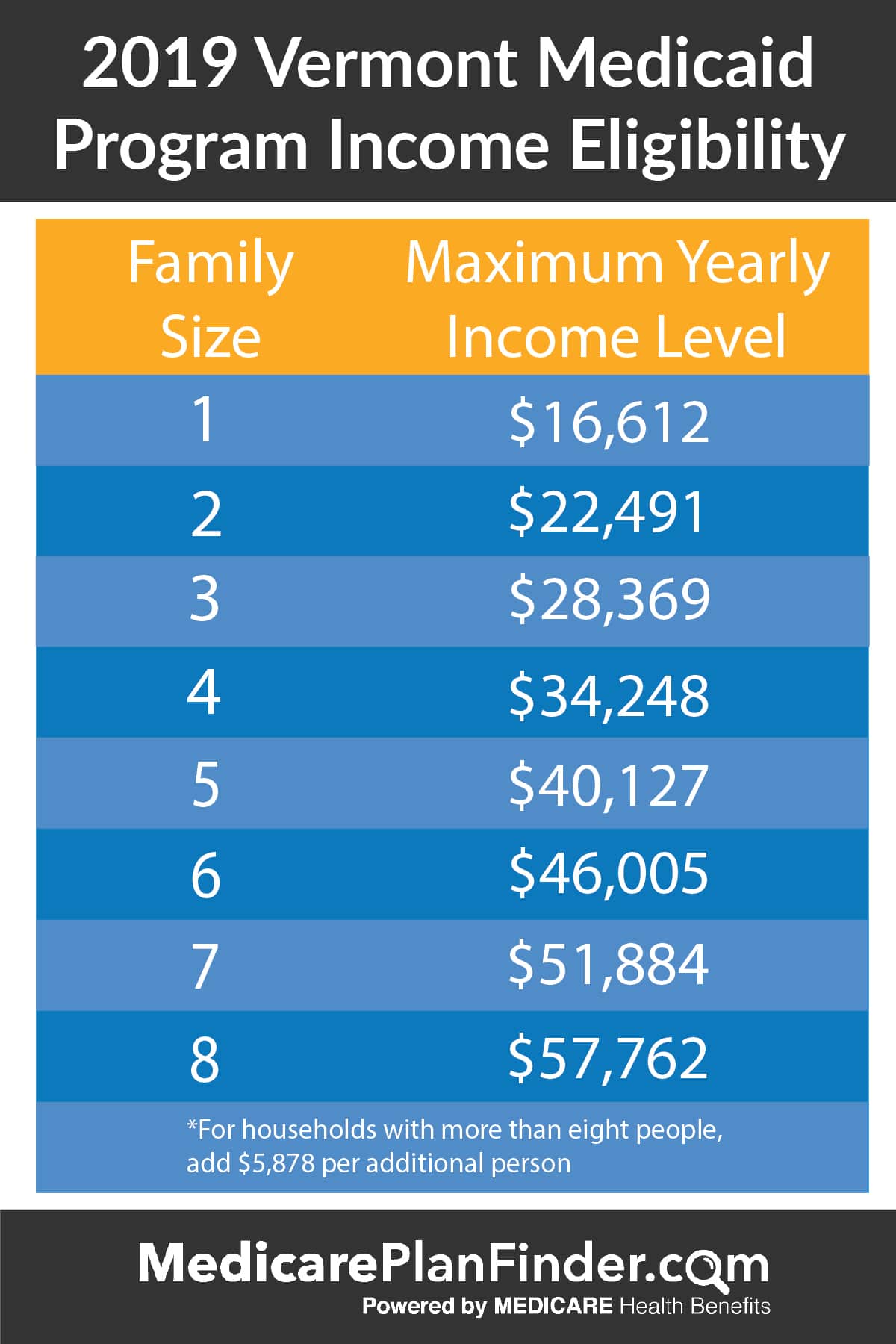
- Find the FPL for your household using the chart above
- Multiply that number by your states Medicaid income limit found below, and then divide by 100
For example, if there are two people living in your household and you live in Arizona, you would multiply $17,420 by 138 and then divide by 100. That equals $24,039.60.
You may also multiply $17,420 by 1.38.
Who Can Get Medicaid
- No matter your state, you may qualify for Medicaid based on your income, household size, disability, family status, and other factors. But if your state has expanded Medicaid coverage, you can qualify based on your income alone.
- Enter your household size and state. We’ll tell you who is eligible for Medicaid, if your state expanded and if you qualify for Medicaid based only on your income.
- If you think you have Medicaid eligibility, you can create an account and fill out a Marketplace application. If it looks like anyone in your household qualifies for Medicaid or CHIP, we’ll send your information to your state agency. They’ll contact you about enrollment. You can apply any time of year.
- If you don’t qualify for Medicaid, we’ll tell you if you qualify for financial help to buy a Marketplace health plan instead.
You May Like: How To Get Medicaid In Colorado
Can I Qualify Even If My State Does Not Have Expanded Medicaid
In states that have not expanded Medicaid, eligibility levels are lower than in states that have expanded. Even if your state hasn’t expanded Medicaid and it looks like your income is below the level to qualify for financial help with a Marketplace plan, you should fill out a Marketplace application.
What Does Medicaid Cover
Medicaid is a joint state and federal program that provides health care coverage to qualifying individuals. Anyone who meets the eligibility requirements has a right to enroll in Medicaid coverage. Although each state has its own Medicaid program, the federal government places rules that all states must follow. Based on the federal rules, states run their Medicaid programs to best serve the qualifying residents.
States can elect to provide more services than mandated by the federal government and may extend coverage to a larger population.
Federal law mandates that states provide certain benefits, known as mandatory benefits, under Medicaid. States also may provide additional benefits and services, known as optional benefits. The table below shows some of the mandatory and optional Medicaid benefits.
| Mandatory Benefits | |
| Certified pediatric and family nurse practitioner services | Private-duty nursing services |
Some Medicaid programs pay for health care directly, while others cover beneficiaries through private managed-care plans.
Because Medicaid is a jointly funded program, the federal government pays states for a certain portion of its program expenditures, known as the Federal Medical Assistance Percentage . States should be able to fund their shares of Medicaid expenditures for the services available under their specific plans.
Don’t Miss: New York State Medicaid Application
Home And Community Based Services For Developmentally Disabled
Home and Community Based Services provides South Dakota Medicaid for individuals with developmental disabilities who would otherwise be institutionalized in a Medicaid-funded hospital, nursing facility or an intermediate care facility.
Eligibility Requirements
- A person must be developmentally disabled.
- A person must be aged, blind or disabled.
- A person must reside in the home of a parent, other relative, legal guardian, adult foster care home licensed by the state, special therapeutic foster home licensed by the state, community residential facilities approved by the Department of Human Services, supervised apartment approved by the Department of Human Services, or community habilitation facilities approved by the Department of Human Services of an individuals own home.
- A person’s monthly income must be less than 300 percent of the SSI Standard Benefit Amount . The resource limit is $2,000 for an individual. Resources include items such as checking and savings accounts and certificates of deposit.
to the standard Medicaid covered services
Case Management and Consumer Support: This includes adaptive equipment needed not to exceed $500 per person per year. Examples of adaptive equipment would be communication devices, eyeglasses, hearing aids, etc.
Other Information for Home and Community Based Services can be found here: Department of Human Services’ Division of Developmental Disabilities
How To Get Medicaid
Since Medicaid programs are state-managed, eligibility requirements vary from state to state. Your eligibility for Medicaid coverage depends in part on whether the state you live in has adopted the expanded program. In all states, you may qualify for Medicaid based on your household size, income, family status, and disability, among other factors.
In states that run an expanded Medicaid program , your income alone level can qualify you for coverage. Your family may be eligible for Medicaid if your current household income is at or below the 2021 100% federal poverty level.
The federal government sets income limits every year to define the federal poverty level for different households. Children between 1 and 6 years are eligible for Medicaid benefits when the household income doesnt exceed 133% of the federal poverty level. Pregnant women and infants younger than one year are eligible for Medicaid with a family income not exceeding the 200% federal poverty level. Pregnant women are factored as two family members.
Depending on how your household income is calculated, some states will use an income limit at or below 138% of the federal poverty level.
Not every low-income individual is eligible for Medicaid. In states that are yet to implement the Affordable Care Act Medicaid expansion, adults over 21 are often ineligible for Medicaid no matter how low their incomes are. Exceptions include when theyre pregnant, elderly, caring for children, or have a disability.
Also Check: Dentist In Gainesville Ga That Accept Medicaid
South Dakota Medicaid For Certain Newborns
South Dakota children born to women eligible for South Dakota Medicaid are also eligible for South Dakota Medicaid.
Eligibility Requirements
- The child must be born to a woman eligible for and receiving South Dakota Medicaid on the date of the childs birth.
- There is no resource or income limit.
- Coverage continues from the month of birth until the end of the month in which the child turns one year of age as long as the child continues to live in South Dakota.
Learn About Requirements For Medicaid In Iowa
Applicants should understand who is eligible for Medicaid in Iowa before applying for medical assistance. Often, Medicaid benefits eligibility candidates wonder what information they need to know before sitting down to begin an application. The best question to ask during this time are What are the requirements for Medicaid in IA? so interested applicants can determine if they meet these requirements and are thus eligible to be considered for health care assistance. Knowing how to qualify for Medicaid can help potential Medicaid recipients be better prepared for the application process, which results in a higher chance of being admitted into the program. Since there are many special requirements for Medicaid applicants, continue reading the sections below to gain a better understanding.
Who qualifies for Medicaid in Iowa?
The basic Iowa Medicaid eligibility requirements are the first guidelines that prospective Medicaid applicants should review. These basic Medicaid requirements are consistent for every applicant, regardless of the familial or personal situations that may also qualify them to receive medical assistance. Additionally, standard requirements for Medicaid enable the system to verify an applicants identity and their financial need for assistance. These requirements are the following:
What are the income requirements for Medicaid in Iowa?
What are the Medicaid application guidelines in Iowa?
What are disqualifications for Medicaid in Iowa?
Also Check: Anthem Blue Cross Medicaid Nevada
Apply Directly With A State Medicaid Program
The most direct way to apply for Medicaid is to contact a state office directly and put in an application. This often requires a brief meeting with a benefits counselor or case worker to establish eligibility for the program. Some states take Medicaid applications online, while others require an in-person visit to a Social Security Administration office.
In many states, applications for Medicaid can be taken at county Human Services offices. Seniors with limited ability to travel or manage their affairs may apply for Medicaid through an authorized representative, including the benefits coordinator at a residential care facility.
What Is The Medicaid Income Limit In My State
Most states use a standard of 138% of the federal poverty level as a basis for Medicaid eligibility. But each state is free to set its own limits.
The table below shows the income limit as a percentage of the FPL required for Medicaid eligibility in each state for two-parent households and for individuals adults.
If 0% appears, that means individuals may not qualify for Medicaid in that state based on income alone and must meet other criteria, such as being pregnant or disabled.
Medicaid Income Limit by State|
State |
|
|---|---|
| 52% | 0% |
FPL is used to determine eligibility for Medicaid, certain welfare benefits and other assistance programs. The FPL is computed by the U.S. Census Bureau and can be adjusted every year based on inflation.
Medicaid uses a percentage of the FPL to determine its income limits for eligibility. For example, you may qualify for Medicaid if you earn less than 133% of the federal poverty level. Or you may qualify if you earn less than 150% of the federal poverty level and are disabled. Again, each state sets its own income limits to determine Medicaid eligibility.
Contact your state Medicaid program for more eligibility information, as most states offer different types of Medicaid programs that may each have their own income limits and other qualifying criteria. Even if you make more than the standard limit found below, there may be additional programs for which you still qualify.
Don’t Miss: Priority Health Medicaid Vision Providers
Who Is Eligible For Medicaid In Pennsylvania
The following people may qualify for Pennsylvania Medicaid if they meet certain financialrequirements:
- Adults age 19-64 with incomes at or below 133% of the Federal Income Poverty Guidelines
- Individuals who are aged , blind and disabled.
- Families with children under age 21
- Special Medical Assistance conditions
Health Care Programs Eligibility
Health care coverage is available to individuals and families who meet certain eligibility requirements. The goal of these health care programs is to ensure that essential health care services are made available to those who otherwise do not have the financial resources to purchase them.
It is very important that individuals and families obtain health care coverage. In Michigan, there are many health care programs available to children, adults, and families. Specific coverages may vary depending on the program and the applicant’s citizenship status . The Michigan Department of Health and Human Services determines eligibility for most of the health care programs that are administered by the State of Michigan).
All of the health care programs in Michigan have an income test, except Children’s Special Health Care Services, and some of the programs also have an asset test. These income and asset tests may vary with each program. For some of the programs, the applicant may have income that is over the income limit and still be able to obtain health care benefits when their medical expenses equal or exceed their deductible amount.
Recommended Reading: How To Become A Medicaid Consultant
Reduced Coverage / Medicare Cost Sharing Or Premium Payment
Qualified Medicare BeneficiariesCovered group: individuals covered by MedicareIncome limits: Income cannot exceed 100% of the federal poverty level. For more information, view the Guidelines for Medicare Cost-Sharing Programs brochure.Age: Medicare beneficiaries of any ageQualifications: Individuals must be eligible for Medicare Part A hospital insurance.
Specified Low-Income Medicare BeneficiariesCovered group: individuals covered by MedicareIncome limits: Income cannot exceed 135% of the federal poverty level. For more information, view the Guidelines for Medicare Cost-Sharing Programs brochure.Age: Medicare beneficiaries of any ageQualifications: Individuals must have Medicare Part A
Qualified IndividualsCovered group: individuals covered by MedicareIncome limits: Income cannot exceed 135% of the federal poverty level. For more information, view the Guidelines for Medicare Cost-Sharing Programs brochure.Age: Medicare beneficiaries of any ageQualifications: Individuals must have Medicare Part A
Can You Decline Medicaid
You can decline Medicaid if you qualify for benefits but don’t want them. You can purchase a private plan on the marketplace, but most people who qualify for Medicaid find paying for private health insurance challenging. You should also be aware that declining Medicaid won’t let you get tax credits or reductions to use on a different insurance policy.
There is no longer a federal penalty for not having health insurance. You can decline Medicaid coverage and not buy another plan without worrying about a federal penalty. However, some states impose penalties on those without health insurance. You may want to check if your state will impose a tax penalty or fee if you don’t have insurance.
Recommended Reading: Will Medicaid Pay For Assisted Living In Ohio
What Services Does Medicaid Cover
Medicaid covers more than 60 percent of all nursing home residents and roughly 50 percent of costs for long-term care services and supports.
Federal rules require state Medicaid programs to cover certain mandatory services, such as hospital and physician care, laboratory and X-ray services, home health services, and nursing facility services for adults. States are also required to provide a more comprehensive set of services, known as the Early and Periodic Screening, Diagnostic, and Treatment benefit, for children under age 21.
States can and all do cover certain additional services as well. All states cover prescription drugs, and most cover other common optional benefits include dental care, vision services, hearing aids, and personal care services for frail seniors and people with disabilities. These services, though considered optional because states are not required to provide them, are critical to meeting the health needs of Medicaid beneficiaries.
About three-quarters of all Medicaid spending on services pays for acute-care services such as hospital care, physician services, and prescription drugs the rest pays for nursing home and other long-term care services and supports. Medicaid covers more than 60 percent of all nursing home residents and roughly 50 percent of costs for long-term care services and supports.
How Much Does Medicaid Cost? How Is It Financed?
Appealing For Denial Of Coverage
Youll start receiving the appropriate Medicaid services if you meet all the requirements and are deemed financially eligible. If you dont meet all the eligibility requirements, you will be notified of your right to a fair hearing. States must provide individuals who think they should be eligible the opportunity to appeal the denial of coverage, either on the grounds that an error was made or that the state failed to act promptly.
The structure of the appeals process varies among states. The Medicaid agency may conduct the appeals process or otherwise delegate it. Another state agency may conduct the appeal following approval from the Centers for Medicare & Medicaid Services .
Don’t Miss: Pediatricians In Amarillo Tx That Accept Medicaid
I Qualify For Medicaid But Don’t Want It
Not everyone who qualifies for Medicaid wants the benefits, but there are some important things to consider before opting out.
People have various reasons for not wanting Medicaid even though they qualify:
- They believe they will only meet the low-income requirements for a short time and don’t want the hassle of having to switch to other insurance.
- They would prefer to get private insurance.
- They don’t want to deal with perceived administrative hassles of enrolling in Medicaid.
- They don’t want to accept government assistance.
In most cases, you don’t have to accept Medicaid benefits, but there are some things to consider before declining. Medicaid can help you avoid massive medical bills if you get sick or are in an accident. Some people don’t want Medicaid because they think they won’t need it for long. However, if an employment opportunity falls through or you can’t get private insurance as planned, you may be left without healthcare.
You can usually have Medicaid and private insurance, so long as you otherwise qualify for Medicaid. Medicaid may cover services that the private plan won’t, but you must pay for expenses associated with your private health insurance. When combined with other coverage, Medicaid is typically the “payer of last resort,” which means the private insurance company must be billed first.
