Waivers With Eligibility And Enrollment Restrictions: Approved And Pending As Of January 12 2022
In December 2021, CMS under the Biden Administration notified several states with approved Section 1115 premium requirements that it had decided that these requirements are not likely to promote the objectives of Medicaid. In approving demonstration extensions for states with previously approved and implemented premiums , CMS renewed these premiums for one year only to allow for a phase-out period CMS notified Georgia that it was withdrawing the states authority to charge premiums. Eligibility restrictions including premium requirements had been a key Section 1115 waiver priority under the Trump Administration.
Taxes Or Fees Tied To Medicaid Expansion
Several states have explicitly raised taxes and fees to cover their share of Medicaid expansion. Other states already had provider taxes or fees that grew naturally with expansion. According to the most recent 50-state Medicaid Budget Survey, 11 states fund the state portion of expansion with new or expanded taxes or fees.16 However, nearly every state has at least one type of provider fee used to pay for Medicaid, and several have expanded or changed these taxes/fees since Medicaid expansion .17 These taxes or fees are often explicitly tied to Medicaid expansion. However, they are also used to fund traditional Medicaid, and state funding data often do not allocate funds between different parts of Medicaid. This makes it difficult to quantify the share of these taxes that directly fund expansion.
Exhibit 7 describes several taxes implemented by states to cover all or part of the state share of Medicaid expansion. The table is limited to taxes/fees where the amount of revenue allocated to expansion is clearly stated. Consistent with the 50-State Medicaid Budget Survey, several states impose taxes that raise sufficient revenue to pay the full sticker price of expansion.
Introduction: How Does Medicaid Expansion Affect State Budgets
Is expanding eligibility for Medicaid a good deal for states? This question has loomed over state policymakers for more than a decade. While hundreds of studies have detailed the costs and benefits of Medicaid expansion in terms of access to care, fiscal impacts, health outcomes, and other factors, consensus remains elusive.1 Many skeptics still question whether expansion is worthwhile from a budget perspective. Fourteen states still have not expanded Medicaid, and support for expansion in states that have done so is not unanimous.
In this brief, we focus on a common barrier to Medicaid expansion: concerns about its impact on state budgets. Expansion opponents often argue that its fiscal cost is too high. For the first three years, the federal government paid the full cost of expansion. States began covering a portion of expansions cost in 2017 and, starting in 2020, are responsible for 10 percent of its cost. Given recent spending levels, expansion states will collectively pay more than $7 billion in 2020. For the median expansion state, expansion will cost more than $100 million.2
Ultimately, while each states Medicaid program is unique and the impacts of expansion vary from state to state, the accumulated information points in a single direction: states do not pay the full cost of Medicaid expansion. The net impact on their general funds is much smaller than expansions costs. In some cases, Medicaid expansion more than pays for itself.
Also Check: Medicaid South Dakota Income Guidelines
Changes In State Medicaid Spending
Exhibit 1 illustrates the cumulative effects of expansion on states Medicaid spending using data from the National Association of State Budget Officers .4 Excluding the first state fiscal year of expansion , Medicaid expansion increases total Medicaid spending by approximately 23 percent and federal Medicaid spending by approximately 38 percent, but it does not increase state Medicaid spending .
The teal bars show the two competing effects of expansion on state Medicaid spending. During FY2015 and FY2016, the federal government paid the full cost of expansion and Medicaid spending in expansion states declined by approximately 6 percent relative to nonexpansion states. In FY2017, states began paying a share of the cost of expansion , which grew each year between FY2017 and FY2020. As the share of Medicaid expansion costs paid by the states grew, net savings fell. However, at least through FY2019 in the average state, expansion generated sufficient savings to states traditional Medicaid programs to offset its costs.
This suggests that Medicaid expansion generates substantial savings in states traditional Medicaid programs because states expansion costs are significant. As shown in Exhibit 2, state spending on Medicaid expansion exceeded $4 billion in 2018 and, if spending remains at current levels, will exceed $7 billion in 2020 .
Quality Total Points: 3333
- Adult Care Quality : Full Weight Note: This metric measures performance rates on frequently reported health care quality measures in the CMS Medicaid Adult Core Set.
- Medicaid Denial Rate for In-Network Claims by Healthcare.gov Issuers: Full Weight
- Transparency in Reporting Quality Measures: Full Weight Note: This metric measures the share of voluntarily reported sets of core measures showing the quality of care and health outcomes for adults participating in Medicaid, and children enrolled in Medicaid and the Childrens Health Insurance Program .
Recommended Reading: Dentist In Great Falls Mt That Take Medicaid
The Human Toll Of The Medicaid Coverage Gap
Of course, theres more to Medicaid expansion than just money. Harold Pollack very clearly explains the human toll of the Medicaid coverage gap: Based on the 3,846,000 people who were expected to be in the coverage gap in January 2015, we can expect 4,633 of them to die in any given year because they dont have health insurance.
What Are The Reasons For Not Expanding Medicaid
Here are twelve reasons states should not expand Medicaid and should instead demand from Washington greater control over spending to better fit coverage expansion with their states needs, resources, and budgets. 1. Medicaid harms the poor. The Medicaid program actually harms the people it is intended to serve.
Don’t Miss: Dc Medicaid Customer Service Number
How Many Uninsured People Who Could Have Been Eligible For Medicaid Are In The Coverage Gap
Nationally, more than two million3 poor uninsured adults fell into the coverage gap that results from state decisions not to expand Medicaid , meaning their income was above Medicaid eligibility but below the lower limit for Marketplace premium tax credits. These individuals would be eligible for Medicaid had their state chosen to expand coverage. Reflecting limits on Medicaid eligibility outside ACA pathways, most people in the coverage gap are adults without dependent children.4
Adults left in the coverage gap are spread across the states not expanding their Medicaid programs but are concentrated in states with the largest uninsured populations. More than a third of people in the coverage gap reside in Texas, which has both a large uninsured population and very limited Medicaid eligibility . Nineteen percent of people in the coverage gap live in Florida, twelve percent in Georgia, and ten percent in North Carolina. There are no uninsured adults in the coverage gap in Wisconsin because the state is providing Medicaid eligibility to adults up to the poverty level under a Medicaid waiver.
Figure 2: Distribution of Adults in the Coverage Gap, by State and Region, 2019
Looking Back Adoption Of The Original Program And The Adoption Of Medicaid Expansion
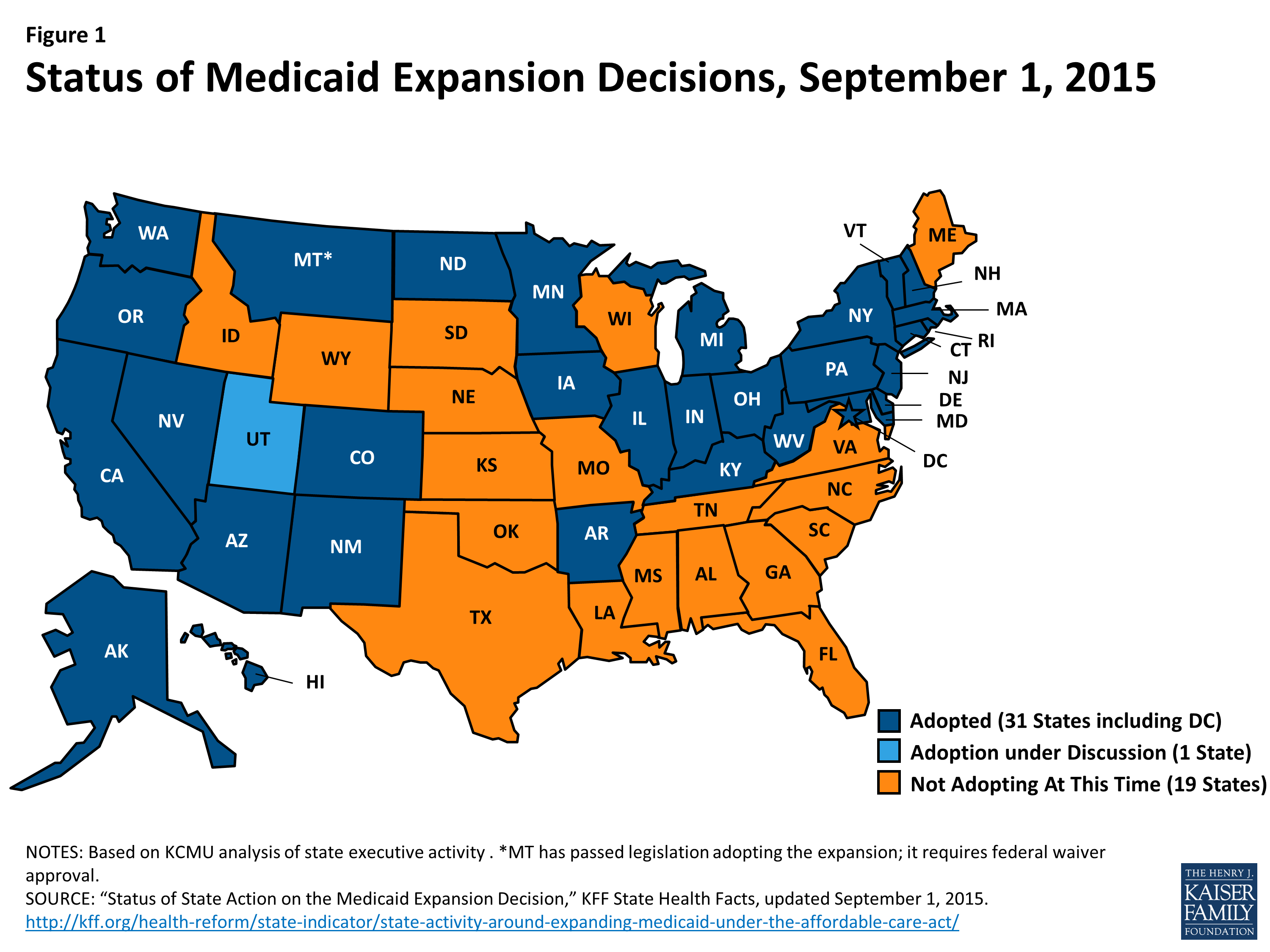
While the court ruling represents in many ways the back-and-forth intensity of the current political times, the dynamics at the time of the original adoption of the Medicaid program were every bit as compelling. As Figure 1 notes, it took 16 years for 50 states to adopt Medicaid programs. While 49 states adopted the program by 1970 the last holdout, Arizona, did not adopt Medicaid until 1982 a full 12 years after the 49th adoption. There are certainly parallels between the order in which states adopted Medicaid and the order in which states adopted Medicaid expansion, as Figure 1 demonstrates.
Some key assumptions were made in the categorization of states in Figure 1:
- Wisconsin is considered an expansion state due to childless adults being covered under the BadgerCare program that pre-existed the ACA
- Idaho, Utah, Maine and Nebraska are categorized as pending given the successful Medicaid expansion ballot initiatives in those states
- Kansas remains in the non-expansion category due to the opposition of the state legislature, although the election of a new Governor who supports expansion may boost the chances of expansion in 2019 or in subsequent years.
Figure 1 Adoption of Medicaid in 1966 Compared to 2014 Medicaid Expansion Provisions enabled by ACA
Don’t Miss: Does Medicaid Cover Gastric Bypass In Michigan
Medicaid Waiver Tracker: Approved And Pending Section 1115 Waivers By State
This page aggregates tracking information on pending and approved Section 1115 Medicaid waivers. Scroll down or click on the links below to jump to resources such as an overview map and figure, detailed waiver topic tables, and explanatory briefs.
Previously-approved Section 1115 work requirements have been withdrawn by CMS under the Biden Administration and are reflected on the Work Requirements Tab. Additionally, the detailed Waivers with Eligibility and Enrollment Restrictions table on this tab includes still-pending work requirement requests.
For information on Section 1115 waiver approvals related to COVID-19, see our Medicaid Emergency Authority Tracker.
Landscape of Approved vs. Pending Section 1115 Medicaid Demonstration Waivers, January 12, 2022
Tracker contents:
Medicaid Expansion Presents Opportunity For The South
Georgia, Mississippi, and Louisiana are among the 12 states that have not expanded Medicaid in the face of robust financial incentives and moral imperatives to do so. 8 of the 12 states are in the geographic South.
The disproportionate majority of the Georgians trapped in the Medicaid coverage gap are Black, Hispanic, Asian or Pacific Islanders, and those who live in rural communities. Those left in the Medicaid coverage gap are forced to make unfair and heartbreaking decisions about how to care for their families, their children, and themselves.
We can work together to end the devastating impacts of medical debt on the uninsured by expanding Medicaid. Not only would expanding Medicaid improve health outcomes for millions of Americans, it would also create more than 1 million jobs nationwide, with largest gains in:
- Texas
- North Carolina , and
- Georgia
Collectively, the 12 states that have not acted yet to protect their citizens could expand their economies by over $300 billion from 2022 to 2025 if they expanded Medicaid.
We must demand that our elected officials expand Medicaid in Georgia and the 11 other states that continue to refuse to help hard-working Americans who deserve access to quality healthcare. The future of our countrys well-being and the lives of our community members are on the line.
Read Also: Assisted Living Facilities In Arkansas That Accept Medicaid
Where The $100 Billion Figure Comes From
When we reached out to O’Rourke’s campaign for evidence to support the claim, an official pointed us to a 2018 editorial from the Houston Chronicle that shared the opinion that turning down federal funding for Medicaid expansion puts the onus on counties to figure out how to serve uninsured people.
The editorial board wrote, “Under the plan passed as part of the Affordable Care Act in 2014, Texas would have received an estimated $100 billion over the course of a decade in exchange for increasing Medicaid eligibility to 138 percent of the poverty line.”
In 2021, 138% of the federal poverty line works out to an income of $17,774 for an individual and $36,570 for a family of four.
Texas lags behind the rest of the nation when it comes to health care coverage. According to 2019 Census Bureau health insurance coverage data released in 2020, nearly 1 in 5 Texans, or 18.4%, are uninsured.
Adults without dependents or disabilities are not eligible for Medicaid regardless of income in Texas, and parents of dependent children are eligible up to about 14% of the federal poverty level, according to a 2020 Texas A& M study on Medicaid expansion for Episcopal Health Foundation, an advocate for Medicaid expansion.
So, Texas has a coverage gap between Medicaid eligibility and eligibility for a federally subsidized Affordable Care Act Marketplace plan that begins at 100% of the federal poverty line.
History Of Medicaid Expansion
As noted at the start of this summary, Medicaid was a cornerstone of ACA lawmakers efforts to expand access to healthcare. The idea was that everyone with household incomes up to 133% of the federal poverty level would be able to enroll in Medicaid.
People above that threshold would be eligible for premium tax credits in the exchanges to make their coverage affordable, as long as their income didnt exceed 400% of the poverty level. The idea was that people with income above 400% of the poverty level would be able to afford coverage without subsidies, but that has not proven to be the case. So the American Rescue Plan temporarily eliminated the income cap for subsidy eligibility, and the Build Back Better Act aims to extend that for several more years.
Because Medicaid expansion was expected to be a given in every state, the law was written so that premium subsidies in the exchange are not available to people with incomes below the poverty level. They were supposed to have access to Medicaid instead.
You May Like: Who Qualifies For Medicaid In Kansas
States Still Say No To Medicaid Expansion
Unfortunately for millions of uninsured Americans, in 2012 the Supreme Court ruled that states could not be penalized for opting out of Medicaid expansion. And a dozen states have not yet expanded their programs.
Until late 2015, there were still 22 states that had not expanded Medicaid, but Montana began enrolling people in their newly expanded Medicaid program in November 2015, for coverage effective January 2016, Alaskas Medicaid expansion took effect in September 2015, Louisianas Medicaid expansion took effect in July 2016, and Virginia began enrolling people in expanded Medicaid as of November 2018, for coverage effective January 2019. Maine expanded Medicaid as soon as Governor Mills took office in early 2019. Utah and Idaho both implemented full Medicaid expansion as of 2020, and Nebraskas Medicaid expansion took effect in October 2020. Medicaid expansion took effect in Oklahoma in July 2021, and in Missouri in October 2021.
As a result of those 12 states refusal to accept federal funding to expand Medicaid, the Kaiser Family Foundation estimates there are 2.2 million people in the coverage gapacross 11 of those states .
Being in the coverage gap means you have no realistic access to health insurance. These are people with incomes below the poverty level, so they are not eligible for subsidies in the exchange. But they are also not eligible for their states Medicaid program.
What States Are Next To Watch
After the 2018 November election and ballot initiative results, 37 states have adopted or are poised to adopt Medicaid expansion. Voters in Utah, Nebraska, and Idaho elected to expand Medicaid on their 2018 midterm ballots. Each of these states has discussed work requirements for Medicaid enrollees, and Utah has drafted a waiver.
Figure 2 identifies the remaining non-expansion states and provides context as to the size of the potential expansion population relative to existing Medicaid enrollment. A subset of non-expansion states to watch are states that allow ballot initiatives Florida, Oklahoma, Missouri, Mississippi, and Wyoming. Additionally, hospital and hospital associations continue the push for expansion, either at the statewide level or even a regional approach, as hospitals exhaust substantial resources as required by the EMTALA law to provide medical screenings and treatments for emergency medical conditions.
Figure 2 13 Non-Expansion States Medicaid and Coverage Gap Populations
| State | |
| 11.5% |
Also Check: Anthem Medicaid Ky Dental Providers
If Your Income Is Low And Your State Hasnt Expanded Medicaid
If your state hasnt expanded Medicaid, your income is below the federal poverty level, and you don’t qualify for Medicaid under your state’s current rules, you wont qualify for either health insurance savings program: Medicaid coverage or savings on a private health plan bought through the Marketplace.
- Find out why
-
- When the health care law was passed, it required states to provide Medicaid coverage for all adults 18 to 65 with incomes up to 133% of the federal poverty level, regardless of their age, family status, or health.
- The law also provides premium tax credits for people with incomes between 100% and 400% of the federal poverty level to buy private insurance plans in the Health Insurance Marketplace®.
- The U.S. Supreme Court later ruled that the Medicaid expansion is voluntary with states. As a result, some states havent expanded their Medicaid programs.
- Adults in those states with incomes below 100% of the federal poverty level, and who dont qualify for Medicaid based on disability, age, or other factors, fall into a gap.
- Their incomes are too high to qualify for Medicaid in their states.
- Their incomes are below the range the law set for savings on a Marketplace insurance plan.
-
States are continuing to make coverage decisions. They could expand Medicaid in the future.
Work Requirements For States That Have Not Expanded Medicaid:
Several states that have not expanded Medicaid have sought federal permission to impose Medicaid work requirements, despite the fact that their Medicaid populations are comprised almost entirely of those who are disabled, elderly, or pregnant, as well as children.
The Trump Administration has begun granting work requirements in some of these states, although CMS Administrator, Seema Verma clarified in May 2018 that these states would have to clearly demonstrate how they plan to avoid situations in which people lose access to Medicaid as a result of the work requirement, and yet also do not have access to premium subsidies in the exchange.
Non-expansion states with approved work requirement waivers that have since been withdrawn by HHS
Two non-expansion states have been granted federal approval to implement Medicaid work requirements for their existing Medicaid populations:
Non-expansion states seeking federal permission to impose a Medicaid work requirement:
Note that these states waiver proposals were all pending when the Biden administration took office, and none have been approved. The Biden administration has noted that work requirements are not in line with the overall mission of Medicaid .
- Tennessee (pending CMS approval 20 hours per week.
- Oklahoma
You May Like: Pregnancy Medicaid Ga Phone Number
