Missouri Medicaid Expansion Brings Quality Essential Health Coverage To More Than 275000 Missourians
Biden-Harris Administration Encourages Eligible Missourians to Apply for Coverage
The Centers for Medicare & Medicaid Services announced today that approximately 275,000 Missourians are now eligible for comprehensive health coverage, thanks to Medicaid expansion under the Affordable Care Act. Through the American Rescue Plan , Missouri will be eligible to receive an estimated $968 million in additional federal funding for its Medicaid program over the next two years.
Free or low cost health coverage is now available to Missourians in many cases for the first time. For example, a single adult making up to $17,774 a year, or a family of 4 making up to $36,750 a year, may qualify for Medicaid through MO HealthNet. This includes parents who have not qualified before, as well as adults without children.
Hundreds of thousands of Missourians can now gain the peace of mind of having health coverage through Medicaid, said Health and Human Services Secretary Xavier Becerra. This is a win for all Missourians who have fought long and hard to gain their rightful access to quality health insurance made possible through the Affordable Care Act. As we celebrate Missouris Medicaid expansion, the Biden-Harris Administration will double down on our outreach efforts to urge the remaining twelve states to join the rest of the nation in ensuring access to health care during this critical time.
History Of Medicaid Expansion
As noted at the start of this summary, Medicaid was a cornerstone of ACA lawmakers efforts to expand access to healthcare. The idea was that everyone with household incomes up to 133% of the federal poverty level would be able to enroll in Medicaid.
People above that threshold would be eligible for premium tax credits in the exchanges to make their coverage affordable, as long as their income didnt exceed 400% of the poverty level. The idea was that people with income above 400% of the poverty level would be able to afford coverage without subsidies, but that has not proven to be the case. So the American Rescue Plan temporarily eliminated the income cap for subsidy eligibility, and the Build Back Better Act aims to extend that for several more years.
Because Medicaid expansion was expected to be a given in every state, the law was written so that premium subsidies in the exchange are not available to people with incomes below the poverty level. They were supposed to have access to Medicaid instead.
How Can People Apply
- Apply online at www.MySoonerCare.org.
- Apply by phone by calling the SoonerCare Helpline 800-987-7767.
- Fill out an English or Spanish paper application and mail it to the address on the application.
- Apply through one of our agency partner facilities.
Training opportunities are available for community partners.Email if your organization is interested in training.A toolkit is available for community partners at on our Community Partners page.
You May Like: Medicaid For The Elderly And People With Disabilities
Will Any Of These Ideas Come To Fruition
Even with a variety of ideas on the table, “there’s no slam dunk option, it’s a tough policy issue,” Rudowitz says. All of these would be complicated to pull off.
It’s possible Democrats will include one of these ideas in a reconciliation bill that could pass without the threat of a Republican filibuster. But that bill has yet to be written, and what will be included is anyone’s guess.
Even so, Michener says she’s glad the discussion of the Medicaid coverage gap is happening, because it’s sensitizing the public, as well as people in power, to the problem and potentially changing the political dynamic down the line. “Even in policy areas where you don’t have any kind of guaranteed victory, it is often worth fighting the fight,” she says. “Politics is a long game.”
Building On The Evidence Base: Studies On The Effects Of Medicaid Expansion February 2020 To March 2021
The new financial incentive for expansion in the American Rescue Plan Act of 2021 has reignited debate on Medicaid expansion under the Affordable Care Act in the twelve states that have not adopted the expansion. Further, the coronavirus pandemic has adversely affected health outcomes and economic wellbeing. While Medicaid has served as a coverage safety net during the pandemic and resulting economic crisis, coverage options for many low-income adults are limited in non-expansion states.
This literature review provides context for these expansion debates by summarizing evidence from nearly 200 studies published between February 2020 and March 2021 on the impact of state Medicaid expansions under the ACA. This review builds on an earlier report concluding that expansion is linked to gains in coverage improvements in access, financial security, and some measures of health status/outcomes and economic benefits for states and providers .
This recent body of research finds positive effects of expansion across a range of increasingly complex and specific categories. Accordingly, this report highlights study findings across multiple key themes of interest:
Recommended Reading: Does Medicaid Cover Glasses In Texas
Frequently Asked Questions About Medicaid Expansion
Misconceptions about Medicaid expansion under the Affordable Care Act obscure the fact that the Medicaid program boasts a long track record of proven effectiveness in providing care and assistance to those most in need.
A centerpiece of the Patient Protection and Affordable Care Actoften referred to as Obamacareis the expansion of Medicaid eligibility to people with annual incomes below 138 percent of the federal poverty level, or $26,347 for a family of three and $15,417 for an individual. Despite the fact that the Affordable Care Act was passed into law in 2010 and was subsequently upheld by the U.S. Supreme Court in the summer of 2012, many questions persist about the law, particularly as it relates to Medicaid expansionwhat that expansion actually means, who it will cover, what it will cost, and more.
As we mark the third anniversary of the passage of the Affordable Care Act, it is important not to lose perspective about what Medicaid expansion actually means for the millions of people it will help to insure, as well as the economic benefits it will bring to states and local economies. Here are the 10 questions about Medicaid expansion under the law that are asked most frequently and are too often answered incorrectly.
Medicaid Expansion Updates And Waivers
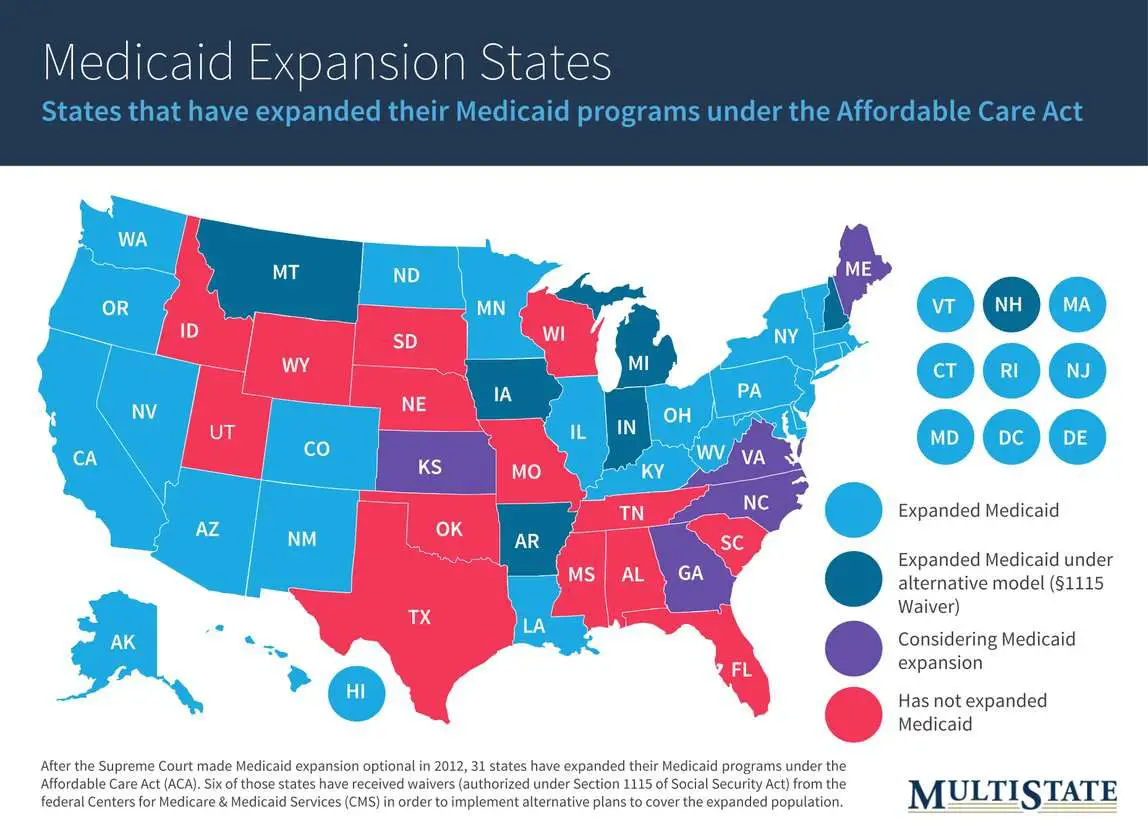
As of 2020, 38 states and the District of Columbia have Expanded Medicaid or voted to expand Medicaid, while 12 states have not. Although the number gets lower with each new state that passes expansion, 4.8 million adults who should have been covered under the ACA still lacked coverage as recently as 2020.
NOTE: Make sure to check the up-to-date list of states expanding Medicaid and an interactive map with descriptions of states considering expansion to see if your state is on there, we try to keep this page up to date, but details are subject to change.
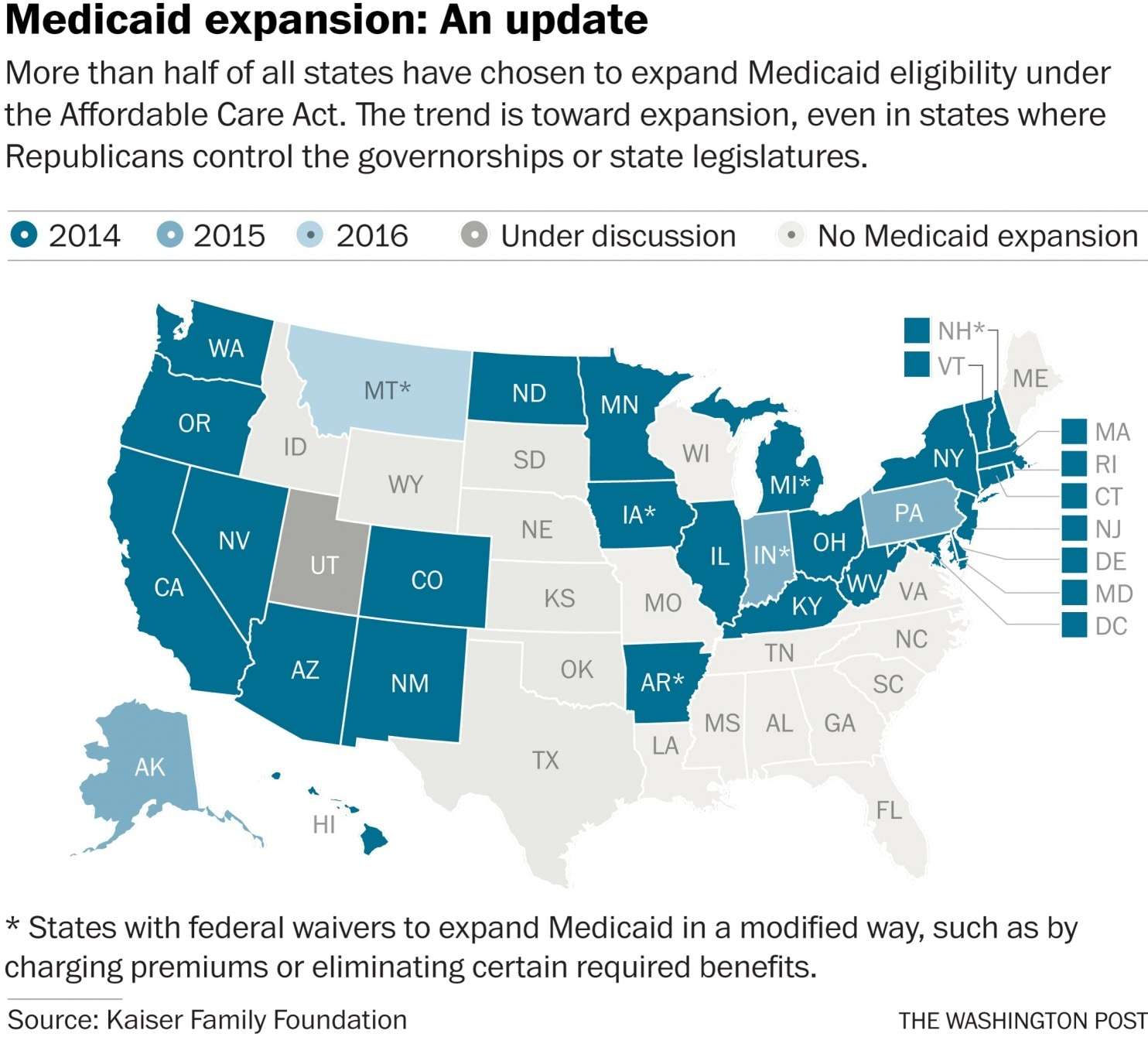
Arizona, Arkansas, California, Colorado, Connecticut, Delaware, Washington D.C., Hawaii, Illinois, Iowa, Kentucky, Maryland, Massachusetts, Michigan, Minnesota, Nebraska, Nevada, New Hampshire, New Jersey, New Mexico, New York, North Dakota, Ohio, Oregon, Rhode Island, Vermont, Washington, and West Virginia started expanded Medicaid in 2014. Alaska, Indiana, and Pennsylvania expanded in 2015. Louisiana expanded in 2016. Montana also expanded in January 2016, but it will sunset on June 30, 2019 unless the state legislature acts to extend it. Maine adopted the Medicaid expansion through a ballot initiative in November 2017. Virginia expanded in 2018. Nebraska, Utah, and Idaho voters passed Medicaid expansion via ballot initiatives in November 2018. Then in 2019 even more states embraced Medicaid expansion like Montana. In 2020 Oklahoma and Missouri voted to expand Medicaid as well.
Recommended Reading: Anthem Healthkeepers Plus Medicaid Transportation
Option : Create A Federal Public Option To Fill The Gap
Some have advocated for circumventing these holdout states and creating a new, standalone federal Medicaid program that people who fall into this coverage gap could join. It would be kind of like a tailored public option just for this group.
This idea was included in Biden’s 2022 budget,which says, in part: “In States that have not expanded Medicaid, the President has proposed extending coverage to millions of people by providing premium-free, Medicaid-like coverage through a Federal public option, paired with financial incentives to ensure States maintain their existing expansions.”
Did Missouri Accept The Medicaid Expansion
The Affordable Care Act Medicaid expansion aims to help more low-income individuals receive medical benefits. The expansion, which is abbreviated as the ACA Medicaid expansion and sometimes referred to as the Obamacare Medicaid expansion, was offered from the federal government to all 50 states and Washington D.C. The ACA Medicaid expansion is not a required program, and each state is given the ability to accept or opt out of the expansion plan. If widely instituted, thousands of people in each state would be eligible for coverage. Many residents find themselves asking, What is the Obamacare Medicaid expansion in Missouri and did the state adopt the expansion? when they first learn about the expansion plan. Learn about the ACA expansion and find out if an MO Affordable Care Act Medicaid application is available by reading the following topics on this page.
What is the expansion of Medicaid in Missouri?
Learn About the ACA Medicaid Expansion in Missouri
What does opting out of the Affordable Care Act Medicaid expansion mean for Missouri?
Anyone can fill out the Missouri Medicaid application, but not everyone can get in. If you are applying for Medicaid or any other benefits program, be sure to read the eligibility criteria before submitting an application. Please be aware that the Medicaid program is called MO HealthNet in Missouri. Medicaid is not a lifelong program, and most benefit recipients will be reevaluated after a 12-month period.
Also Check: Illinois Nursing Homes That Accept Medicaid
Medicaid Expansion 133% Or 138%
Sometimes we say Medicaid is expanded to 133% FPL, and sometimes we say 138%. Both are correct. The text of the ACA says 133%, but the law also calls for a new methodology of calculating income, which will make the effective minimum threshold of 138%. Either way, remember that these are minimum thresholds states can set eligibility thresholds higher, and many already have for certain populations, which means that more people qualify.
Selected federal poverty level thresholds regarding annual income, 2014. Please note that ObamaCare uses the 2014 Federal Poverty Guidelines for 2015. Please also note the chart below is meant for educational purposes, for assistance in the current year see our federal poverty level page.
| FPL | ||
| $46,680 | $95,400 | This will be the upper limit for eligibility for income-based subsidies for the purchase of private insurance through the new health insurance exchanges. |
What Does The Obamacare Supreme Court Ruling Really Mean
The Supreme Court upheld the Affordable Care Act in 2012, but it gave the states the choice to opt out of Medicaid expansion. It is now rests with governors and state legislatures to decide whether it is in the best interest of the state to implement the Medicaid portion of the law that affords health coverage to those in need.
If a state chooses not to expand the program, the federal government cannot take away the Medicaid funds a state already receives. So while states have the carrot of extra Medicaid funding if they take up the expansion, they dont have the stick of losing federal funding if they do not take it. This ability to opt out of the expansion but suffer no serious consequences undermines the laws ability to ensure that millions of low-income Americans benefit from the expansion of Medicaid coverage. This caveat in the Courts decision opened the door to allow governors to deny an essential aspect of health care reform. Unfortunately, states opting out of Medicaid expansion do so to the detriment of their residents, as well as their state budget.
You May Like: Can You Get Plan B For Free With Medicaid
Medicaid And The Covid Pandemic
As noted above in the section about work requirements, the Families First Coronavirus Response Act essentially prevents states from making their eligibility standards any more strict during the COVID emergency period than they were as of the start of 2020.
Section 6008 of the FFCRA provides states with a 6.2 percentage point increase in their federal Medicaid matching funding for the duration of the COVID public health emergency period, as long as the state Medicaid program:
- keeps its eligibility standards no more restrictive than they were at the start of 2020,
- does not raise premiums above the levels they were at in January 2020,
- provides no-cost coverage for COVID testing and treatment,
- does not terminate enrollees coverage for the duration of the COVID emergency period, unless they move out of the state or request that their coverage be terminated.
CMS previously interpreted this last point to mean that in order to receive the increased federal Medicaid funding, a state must keep beneficiaries enrolled in Medicaid, if they were enrolled on or after March 18, 2020, with the same amount, duration, and scope of benefits, and that states could not subject such beneficiaries to any increase in cost-sharing or beneficiary liability for institutional services or other long-term services and supports during this time period.
Who Is Eligible For Medicaid In Oklahoma
Since Medicaid expansion took effect in July 2021, non-elderly adults are eligible for Medicaid with household income up to 138% of the poverty level . Children and pregnant women continue to be eligible for Medicaid at higher income levels, although nothing has changing about Medicaid eligibility rules for people age 65 and older.
As part of a demonstration waiver that was approved in 2019, up to 3,000 full-time college students aged 19 to 22 in Oklahoma could be covered under Medicaid if their incomes dont exceed 200% of the poverty level . The state has clarified that dependent college students must count their parents household income, whereas independent college students can enroll based on their own income. SB1548, introduced in February 2016, would have increased the age limit for the demonstration waiver to 26, would have removed the requirement that the student be in school full-time, and would have expanded the term college to include trade and technical schools. But SB1548 did not advance out of committee.
Don’t Miss: Medicaid Assisted Living Austin Texas
Medical Infrastructure And National Health Insurance
At the same time that Medicare was passed in 1965, the Johnson administration also was interested in a program designed to counter the risks of heart disease, cancer, and stroke. The administration proposed to spend $1.2 billion over 6 years to establish 32 university-based medical complexes that would contain diagnostic and treatment centers for these diseases. The administration also favored aid to medical schoolsâinstitutional support with the objective of increasing the number of doctors and dentists available for private practice as well as $15 million for the construction and renovation of medical libraries . Variations of each of these proposals became law during the same session that Congress passed Medicare.
Option : Change The Aca To Open Up The Exchanges
A fourth idea, Rudowitz says, is to change the law to remove the minimum cutoff for the private health insurance exchanges, since “right now, individuals who are below poverty are not eligible for subsidies in the marketplace.” With this option, states wouldn’t be paying any of the costs, since the federal government pays premium subsidies, Rudowitz says, but “there are issues around beneficiary protections, benefits, out-of-pocket costs.”
What’s next: This idea hasn’t yet been included in any current congressional bills.
Don’t Miss: Will Medicaid Pay For Braces For Adults
What Are The Costs If Medicaid Isnt Expanded
There is both a human and fiscal cost if Medicaid expansion is rejected. States will have to continue to pay for the treatment of the uninsured in hospitals, public clinics, and other care facilities with state tax dollars, which is much more expensive than the minimal share theyd pay under the Medicaid expansion. And when it comes to the impact of Medicaid coverage, several studies indicate that Medicaid coverage leads to overall better health and lower mortality rates. According to a study by the state of Oregon, after one year of enrollment in Medicaid, low-income childless adults significantly reduced their financial strain, increased their health care use, and reported having overall better health. Expanded Medicaid coverage also led to , especially among residents of poorer counties, as indicated by the New England Journal of Medicine.
Failed Attempt To Cut Medicaid Eligibility For Parents
Despite not expanding Medicaid under the ACA, Oklahoma also attempted to go one step further than that, and tighten already-stringent eligibility rules even more.
Amid a budget shortfall of $1.3 billion, lawmakers in the Oklahoma House of Representatives passed HB2665 in March 2016. HB2665 called for eliminating Medicaid eligibility for non-pregnant, able-bodied adults under age 65. All 30 Democrats in the Oklahoma House opposed the bill, and were joined by four Republicans.
But the Senate did not pass HB2665, so Medicaid eligibility for parents in Oklahoma remained unchanged.
As background, the only non-pregnant, able-bodied adults under age 65 who currently qualify for Medicaid are those with household incomes up to 41% of the poverty level, and who also have dependent children. For a household of two , thats an annual income of about $6,750 in 2018.
Most able-bodied adults with dependent children arent able to qualify for Medicaid in Oklahoma because their incomes arent low enough. And able-bodied adults without dependent children arent eligible for Medicaid at all in Oklahoma, regardless of their income, because the state has not accepted federal funding to expand Medicaid.
Don’t Miss: Does Medicaid Cover Spinal Cord Stimulators
