How Do I Know If I Qualify For Medicaid Services
If youre unsure whether you meet the Medicaid qualifications and income requirements, you can use a Medicaid calculator. Simply enter your information, including your state/zip code, income, household size and the number of adults and children you want to enroll.
Health For California is here to help you determine your Medi-Cal eligibility. Our free agents are always available to answer your question. If you want to enroll yourself or your family in Medi-Cal, get your free quote today.
Not sure how Obamacare affects your health care plans in California? Learn how the ACA works in California, including benefits, costs and enrollment.
How Much Does Medicaid Cost In Texas
There are a variety of Medicaid programs in Texas from traditional Medicaid to a Medicaid Buy-in program. Like any health program, Medicaid is subject to copay and deductibles. But the Medicaid Buy-in program operates more like traditional insurance for the working disabled. The monthly premium depends on a variety of factors including income. There is no way to know the exact premium you will have to pay without first applying.
When And Why Was The Federal Poverty Level Established
The federal poverty thresholds were first introduced in 1965, based on the work of the Social Security Administrations Mollie Orshansky. The amounts were tied to the bare minimum amount that people needed in order to have adequate food, with a multiplier used to account for other necessary expenses. Orshansky noted at the time that the poverty thresholds were a measure of the amount of income that would be inadequate for people to live, as opposed to a minimum adequate amount.
Don’t Miss: Does Disability Count As Income For Medicaid
Who Can Get Medicaid
- No matter your state, you may qualify for Medicaid based on your income, household size, disability, family status, and other factors. But if your state has expanded Medicaid coverage, you can qualify based on your income alone.
- Enter your household size and state. We’ll tell you who is eligible for Medicaid, if your state expanded and if you qualify for Medicaid based only on your income.
- If you think you have Medicaid eligibility, you can create an account and fill out a Marketplace application. If it looks like anyone in your household qualifies for Medicaid or CHIP, we’ll send your information to your state agency. They’ll contact you about enrollment. You can apply any time of year.
- If you don’t qualify for Medicaid, we’ll tell you if you qualify for financial help to buy a Marketplace health plan instead.
Work Requirements And Medicaid In 2018 And Beyond
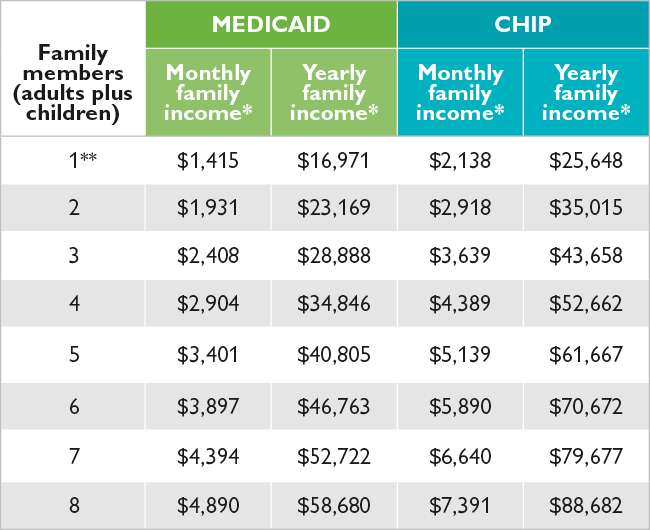
In April 2021 President Joseph Biden began unwinding the previous administrations attempts to create and implement new eligibility requirements for adults without children or disabilities. These requirements would have allowed states to remove Medicaid coverage from childless adults who are not disabled, who do not have jobs, or are not involved in work-related or volunteer programs. Even states that received approval had not enforced work requirements as of April 2021, because federal courts invalidated the rules.
In an effort to encourage states to expand Medicaid, President Bidens 2021 American Rescue Plan contains more matching of federal funds as an incentive. The U.S. Department of Health and Human Services has now revoked work requirements in the Medicaid programs of Arizona, Arkansas, Indiana, Michigan, New Hampshire, Ohio, South Carolina, Utah and Wisconsin. Kentucky and Nebraska withdrew their applications for work requirements after initially receiving approval.
According to the Pew Charitable Trusts, at least 15 states either applied for or received permission to impose work requirements during the previous administration. The nonpartisan research and policy Center on Budget and Policy Priorities reported that in 2018, Arkansas removed more than 18,000 Medicaid beneficiaries off the rolls because they did not meet new eligibility requirements.
Don’t Miss: Does Medicare Or Medicaid Cover Cremation
Does Medicaid Check Your Tax Returns
How does Medicaid determine who is in a household? Medicaid determines an individuals household based on their plan to file a tax return, regardless of whether or not he or she actual files a return at the end of the year. Medicaid also does not require people to file a federal income tax return in previous years.
Medicaid Eligibility In Maryland
Medicaid is a nationwide program that provides free and/or affordable health care coverage for millions of citizens including children, expectant mothers, seniors, individuals with disabilities, and low-income families. Benefits include primary care, prescription, dental, eye care, hospitalizations, specialized care, and mental health services.
Also Check: How Do I Add Someone To My Medicaid
Is Inheritance Considered Income For Medicaid
When a Medicaid recipient receives an inheritance, it is counted as income in the month that it is received. Not only must a Medicaid applicant meet this asset limit in order to qualify for benefits, he / she must maintain his / her assets at, or below, this level.
Q What Documents Will I Need To Provide When I Apply
A. You will need to provide verification of your income. You do not need to provide proof of your assets or resources or come into our offices to be interviewed unless you are applying for one of the Long Term Care Medicaid programs .
If you are pregnant, you will need to provide proof that you are pregnant. If you are not a U.S. citizen, you will need to provide proof of your alien status. For example, you can provide a copy of your green card.
If you apply online using ASSIST, a web page at the end of the application will tell you exactly what documents must be sent by mail to support the application you are submitting, and the appropriate mailing address.
Read Also: New Mexico Medicaid Provider Portal
Q Where Do I Go To Apply For Medicaid
A. There are several ways to apply for Medicaid and other medical assistance programs:
- On the internet, you can use ASSIST to check your eligibility for several different assistance programs by completing a self-screening questionnaire. ASSIST then allows you to apply online.
- You may also print an Application for Health Insurance/Medicaid. The application form is also available in Spanish/en Español.
- By phone, you can contact Medicaid Customer Relations at 1-800-372-2022 or 255-9500 to be directed to the Division of Social Services office closest to where you live. DSS staff members will help you find out more about eligibility for Medicaid and other assistance programs. Then the appropriate information and application forms will be mailed to you. Complete, sign and date the application form in ink and mail it to the address provided.
- For Long Term Care applications, please call the Long Term Care Medicaid Unit listed for the county where you live.
How Much Does Medicaid Cost In Virginia
Cost estimates will vary from person to person and the health services needed will also be a factor. If you have a copay, they are typically small and most of the time do not exceed $30. Visits to the clinic, doctor, or eye doctor cost as little as $1. Things like outpatient hospital visits, home health visits, or rehab cost as little as $3. If you are admitted to the hospital, the cost will be $100.
Cost and Coverage of Medicaid in Virginia Medicaid services that may be provided include care for babies, dental, durable medical equipment and supplies, early and periodic screening, diagnosis and treatment, family planning and birth control, long-term care, prescription drugs, clinic services, community-based residential services, and mental health services.
Also Check: Does Missouri Medicaid Cover Assisted Living
Medicaid Eligibility & Requirements In California
Medi-Cal, Californias Medicaid program. Medi-Cal allows low-income seniors, adults and children to gain access to health care and medical services, among other programs.
You may qualify for health and medical insurance coverage at little or no cost if you meet the Medicaid eligibility requirements and guidelines below.
Calculating Your Cpp Benefit
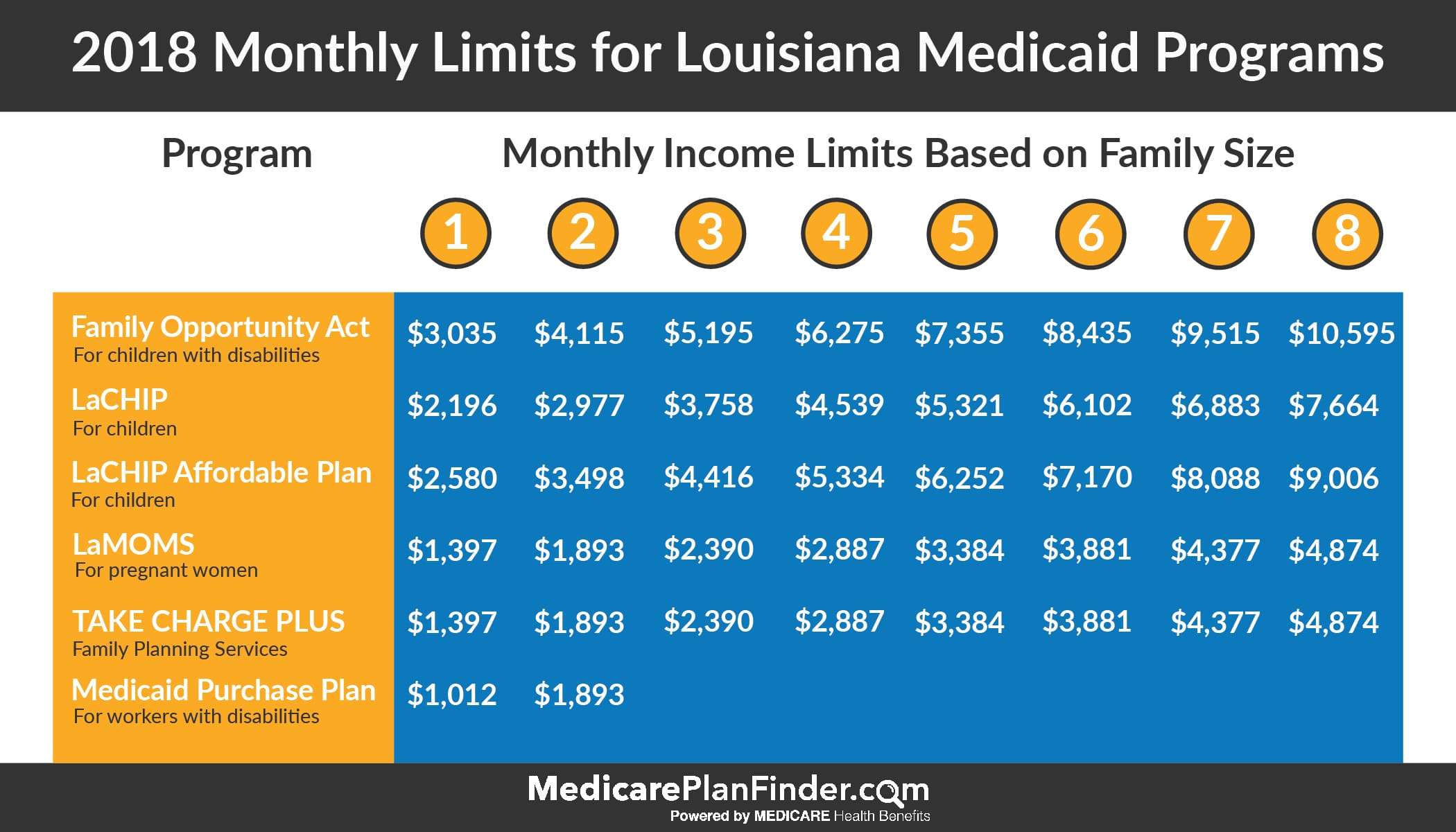
To know how much CPP youll get, you need to calculate your benefit. It goes off a number of factors:
- How long you worked.
- How much you paid in.
- The age at which you took the benefit.
- Whether you have other pension income .
Doing all the CPP calculations by hand can be tough. So, I recommend using the retirement income calculator on Canada.ca. This online app walks you through a series of questions that leads you to an estimate of your monthly CPP benefit. It may not be 100% accurate, but it should be in the right ballpark.
Read Also: General Doctor That Accepts Medicaid
How To Apply For Medicaid In Texas
You can apply online for benefits. You will need to be prepared to answer questions about the following for each family member:
- Social Security number and birth date
- Citizenship or immigration status
- Money from jobs and other sources
- The value of cars and other property
- Costs you pay for bills
You can also call 211 if you are in Texas. Alternatively, you can dial 1-877-541-7905 Monday to Friday, 8 a.m. to 6 p.m.
You can also visit a community partner in person. Printing and mailing a copy to HHS is also an option
Illinoiss Requirements For Medicaid Qualification
The state of Illinois sets particular requirements for enrollees to qualify for the Medicaid program. First, certain income standards must get met if residents in the area hope to qualify. What was once given to children and pregnant women is now available for women and men as well, as long as they meet the criteria. Those who fall far above the poverty level cannot receive this state insurance. If you would like to find out if you should apply, use the Check If I Should Apply button on the Application for Benefits Eligibility website. It asks questions regarding your family size, age, gender, taxes, health coverage through work, medical needs, and more.
Don’t Miss: How To Find Your Medicaid Number
Medicaid And Medicare Dual Eligibility
If you qualify for both Medicare and Medicaid, you are considered dual eligible. In this case, you may qualify for a certain type of Medicare Advantage plan called a Dual Eligible Special Needs Plan . D-SNPs are designed to meet the specific needs of people who have Medicaid and Medicare.
You can compare plans online to find out if D-SNPs are available where you live, or you can call to speak with a licensed insurance agent for information about eligibility and enrollment.
District Of Columbia Medicaid
Eligibility overview: Washington, D.C., has one of the most generous Medicaid programs in the U.S., covering adults with household incomes up to 215% of the FPL as part of its expansion program. It also has programs for pregnant, parent/caretaker, elderly, disabled and child residents.
Income requirements: The expansion covers adults without dependents who make up to $2,082 a month when applying on their own. Elderly, blind or disabled D.C. residents are eligible if they make up to 100% of the FPL, or $1,073.33 per month for one individual, and have resources below $4,000 for one person. D.C. also covers pregnant women with incomes up to 319% of the FPL, or $4,703.40 monthly for a two-person household, and parents/caretakers with incomes up to 216% of the FPL.
How to apply for Washington, D.C. Medicaid: You can apply online at DC Health Link or by visiting your closest Income Maintenance Administration Service Center.
Other notable programs: Long-term care and nursing home care services Spend Down, a Medicaid program for people who exceed income limits, but have high medical bills Emergency Medicaid for people who canât qualify for standard Medicaid due to citizenship/immigration status.
Also Check: Can You Apply For Medicaid If You Have Insurance
Which Medicaid Plan Is Best In Texas
There is no best Medicaid program. There is only the program that is best for you. Again, this is something best determined by a consultation with someone from Health and Human Services. Medicaid and CHIP cover half of all children in Texas. If yours is a low-income family, or you are an individual that meets other Medicaid qualifications, there is a very good chance that one of the programs is right for you.
Do I Qualify For Medicaid Ohio
To be eligible for Ohio Medicaid, you must be a resident of the state of Ohio, a U.S. national, citizen, permanent resident, or legal alien, in need of health care/insurance assistance, whose financial situation would be characterized as low income or very low income. You must also be one of the following: Pregnant, or.
Don’t Miss: Can I Get A Replacement Medicaid Card Online
Medicaid Income Eligibility Requirements
If you meet the qualifications above, you must also show you have financial hardship by meeting the income eligibility requirements. To see if you meet the Medicaid requirements for income, you must examine your family size the number of people living in your household and your modified adjusted gross income your total income from all sources.
Your household income must not exceed more than 138 percent of the federal poverty level based on your household size. For example, if you live alone, your income cannot be more than $16,395 a year. If you live with a spouse or another adult, your combined income cannot be more than $22,108 a year.
To qualify based on your family size, your household income cannot exceed:
- One: $16,395
- Physical and occupational therapy
- Preventive and wellness services and chronic disease management
- Dental and vision care
What Does Medicaid Cover In Maryland
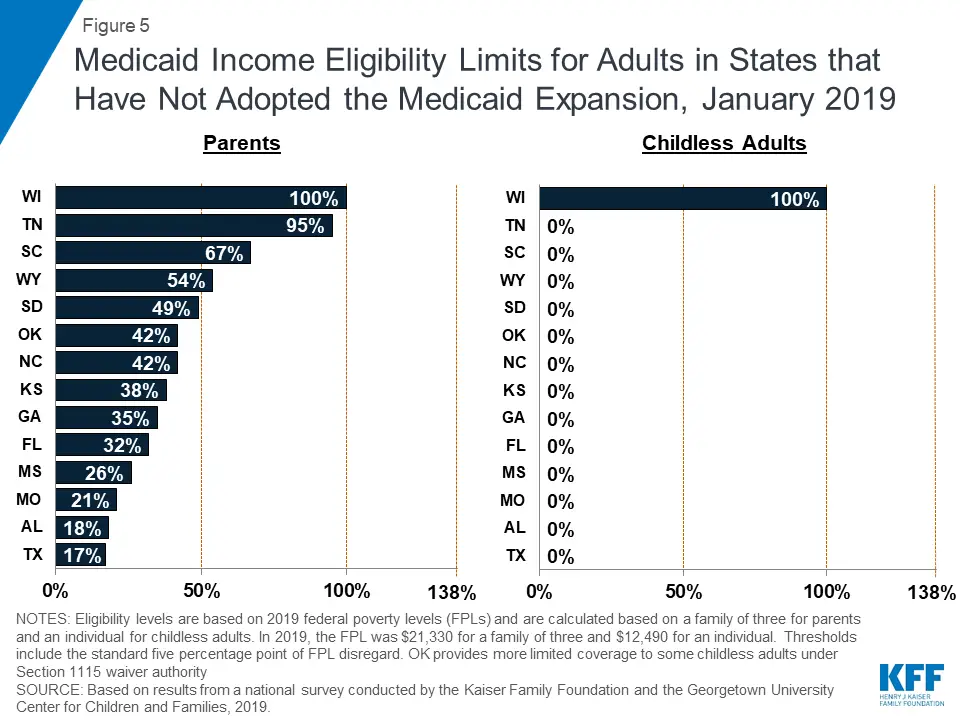
Medicare in Maryland covers several medical services including:
- Ambulance travel and emergency services
- Clinic services
- Screening, diagnosis, and treatment services
- Eyewear
- Inpatient and outpatient hospital care
- Labs and x-rays
- Vision
- Substance abuse treatment
Your chosen Managed Care Organization will cover the cost of visits to the doctor, prenatal care, prescription drugs, hospital and emergency services, and primary mental health services.
You May Like: Braces Place That Take Medicaid
Texas Medicaid Application And Qualifications
It is easy to confuse Medicaid with Medicare. The two programs are not without their similarities. One key difference is that Medicare is a federal program, whereas Medicaid is a state program with rules that vary depending on where you are. The other major difference is that Medicare is based largely on age and disability, while Medicaid is based largely on income.
Depending on your circumstances, you can be on both at the same time. Circumstances is the key word. Medicare tends to be long-term, if not permanent. Medicaid is often a shorter-term solution. There are other programs that are generally associated with Medicaid such as financial and grocery assistance. It is possible that if you have qualified for these other forms of assistance, Medicaid will be included.
What To Do If Your Cpp Payout Is Weak
If youre already about to retire and your CPP payout looks like it will be low, one thing you can do to enlarge it is to wait longer to take it. This results in a steady increase for every year of postponement. While youre waiting on your retirement date, you can invest your paycheque into funds like XIU and re-invest the dividends for a dependable supplement to whatever youll ultimately get in CPP. In retirement, every penny counts. So, make it!
This article represents the opinion of the writer, who may disagree with the official recommendation position of a Motley Fool premium service or advisor. Were Motley! Questioning an investing thesis even one of our own helps us all think critically about investing and make decisions that help us become smarter, happier, and richer, so we sometimes publish articles that may not be in line with recommendations, rankings or other content.
Fool contributor Andrew Button owns iSHARES SP TSX 60 INDEX FUND. The Motley Fool has no position in any of the stocks mentioned.
Also Check: Does Medicaid Cover Gym Memberships
Can You Make Too Much Money For Medicaid
If your income is too high to qualify for Medicaid, you can buy insurance through the Health Insurance Marketplace. Based on the state you live in, your eligibility to buy insurance through the Health Insurance Marketplace will start at the income level you no longer qualify for Medicaid.
Taking Advantage Of Magi
The Affordable Care Act simplified Medicare eligibility and enrollment for millions of Americans. Using MAGI for eligibility simplified the application process. The administrative burden of confirming assets was put to the wayside. Unfortunately, it also gave wealthy people the opportunity to take advantage of taxpayer dollars.
This loophole occurs because the majority of Americans now qualify for Medicaid through MAGI, which unless you are seeking long-term nursing home care no longer uses the asset test. People who are asset rich, particularly those who have investments or real estate properties, can still technically meet MAGI criteria.
Someone could own a home worth $850,000, a Lamborghini, a second vehicle, hundreds of acres of farmland, and still technically be eligible for Medicaid.
These Americans would be considered wealthy by any standards but by sheltering their net worth under the current tax laws, they would be legally eligible for Medicaid or subsidized plans through the Health Insurance Marketplace. This is the case even when they could easily dip into their assets to pay for health insurance.
If the intent is to provide health care to the most financially needy, MAGI Medicaid may need to consider how it addresses this loophole. The GOP is currently looking to repeal Obamacare which would, in effect, put an end to MAGI Medicaid altogether.
Recommended Reading: Having A Baby On Medicaid
