How Do I Enroll In Montana Individual And Family Insurance
For individuals, its a relatively straightforward process to compare plan costs and decide the best value plan. However, getting the best family health plan requires more foresight in planning for future health issues. There are some important considerations when shopping for coverage, whether for yourself or for multiple people. These considerations include:
- Individual vs. family deductibles
Montana Homeowner/renter Credit Program
The Montana Elderly Homeowner/Renter Credit program is a property tax relief program that provides a refundable income tax credit of up to $1,000. Montana homeowners or renters age 62 or older may qualify for this program even if you do not have to file an income tax return if they meet the eligibility criteria.
Montana Department of Revenue1201 US Hwy 10 West, Unit D2Livingston, MT 59047
You May Like: Pediatric Dentist St Louis Medicaid
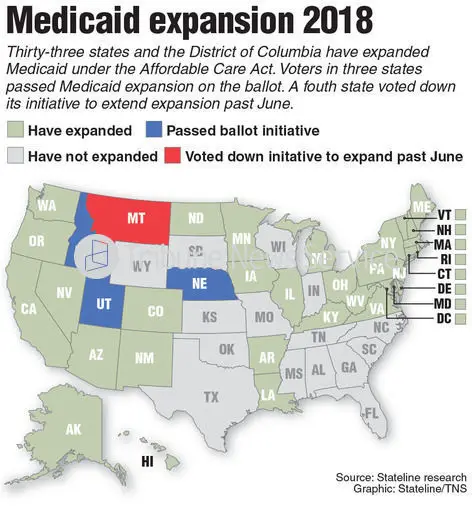
Montanas Medicaid Expansion Waiver Allows For Medicaid Premiums Hb658 Would Have Increased Them But Cms Rejected That Proposal And Is Ending The Premiums Altogether After 2022
Any version of Medicaid expansion that places additional requirements or restrictions on enrollment must be granted a waiver from CMS in order to receive federal funding. Montanas Medicaid expansion legislation that was enacted in 2015 deviated from the straight Medicaid expansion called for in the ACA bill sponsor Ed Buttrey called it the most conservative plan in the US.
S.B.405 called for newly-eligible enrollees to pay 2% of their income in premiums, and it also imposes copays for some medical services. In addition, the legislation included a job training and workforce assessment program, aimed at helping enrollees secure a job or move into a better job .
So although SB405 was the law of the land in Montana, the state still needed to get approval from CMS to proceed with their modified version of Medicaid expansion. On July 7, 2015, the state posted the waiver application and began a 60-day public comment period. Montana residents had an opportunity to comment on the proposal online, and there were two public meetings about the proposal in August.
As noted above, H.B.658, enacted in 2019, calls for premiums to gradually increase to 4% of income, although they would stay at 2% for the first two years a person is enrolled in the program, and premium increases would not apply to people who are exempt from the Medicaid work requirement. But at 4% of income, premiums for Montanas Medicaid would be by far the highest in the country.
Also Check: How Can I Switch My Medicaid Plan
Renew Your Medicaid Or Chip Coverage
As COVID-19 becomes less of a threat, states will restart yearly Medicaid and CHIP eligibility reviews. This means your state will use the information they have to decide if you or your family member still qualify for Medicaid or CHIP coverage. If your state needs more information from you to make a coverage decision, theyll send you a renewal letter in the mail. Go to Medicaid.gov/renewals, find a link to your state Medicaid office and confirm your contact information is up-to-date.
An official website of the United States governmentHeres how you know
Official websites use .gov
Dphhs Preparing For Healthcare Coverage Renewal Process That Begins Later This Year
In anticipation of the federal public health emergency ending soon, Department of Public Health and Human Services officials will soon launch an extensive outreach campaign to Montana Medicaid and Healthy Montana Kids families about upcoming changes that could impact their healthcare coverage.
One of the first critical steps in the process is encouraging the thousands of Montanans who currently receive healthcare through DPHHS to ensure their contact information on file is current.
Its imperative that Montanans update their contact information with DPHHS to ensure they will receive upcoming notices related to their healthcare coverage,DPHHS Director Adam Meier said.We encourage people to utilize one of the numerous options available to complete this crucial task.
The PHE was declared in March 2020 in response to the COVID-19 pandemic. Meier said that DPHHS adjusted its eligibility processes for Medicaid and HMK programs so individuals would keep their healthcare coverage during the emergency.
However, with the PHE anticipated to end in July, some individuals could lose coverage if DPHHS is not able to reach them to verify current eligibility status.
We anticipate many of our clients have changed addresses, phone numbers, and emails over the past couple years, so now is the time to update that information,Meier said.
Updates can be made the following ways:
To assist the public, here is a brief informational guide on the Medicaid changes.
Read Also: Will Medicaid Pay For Root Canal
View Or Download Our Free Guide
While we are not affiliated with the government in any way, our private company engaged writers to research the Medicaid program and compiled a guide and the following answers to frequently asked questions. Our goal is to help you get the benefits that you need by providing useful information on the process.
Our free Medicaid Guide is filled with helpful information about how to apply, program eligibility and how to get in touch with local offices. You can view or download our free guide here.
Rapid Drop In Uninsured With No Decline In Employer Coverage
When states expand Medicaid, they experience steep reductions in the number of uninsured people, which drives many of the fiscal benefits to states. After Montana implemented its expansion on January 1, 2016, the uninsured rate fell steeply while Medicaid enrollment increased roughly 50 percent in only two years. This result is unsurprising, as numerous studies have demonstrated large coverage gains for uninsured people in states that expanded Medicaid.
A simple comparison of uninsured rates in Wyoming and Montana before and after Montanas expansion illustrates the impact of Montanas expansion on the uninsured rate. During the first year of the expansion, the uninsured rate among non-elderly adults dropped by one-quarter, from 16 percent in 2015 to 12 percent in 2016. In contrast, Wyomings uninsured rate rose from 14 to 15 percent during that period. By 2019, Montanas uninsured rate was still 12 percent while Wyomings had further increased to 17 percent.
Recommended Reading: Does Medicaid Cover Deep Teeth Cleaning
How To Qualify For Medicaid
Almost every state has multiple Medicaid programs. But, as a good rule of thumb, if you make less than 100% to 200% of the federal poverty level and are pregnant, elderly, disabled, a parent/caretaker or a child, thereâs likely a program for you. And if you make less than 133% of the FPL**, thereâs possibly a program for you, depending on whether your state expanded Medicaid under Obamacare. In 2021, the federal poverty levels range from $12,880 to $44,660 .
In 2021, the federal poverty level in Alaska ranges from $ $16,090 to $55,850 . The federal poverty level in Hawaii ranges from $14,820 to $51,360 .
What Is Montana Medicaid Fax Number
Montana Medicaid fax number where you can send fax messages including application forms for Montana state health insurance is 888-772-2341.
Are you looking for additional information for Montana Medicaid and Montana state health insurance? Do you need any assistance with Montana Medicaid? Please contact us and we will be happy to help you with any Medicaid application related matter.
You May Like: Will Medicaid Pay For Assisted Living In Ohio
Oregon Medicaid Health Experiment And Controversy
In 2008, Oregon decided to hold a randomized lottery for the provision of Medicaid insurance in which 10,000 lower-income people eligible for Medicaid were chosen by a randomized system. The lottery enabled studies to accurately measure the impact of health insurance on an individual’s health and eliminate potential selection bias in the population enrolling in Medicaid.
A sequence of two high-profile studies by a team from the Massachusetts Institute of Technology and the Harvard School of Public Health found that “Medicaid coverage generated no significant improvements in measured physical health outcomes in the first 2 years”, but did “increase use of health care services, raise rates of diabetes detection and management, lower rates of depression, and reduce financial strain.”
The study found that in the first year:
How To Appeal An Application Denial
Medicaid applications will be denied if applicants do not meet the eligibility requirements. Also, beneficiaries can have their benefits terminated or reduced if their eligibility status changes while they are enrolled.
Learn more about Montana Medicaid eligibility requirements here.
If your Medicaid application is denied or your benefits amount is reduced, you have the right to file an appeal. You must send a written appeal request by the date shown on your determination letter. Your letter will also include instructions for filing your appeal with the DPHHS.
The Montana Department of Public Health and Human Services will review your claim and may ask for additional information or evidence of your eligibility. If you are granted a hearing, you will receive a notice with the date, time and location of the hearing.
Also Check: Medicaid Office San Antonio Tx
Read Also: Does Target Vision Accept Medicaid
What Are Montanas Medicare Options For Seniors And People With Disabilities
The federally funded Medicare program is generally aimed at 65s and over. However, people under 65 with disabilities may also be covered by Medicare. You can qualify if you have end-stage renal disease, ALS, or have received disability benefits for 24 months.
In Montana, people eligible for Medicare have two choices to sign up with Original Medicare or Medicare Advantage.
- Original Medicare has been around since 1965. It consists of two parts hospital insurance and medical insurance . However, prescription medications are not covered, and neither are dental or vision health services. You can purchase a Part D plan for prescription medication. The Medicare Part A deductible for inpatient hospital stays is $1,600 in 2023. Medicare Part B enrollees pay a standard monthly premium of $226 for 2023.
- Medicare Advantage is an Individual health insurance alternative to Original Medicare. Medicare Advantage plans cover hospital and medical services, prescription medications, and often, the choice of dental and vision care all rolled into one health plan package. As of 2023, there are 26 Medicare Advantage Plans available in the state, however, you can only select a plan thats available in your county.
Medicare Supplement Insurance plans can cover health costs Original Medicare doesnt, including copays. Individual insurers in Montana sell Medigap plans.
Eligibility
Enrollment
How Medicaid Eligibility Is Determined
Income eligibility is determined by your modified adjusted gross income , which is your taxable income, plus certain deductions. Those deductions include non-taxable Social Security benefits, individual retirement contributions and tax-exempt interest. For most people, MAGI is identical or very close to your adjusted taxable income, which you can find on your tax return. Specific income requirements in dollars rise alongside the size of your household.
Our guide focuses on each stateâs major programs for adults. Most are only available to state residents, U.S. citizens, permanent residents or legal immigrants .
Recommended Reading: Dentist In Little Rock That Accept Medicaid
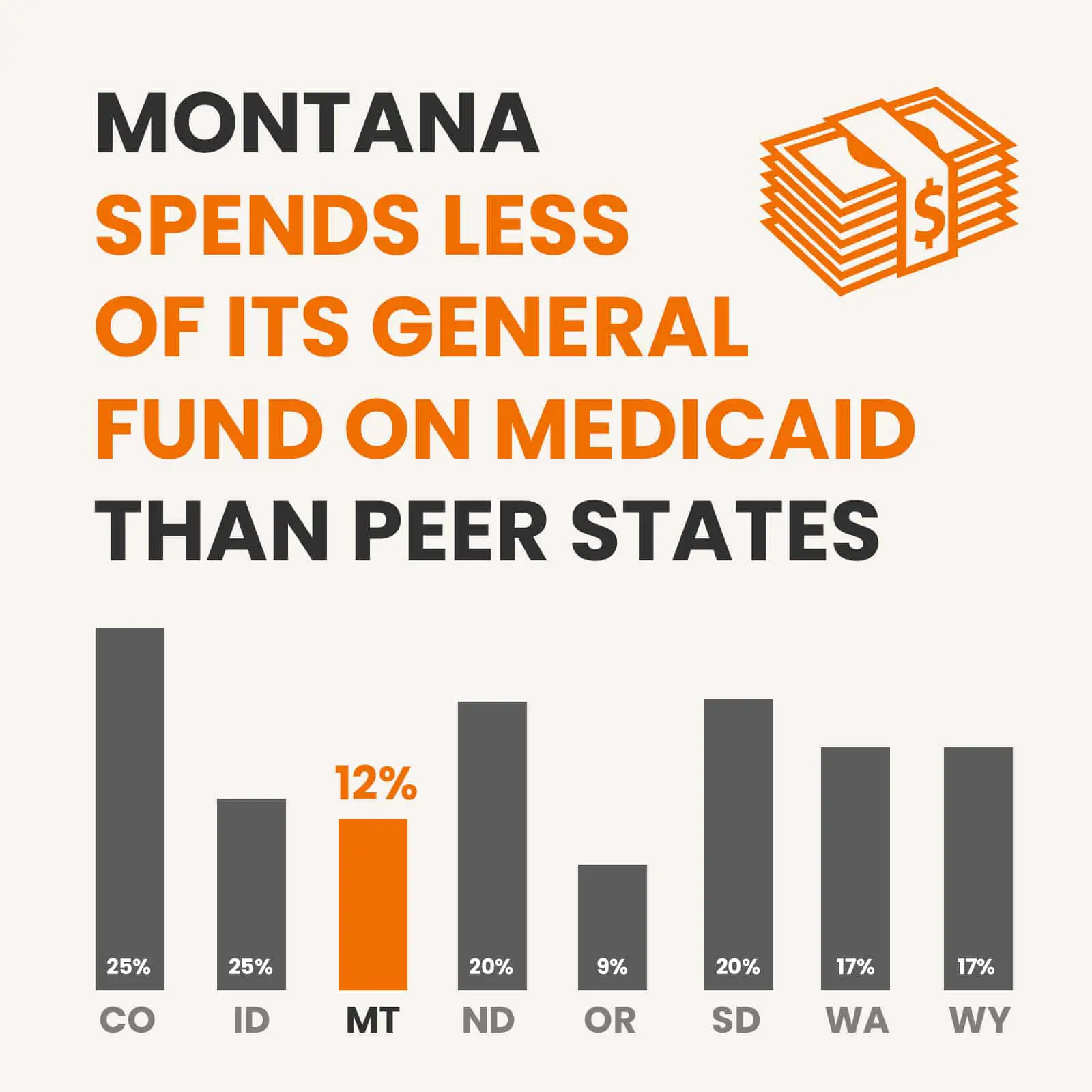
State And Federal Spending
During fiscal year 2016, Medicaid spending nationwide amounted to nearly $553.5 billion. Spending per enrollee amounted to $7,067 in fiscal year 2013, the most recent year for which per-enrollee figures were available as of June 2017. Total Medicaid spending grew by 33 percent between fiscal years 2012 and 2016. The Medicaid program is jointly funded by the federal and state governments, and at least 50 percent of each state’s Medicaid funding is matched by the federal government, although the exact percentage varies by state. Medicaid is the largest source of federal funding that states receive. Changes in Medicaid enrollment and the cost of healthcare can impact state budgets. For instance, in Montana, the percentage of the state’s budget dedicated to Medicaid rose from 15.4 percent in 2010 to 17.4 percent in 2015. However, state cuts to Medicaid funding can also mean fewer federal dollars received by the state.
During fiscal year 2016, combined federal and state spending for Medicaid in Montana totaled about $1.4 billion. Spending on Montana’s Medicaid program increased by about 42.1 percent between fiscal years 2012 and 2016. Hover over the points on the line graph below to view Medicaid spending figures for Montana. Click on the red bar below the graph to view these figures as compared with three of Montana’s neighboring states.
What You Need To Apply:
- The name, address, contact info, and birth date for everyone in your household
- Social security numbers and/or immigration documents
- Employer and income information for everyone in your household. Examples include pay stubs or W2 forms.
- Other income information including Social Security Administration or Supplemental Security Income payments and mentions
- Information about current health coverage for members of your household, including coverage through an employer, a spouse’s employer, or Medicare
Recommended Reading: Psychiatrist In Baton Rouge That Accept Medicaid
Insurance For Individuals In Montana
Before deciding on a specific health plan, consider two types of costs: monthly premiums and out-of-pocket expenses. Annual deductible, copay, and coinsurance costs collectively make up the out-of-pocket side of the equation.
If youre in good health and dont plan to use your insurance often, you may save the most money by enrolling in the plan with the lowest premium. Youll be covered in the event of a sudden illness or injury, but you wont have to worry about paying a high premium each month.
If you have a chronic health condition, however, you need to weigh the low premium against other out-of-pocket costs. A plan that costs $350 per month and has a $500 deductible may be a better fit for your financial needs than a plan that costs $250 per month and has a $5,000 deductible if you require regular medical care. A more expensive plan may also give you access to more specialists or better coverage for your prescriptions.
There are several different plans from which you can choose:
Where Do You Sign Up For Medicaid With Personal Documents In Montana
A caseworker must examine original documents to understand whether or not an applicant can sign up for Medicaid hospital services, dental care, emergency room treatment and more, based on the candidates living situation, finances, resources and residency when he or she applies. Examples of documentation that will be accepted with Medicaid applications include:
- Financial statements going back at least five years
- Valid social security number
- Application for other benefits
Read Also: How To Find Out What Your Medicaid Covers
Who Is Eligible For Montana Medicaid
In addition to low-income elderly residents and those who are disabled, Medicaid is available to the following populations in Montana:
- Pregnant women with household incomes up to 157% of poverty.
- Adults under age 65 with household income up to 138% of poverty
- Children are eligible for Medicaid if their household incomes are up to 143% of poverty. Above that level, they are eligible for CHIP if their household incomes do not exceed 261% of poverty.
- Cancer screening services are available to residents with household incomes up to 200% of poverty.
What To Know About Insurance In Montana
- Individual health insurance plans are available to individuals, families, and self-employed people with no employees. You can buy individual health insurance as long as youre a legal Montana resident.
- Open enrollment: Open enrollment dates in Montana are through November until January 15 each year. New health plans can be signed up for or amendments to existing plans made during this period.
- Special enrollment: Outside of the open enrollment period, special enrollments are available when you experience milestone life events such as moving to a new address, marriage, or having a baby are eligible for Special Enrollment Periods. You have 60 days from the actual event to make health insurance changes.
- Health Insurance Marketplace: Montana does not have a state exchange and uses the federal exchange. Individual health insurance plans in Montana can be bought through Healthcare.gov. Nearly 248,000 individuals are enrolled in Medicare in Montana. All Affordable Care Act health plans guarantee coverage for defined essential benefits.
- Coverage types: Montana employers covered 43% of insured residents. Federal and state funded programs Medicaid and Medicare-had enrollees of 20.8% and 18.1%. Non-group insured made up 8%, while the military only covered 1.8%. Uninsured Montanans were at 8.3%.
You May Like: I Have Medicaid And Im Pregnant
How To Apply For Coverage And Get Covered
Work with an enrollment assister. You can complete an application on your own or work with a Navigator, Certified Application Counselor, or Certified Exchange Producer . With just a zip code you can find a local enrollment assister who can answer questions and help you apply for and enroll in health insurance.Remember, their help is always free and confidential. They will help you get covered!
You can apply over the phone or virtually with the help of the Cover Montana Help Line: .
You can apply online at HealthCare.gov.
Children’s Health Insurance Program

The Children’s Health Insurance Program is a public healthcare program for low-income children who are ineligible for Medicaid. CHIP and Medicaid are related programs, and the former builds on Medicaid’s coverage of children. States may run CHIP as an extension of Medicaid, as a separate program, or as a combination of both. Like Medicaid, CHIP is financed by both the states and the federal government, and states retain general flexibility in the administration of its benefits.
CHIP is available specifically for children whose families make too much to qualify for Medicaid, meaning they must earn incomes above 138 percent of the federal poverty level, or $33,948 for a family of four in 2017. Upper income limits for eligibility for CHIP vary by state, from 175 percent of the federal poverty level in North Dakota to 405 percent of the FPL in New York. States have greater flexibility in designing their CHIP programs than with Medicaid. For instance, fewer benefits are required to be covered under CHIP. States can also charge a monthly premium and require cost sharing, such as copayments, for some services the total cost of premiums and cost sharing may be no more than 5 percent of a family’s annual income. As of January 2017, 14 states charged only premiums to CHIP enrollees, while nine states required only cost sharing. Sixteen states required both premiums and cost sharing. Eleven states did not require either premiums or cost sharing.
You May Like: Spend Down To Qualify For Medicaid
