Misconception : Someone Told Me That Medicaid Will Take My Parents House To Pay For The Nursing Home
Depending on the situation, you can in fact be forced to sell your home to help pay for long-term care. This can occur once you have spent down your assets and successfully applied for Medicaid.
There are, however, protections against losing your home. If the Medicaid beneficiary and/or their spouse is a permanent resident of the house, they cannot lose it. The basic rule is that a persons primary residence is an exempt asset and therefore, will not be counted when they apply for Medicaid, says Beisker. If a Medicaid applicant is married and their spouse continues to live in the home , then the home is exempt regardless of its value.
Beisker says that once a Medicaid recipient has died, the state may seek repayment of its outlays for the seniors long-term care. This has become increasingly common as more seniors require long-term care but do not have the personal funds to pay for it. The Medicaid Estate Recovery Program recoups this money by filing claims against any assets a Medicaid recipient held an interest in at the time of their death, such as a home. However, if a senior died without any assets , then there is no way for the state to be repaid.
Medicaid For Texans Needing Home Health Care
Texas covers home health services under its Medicaid program. If your doctor prescribes home health services like nursing or therapy services in your plan of care for a particular medical condition, Medicaid will cover those. Medicaid reviews your need for home health care every 60 days. You do not need to meet the nursing home level of care to qualify for home health services. However, because these Medicaid-funded home health services are related to a doctor’s plan of care for a particular medical condition, they are generally offered on a short-term basis.
If you otherwise qualify for Medicaid, and if your doctor says that you have a medical condition that causes you to need assistance with one or more activities of daily living, then you may qualify for Primary Home Care , a Texas program providing long-term care services at home. Activities of daily living are those like bathing, getting dressed, doing routine hair and skin care, preparing meals and eating, getting exercise, using the toilet, walking, and getting in or out of a bed, chair, or wheelchair.
Medicaid For Texans In Nursing Homes
In 2018, the average monthly cost of a private room in a nursing home in Texas was approximately $6,540, or over $78,000 per year. Thus, most people cannot afford to pay their own nursing home expenses. Nursing homes are residential facilities that offer 24-hour skilled nursing care in addition to other supportive services.
If you already qualify for Texas Medicaid, then your Medicaid coverage includes nursing home care if you need it. Groups of people who can automatically qualify for Medicaid include SSI recipients, participants in the TANF program, and children in its foster care system. In addition, people who are 65 or older, disabled, or blind can qualify for Medicaid if they also meet income and resource limits.
Also Check: Medicaid Brooklyn Ny Phone Number
Nursing Home Care Vs Assisted Living
Not every nursing home resident actually requires nursing home care. It is important to recognize many assisted living communities now offer advanced care services that are almost on par with nursing homes. One option for reducing nursing home costs is to consider assisted living instead. Read about the key differences between assisted living and nursing home care.
How Long Does Medicare Pay For Long

Total Medicare payments for long-term care delivered in an SNF are limited.
- Medicare pays 100% of the cost through day 20 of your stay in an SNF
- You are responsible for any out of pocket co-pay . Medicare will cover the balance owed through day 100 of your stay in an SNF
- After day 100, Medicare does not cover any costs for stays in an SNF
The above applies to Original Medicare.
Medicare Advantage plans cover the same services in an SNF, but the way cost-sharing is determined can vary.
Don’t Miss: Eye Exam Places That Take Medicaid
Pennsylvania’s Medicaid Program Will Pay For A Nursing Home Or Home Care If You Have Limited Income And Assets And Your Doctor Certifies That You Need The Care
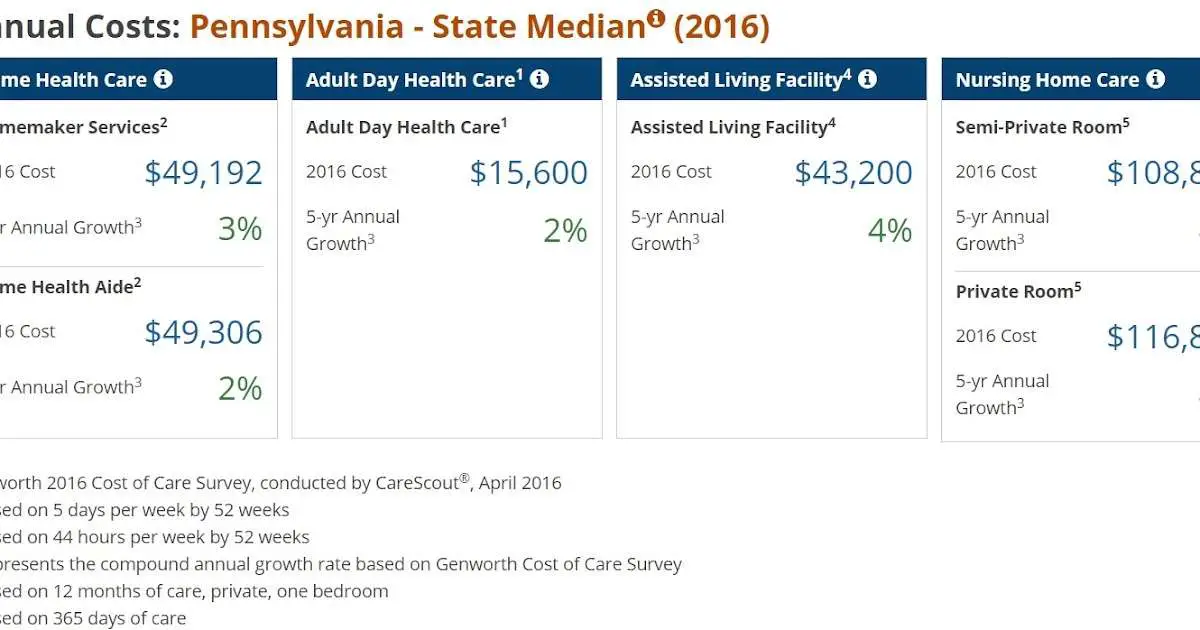
Nursing homes and assisted living facilities in Pennsylvania are expensive, and even alternative long-term care like home health care can be costly. In 2017, the median annual cost of a private room in a nursing home in Pennsylvania was $120,085. Private health insurance policies generally don’t cover long term care, very few people purchase private long-term care insurance policies, and Medicare coverage for long-term care services is limited.
When people can’t afford to pay the $5,000 to $8,000 per month of long-term care, they often turn to Medicaid, which has become a very common source of funding for long-term care. In 2017, approximately 60% of nursing home residents in Pennsylvania used Medicaid to pay for their nursing home care.
There are many different ways to become eligible for Medicaid in Pennsylvania, and there are specific eligibility rules for long-term care services like nursing homes, assisted living facilities, and home health care services.
Who May Receive Nursing Facility Services
NF services for are required to be provided by state Medicaid programs for individuals age 21 or older who need them. States may not limit access to the service, or make it subject to waiting lists, as they may for home and community based services. Therefore, in some cases NF services may be more immediately available than other long-term care options. NF residents and their families should investigate other long-term care options in order to transition back to the community as quickly as possible.
Need for nursing facility services is defined by states, all of whom have established NF level of care criteria. State level of care requirements must provide access to individuals who meet the coverage criteria defined in federal law and regulation. Individuals with serious mental illness or intellectual disability must also be evaluated by the state’s Preadmission Screening and Resident Review program to determine if NF admission is needed and appropriate.
Nursing facility services for individuals under age 21 is a separate Medicaid service, optional for states to provide. However, all states provide the service, and in practice there is no distinction between the services.
In some states individuals applying for NF residence may be eligible for Medicaid under higher eligibility limits used for residents of an institution. See your state Medicaid agency for more information.
Recommended Reading: Pregnancy Medicaid Florida Phone Number
Does Medicare Pay For Nursing Home Care
If you have had a qualifying inpatient hospital stay and your doctor orders an additional period of treatment in a skilled nursing facility, Medicare Part A generally covers allowable expenses. Your Part A nursing home benefit usually covers:
- A semi-private room
- Medical equipment and devices you use during your hospital stay
- Ambulance transportation to and from the facility
There are costs for a covered stay in a skilled nursing facility . In 2019, you pay no coinsurance for days 1 through 20, $170.50 per day for days 21 through 100, and all nursing home costs for your care after the 100th day.
Medicare does not, however, pay any nursing home costs for long-term care or custodial care. If you need unskilled care for activities of daily living, care for an extended period of time, or care that is not reasonably expected to improve your condition within a limited timeframe, Medicare will not cover it.
Nursing Home Average Costs
On average, a nursing home costs $225 daily for a semi-private room and $253 for a private room. Monthly charges range from $6,844 to $7,698 for semi-private and private rooms respectively. Annual costs range from $82,128 to $92,376 for full time nursing home care. Additional costs may be incurred if dementia, memory care or other special services are required.
Read Also: What Is Medicaid Buy In Program
How Your Assets Impact Eligibility
Besides income, your assets will be counted toward meeting eligibility requirements. Countable assets include checking and savings account balances, CDs, stocks, and bonds.
In most states, you can retain up to $2,000 as an individual and $3,000 for a married couple outside of your countable assets. However, these amounts may vary depending on the state in which you live.
Your home, your car, personal belongings, or your savings for funeral expenses remain outside of countable assets. If you can prove other assets are not accessible , they too are exempt. A house must be a principal residence and does not count as long as the nursing home resident or their spouse lives there or intends to return there.
Upon becoming eligible for Medicaid, all of the applicant’s income must be used to pay for the nursing home where the applicant resides. However, you may be allowed to keep a monthly “allowance” and a deduction for medical needs, such as private health insurance. The amount of the allowance varies depending on your living arrangements, type of nursing facility, and state rules. If you are married, an allowance may be made for the spouse still living in the home.
Home Care Waiver Programs
Pennsylvania also operates several Medicaid Waiver programs that provide home health care services to low-income Pennsylvanians.
To qualify for any of Pennsylvania’s Waiver programs, you must meet the nursing home level of care. In addition, you must have income less than $2,163/month and fewer than $8,000 in resources. To apply for waiver programs, contact the Office of Long-Term Living Helpline at 866-286-3636.
You May Like: How Do You Know If You Still Have Medicaid
What Kind Of Nursing Home Care Does Medicare Cover
The term nursing home can refer to different types of places, including rest homes, nursing homes, board-and-care homes, assisted-living facilities, congregate living homes, and sheltered care homes. All of these provide whats called custodial care, which is long-term residence and non-medical assistance with the activities of daily living such as bathing, eating, walking, and dressing for people who dont have acute medical conditions but who are no longer able to care for themselves completely. This type of custodial long-term care is not covered by Medicare.
At the other end of the nursing home spectrum is high-level inpatient medical care, referred to as skilled nursing or rehabilitation care. Under certain circumstances, Medicare Part A covers this skilled care for a limited time while a patient is recovering from a serious illness, condition or injury. For Medicare to cover this care, it must be provided in the skilled nursing facility wing of a hospital, in a stand-alone skilled nursing or rehabilitation facility, or in the skilled nursing or rehabilitation unit within a multilevel facility.
Does Medicaid Cover The Costs Of A Nursing Home

As people age, the probability that they will need long-term care in a nursing home increase. Most Americans over the age of 65 rely on Medicare insurance to cover their health care costs. Unfortunately, Medicare coverage does not extend to long-term nursing home care and many people find themselves paying out-of-pocket.
If you or a loved one are Medicare recipients and facing the possibility of needing nursing home care, it is important to know all your insurance options ahead of time. If you do not have the financial means to pay out-of-pocket for nursing home care after your Medicare coverage ends, you may be able to get help from Medicaid.
Medicare Coverage for Nursing Home CareMedicare recipients have coverage for skilled nursing care lasting up to 100 days for every separate instance of an illness or injury. In order to be eligible for coverage, you must stay in a Medicare-approved facility, you must be admitted within 30 days of a hospital stay which lasted for three days or more, and you must have an order from a physician stating that you require treatment. The physician must certify that you need skilled nursing care to maintain or to slow the deterioration of your current status of health.
Medicare covers the cost of skilled nursing care, rehabilitative services, a semi-private room and meals, plus any medical supplies needed for treating your prescribed condition. It does not cover the cost of custodial care like bathing, feeding, or dressing.
Related articles:
You May Like: Michigan Medicaid Nursing Home Application
What Do Va Long
For extended care services, veterans may be subject to a co-payment of up to $97 per day. The amount of the co-payment depends on the veterans VA health system priority group and individual financial circumstances, and also on the type of care or service provided. The amount of co-payment for extended care services is based on income, and for some services, co-pay amounts are based on the assets held by both the veteran and the veterans spouse.
For extended care services expected to last 180 days or less, the VA looks only at the income of the veteran and spouse, taking into account the veterans expenses. For extended care services expected to last 181 days or longer , the VA looks at the income and the assets of the veteran and spouse. Details of these financial calculations are available from the VAs publication VA Copays and Charges.
How Much Does 24/7 In Home Care Cost
Typically, the daily rate for most home care agencies ranges from $200 to about $350 per day. This, of course, is dependent on the cost of living within your given region as well as the amount of specialized care that you need as a client.
You May Like: I Lost My Medicaid Card
What Type Of Long Term Care Bill Will Medicare Pay For
An overnight stay in the hospital causes your body to become dehydrated and can cause you to become depressed. After you have recovered from this injury, you will benefit from Medicare. For skilled nursing care, Medicare pays up to $185 out-of-pocket in the first 20 days. Approximately $50 per day is expected to be paid by 2021. Medicare ceases to cover expenses after 100 days.
How Much Is The Medicaid Copayment To The Nursing Home
The Medicaid program requires nursing home benefit recipients to share in the monthly cost of their care. This is called the Medicaid copayment or their applied income. In Texas, every nursing home Medicaid recipient is entitled to a personal needs allowance of $60 per month. But as explained in more detail below, Medicaid recipients can actually keep more of their income than the $60 allowance suggests. It is also important to understand that the Medicaid recipient still receives their income. Therefore, even if an individual is on Medicaid, the recipient will still be responsible for satisfying a monthly copayment to the nursing facility. If this copayment is not paid, the nursing facility can begin the process to discharge the resident for nonpayment.
As the payor of last resort, Medicaid encourages benefit recipients to keep their Medicare or other health coverage by reducing the monthly Medicaid copayment dollar for dollar by the premium paid to maintain health insurance. To be more specific, the Medicaid copayment will be reduced for incurred medical expenses not covered by a third party. These expenses are limited to Medicare and other general health insurance premiums, deductibles and coinsurance, and to medically necessary medical care and services that are recognized by state law but not covered under the Medicaid state plan.
Other Frequently Asked Questions
You May Like: Does Medicaid Pay For Implant Dentures
Do All Nursing Homes Accept Medicaid
A majority of nursing homes accept Medicaid however, this is also largely dependent on the state you reside in. To avoid complications with payment and coverage, Id recommend checking with your nursing home facility to see if they are a Medicaid-certified nursing facility. If it is, then you should be eligible for coverage under the Medicaid skilled nursing facility.
In the event that you find out the nursing home is not Medicaid-certified, you would have to transfer to a nursing facility thats covered by Medicaid.
What Are The Requirements For Medicare Nursing Home Coverage
Before Medicare covers skilled nursing home costs, you must have a qualifying hospital stay of at least three inpatient days prior to your nursing home admission. You must have inpatient status for at least three days time spent in the emergency department or observation unit doesnt count toward the three-day requirement.
If you refuse nursing care or medical therapies recommended by your doctor while you are in a skilled nursing facility, you may lose your Medicare nursing home coverage.
Also Check: How To Apply For Women’s Medicaid
What If I Dont Have Health Insurance
Under the new policy, only people who are privately insured can seek rapid at-home test reimbursements. The White House is working on a plan to deliver 500 million free test kits to people who request them on a forthcoming website, but government officials still havent released details about the website and shipment plans.
Several states, such as New Jersey, Connecticut, and Massachusetts have already been distributing free at-home tests to residents since the Omicron surge began. Some cities, such as Miami and Washington D.C., are making free tests available at public libraries. Check with your local health centers or health department to see if and where you can pick up free test kits.
Medicare And Medicaid Long
If you or a loved one require long-term personal or medical care, you may be wondering what is covered and what isnt under federal and state programs such as Medicare and Medicaid.
Both Medicare and Medicaid may help pay for some long-term care services. However, the circumstances in which each coverage can be used are limited, and each program has strict rules about
- Whether you qualify for benefits
- Which long-term services are covered
- How long you can receive specific benefits such as long-term care
- How much your out-of-pocket costs will be for long-term care
- Whether or not your estate must reimburse the government after your passing
Knowing the differences between what the programs cover can help you navigate the maze of senior care and find viable solutions.
Don’t Miss: Does Medicaid Cover Gastric Bypass In Michigan
