Medicare Part D Premiums
Medicare Part D is prescription drug coverage. Part D plans have their own separate premiums. The national base beneficiary premium amount for Medicare Part D in 2022 is $33.37, but costs vary.
Your Part D Premium will depend on the plan you choose. Just like with your Part B coverage, youll pay an increased cost if you make more than the preset income level.
In 2022, if your income is more than $91,000 per year, youll pay an IRMAA of $12.40 each month on top of the cost of your Part D premium. IRMAA amounts go up from there at higher levels of income.
This means that if you make $95,000 per year, and you select a Part D plan with a monthly premium of $36, your total monthly cost will actually be $48.40.
Determine Your Asset Limit
Before applying for medicaid, it is important to determine the asset limit as it varies for married applicants and single applicants and from state to state.
Most married couples, when both spouses are applicants, can retain up to $3,000 of the countable assets . However, for an individual applicant, this rule is based on the state in which the applicant resides. The asset limit is also based on the applied Medicaid program.
Individual Applicant
The standard asset limit for single Medicaid applicants is $2,000 in countable assets, but this also depends on the state of residence.
For More information on Medicaid income and asset spend-down contact our qualified and experienced Colorado trust and estate planning attorneys through the contact link on our website.
Aca Medicaid Eligibility Expansion In Colorado
One of the Affordable Care Acts primary strategies for reducing the uninsured rate is Medicaid expansion to cover low-income adults under the age of 65.
Medicaid expansion was a required element of the ACA as originally written. However, a coalition of states challenged Medicaid expansion and several other provisions of the ACA, and the case ended up before the Supreme Court in 2012. While the Court rejected most of the challenges, it did rule that Medicaid expansion was optional.
Fortunately for Colorados uninsured residents, the state opted to expand Medicaid. Then-Governor John Hickenlooper signed the legislation authorizing Medicaid expansion in May 2013.
As of late 2013, when the exchanges and Medicaid expansion were first up and running, about 45% of Colorados 737,000 uninsured qualified for Medicaid or CHP+ according to the Kaiser Family Foundation. And under the ACA, another 22% qualified for premium subsidies to help them afford private health insurance through the health insurance marketplace.
Coupled with the widespread job losses in the early days of the pandemic, Medicaid/CHIP enrollment has grown significantly across the country in 2020 and 2021. By early 2021, Medicaid enrollment in Colorado had surpassed 1.5 million people, and was nearly double what it had been in 2013.
As of December 2020, Medicaid expansion enrollment in Colorado was 488,200, accounting for nearly a third of the states total Medicaid/CHIP enrollment.
Read Also: Medicaid Health Insurance Income Limits
What To Do If You Don’t Qualify For Medicaid
If you don’t qualify for Medicaid, you can possibly get subsidized health care through the Obamacare marketplaces during a special enrollment or open enrollment period. Americans who making more than 100% of the FPL qualify for a premium tax credit that can significantly lower the cost of a plan.
Federal open enrollment for 2022 health care plans runs until Jan. 15, 2022, though some state exchanges are open longer. Learn 2022 open enrollments dates by state. Healthcare.gov, the federal exchange, usually opens from November 1 to December 15 each year.
If you can’t find affordable health care on your marketplace during open enrollment, you have a few back-up options.
These include:
Short-term health insurance: Originally designed to prevent short-term health insurance gaps, these plans are cheaper, but much less comprehensive than traditional coverage. They don’t have to cover Obamacare’s 10 essential benefits or pre-existing conditions. Following changes by the Trump administration, short-term health plans can last from three months to potentially three years, though som estates have stricter limits.
Limited benefit plans: These plans cover a very small portion of the costs associated with certain “medical events,” like a doctor’s visit or ambulance ride. Both the number of events and dollar amounts covered are capped.
Colorado Long Term Care
Colorado is an income cap state for 2021, meaning that in order to be eligible for Medicaid long term care benefits there is a hard income limit. Non income cap states allow applicants to spend down money for their care, whereas income cap states require the amount to be no higher than their limit at time of application.
Unlike traditional Medicaid sponsored long term care, Colorado has what they call a long term care partnership. The partnership melds together private insurance and state funds. This is a beneficial system for recipients who do not wish to deplete all of their assets paying for care. It is designed to reward residents who have planned ahead for their long term care needs. Colorado allows insurance companies to sell LTC partnership policies and guarantees that for every dollar paid out by an LTC partnership plan, a dollar of the recipients personal assets can be protected. Protected assets are ignored when reviewing an applicants financial eligibility and during estate recovery after a long term care recipients death. LTC partnership policy holders who apply for Medicaid are able to keep assets above the $2,000 Medicaid asset maximum.
Types of Care in 2021:
Long Term Care Services can cover a nursing facility stay or community based services . An individual receiving HCBS is not required to make a payment towards the cost of care.
NOTE:
Also Check: Does Medicare Or Medicaid Pay For Glasses
Option 1 Apply Online
You can apply online through the MI Bridges Portal as shown in the image below.
If you have an account, you can log in or create your MI Bridges Account. to be taken to the website.
The video below, by the Michigan HHS does a great job of explaining how to apply online for benefits with MI Bridges.
We highly recommend you watch it if you are applying online for Michigan Medicaid.
Additional Ui Design And Readability Adjustments
Also Check: Does Medicare Or Medicaid Cover Cremation
How To Qualify For Medicaid
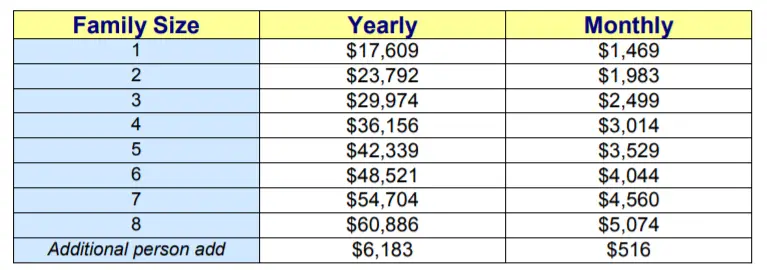
Almost every state has multiple Medicaid programs. But, as a good rule of thumb, if you make less than 100% to 200% of the federal poverty level and are pregnant, elderly, disabled, a parent/caretaker or a child, thereâs likely a program for you. And if you make less than 133% of the FPL**, thereâs possibly a program for you, depending on whether your state expanded Medicaid under Obamacare. In 2021, the federal poverty levels range from $12,880 to $44,660 .
In 2021, the federal poverty level in Alaska ranges from $ $16,090 to $55,850 . The federal poverty level in Hawaii ranges from $14,820 to $51,360 .
What Are The Income Rules In Colorado On Medicaid
Do you think you have too many assets to qualify for Medicaid assistance with nursing home costs? Think again.
At The Hughes Law Firm, P.C., in Denver, we help people just like you qualify for Medicaid benefits as well as provide assistance with many issues of elder law, VA benefits and estate planning. Let our lawyers help you understand how Colorados Medicaid income rules work.
Read Also: Is Invisalign Covered By Medicaid
Make Allowable Spend Down Payments And Purchases
Some payments for permissible expenses and purchases of non-countable assets can be made to reduce the value of your assets to qualify for Medicaid, for example:
- You can pay your nursing home bills
- Pay outstanding debt like mortgage payments and credit card bills
- Pay property taxes, income taxes, and capital gains taxes
- Pay for home repairs
- Purchase household goods and personal effects and
- Buy a new car.
Medicaid Eligibility In :
- Eligibility is determined by an applicants local county department of social services.
- Medicaid has both financial and medical related requirements.
- Income limit Up to 300% of the Social Security Income rate, adjusted annually. There is a personal needs allowance of $84.41 per month that is not factored into the countable income
- Resource limit $2,000 for individuals and $3,000 for couples both on Medicaid LTC.
- Must be 65+, or disabled, or blind.
- OR the applicant must be in a medical institution for 30+ consecutive days , receiving nursing facility level of care in the community for HCBS, or a combination of both.
An individual receiving Medicaid LTC Services in a LTC facility is required to make a monthly payment towards the cost of care to the facility. The payment is based on gross monthly income with deductions.
The countys department of human services configures the payment towards the cost of care as follows:
- Gross monthly income
- Minus $80 of personal needs allowance
- Minus potential deductions:
- Additional miscellaneous allowances allowed by law
Assets/Resources for 2021: Resources are divided into two categoriescountable and exempt.
Countable resources include: cash, checking accounts, savings accounts, CDs, mutual funds, IRAs, investment portfolios, bonds, life insurance policies totaling more than $1500, vehicles if more than one is owned, properties.
Spousal Rules in 2021:
Read Also: Does Medicaid Cover Substance Abuse Treatment
Planning For Medicaid Approval May Involve Gifts Or A Trust
There are many ways in which you can reduce the value of the assets the government will consider during the Medicaid application process. One of the simplest and most direct is to begin distributing some of your assets to loved ones and family members. Instead of leaving everything as an inheritance when you die, you can choose to strategically gift items and assets to your family members and heirs to reduce the total value of your possessions.
If you worry about how such distributions could impact your family or that they might result in the misuse of your assets, the creation and funding of a trust can be another means by which to insured Medicaid eligibility. You can place many assets in a trust, from financial accounts to the title for your home. So long as you do so at least five years before you apply for Medicaid, those assets should have protection from liquidation to pay for medical expenses.
Medicaid Expansion: The Bottom Line
Clearly, Medicaid expansion in Colorado has cost much more than initially projected.
And even with the federal government footing most of the bill, state policymakers will continue to confront tough budget choices as Colorados portion of the cost increases over the next years.
The budget for HCPF, the state department that administers Medicaid, has accounted for a larger portion of the states General Fund over the past decade, increasing from 17 percent in FY 1999-2000 to 24 percent in the FY 2016-17 budget request. Other parts of the budget, including education, have shrunk over that time.
A good deal of this increase for HCPF relates to the cost of Medicaid. Not only will Colorados expansion require additional spending, the states traditional,
non-expansion Medicaid spending which currently averages a little over $4 billion annually7 will continue to grow as well.
While it is important to analyze the costs of Medicaid expansion, it is also important to consider the benefits.
Research by the National Academies Health and Medicine Division has found that access to care, quality of care, sickness and even life expectancies are worse for uninsured Americans.
States may save money by reducing spending on programs for the uninsured. Some research has found that these cost savings outweigh the price of Medicaid expansion, even as states begin to pay a larger share.
| 0-200% FPL |
Also Check: How To Renew Medicaid Ny Online
Sudden Growth: The First Two Years
Colorado saw 289,000 residents enroll in Medicaid due to expanded eligibility in FY 2013-14 and FY 2014-15.2
This expansion group made up nearly one of four of the states 1.2 million Medicaid beneficiaries by June 2015.2 Most of the expansion enrollees were newly eligible for the program. But 12 percent, or one of eight, were welcome mat enrollees, which means they were already eligible under pre-expansion criteria but hadnt yet signed up for Medicaid.
The difference is crucial because the federal government reimburses half of the cost for the care of welcome mat enrollees, the same rate as the rest of the states traditional Medicaid enrollees, not the full 100 percent that is reimbursed for the newly eligible.
The expansion costs added up to nearly $1.6 billion during the first two years 29 percent more than the $1.2 billion forecasted by the fiscal note for the authorizing legislation.
Costs exceeded projections primarily due to the unexpectedly high enrollment. Caseload growth was 71 percent higher than anticipated. But per capita costs were actually lower than predicted, which kept total costs from exceeding forecasts even more.
On average, each expansion enrollee both newly eligible and welcome mat enrollees cost approximately $4,100 annually in the first two years. Projections had anticipated spending approximately $5,200 per enrollee.
Adults without kids were one of the more expensive groups on a per capita basis, costing an average of $4,600 a head.
District Of Columbia Medicaid
Eligibility overview: Washington, D.C., has one of the most generous Medicaid programs in the U.S., covering adults with household incomes up to 215% of the FPL as part of its expansion program. It also has programs for pregnant, parent/caretaker, elderly, disabled and child residents.
Income requirements: The expansion covers adults without dependents who make up to $2,082 a month when applying on their own. Elderly, blind or disabled D.C. residents are eligible if they make up to 100% of the FPL, or $1,073.33 per month for one individual, and have resources below $4,000 for one person. D.C. also covers pregnant women with incomes up to 319% of the FPL, or $4,703.40 monthly for a two-person household, and parents/caretakers with incomes up to 216% of the FPL.
How to apply for Washington, D.C. Medicaid: You can apply online at DC Health Link or by visiting your closest Income Maintenance Administration Service Center.
Other notable programs: Long-term care and nursing home care services Spend Down, a Medicaid program for people who exceed income limits, but have high medical bills Emergency Medicaid for people who canât qualify for standard Medicaid due to citizenship/immigration status.
Don’t Miss: Residential Treatment Centers That Accept Medicaid
Are There Too Many Nursing Homes In Colorado
One year into the coronavirus pandemic, nursing homes across Colorado are feeling significant financial strain. Two of the states largest nursing home operators are seeking to transfer a combined 29 facilities to new management. Residents of long-term care facilities have accounted for 40 percent of Colorados COVID-19 deaths.
Who Is Eligible For Medicaid In Colorado
Since 2016, Colorado Medicaid has been called Health First Colorado. Each state sets eligibility criteria for the covered populations, which must meet minimum standards set by the federal government.
Colorados income limits for Medicaid qualification are:
- 147% of FPL for children ages 0-18 children with family incomes up to 265% of FPL qualify for Child Health Plan Plus
- 200% of FPL for pregnant women pregnant women with family income up to 260% of FPL qualify for CHP+
- 138% of FPL for adults under the age of 65
Note that income refers to an ACA-specific version of modified adjusted gross income . All of the above income limits include a 5% income disregard thats added to MAGI for the purposes of determining Medicaid/CHIP eligibility for children, pregnant women, and nonelderly adults.
Colorado is also one of the states that uses state Medicaid funds to provide coverage for lawfully present children and pregnant women who have not yet been in the U.S. for five years . This has mostly been the case since 2009, but the provision was extended to apply to all income-eligible, lawfully present children and pregnant women.
You May Like: Dentist In Lafayette That Accept Medicaid
Colorado Medicaid Expansion Update
Colorado opted to expand Medicaid and Gov. John Hickenlooper signed the legislation authorizing Medicaid expansion in May 2013.
Medicaid enrollment in Colorado grew by 73 percent between late 2013 and late 2017, driven mostly by the expanded eligibility rules.
As of June 2019, Medicaid expansion enrollment in Colorado was 380,400.
The Truth About Calculating Assets For Medicaid Eligibility
In Colorado, the general rule is that you are not eligible for Medicaid if you have more than $2,000 in countable assets, including investments and bank accounts. While this number may seem unrealistically low, it is important to remember that there are several assets you dont have to include when calculating your total countable assets.
There are a number of exemptions when applying for Medicaid. These exempt assets include:
Keep in mind that the income and asset rules above are merely a basic outline of how Medicaid asset limitations work, and they can change from year to year. At The Hughes Law Firm, P.C., we will help you understand your options, including:
- Gifts
Recommended Reading: Pregnancy Medicaid Florida Phone Number
