How To Check Medicaid Status In Georgia
There are three main ways to check if you have active Medicaid in Georgia. You can contact your Eligibility Specialist directly, you can contact the appropriate Georgia Medicaid department or you can check online on the Georgia Gateway Customer Portal. When checking your status by phone, you will need your Medicaid case number.
The Georgia government’s website provides contact information for the Medicaid department. You may also have received your Eligibility Specialist’s direct contact information during your application process. If you do not have it, you can call the DFCS to request it. However, as long as your application has been registered in the system , the most expedient way to check is by going to the Georgia Gateway Portal.
Finally, you may find yourself at a doctor’s office or pharmacy when you need to know your Medicaid status. In this case, the doctor’s office or pharmacy can usually verify whether your Medicaid is active. They will need your full name and your Georgia Medicaid ID number, which is located on your insurance card.
How Do I Report An Address Change
Call Medicaid Customer Service toll free at 1-888-342-6207 or go online by visiting the Medicaid Self-Service Portal to update your address.
If you do not have an online account, you can create an account at any time. Creating an online account allows you to check the status of your application, report any household changes, report an address change, request a replacement Medicaid ID card, and renew your Medicaid benefits.
Your Original Medicare Premium Payments
They affect all of your Medicare coverage
To maintain continuous health coverage, make sure you always pay your Original Medicare monthly premiums on time. Many beneficiaries dont pay a Medicare Part A premium you dont have to pay this premium if you worked at least 10 years while paying Medicare taxes. However, most beneficiaries must pay a monthly Medicare Part B premium, even if theyre enrolled in Medicare Advantage or another Medicare plan option
If you receive Social Security, Railroad Retirement Benefits , or Civil Service benefits, your Medicare premium may be automatically deducted from those benefits. In other cases, you may have to make the Medicare payment yourself when you receive your monthly bill, or choose one of the payment options described below.
You can pay your Original Medicare premium in one of three ways: Sign up for Medicare Easy Pay, which is free and automatically deducts the premium payment from your checking or savings account pay by check or money order or pay by credit card.
Read Also: High Risk Ob Gyn That Accepts Medicaid
How Do I Know If My Child Is Due For A Texas Health Steps Checkup
Texas Health Steps will send you a letter when its time for your childs medical and dental checkups. You can also visit YourTexasBenefits.com or call the number below to find out if your child is due for a checkup.
Phone
Read Also: How To Find Your Medicaid Number
What To Watch For

Both mandate cases will now go back to the lower courts to decide whether theyll be permanently upheld or struck down. With the healthcare mandate now in effect, healthcare workers will be required to receive a first Covid-19 vaccine dose by January 27 and be fully compliant with the policy by February 28.
You May Like: Blue Cross Blue Shield Medicaid Dental Providers
Also Check: Aetna Better Health Of Ohio Mycare Ohio Medicare Medicaid Plan
Medicaid Offers A Full Range Of Health Services For Eligible Persons Including:
- All regular medical checkups and needed follow-up care.
- Immunizations.
- Eye care and eye glasses.
- Emergency care.
- Emergency ambulance transportation to a hospital.
- Hospital stays.
For some pregnant women, services may be limited to perinatal care if their incomes are too high to qualify for full Medicaid coverage.
For children birth to 21 years old, Medicaid offers the Child/Teen Health Program , which provides the services listed above for all Medicaid recipients. C/THP places an emphasis on preventive care and treatment. For example, Medicaid requires that all children be screened with a blood lead test at one and two years of age. C/THP is available from fee-for-service healthcare providers. Also, all managed care plans must offer C/THP to Medicaid recipients under 21 years of age who are enrolled in their plan.
Child Health Plus and Family Health Plus provide services to eligible children and adults, respectively, through managed care plans.
I’m Not Sure If I Am In A Medicaid Program Or Not How Can I Find Out Which Program I’m In
You can find out if you have Medicaid by phone or through the web.
Phone
Web
Note: If you are a legally authorized representative, you must click on the client drop-down menu on the upper right side, and choose a name from the list to see who has Medicaid and the plan and program names.
Don’t Miss: How To Obtain Medicaid In Florida
What Is A Dea Number
A DEA number is a unique identifier that enables medical practitioners to write controlled drug prescriptions. Two letters, six digits, and one check digit make up DEA numbers. DEA numbers are intelligent numbers, which means that some of the digits are meaningful.
The first letter denotes the category of registrant:
- B stands for clinics and hospitals.
- C for practitioners
- E for manufacturers
- The letter R stands for narcotic recovery services.
- The second letter is the first letter of the prescribers last name the number 9 is for prescribers who use their business address rather than their names.
- The remaining characters are numbers.
Verifying Eligibility For Enrolled Members
- Web Tool: As always, the web tool allows providers to obtain information online to determine whether an individual is enrolled in Medicaid. To access the web tool, providers should visit . Providers do not need to have a completed Authorized Representative agreement when submitting an inquiry on the web tool.
You May Like: Pediatricians In Fort Worth That Accept Medicaid
Can I Print My Card From The Web
Yes. If your computer is connected to a printer, you can print a paper copy of the Your Texas Benefits Medicaid card. You can see an electronic version using a smartphone or tablet.
Do I Need A Referral To See A Provider Other Than My Pcp
Yes. Most services from another provider require a referral from your PCP. You should get a referral before receiving the service. This is true even if it is a specialist, hospital service , or acute/urgent care visit. View the recipient handbook for a complete list of services that require a referral and services that do not. A referral can be made by your PCP via a telephone referral, physician order, prescription, referral card, or certificate of medical necessity.
Recommended Reading: Medicaid For Non Us Citizens
How Does Medicaid Work
The Medicaid program does not provide health care services for everyone. Your application will be reviewed for all Medicaid programs. If you are found eligible for Medicaid, you will get:
- A letter in the mail from Medicaid telling you about your coverage
- A Medicaid ID card
- A Healthy Louisiana plan ID card, if you enroll in a plan.
Each time you go to your health care provider or pharmacy, take your Medicaid ID and Healthy LA plan ID cards with you. Show them at all medical visits before you receive any service. The health care provider or pharmacy will tell you if they accept your Medicaid benefits. You should also ask your health care provider or pharmacy if the service or prescription is covered by Medicaid before receiving the service or filling a prescription.
Medicaid does not pay money to you instead, it sends payments directly to your health care provider or pharmacy.
What Do I Do With Medical Bills
Pay attention to the mail you get for medical care. If the bill says that you owe money, you should:
You may have to pay your own medical bills for Medicaid covered services if:
- You see a provider who is not part of your health plan
- You receive services without showing your Medicaid Member Card to the provider
You will have to pay the bill for services you get:
- When you were not eligible for Medicaid
- During an appeal, grievance or hearing if the action is denied
- If the services you receive are not covered by Medicaid
If you get services that Medicaid does not cover, you have to pay for the services yourself. You should sign a form that says:
If you receive about a bill from a medical provider, you talk to the provider about the bill, and you still have a question, call Medicaid Information at 801-538-6155 or toll-free at 1-800-662-9651.
Cannon Health Building
Also Check: Michigan Medicaid Prescription Coverage List
How To Check If My Medicaid Is Active
The Center for Medicaid and CHOP Services is the state and federal organization founded in 1965 by the US government to run medical assistance programs like Medicaid, the Basic Health Program , and the Childrens Health Insurance Program .
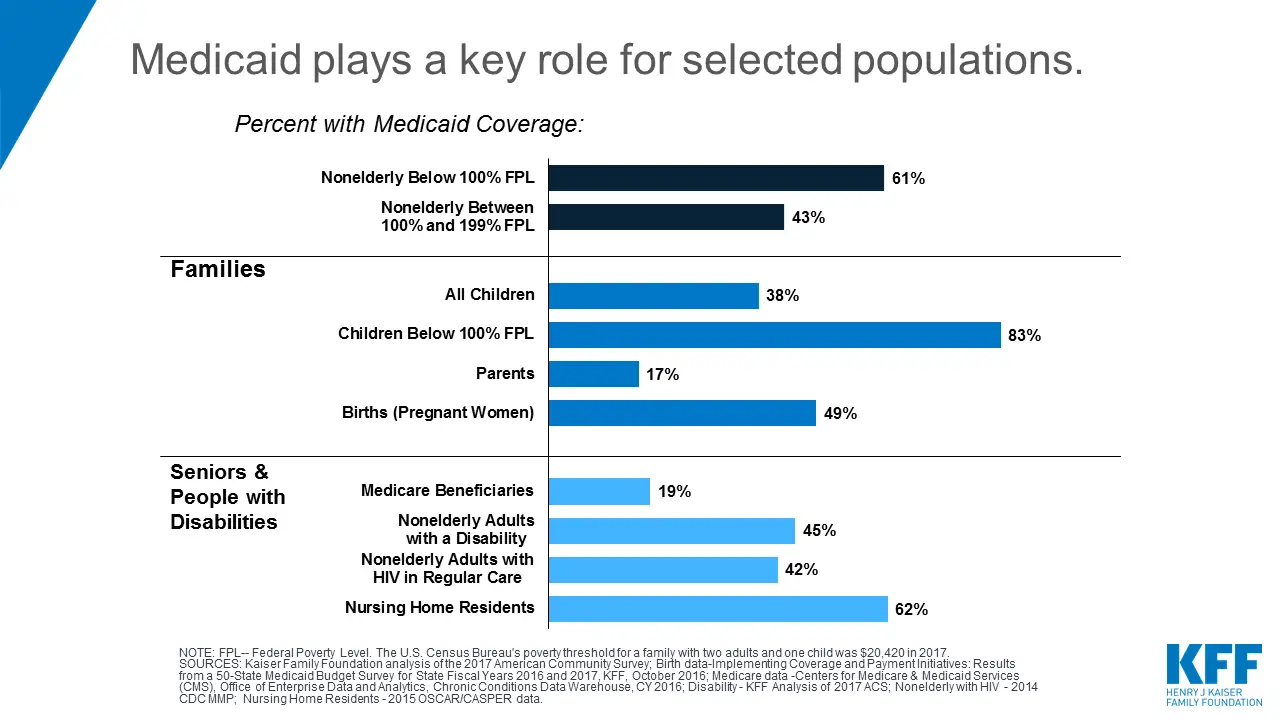
Medicaid is the one with the most coverage in the country, providing medical assistance to over 72.5 million American citizens. Its primary mission is to guarantee quality health to low-income families, qualified pregnant women, seniors, parents, and disabled people that are not capable of providing this service to themselves.
In this article, we will explain more about this subject, and specifically how to check if your Medicaid is active.
Contents
Speak With Case Manager
Your Case Manager is usually present at your local welfare office. When you contact the welfare office, tell them that you want to speak with your Case Manager. He will ask you to provide him with your Medi-cal identification number and your social security number. If you are wondering where you can find your Medi-cal identification number, then it is mentioned on your Beneficiary Insurance Card . In case you do not know who your Case Manager is, you can ask the local welfare office to provide you the required information. The local welfare office will also transfer your call to your Case Manager.
You May Like: Colorado Medicaid Phone Number For Providers
How Do I Find Out My Medicaid Application Status
Medicaid is a federally-funded health insurance program for low-income families that is administered by each state. The income requirements and types of coverage you get depend on state laws, but there are federal minimums that every state has to meet to qualify for funding. Each year, low-income families apply for Medicaid services that will allow them to get the health care they need. The application process can sometimes take a while, but there are ways to check the progress of your application.
Wait For The Letter
When your state Medicaid office receives your application, it will send out a letter that will give you a date you can expect coverage to start. At some point before that date, you should get insurance cards in the mail and a confirmation of the effective date. If you dont mind waiting, then you will get your application status mailed to you.
Look Online
These days, most states have an online application process set up for Medicaid that makes the process much easier. When you submit your application online, the website will create an account for you. If you ever want to check the status of your application, then you can just log into your online account and check.
Go To Your Medicaid Office
Make Your First Wellness Appointment
Call your doctor to schedule your initial wellness checkup. If you need help finding a doctor or scheduling an appointment, please call 1-800-962-8074, TTY 711,Monday through Friday, 8 a.m. to 6 p.m. local time.
You can also stop by our offices and a member of our team would be happy to assist you.
Our offices are located at:
2720 N. Tenaya Way, Suite 102Las Vegas, NV 89128
You May Like: What Does Share Of Cost Mean For Medicaid
Help With The Medicaid Application
When people initially apply for Medicaid through this portal, they are required to create accounts with usernames and passwords. This information should be kept in a secure location since it is needed to log in and access information.
For help with this and other questions, the Florida Medicaid phone number is 1-877-711-3662, TDD 1-866-467-4970. Hours of operation are Monday through Thursday 8 a.m. to 8 p.m. and Fridays 8 a.m. to 7 p.m. Frequently asked questions and enrollments can also be texted to 357662 or people without Internet access can call 1-888-367-6554 for assistance.
Read Also: Does Medicaid Give You A Free Breast Pump
How Can I Change My Address And Phone Number
You can change your address and phone number by visiting YourTexasBenefits.com. You can also make changes by phone.
Phone
Important: You must report changes to your case within 10 days of the change.
Note:
- If you get Social Security benefits or Supplemental Security Income, you must contact them first to update your information. If your address isn’t correct in the Social Security system, the wrong address will show up in our system too. Call the Social Security office at 800-772-1213 to correct your address. After that, visit YourTexasBenefits.com or call 2-1-1 or 877-541-7905 to correct your address.
- We won’t send you another Your Texas Benefits Medicaid card unless you ask us to send you a new card to replace one that has been damaged, lost or stolen.
Don’t Miss: Blue Cross Blue Shield Medicaid Dental Providers
Apply For Benefits In Person
Use The Online Portal

Another option is to use the MyBenefits CalWIN website to check your case status and benefits amount. The system also allows you to view any notices that were sent, such as requests for further documentation and whether you are eligible for additional assistance programs. If you don’t currently have a MyBenefits account, you’ll need to create one. Then you can go back and log in to see whether your Medi-Cal is approved and active.
Also Check: Medicaid Out Of Country 30 Days
The Florida Medicaid Portal
To qualify for Medicaid in the Sunshine State, Benefits.gov posts that an applicant must be a Florida state resident, U.S. national, U.S. citizen, permanent resident or legal alien who is low income and in need of health care and/or insurance help. Applicants must also check at least one of the following boxes: being 65 or older, responsible for a child aged 18 or younger, having a disability or a household family member with a disability, being blind or being pregnant. There are also income limits for Medicaid approval, with a chart to refer to. As an example, a household of four cannot be approved if their income is $35,245 per year or more.
Video of the Day
According to the American Council on Aging, it can take anywhere from 45 to 90 days for an application to be processed and then accepted or denied. The whole process from start to finish can take even more time and it can be frustrating for applicants to have to wait that long. This is why people are always trying to check their status through websites like the Florida Medicaid Portal.
Do You Need More Help
If you arent sure if your Medicaid coverage has been approved yet or if it is still active, you can check Manage My Case or call the states Automated Voice Recognition System at 1-855-828-4995 with your Recipient Identification Number .
If you have an urgent medical need and need Medicaid quickly, call the DHS Helpline at 1-800-843-6150.
Read Also: Can You Pay For Medicaid
