How Do I Apply For Benefits If I Was Fired For Not Getting Vaccinated
If your state has mandated a vaccination requirement for your industry and youre fired for refusing to comply you might not be eligible. Youll want to check if theres an exemption you qualify for based on state or company law. You can apply for benefits by filing a claim with your states unemployment insurance program. You can find the contact information to start your claim here.
If you do apply for unemployment benefits and the employer challenges your claim, you will likely end up in court. As such, you should contact an attorney to pursue a claim or file an appeal.
Recommended Reading: Maximum Unemployment Benefits Mn
Learn About The Childrens Health Insurance Program
If your income is too high for Medicaid, your child may still qualify for the Childrens Health Insurance Program . It covers medical and dental care for uninsured children and teens up to age 19.
Is my child eligible for CHIP?
CHIP qualifications are different in every state. In most cases, they depend on income.
How do I apply for CHIP benefits?
You have two ways to apply for CHIP:
- Fill out an application through the Health Insurance Marketplace.
What else do I need to know about CHIP?
- You can apply for and enroll in Medicaid or CHIP anytime during the year.
Unemployed Applicants Should Use State Or Federal Marketplace
An unemployed person can apply for health insurance on the federal or state exchanges. They may find affordable low-premium options based on family income. Should they not find an affordable option, they may qualify for an exemption, Medicaid, or the CHIP.
Many states offer assistance to low-income families to help them qualify for affordable health insurance including payment assistance. If income is below the minimum needed for Obamacare, then applicants can seek coverage under the applicable state Medicaid program or CHIP for minors.
Recommended Reading: Unemployment Ticket Checker
Don’t Miss: What States Do Not Have Medicaid Expansion
Q If I Dont Qualify For Medicaid Is There Any Other Help For Me Or My Children
A. Yes. Many organizations in Delaware are dedicated to the principle that health care should never be beyond the reach of those who need it. If you need health care, but do not have insurance coverage, the people at the Delaware HelpLine have a wealth of information about organizations that provide health care at reduced rates for uninsured individuals. Call the Delaware HelpLine toll-free at 1-800-464-HELP from Monday Friday from 8:00 a.m. to 5:00 p.m. The Delaware Helpline service is also available in Spanish. Additional information about the support provided by the Delaware Helpline can also be found by visiting www.delawarehelpline.org.
For example, you may qualify to receive discounted medical services through the Community Healthcare Access Program . CHAP helps connect uninsured individuals with affordable health care from primary care doctors, medical specialists, and other health providers including prescription programs, laboratory and radiology services. To find out more about this program, visit the website for the Community Healthcare Access Program, or call 1-800-996-9969 for eligibility guidelines.
You can read about CHAP and other healthcare resources for uninsured individuals in the Delaware Healthcare Resource Guide. This guide is also available in Spanish: Guía de Recursos de Salud.
Under 18:
Over 65:
Current Law: 16 Weeks Of Federal Additional Income Included In Eligibility

At present, vulnerable workers who become unemployed can receive $600 in additional federal income for 16 weeks. This federal unemployment compensation is included in income eligibility determinations for ACA marketplace eligibility but not for Medicaid and CHIP eligibility.
Eligibility for assistance of any kind is not substantially different between expansion and nonexpansion states when all the cash assistance available is received, the researchers stated.
READ MORE:Medicaid Expansion States May See Lower Uninsurance Amid COVID-19
However, workers in expansion states are seven times more likely to be eligible for Medicaid, the researchers found. This is a critical metric because Medicaid usually has limited additional out-of-pocket healthcare spending for beneficiaries, as opposed to health plans on the ACA federal or state health insurance marketplace. This would make healthcare more affordable for Medicaid-eligible workers in Medicaid expansion states.
In both Medicaid expansion and nonexpansion states, under the current law, a similar percentage of vulnerable workers are not eligible for any federal funding . The percentage is slightly lower in Medicaid expansion states.
Read Also: Does Quest Diagnostics Accept Medicaid
How To Qualify For Medicaid
May 15, 2020, 12:00 AM
It can be expensive to pay for health insurance when you lose your job, but many people dont realize that theyre eligible for Medicaid coverage. If you live in one of the 36 states that expanded Medicaid coverage for low-income adults, you can qualify for coverage if your monthly income is less than $1,467 for an individual or $3,013 for a family of four even if you earned a lot more than that during the first few months of the year.
This type of Medicaid has different eligibility requirements than the version that provides nursing home coverage for people over age 65 there is no asset test for this type of Medicaid. Instead, eligibility is based on your family size and your modified adjusted gross income .
Many people dont know that theyre eligible for Medicaid, says Robin Rudowitz, co-director of the Program on Medicaid and the Uninsured at the Kaiser Family Foundation. Medicaid is based on monthly income, so people who have significant drops in income could become eligible. There is no open enrollment period for Medicaid, so when people experience a change in their circumstances, they dont have to wait for a special open enrollment period to enroll.
Heres more information about how to qualify for Medicaid, how the coverage works and what you can do if your state hasnt expanded coverage.
Who Is Eligible for Medicaid?
Dont Miss:
Income Requirements For Florida Medicaid
There are income requirements for Medicaid in Florida. You need to earn an income that is within the federal poverty level for your group. This is calculated by a specific system that is known as the Modified Adjusted Gross Income, or MAGI.
Basically, before taxes, income needs to be under these amounts, according to Benefits.gov:
Household Size Maximum Income Level
1 $15,000
- Speech-language pathology, respiratory, physical, and occupational therapy services
Don’t Miss: Office Of Medicare And Medicaid Services
How Your Snap Benefits Work
- Your state will issue benefits each month on a plastic electronic benefits transfer card. Much like a credit or debit card, you can use your EBT card to buy eligible food items. You must buy them from:
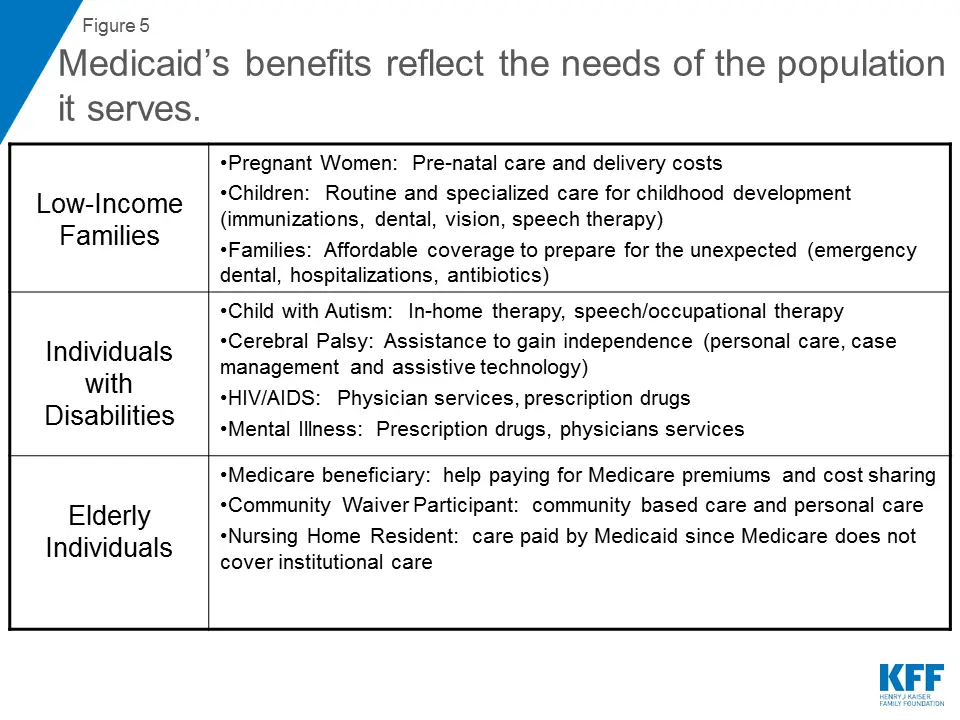
What help is available through Medicaid?
Medicaid provides free or low-cost medical benefits to eligible:
- Adults with a low income
- Children
- People who are age 65 or over
- People with disabilities
Am I eligible for Medicaid?
Check with your states Medicaid office to see if you or your family members are eligible for benefits. In general, it depends on at least one or a combination of:
- Age
- Number of people in your family
- If you are pregnant or have a disability
How do I apply for Medicaid?
There are two ways to apply for Medicaid:
- Contact your state Medicaid agency. You must be a resident of the state where you are applying for benefits.
- Fill out an application through the Health Insurance Marketplace.
Impact Of The Affordable Care Act
The Affordable Care Act , enacted in 2010, had a significant impact on Medicaid eligibility, as it is what offered Medicaid Expansion to states. In exchange for federal funding, states agreed to expand Medicaid coverage to anyone with incomes up to 133% of the FPL, regardless of other factors. The remaining states continue to follow the traditional Medicaid eligibility guidelines.
Don’t Miss: Is Dental Bonding Covered By Medicaid
Florida Medicaid Program Eligibility
Medicaid is a program for medical assistance that gives low-income individuals and families access to health care that they wouldnt otherwise have. Medicaid also assists people with disabilities and the elderly with the costs of expenses like care in nursing facilities and other long-term medical bills.
The agency responsible for Medicaid in Florida is the Agency for Health Care Administration, also known as simply the Agency. The Agency has successfully completed implementing the SMMC program. Under this program, most of the recipients of Medicaid are enrolled into one of a variety of health plans. These health plans are accredited nationally and selected by a competitive procurement process.
Learn About Medicaid Asset Limits And Eligibility Requirements
Although Medicaid is federally funded, it is administered at the state level, and each state has its own set of rules and regulations for this program. The income and asset levels allowed differ from one state to another, so be sure to find out where your balance sheet falls in relation to the threshold.
If you are single, you generally cannot have more than $2,000 worth of cash or other assets outside of your residence, vehicle, and other necessary items unless your state has a higher limit.
If you are married and your spouse is still able to live independently, they are allowed to retain 50% of your joint assets up to a threshold of $130,380 as of January 2021. Your single or joint income usually cannot exceed 138% of the federal poverty level, although several states have thresholds above this amount.
In nearly all cases, you will also have to prove via medical documents that you are disabled. However, certain exceptions apply . You must also be either a U.S. citizen or have a green card and prove your residency within the state.
Don’t Miss: How Long Does It Take For Medicaid To Start
Which Medicaid Plan Is Best In Virginia
The best Medicaid plan will be different from person to person based on their specific needs. There are a variety of plans to choose from. Not all of them are available in all areas, so check to see which ones are available to you before choosing one. You might also want to check with your doctors to see which plans they accept if you dont want to have to change doctors.
How Do I Apply For Medicaid
- Start by going to Healthcare.gov. This web site is also called a Marketplace. You can find out if you qualify for Medicaid or other federal assistance to purchase health insurance. If your state has its own Marketplace, HeathCare.gov will send you to it.
- Apply online.
- You can also get in-person help signing up. To find a navigator near you, go to “Find Local Help” on Healthcare.gov.
You may need documents that show your income, home address, and other details.
Recommended Reading: How Do I Enroll My Newborn In Medicaid
Q What Documents Will I Need To Provide When I Apply
A. You will need to provide verification of your income. You do not need to provide proof of your assets or resources or come into our offices to be interviewed unless you are applying for one of the Long Term Care Medicaid programs .
If you are pregnant, you will need to provide proof that you are pregnant. If you are not a U.S. citizen, you will need to provide proof of your alien status. For example, you can provide a copy of your green card.
If you apply online using ASSIST, a web page at the end of the application will tell you exactly what documents must be sent by mail to support the application you are submitting, and the appropriate mailing address.
Q How Can I Find Out If I Can Get Medicaid
A. You can find out if you qualify for Medicaid or other medical assistance and social service programs by speaking with a representative at your local State Service Center. Call Medicaid Customer Relations at 1-800-372-2022 or 255-9500 to be directed to the appropriate office where someone can help you.
You May Like: Braces Place That Take Medicaid
Q How Do I Join A Managed Care Organization
A. After being notified that you are eligible for Medicaid , you will receive in the mail a packet of information about the different MCO plan options for receiving your Medicaid benefits. You may choose any plan described in this mailing. You probably want to choose a Managed Care Organization to which your doctor belongs. If you need help making this decision, call the Health Benefit Manager at the phone number in the mailing.
Other Types Of Benefits And Programs For The Unemployed
Educational Help
Federal agencies offer many unemployment education and training programs. They are generally free or low cost to the unemployed.
Self-Employment Help
Self-employment assistance programs help unemployed workers start their own small businesses. Delaware, Mississippi, New Hampshire, New York, and Oregon offer this program.
Recommended Reading: Select Health Medicaid Provider Portal
Using Your Healthy Connections Plan
Q. What medical services does Medicaid cover? A. Within certain limits, Medicaid will pay for services that are medically necessary. Examples of services that may be covered include doctor visits, medications, hospital visits, and many other medical services.
If you have any questions about what is covered, to view a chart that shows each health plan and what they cover. You can also contact Healthy Connections toll-free at 1-888-549-0820.
Q. How long will my Medicaid benefits remain active? A. Eligibility for most Healthy Connections programs lasts for 1 year. After 1 year, South Carolina Health and Human Services will review your case annually.
Q. I was enrolled in S.C. Healthy Connections Choices and now am told I must choose between health plans. What should I do? A. The Healthy Connections Choices website offers comprehensive information on its health plans. Members may utilize a Quick Start Guide, search for doctors, compare plans, and more. Please visit S.C. Healthy Connections Choices for more information.
Q. Do I need to tell South Carolina Healthy Connections when I move or change jobs? A. Yes. If you have any changes to your income, resources, living arrangements, address or anything else that might affect your eligibility you must report these changes to Healthy Connections right away at 1-888-549-0820.
Q. What if my Medicaid card is lost or stolen? A. Report a lost or stolen card to Healthy Connections immediately at 1-888-549-0820.
Most Medicaid Enrollees Get Care Through Private Managed Care Plans
Over two-thirds of Medicaid beneficiaries are enrolled in private managed care plans that contract with states to provide comprehensive services, and others receive their care in the fee-for-service system . Managed care plans are responsible for ensuring access to Medicaid services through their networks of providers and are at financial risk for their costs. In the past, states limited managed care to children and families, but they are increasingly expanding managed care to individuals with complex needs. Close to half the states now cover long-term services and supports through risk-based managed care arrangements. Most states are engaged in a variety of delivery system and payment reforms to control costs and improve quality including implementation of patient-centered medical homes, better integration of physical and behavioral health care, and development of value-based purchasing approaches that tie Medicaid provider payments to health outcomes and other performance metrics. Community health centers are a key source of primary care, and safety-net hospitals, including public hospitals and academic medical centers, provide a lot of emergency and inpatient hospital care for Medicaid enrollees.
Figure 6: Over two-thirds of all Medicaid beneficiaries receive their care in comprehensive risk-based MCOs.
Recommended Reading: United Healthcare North Carolina Medicaid
Q How Much Income Can I Receive And Still Be Eligible For Medicaid
A. Income is money that you get from working, or money that someone gives you, or checks that you receive, such as a Social Security check, unemployment benefits, child support, retirement benefits, or sick pay. Whether your income level qualifies you or your family for Medicaid depends on the size of your family and the Medicaid program for which you are applying.
Income limits are set each year by the federal government to define the Federal Poverty Level for different family sizes. In general, if your household income is at or below the current 100% Federal Poverty Level for your household size, your family is likely to be eligible for Medicaid. Children from age 1 to under age 6 can qualify for Medicaid benefits when household income is at or below 133% of the Federal Poverty Level. Pregnant women and infants under age 1 qualify for Medicaid with family income at or below the 200% Federal Poverty Level, and pregnant women count as 2 family members.
See our tables of income limits for applying for DMMA programs to find out where your family income is, in relation to these income benchmarks.
Medical assistance programs other than Medicaid have different income level requirements. For example, uninsured children under age 19 who live in families with incomes at or below the 200% Federal Poverty Level are eligible for low cost health insurance under the Delaware Healthy Children Program.
What Is Not Covered By Montana Medicaid
Medicaid does not provide coverage for private podiatrists, chiropractors, naturopaths, psychologists, or therapists .
Medicaid is not obligated to pay for personal care services or nursing supplied by a family member. Bandages, adult diapers, and other disposable items are frequently excluded from coverage, as well as cosmetic surgery and other elective procedures.
Read Also: Does Pregnancy Medicaid Cover Emergency Room Visits
