The Sam Exclusion List
Employers should also be cognizant of another exclusion list managed by the US government, The System for Award Management . Its primary purpose is for businesses, organizations, and federal agencies to win US government contracts.
SAM was developed in 2012 when the General Services Administration consolidated several federal award and procurement systems into one streamlined system. This was done to eliminate duplicate data entry, improve data quality, and save taxpayer money. Just as the OIG maintains an exclusion list, SAM does as wellexcept this list includes contractors and entities who are excluded from working with the federal government.
While theres a lot of overlap between the two exclusion lists, there are some differences employers need to be aware of:
Mandatory And Permissive Exclusions
While many exclusions are the result of fraudulent or abusive behavior, others are levied due to administrative actions. Regardless of the type or reason, the excluded party is barred from directly or indirectly receiving government healthcare dollars until reinstated.
There are two types of exclusions, mandatory and permissive, depending on the severity of the excluded partys actions. Mandatory exclusions carry a longer required duration. The reasons for exclusions are described in the Social Security Act 1128.
Mandatory Exclusions
- Sexual assault
- License revocation due to any of the above
The mandatory exclusion can last from five years up to 50 yearsand in certain cases, can be permanent if the felony warrants it.
Permissive Exclusions
To receive a permissive exclusion, an individual or entity must have received a misdemeanor conviction for the crimes listed above. Defaulting on a federal student loan also can also result in a permissive exclusion. The permissive exclusion can last up to five years, but typically lasts one to three years.
When the exclusion period is over for either a mandatory or permissive exclusion, the individual or entity must apply for reinstatement at the federal and state level. Reinstatement is not automatic after the duration has expired.
Placement On An Exclusion List
Providers named on the excluded providers list have been terminated due to fraud, theft, abuse, error or noncompliance in connection with a Minnesota health care program. Providers are notified that they are being terminated before they are named on the published list. They are not eligible for payment from MHCP effective the date of the notification. Excluded providers are not prohibited from providing services for private-pay clients.
Recommended Reading: Does Medicare Or Medicaid Cover Cremation
What Does The Oig Govern
There are 11 departments in the HHS OIG organization: They revolve around auditing, investigating, enforcement, evaluating, and policy making. For the purpose of this blog, well be addressing the enforcement function of the OIG.
There are three departments that focus on the enforcement of health care fraud, waste, and abuse.
Oig Exclusion List Database
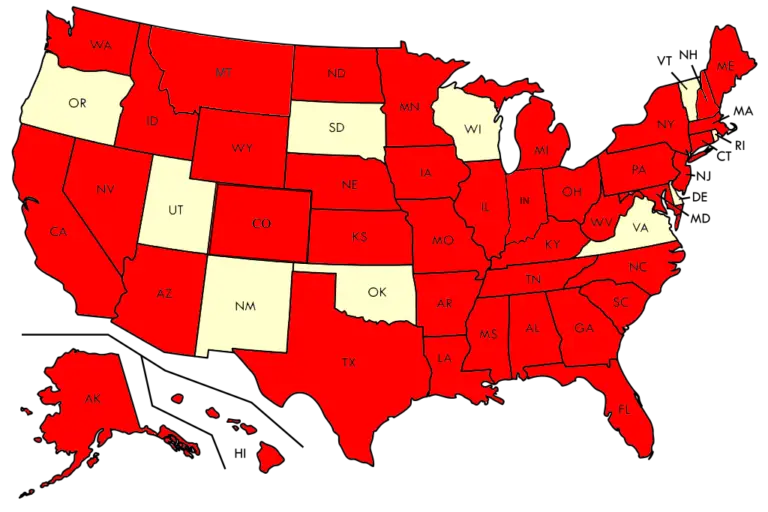
Understanding the differences between the exclusion datasets in the healthcare compliance industry can be overwhelming at times. To clarify, there are two main federal exclusion lists and 42 available state Medicaid exclusion lists. All of these exclusion lists need to be individually cross-checked and monitored on a monthly basis in order to remain compliant.
The most familiar safeguard for our industry is the HHS OIGs List of Excluded Individuals and Entities . The LEIE, along with the other federal datasets, exists to inform the healthcare industry of currently excluded individuals, likely due to an offense related to fraud or abuse. A person or entity becomes excluded, or sanctioned, and is placed on the LEIE, maintained by the OIG.
To make it even more complicated, not every list shares the same data with the OIG on a timely basis, let alone with each other. Excluded individuals or entities can be found on federal or state exclusion lists. In some cases, Medicaid Fraud Control Units also have Medicaid exclusion lists as well.
Recommended Reading: How Does Emergency Medicaid Work
Using The Medicaid Exclusion List
Anyone can use the LEIE database to find excluded individuals or entities.
For limited or individual searches, users can search for up to five names at once using Social Security Numbers or Employer Identification Numbers .
For more extensive searches, the OIG recommends downloading the entire list into a spreadsheet or data program to find information. However, its important to note that the downloadable database doesnt have SSNs or EINs, so employers can only verify those people through the online database.
The OIG also provides a helpful list of search tips, like checking former names, hyphenated names, verifying results, and more.
About The Texas Exclusions Database
The Office of Inspector General works to protect the health and welfare of people receiving Medicaid and other state benefits. To help protect these recipients, OIG may prevent certain people or businesses from participating as service providers. The people or businesses who are excluded from participating as providers are added to the Texas Exclusions List.
A person, or entity, may be excluded for many reasons. These include, but are not limited to:
- A conviction for program-related fraud or patient abuse
- Being excluded from the Medicare program
Every service provider is responsible for making sure that no excluded individuals or entities are receiving state funds. Specifically, it is each provider’s or person’s responsibility to ensure that items or services furnished personally by, at the medical direction of, or on the prescription or order of an excluded person are not billed to the Titles V , XIX , XX , and/or other HHS programs after the effective date of exclusion. This section applies regardless of whether an excluded person has obtained a program provider number or equivalent, either as an individual or as a member of a group, prior to being reinstated.
When a person or entity is excluded from Medicaid, Title V, Title XX, and other HHS programs,
Recommended Reading: Medicaid Free Cell Phone Application
Exclusion Monitoring: How And When
CMS requires healthcare organizations to conduct monthly exclusion monitoring of all employees, contractors, vendors, and ordering and referring providers. But given the irregularity of primary source updates, an ongoing exclusion program is best practice. If you have an excluded provider in your organization, you need to know as soon as possible.
To find all the current exclusion sources, you can use our interactive exclusion map.
Given how tedious and time-consuming exclusion monitoring can become, most healthcare organizations choose to partner with a vendor like ProviderTrust who specializes in this monitoring and can provide a more efficient experience. But be aware: not all exclusion monitoring vendors successfully overcome the many challenges involved.
Searching State Exclusion Lists: Why It Matters For Assured Compliance
If your profession involves compliance management, you know the Office of Inspector Generals List of Excluded Individuals/Entities is the federal database for all Medicaid sanctions and no doubt your team checks it regularly for sanctioned providers. However, many investigations are conducted by state Medicaid offices and do not always include federal participation. Is your compliance team checking for sanctions and exclusions at the state level as well? If not, they should be.
In fact, OIG Best Practices state that you should also search every state sanction and exclusion list that corresponds with your business or service delivery location meaning, all states where you operate or have a physical business presence. Some organizations are required to check all 41 state Medicaid sanction lists, but if yours is not one of them, our compliance experts recommend at least checking border states and any other state where the providers in your network or health system have practiced in the past.
Why? Because state actions may appear before federal listings, and in some cases, the states and federal databases do not fully synchronize their entries. But, to be clear, if a person or organization you do business with is excluded by your state, you will face the full threat of repercussions, for hiring and reimbursing them, even if they do not appear on the federal exclusion list.
Read Also: What Does Medicaid Family Planning Services Cover
Iv Some States Require Screening Extraneous Lists
V. A Simple and Affordable Solution
Without a doubt, state and federal exclusion screening requirements are incredibly burdensome for most providers. If screening your employees against each federal and state list that your state requires is not cost effective for your office to do in-house, contact Exclusion Screening, LLC today at 1-800-294-0952 or fill out our online service form found below. We would be happy to discuss your specific state obligations, provide a cost assessment, and help you create your employee and vendor list.
Did you find this article interesting and/or helpful? Are you interested in hearing more insights, exclusion news, and updates about upcoming webinars and promotions? If so, please take the time to Subscribe to Our Newsletter. We will not share, sell, or distribute your information in anyway under any circumstances. The information provided will be used to send you Newsletters as you have requested.
Ashley Hudson, Associate Attorney at Liles Parker, LLP and former Chief Operating Officer for Exclusion Screening, LLC, is the author of this article.
See Letter from Centers for Medicare and Medicaid Services to State Medicaid Directors 5 .
Newsletter to All Providers, from the New Jersey Dept of Human Servs., et al., Excluded, Unlicensed or Uncertified Individuals or Entities .
Avoid Oig Penalties & Risks To Your Company With Healthcare Sanction Checks
For employers in the healthcare field and other regulated industries, a healthcare sanctions check is an important part of a comprehensive background check. Depending on the level you search you need, it helps you mitigate risks by searching more than 1,000 government sources to find any penalties, suspensions, or punitive or disciplinary actions taken against a healthcare professional.
Through this screening, employers can also verify information that typically isnt available through the OIG and SAM exclusion lists, including:
- The violation or reason for the exclusion
- Whether the exclusion is currently active
- The name of the source or board that took the disciplinary action
- The ability to add Ongoing Alerts to notify employers if an employee is added to an exclusion list
Ensuring that job candidates and employees arent listed on government exclusion lists is more than just doing a thorough screeningit helps avoid steep penalties and consequences that can be detrimental to your business and reputation.
Find out if your healthcare candidates are in good standing. GoodHire offers sanction checks and hundreds of employment screening services.
Read Also: Michigan Pregnancy Medicaid Income Limits
System For Award Management
SAM.gov now houses the old Excluded Parties List System which contains debarment actions taken by various federal agencies, including exclusion actions taken by the OIG. Not all OIG records are contained at SAM.gov, and the OIG recommends searching the OIG-LEIE database as the primary source for OIG-LEIE records.
The System for Award Management system is to prevent companies from doing business with an individual or entity that has been debarred, sanctioned, or excluded by a federal agency.
List Of Suspended And Excluded Providers
MassHealth updates the list of suspended or excluded providers on a monthly basis. The update is posted around the second week of the month for the previous month.
See below for the list.
Questions regarding this list can be directed to:
- For OLTSS providers, please email the MassHealth .
- For dental providers, please call the MassHealth Dental Program Customer Service at 207-5019.
- For all other MassHealth providers, please email the MassHealth .
You May Like: Dentists In Logan Utah That Accept Medicaid
Provider Termination And Exclusion List
The following lists contain:
- Individuals or entities whose participation in the Medicaid program has been terminated for cause under the provision of WAC 182-502-0030 or 388-71-0551 388-71-0540 388-71-0544 388-110-260 .
- Medicaid providers who have been excluded from participation .
Not every action taken by the Department of Social and Health Services or the Health Care Authority involves a finding of wrongdoing ). Individuals terminated without cause pursuant to WAC 182-502-0040 are not included on this list.
The Affordable Care Act requires that all ordering physicians or other professionals who prescribe, order, or refer services to Medicaid or provide services under the State Plan or under a waiver of the plan to be enrolled as participating providers ). Therefore, any non-enrolled provider, including any provider who is terminated from the Medicaid Program, for any reason, is not permitted to provide services to Medicaid recipients.
Reasons For Suspension Or Exclusion
Providers may be suspended or excluded due to
- Not complying with participatory requirements of the MassHealth program
- Being excluded under Medicare
- Suspension of exclusion by any other state Medicaid agency
- An inactive, terminated, suspended, or revoked license or authorization to provide services
- Conviction of health care fraud
- Pleading guilty to or being convicted of criminal activity materially related to Medicare or Medicaid
- The U.S. Department of Health and Human Services initiating an action that is binding on a provider’s participation in the Medicaid program
If the period of suspension or exclusion expires, reinstatement rights into the MassHealth Program are not automatic. The individual or entity must submit an application for re-enrollment and cannot submit claims for services rendered to MassHealth members until they are notified that the application has been approved. Once approved, the providers name will be removed from the published list of suspended and excluded providers.
Don’t Miss: How To Become A Medicaid Consultant
Learn About Suspended Or Excluded Masshealth Providers
The MassHealth program maintains a list of providers who have been suspended or excluded from participating in the MassHealth program. This list is updated monthly and reflects suspensions or exclusions effective on or after March 23, 2010. They are listed according to the provider type at the time of such action.
Where Did Healthcare Exclusions Come From
Since the early 1970s, the Department of Health and Human Services , Office of the Inspector General has the authority and responsibility to protect the integrity of Department of Health & Human Services programs as well as the health and welfare of program beneficiaries. The OIG is acting in the peoples best interest to regulate and enforce violations of healthcare fraud, waste, and abuse.
The OIG was created in 1976 and oversees more than 300 other HHS programs. The most common and well known are Medicare, Medicaid, TriCare, and CHIPs. Others include the Centers for Disease Control and Prevention, National Institutes of Health, and the Food and Drug Administration. The OIG for HHS is the largest Inspector Generals office in the federal government, with approximately 1,600 employees. The current Inspector General for HHS is Daniel Levinson.
Also Check: Will Medicaid Pay For Portable Oxygen Concentrator
State Medicaid Exclusion List
Individual states maintain a Medicaid exclusion list as well as federal. Employers need to search these in addition to the OIG LEIE and the SAM.gov. Today, there are 42 states that have a state Medicaid exclusion list. Each year, more state Medicaid exclusion lists are added and made publicly available. Efficiency and accuracy from Medicaid Fraud Control Units reporting excluded individuals or entities to the OIG have been a serious issue, and many times can leave HR professionals and compliance programs open to risky situations if they are solely checking federal databases.
Entities Participating Or Applying To Participate In Masshealth
On a monthly basis, any entity participating or applying to participate in the MassHealth program must search the list on this page, as well as the list of excluded individuals and entities of the federal Office of Inspector General to determine if any existing employee, contractor, owner, or board member has been suspended or excluded from participation in the Medicaid program.
In addition, the provider must immediately report any discovered exclusion of an employee or contractor to the Executive Office of Health and Human Services .
You May Like: How Do I Add My Newborn To My Medicaid
State Medicaid Exclusion Sources
State Medicaid exclusion sources are varied and present significant challenges to manual screening processes. They publish exclusion records in different formats and with varying amounts of data, making it difficult and resource-intensive to identify a match within your population.
Learn more about Why Your Low-Cost Exclusion Monitoring is Costing More than You Think.
Why is it important to check every available state exclusion source? Because if an individual or entity is excluded in one state, theyre excluded in every state. And because 50% of all state Medicaid exclusions never show up on the OIG LEIE.
What Is The Medicaid Exclusion List
The formal term for the Medicaid Exclusion list is called the List of Excluded Individuals/Entities , which is managed by the Office of the Inspector General . It is also sometimes referred to as the OIG Exclusion List. Its purpose is to provide information to the healthcare industry, patients, and the public about people and entities currently excluded from participating in federally funded healthcare programs like Medicare and Medicaid.
The OIG has been implementing exclusions since about 1981, but the Department of Health & Human Services first began imposing them in 1977. Contractors and providers may become excluded for a number of reasons, including:
- A conviction of Medicare or Medicaid fraud
- Patient abuse or neglect
- Felony convictions for healthcare-related fraud, theft, or other financial misconduct
- Felony convictions relating to the unlawful manufacture, distribution, prescription, or dispensing of controlled substances
As a result, employers and healthcare organizations that participate in federally funded healthcare programs are barred from hiring or contracting with excluded individuals or entities, which may pose several risks to their business, employees, and patients.
Read Also: How To Find Your Medicaid Number
