How Do I Know If My Child Is Due For A Texas Health Steps Checkup
Texas Health Steps will send you a letter when its time for your childs medical and dental checkups. You can also visit YourTexasBenefits.com or call the number below to find out if your child is due for a checkup.
Phone
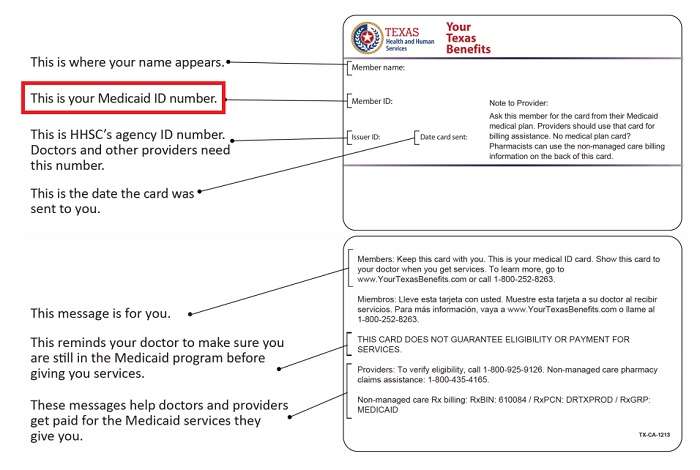
Read Also: How To Find Your Medicaid Number
Rhode Island Medicaid Eligibility
Rhode Island provides Medicaid benefits to assist low-income individuals and families, as well as seniors and people with disabilities, in receiving the healthcare they need.
Which Medicaid plan is best in Rhode Island?
Rhode Island provides many Medicaid-related programs that help low-income households with healthcare costs, though like many states, what benefits are available to you depends on your health needs and financial situation.
You can apply for Rhode Island Medicaid assistance by completing an online application.
Rhode Island Medicaid Application:
How To Check If My Medicaid Was Approved
Medicaid provides medical care to over 73 million citizens of the United States. It is considered the program with the most coverage in the country. The US government launched Medicaid in 1965 along with two other programs CHIP and BHP . The aim of the programs was to provide quality healthcare to disabled people, parents, seniors, pregnant women, and low-income families.
People who apply for Medicaid are always anxious to know their status. If you are wondering how to check if my Medicaid was approved then continue reading this article.
You apply for Medicaid assistance once you know that you are eligible for it. Your coverage begins either from the first day of the month you applied or from the exact date you applied. Either date can be your first day of coverage. The office of the Center of Medicaid makes the decision which is based on your economic record and medical record. The office also informs you of the assigned date.
If you fulfill certain requirements, your Medicaid coverage can work retroactively for a period of three months before you apply at a particular month.
There are two ways to find the status of your Medicaid application:
Also Check: Find Primary Care Doctor Medicaid
How To Find Out If My Medicaid Is Active
Medicaid is a state-operated program funded by the state and federal government in order to provide health care to certain low-income residents, including disabled individuals, pregnant women, children, the elderly and others. A medical provider will typically run a Medicaid eligibility check in order to verify the status of your Medicaid.
Obtain your state’s Medicaid office contact information from the National Association of State Medicaid Directors website, a link to which is included in the “Resources” section of this article. If you do not have access to the Internet, you can call NASMD at 682-0100. If you have your Medicaid number, skip to Step 3. If you do not, continue to Step 2.
Contact your local or state Medicaid office in order to verify the status of your Medicaid coverage. If you have your Medicaid card, this number is typically listed on the back of the card. If you do not have your card, you may use the number used in Step 2 to verify your Medicaid status.
Tips
-
Obtain information regarding reasons why your Medicaid is not active if you discover that your Medicaid is currently inactive. In many cases, you can file an appeal if your Medicaid was discontinued for reasons such as the Medicaid office losing paperwork that you submitted or determining that you no longer meet the requirements for Medicaid.
References
Why Coordinate Medicaid And Snap Renewals
About three-quarters of SNAP households had at least one member receiving Medicaid or CHIP in 2014. To qualify for SNAP, households generally must have gross income below 130 percent of the poverty line. Medicaid eligibility varies among states and types of participant. In states that have expanded Medicaid for adults under the ACA, the minimum eligibility threshold is 138 percent of the poverty line. In most states that havent expanded Medicaid, adults without children arent eligible at all and parents are eligible at lower income levels. Children in all states are eligible for either Medicaid or CHIP at income levels higher than the SNAP eligibility threshold.
Similarities also exist between SNAPs and Medicaids processes for applying and determining eligibility. Households newly applying for Medicaid and/or SNAP must submit an application with information on who is in the household, their citizenship and immigration status, and what income they receive. State or county eligibility workers verify that information using available data sources as well as documentation the applicant submits, such as pay stubs. After approval, participants must report certain changes in their income or household situation, and states periodically renew eligibility by examining information the participants report as well as available data sources to determine if households remain eligible.
Read Also: Medicaid Community Choices Waiver Program
Q How Much Income Can I Receive And Still Be Eligible For Medicaid
A. Income is money that you get from working, or money that someone gives you, or checks that you receive, such as a Social Security check, unemployment benefits, child support, retirement benefits, or sick pay. Whether your income level qualifies you or your family for Medicaid depends on the size of your family and the Medicaid program for which you are applying.
Income limits are set each year by the federal government to define the Federal Poverty Level for different family sizes. In general, if your household income is at or below the current 100% Federal Poverty Level for your household size, your family is likely to be eligible for Medicaid. Children from age 1 to under age 6 can qualify for Medicaid benefits when household income is at or below 133% of the Federal Poverty Level. Pregnant women and infants under age 1 qualify for Medicaid with family income at or below the 200% Federal Poverty Level, and pregnant women count as 2 family members.
See our tables of income limits for applying for DMMA programs to find out where your family income is, in relation to these income benchmarks.
Medical assistance programs other than Medicaid have different income level requirements. For example, uninsured children under age 19 who live in families with incomes at or below the 200% Federal Poverty Level are eligible for low cost health insurance under the Delaware Healthy Children Program.
Who Is Eligible For Medicaid
You may qualify for free or low-cost care through Medicaid based on income and family size.
In all states, Medicaid provides health coverage for some low-income people, families and children, pregnant women, the elderly, and people with disabilities. In some states the program covers all low-income adults below a certain income level.
- First, find out if your state is expanding Medicaid and learn what that means for you.
- If your state is expanding Medicaid, use this chart to see what you may qualify for based on your income and family size.
Even if you were told you didnt qualify for Medicaid in the past, you may qualify under the new rules. You can see if you qualify for Medicaid 2 ways:
- Visit your states Medicaid website. Use the drop-down menu at the top of this page to pick your state. You can apply right now and find out if you qualify. If you qualify, coverage can begin immediately.
- Fill out an application in the Health Insurance Marketplace. When you finish the application, well tell you which programs you and your family qualify for. If it looks like anyone is eligible for Medicaid and/or CHIP, well let the state agency know so you can enroll.
Read Also: How To Change Medicaid Plan Pa
Modified Adjusted Gross Income
MAGI is your adjusted gross income with tax-exempt social security, interest, or foreign income added in if you have any of these. The total amount is your modified adjusted gross income. Your adjusted gross income is your total income minus specific deductions. If you have multiple sources of income, they must all be added together in order to get your gross income.
How Can You Check Medicaid Coverage Status
To verify Medicaid coverage status, recipients can visit their states Medicaid website, contact a local Medicaid office by phone or visit a Medicaid office in person. Checking online is fast and convenient, but an in-person is better for in-depth question.
Medicaid provides medical insurance for low-income people, seniors, children, pregnant women and the disabled. Services are based on income and family size. All Medicaid programs follow federal guidelines, but these guidelines vary by state. For example, some state plans pay service providers directly, while others use private insurance companies. Information on Medicaid is available in languages other than English, even if the local office does not advertise multilingual services.
Also Check: Medicaid Recipient Fraud Investigation Process
Important Terms For Medicaid Qualification
Modified Adjusted Gross Income is your total gross income. This includes income from employment, other benefits, child support, alimony, interest, foreign income, etc. All your income sources are included.
Federal Poverty Level is the line designated by the Department of Health and Human Services to determine who is living in poverty.
How Do I Know If My Medi Cal Is Active
Medi-cal is a Medicaid program of the state of California that was initiated in 1966. It provides medical, vision and dental healthcare services to disabled and poor people. According to the Department of Health Care Services of California state, one-third of Californias population is registered for Medi-cal. It is almost a population of 13.3 million people. There are always some people who are not sure if their Medi-cal status is active. If you are wondering how do I know if my Medi cal is active, then keep reading.
When your Medi-cal status is active, you are able to get healthcare services from doctors and hospitals. There are five ways to find out if your Medi-cal status is active:
You May Like: How To Check My Medicaid Eligibility
How Does Medicaid Work
The Medicaid program does not provide health care services for everyone. Your application will be reviewed for all Medicaid programs. If you are found eligible for Medicaid, you will get:
- A letter in the mail from Medicaid telling you about your coverage
- A Medicaid ID card
- A Healthy Louisiana plan ID card, if you enroll in a plan.
Each time you go to your health care provider or pharmacy, take your Medicaid ID and Healthy LA plan ID cards with you. Show them at all medical visits before you receive any service. The health care provider or pharmacy will tell you if they accept your Medicaid benefits. You should also ask your health care provider or pharmacy if the service or prescription is covered by Medicaid before receiving the service or filling a prescription.
Medicaid does not pay money to you instead, it sends payments directly to your health care provider or pharmacy.
Q If I Dont Qualify For Medicaid Is There Any Other Help For Me Or My Children

A. Yes. Many organizations in Delaware are dedicated to the principle that health care should never be beyond the reach of those who need it. If you need health care, but do not have insurance coverage, the people at the Delaware HelpLine have a wealth of information about organizations that provide health care at reduced rates for uninsured individuals. Call the Delaware HelpLine toll-free at 1-800-464-HELP from Monday Friday from 8:00 a.m. to 5:00 p.m. The Delaware Helpline service is also available in Spanish. Additional information about the support provided by the Delaware Helpline can also be found by visiting www.delawarehelpline.org.
For example, you may qualify to receive discounted medical services through the Community Healthcare Access Program . CHAP helps connect uninsured individuals with affordable health care from primary care doctors, medical specialists, and other health providers including prescription programs, laboratory and radiology services. To find out more about this program, visit the website for the Community Healthcare Access Program, or call 1-800-996-9969 for eligibility guidelines.
You can read about CHAP and other healthcare resources for uninsured individuals in the Delaware Healthcare Resource Guide. This guide is also available in Spanish: Guía de Recursos de Salud.
Under 18:
You May Like: Can A Single Man Get Medicaid
New Mexico Medicaid Eligibility
In New Mexico, Medicaid eligibility is partially based on your household income, as well as other medical needs you may have . You must be a resident of the state to qualify for Medicaid.
Which Medicaid plan is best in New Mexico?
Many adults who receive Medicaid benefits are entitled to the New Mexico Alternative Benefit Plan . Though other recipients with special needs such as disabilities or serious medical conditions qualify for the states Standard Medicare plan. How you and your family qualify depends on your particular needs and financial situation.
You can submit an application through the YesNM website.
New Mexico Medicaid Application:
Can You Have A Medicare Advantage Plan And Medicaid At The Same Time
Medicare Advantage plans are Medicare plans offered by private insurers, while Medicaid provides health coverage for low-income eligible Americans. In some cases, you can have both at the same time if you qualify for dual eligibility.
- V.
What you should know
| 1. Medicare Advantage is a private Medicare plan, also referred to as Medicare Part C or MA plans. | 2. Medicaid is offered to those who meet low-income eligibility and covers additional health services that are not covered by Medicare. |
| 3. Dual eligibles can have both Medicare Advantage and Medicaid at the same time. | 4. Private healthcare providers offer specialized plans for dual eligibles that can coordinate Medicaid benefits with a Medicare Advantage plan. |
For those who meet income eligibility, Medicaid can be an important resource for covering healthcare expenses that Medicare does not. In addition, some people can benefit from having both Medicaid and Medicare Advantage, which is Medicare coverage through private insurance companies. Those who qualify are known as dual eligibles. Learn more about how it works.
Recommended Reading: How Much Does Medicaid Pay For Family Caregivers
This Article Offers An Overview Of How You Can Check The Status Of Your Health Insurance: How To Know Your Medi
Are you one of those people who say how do I know if my health insurance is active? If yes is the answer, then this article is for you. To keep your health insurance active, you need to regularly pay your premiums to the insurer. Every health insurance company has a different way to handle insurance payments. It is important that you follow the instructions of your health insurer to keep your health insurance active and valid. Some of the most popular health insurance companies in the United States are Medi-Cal and Medicaid. In some situations, people have health insurance but no card. Some people are not sure if they can use health insurance without a card. Keep reading this article to get the answers.
Q Can I Have Both Medicaid And Medicare At The Same Time
A. It depends. If you receive Supplemental Security Income from the Social Security Administration, you are automatically eligible for Medicaid and often receive Medicare as well. If you receive both Medicaid and Medicare, Medicaid will pay your Medicare premium, co-payments and deductibles. If you have both Medicare and Medicaid, you should show both cards to your medical care provider each time you receive services. Resources for Those Who Have Medicare and Full-Benefit Medicaid
Also Check: Can You Have Insurance And Medicaid
Manage Your Access Nevada Plan
Medicaid is an optional medical coverage program that states elect to provide to their residents. Depending on your income and family size, you or your family members may qualify for government-supplied healthcare, such as Medicaid. If you do qualify for Medicaid, there is no limited-enrollment period, meaning you can enroll at any time.
If you need to manage your Medicaid or Nevada Check Up plan, you can call 1-877-543-7669, visit Access Nevada, or visit the Division of Welfare and Supportive Services for a list of local numbers.
Can I Get Medicare Or Medicaid While Receiving Social Security Disability Payments
After being approved for disability benefits, whether you receive Medicaid or Medicare will depend on whether youre also getting SSI or SSDI benefits. Those who qualify for Supplemental Security Income are eligible for Medicaid, while those who receive Social Security Disability Insurance qualify for Medicare. However, SSD recipients wont receive medical benefits from Medicare until two years after their application has been approved. Those who receive SSI dont have to wait before receiving Medicaid. Lets take a closer look at SSI, SSDI, and Medicare/Medicaid.
Recommended Reading: Does Medicare Cover In Home Care For Seniors
You May Like: Dentist In Ashland Ky That Take Medicaid
Application Processing And Case Overview
Case ReviewAfter you submit an application for Mississippi Medicaid health benefits, the regional office that serves your county of residence will be in contact with you by phone or you may get a letter regarding your eligibility determination. If something is incorrect, missing or needs clarification a regional office staff member will contact you.
Case ApprovalIf you are approved to receive health benefits, a letter and a blue Medicaid identification card will be mailed to you. Mississippi Medicaid has a large network of health care providers available for medical services. When you make an appointment be sure the provider you choose accepts Mississippi Medicaid.
You may be eligible for health benefits through a coordinated care program called Mississippi Coordinated Access Network . Those who are automatically qualified for this program will have the option of choosing between one of three Coordinated Care Organizations : Magnolia Health, UnitedHealthcare Community Plan and Molina Healthcare. Mandatory populations are not eligible for dis-enrollment.
Those individuals who qualify for this program in an optional population have the choice to either enroll in a CCO or choose to stay in the traditional Medicaid fee-for-service program.
The Childrens Health Insurance Program is currently administered by Molina Healthcare and UnitedHealthcare Community Plan.
