Who Is Dual Eligible For Medicare And Medicaid
To be Medicare dual eligible, you have to meet the requirements for Medicare and your states Medicaid program.
To be eligible for Medicare, you must:
- Be at least 65 years old or having a qualifying disability
- Be a U.S. citizen or permanent legal resident
- Be eligible for benefits through Social Security or the Railroad Retirement Board
Generally speaking, Medicaid provides health insurance to low-income individuals and families, children and pregnant women. The best way to find out if you are eligible for Medicaid is to visit your states Medicaid website.
If you’re eligible for Medicaid and want to find out if you’re also eligible for a dual-eligible Medicare Medicaid plan, you can all to speak with a licensed insurance to find out if you’re eligible. An agent can help you compare the plans that are available where you live and find out what they may cover, which could include benefits like prescription drugs and other services.
Find $0 premium Medicare plans in your area
Or call 1-800-557-6059TTY Users: 711 24/7 to speak with a licensed insurance agent.
Who Is Eligible For Both Medicare And Medicaid
At this point you might be asking, Can you have Medicare and Medicaid at the same time? Yes under certain circumstances, you may qualify for both programs. This is known as dual eligibility.
Who is eligible for Medicare and Medicaid at the same time? Generally those living with disabilities or chronic medical needs who also have limited income may qualify for dual eligibility. If youre dual eligible, Medicare is the primary payer for most of your services, and Medicaid pays most or all of the rest.
If youre dual eligible, youll typically fall into one of several categories of Medicare Savings Programs. These can include:
- Qualified Medicare Beneficiary Program Receive help paying premiums for Medicare Part A and Medicare Part B.
- Specified Low-Income Medicare Beneficiary Program Receive help paying your Part B premium if youre between 100 and 120 percent of the Federal Poverty Level.
- Qualifying Individual Program QIs have higher income limits than SLMB and can help pay for Part B premiums.
- Qualified Disabled Working Individual Program Certain disabled and working beneficiaries may get help paying the Part A premium.
Can You Have Medicare And Medicaid At The Same Time
Medicare and Medicaid are both public health insurance programs. If you are dual eligible, you can have both Medicare and Medicaid coverage at the same time.
Two of the key differences between Medicare vs. Medicaid include:
- Medicare is for people age 65 and over and for certain people under 65 who have a qualifying disability. Medicare eligibility is consistent for everyone across the U.S., no matter what state you live in.
- Medicaid is for people of any age who meet certain income qualifications. Medicaid is administered by state governments, and eligibility requirements can differ between states.
Read Also: What Is The Income Limit For Arkansas Medicaid
Benefits Of Enrolling In A D
Enrolling in a D-SNP does not change what Medicare or Apple Health covers.
The primary benefit of a D-SNP is having one plan for your Medicare and Apple Health coverage. D-SNP coverage makes finding a provider easier, since providers only need to accept one plan.
A D-SNP also improves your care coordination. Being in a D-SNP makes it easier for your providers to make referrals and plan your treatment.
You may choose the same plan for both D-SNP and BHSO coverage. If so, the plan covers both your physical health care and your behavioral health care needs.
Some D-SNP plans offer supplemental benefits in addition to what Medicare and Apple health covers. Please contact the plans for more information.
Our D-SNP service area guide has three resources:
-
D-SNP Service area map: shows which counties have D-SNPs coverage.
-
Aligned enrollment map: Shows counties where D-SNPs and BHSOs offer aligned enrollment.
-
D-SNP Service area matrix: shows which D-SNP is in each county. In some counties, plans have only D-SNPs. In other counties, they have both D-SNPs and BHSOs.
Consult with your providers to see which plans they accept. You can also contact the plans to see if your providers are in their networks.
Dual Eligibility With Medicaid
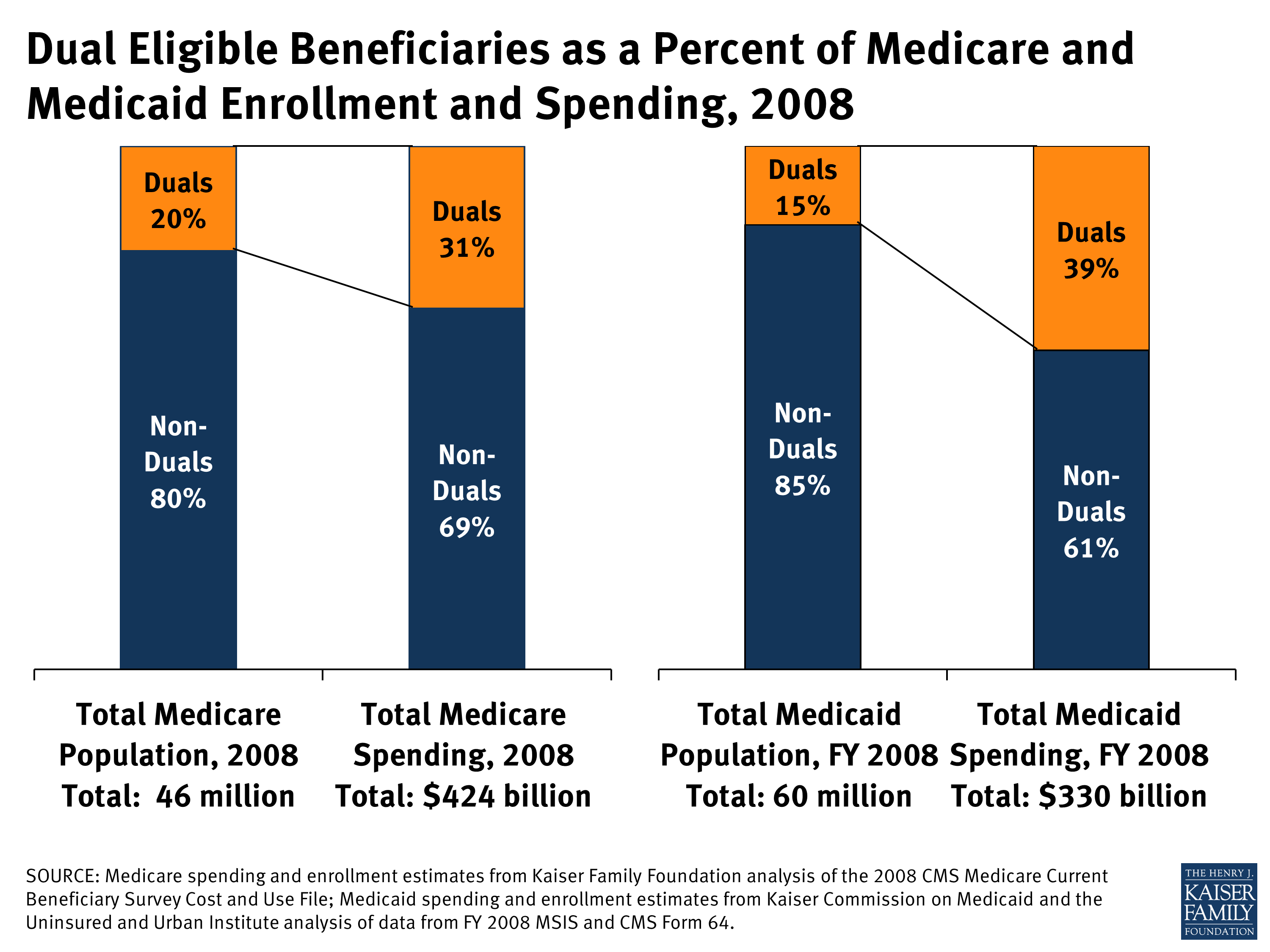
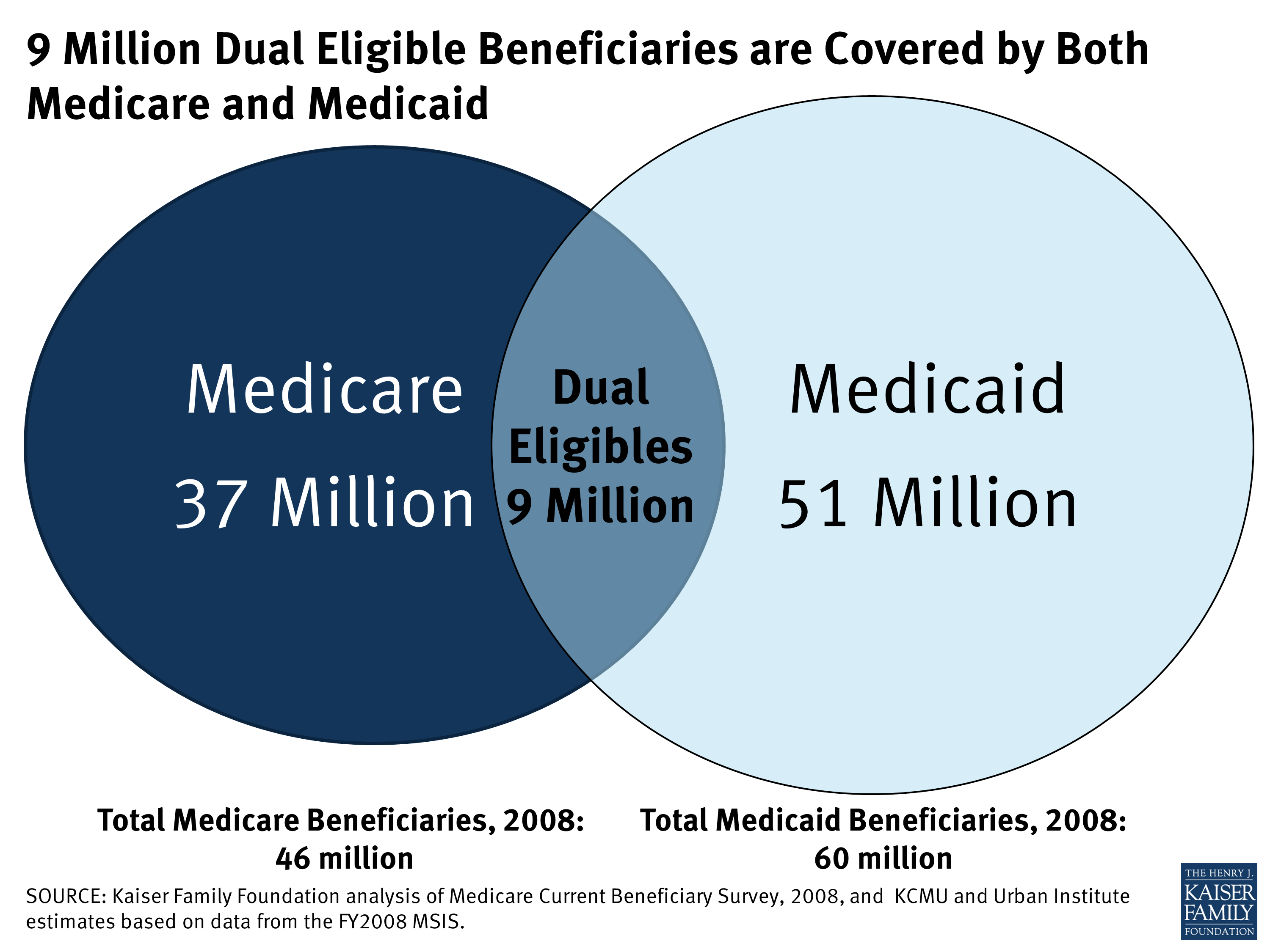
Millions of Americans are eligible for both Medicare and Medicaid every year. This dual eligibility may provide extra coverage to beneficiaries but with that comes extra regulation. It is important to note that both programs are managed by the same federal agency, the Centers for Medicare and Medicaid Services .
Although Part D plans are voluntary for most Medicare beneficiaries, those who are dual eligible have no choice. Medicaid requires that you sign up for Medicare as soon as you are eligible and this includes signing up for a Part D plan. If you do not sign up yourself, you will be automatically enrolled in Original Medicare and a Part D plan by the government. You will have the option to change to a MA-PD or pick a different Part D plan at a later time.
Also Check: Utah Medicaid Mental Health Providers
What Is Medicare Extra Help
Extra Help is a federal program that helps pay for out-of-pocket costs related to Medicare prescription drug coverage. Extra Help is also known as the Medicare Part D Low-Income Subsidy
The assistance that Medicare Extra Help may provide includes:
- Help paying Part D premiums
- Lowered out-of-pocket costs of prescription drugs
- An annual Special Enrollment Period to enroll in a Part D plan or switch to a new one
- Elimination of Part D late enrollment penalties
You automatically qualify for Extra Help if you are enrolled in Medicaid, Supplemental Security Income or a Medicare Savings Program.
You may still qualify for Extra Help if you are not enrolled in any of those programs but still have income and assets below a certain limit.
Do I Have To Pay For Medicaid
What you pay for Medicaid will depend on your state and your income. Most states have caps on what can be charged for certain services. For the most part, Medicaid is designed to provide low- or no-cost healthcare, and also qualifies you for other cost-saving programs like Medicare Savings Programs and Extra Help.
Also Check: Family Of Three Income For Medicaid
Qualified Disabled Working Individual Program
The QDWI Program helps pay for the Medicare Part A premium for certain people who meet one of the following criteria:
- Have a disability but are still working
- Lost their premium-free Part A coverage when they returned to work
- Are not receiving medical assistance from their state
- Meet the income and resource limits below
- Income of no more than $4,379 per month for an individual in 2021, or $5,892 for a married couple.
- Resources of $4,000 for an individual in 2021, or $6,000 for a married couple.
The income and resource limits listed above may increase in 2022. If your income and resources are slightly higher, you should still apply.
Can You Draw Medicaid You Get Medicare
Some people qualify for both Medicare and Medicaid and are called dual eligibles. If you have Medicare and full Medicaid coverage, most of your health care costs are likely covered. You can get your Medicare coverage through Original Medicare or a Medicare Advantage Plan.
Also Check: Can I Get A Replacement Medicaid Card Online
D Eligibility With Medicare
Once you are eligible for Medicare, you can decide which parts you want to sign up forParts A, B, C, or D.
Your first decision will be whether to opt for Original Medicare or a Medicare Advantage plan. You cannot have both. For clarification, Medicare Advantage plans offer everything that Parts A and B do but may provide additional benefits for an added cost.
In order to apply for Part D, you may enroll in Part A, Part B, or both. There is no option to apply for Part D alone.
Alternatively, you can choose to sign up for a Medicare Advantage plan. There are Medicare Advantage Prescription Drug Plans that include Part D coverage.
In summary, you will need to have one of these Medicare plans or combinations to be eligible for Part D coverage:
- Part D + Part A
- Part D + Original Medicare
- MA-PD
There are times you may be eligible for Medicare but are not allowed to enroll in a Part D plan. This occurs when you reside outside of the country or U.S. territories. When you return to the United States, you will be eligible to sign up. When you are incarcerated, you receive benefits from the prison system, not Medicare. You may enroll in Part D after you are released.
What Are The State
Benefits for dual eligible beneficiaries candiffer based on your state of residence. Differences by state may include:
- Medicaid offered through Medicaid managed care plans
- fee-for-service Medicaid coverage
- plans that include all Medicare and Medicaid benefits
Income and resource standards are defined by federal law for full Medicaid and the Medicare Savings Programs. At their discretion, states can effectively raise the federally mandated limits.
Youre also considered a dual eligible beneficiary if youre enrolled in Medicare Part A or Part B and receiving cost-sharing through a Medicare savings program .
Below is table summarizing the benefits and eligibility criteria for each of the different MSPs in 2021:
| MSP | ||
|---|---|---|
| Specified Low-Income Medicare Beneficiary program | assists in the payment of Part B premiums | individual monthly income of $1,308 or less, individual resources limit of $7,970 married couple monthly income of $1,762 or less, married couple resources limit of $11,960 |
In addition to the Medicare savings programs, you also may be eligible for some of the following needs-based programs through Medicare:
- PACE : a Medicare-Medicaid joint program that provides medical and social services for people with significant needs who want to continue living at home
- Medicares Extra Help program: can help those with low incomes get the prescription drugs they need at reduced or no cost
Dual eligibility for Medicare and Medicaid means that youre enrolled in Medicare and either:
Recommended Reading: Phone Number For California Medicaid
What To Consider When Enrolling In A D
You cannot enroll in both a D-SNP and a Health Home program. Enrollment into a D-SNP will disenroll you from your Health Home program. For more information on the Health Home program, see the Health Home page.
You have the option to choose the plan for your D-SNP and BHSO coverage if you live in a county that offers aligned enrollment.
Aligned enrollment helps dual-eligible clients manage their physical and behavioral health services under one plan. This makes it easier to find a provider and coordinate your Medicare and Apple Health services.
View the aligned enrollment map in our service area guide to see if alignment is available in your county.
D Price Concessions To Be Applied At Point

More Part D plans and pharmacies are entering into price concession agreements, where plans pay less money to pharmacies for dispensed drugs if the pharmacies fail to meet certain metrics. However, there’s little public visibility on the price concessions, and any lower prices aren’t being passed down to beneficiaries, CMS said.
As a result, in 2018, the government asked for public comment on a policy that would require Part D plans to apply all price concessions received from network pharmacies at the point of sale, which should in turn reduce beneficiary cost-sharing.
After digesting the comments, CMS is now proposing this policy. The agency said it would reduce beneficiaries’ Medicare Part D out-of-pocket costs while bettering market competition and price transparency in Part D.
The policy, which would also redefine the negotiated price as the lowest admissible payment to a pharmacy, will take affect in 2023, if finalized.
CMS is also looking for feedback on the challenges with building behavioral health provider networks within MA plans, and how the changes proposed Thursday might impact network adequacy.
Don’t Miss: What Doctors Take Florida Medicaid
Do You Need Supplemental Insurance If You Are Dual Eligible For Medicare And Medicaid
If you qualify for both Medicare and Medicaid, chances are most or all of your healthcare costs will be covered. Dual-eligible individuals usually qualify for their healthcare plus Extra Help programs that help pay their out-of-pocket drug costs.
Are you still asking Whats the difference between Medicare and Medicaid? GoHealth can provide the answers youre looking for. Our licensed insurance agents can break down the different types of healthcare you may be eligible for, and offer impartial guidance to help you choose the plan thats right for you. Well shop for plans, explain the finer points and make sure you get the coverage you need.
What extra benefits and savings do you qualify for?
What Is Pace
The Program of All-Inclusive Care for the Elderly is a program for older Medicare and Medicaid beneficiaries that allows people to meet their health care needs within the community instead of in a nursing home or other care facility.
PACE uses a team of health care professionals that coordinate your care including prescriptions, doctor appointments, hospital visits and even transportation. There are no deductibles or copayments in PACE and the program covers everything included under Medicare and Medicaid if authorized by the persons health care team.
Qualifying for PACE requires being at least 55 years of age, living in an area serviced by PACE, require a nursing-home level of care and able to live safely in the community with assistance from PACE.
Don’t Miss: Does Medicaid Cover Assisted Living In Michigan
What Is A D
Before we break down what a D-SNP is, we need to discuss its parent category the SNP.
Special Needs Plans are a form of Medicare Advantage Plan specifically designed to provide targeted care and limit enrollment to individuals that meet specific needs.i There are three types of SNPs, includingii:
Chronic Condition SNP : For those with a severe or disabling chronic condition, such as End-Stage Renal Disease , dementia, HIV/AIDS, chronic heart failure, etc.
Institutional SNP : For those who live in an institution such as a nursing home or require nursing care at home.
Dual-Eligible SNP : For those with both Medicare and Medicaid.
D-SNPs are designed to work together with your Medicaid plan and often come with additional benefits and resources not typically offered by Original Medicare or Medicare Advantage Plans alone.
Can You Have Both Medicare And Medicaid
- Beneficiaries who are eligible for both Medicare and Medicaid are considered dual eligible. Learn how to enroll and the benefits you can expect if you qualify for dual eligibility.
More than 62 million Americans are enrolled in Medicare in 2020, and nearly 69 million people are enrolled in Medicaid.
As of 2019, well over 12 million Americans are dual eligible for both Medicare and Medicaid. You may wonder how someone can have both Medicare and Medicaid, and you may wonder if you qualify for dual eligibility.
Below well discuss the eligibility qualifications for Medicare and Medicaid, the benefits available to you if youre dual eligible and other information you may want to know about dual eligibility.
Recommended Reading: Washington State Medicaid Residency Requirements
Definitions For Medicare/medicaid Dual Eligibles And Medicare Part D Information
The following list consists of definitions of words commonly referred to in reference to the new Medicare Part D prescription drug program. This list is provided to help clarify terminology to people unfamiliar with thedetails of the Part D program as it relates to persons receiving both Medicaid and Medicare. If you have further questions about these definitions, please contact 1-800-Medicare . Visit Medicare’s website for the Official Medicare Frequently Asked Questions.
What Are The Main Differences
The main differences between Medicare and Medicaid are who runs the programs and who is eligible. If you are older or disabled, you will likely qualify for Medicare. If you have certain health and financial needs but dont qualify for Medicare, you may be able to receive services through Medicaid. The federal government sets rules for both programs, but states have control over the specifics of their Medicaid plans and what additional services they may offer.
Recommended Reading: Does Medicaid Cover Gym Memberships
Who Is A Dual
A dual-eligible individual has both Medicare coverage and Apple Health coverage. This includes physical and behavioral health care coverage.
If you are a dual-eligible client, Medicare is your primary coverage for your physical health care needs. You also have Apple Health as secondary coverage.
Dual-eligible clients also have behavioral health coverage through an Apple Health managed care plan. This is a Behavioral Health Services Only plan. Behavioral health includes mental health and substance use disorder treatment.
Ensuring An Effective Transition Of Dual Eligibles From Medicaid To Medicare Part D
ENSURING AN EFFECTIVE TRANSITION OF DUAL ELIGIBLES FROM MEDICAID TO MEDICARE PART D
Beginning January 1, 2006, responsibility for the prescription drug coverage for over 6 million low-income Medicare beneficiaries who also are enrolled in Medicaid shifts from the states to the federal government consistent with the Medicare Modernization Act of 2003. These beneficiaries, referred to as the full-benefit dual eligibles, will qualify for Medicare prescription drug coverage with low or no premiums and co-payments of a few dollars.
CMS recognizes the enormity of this transition from Medicaid drug coverage to Medicare and has been working intensively with many partners in and out of government to ensure that the transition process for these beneficiaries is as seamless and efficient as possible. The most important goal of this transition is to ensure full-benefit dual eligible beneficiaries will get the prescription drug coverage they need as of January 1, 2006.
CMS is committed to accomplishing the following two key objectives to ensure a safe and appropriate transition of the dual eligible population from Medicaid to Medicare Prescription Drug Coverage:
I. Providing comprehensive coverage and high quality prescription drug coverage plans for all people with Medicare, but especially for the dually eligible population, who often take a number of prescriptions to manage one or more chronic conditions. To achieve this objective, CMS has taken the following steps:
Don’t Miss: Psychiatrist In Nyc That Take Medicaid
