Medicaid For Gastric Sleeve Coverage Guidelines
Medicaid for gastric sleeve surgery is a possibility. Medicaid for gastric sleeve surgery may only be covered if used as a primary or a final stage surgery for Medicaid beneficiaries that have one of the following medical signs that poses a high risk for a standard bariatric procedures :
- Morbidly obese
- Has a history of multiple previous abdominal operations with a possible presence of intra-abdominal adhesions.
- A presence of an inflammatory bowel disease.
- Has hepatic cirrhosis with an elevated liver function tests.
- Has undergone an organ transplant or the patient is currently taking an immunosuppressive therapy that is associated with the transplant operation.
- Has a severe systemic disease.
Medicaids Bariatric Surgery Requirements
What are the specific requirements for Medicaids bariatric surgery program?
Medicaid coverage for weight loss surgery is decided on a state-by-state basis meaning some states cover it, and others do not. Medicaids requirements for weight loss surgery are different when compared to other insurances because it is unique in who they cover and how they include these patients. You will need to meet several requirements to qualify for surgery through Medicaid. You will also need to be free from any medical issues that may prevent you or create a risk for you to have surgery. If you pass these two tests, then Medicaid generally will pay for your weight loss surgery.
Brief Overview Of Medicaid Requirements
To qualify for weight loss surgery while using Medicaid, the patient must still meet the requirements of what most other insurance companies state:
- Your Body Mass Index exceeds 35 and you must have at least one comorbidity, such as high blood pressure, sleep apnea, high cholesterol or diabetes.
- If you are below the age of 21, you need to have a Body Mass Index exceeding 40 with at least one of the aforementioned comorbidities.
One of the requirements for Medicaid to pay for your surgery coverage is that you need to have your weight loss surgery done through a Center for Excellence. Bariatric Center for Excellence accreditation is designed to indicate which bariatric surgery centers have achieved a level of excellence in both surgery and patient care. Medicaid requires that you visit one of these specific centers to guarantee that you get the best possible treatment. Fortunately Western Bariatric meets the criteria, and is one of the nations Bariatric Centers of Excellence.
Your states Medicaid office can be found, here.
Contact Western Bariatric today and let us help you start your weight loss journey.
Read Also: Does Missouri Medicaid Cover Assisted Living
How To Get Medicaid Approval For Weight Loss Surgery
If the Medicaid provided by your state covers bariatric surgery, you must consult your physician. Medicaid accepts coverage when there is a medical need for the surgery. It is vital to have a physician who can share relevant information for the medical necessity of bariatric surgery for the patient. Further, to assess the situation, a physician can recommend the patient to approved surgeons.
Approved surgeons help you understand the surgerys basics and different options you may have. After you make a decision, you need to go through some tests and then consult the Medicaid office for pre-approval of the surgery. The process is time-consuming and requires patience as well as perseverance.Before approval, you may have to attend classes to understand the surgery, nutritional requirements, lifestyle changes, and exercises, which are mandatory post the operation. This ensures that the patient understands all implications of the surgery and whats essential to make it successful.
With necessary provisions, you may get approval from Medicaid. These provisions can further include additional classes or further testing. After approval from Medicaid, your surgeon needs to determine your ability to undergo the procedure. This can include medical preparation, blood work, and X-rays. Finally, the surgery is booked. Hence, you get a step closer to a healthier lifestyle and your weight goals.
How To Get Approved For Weight Loss Surgery In Mexico
Since weight loss surgery costs around $15,000 $30,000+ in the US, more and more patients are heading over to Mexico to receive the procedure. Statistics show that almost 1.4 million Americans crossed the border in 2018 to undergo medical treatment including some form of bariatric surgery.
If your insurance carrier is refusing to cover your bariatric procedure and youre wondering how to get weight loss surgery approved in Mexico, here are some simple guidelines for you:
You have to meet the following criteria to be eligible for weight loss surgery in Mexico:
- You must have a body mass index of 30-35
- You must have BMI for gastric sleeve of 35-40+
- You must be suffering from obesity-related illnesses like diabetes, breathing issues, heart problems, hypertension, etc.
Bariatric surgery in Mexico costs around $3,599 $5,500 for inpatient treatment. This means everything from ground transportation and hotel stay to cost of medications is included in this price tag. However, if you cant afford to pay for the surgery all at once, our Jet Medical Tourism® team can provide you with super affordable payment plans as well.
Recommended Reading: How Poor Do You Have To Be To Get Medicaid
Medicaid Guidelines Coverage Bariatric Surgery
- That the patient is psychologically mature and can cope with the post-surgical changes.
- That the patient and the parent/guardian understand and will follow the required changes in eating habits.
- That pre-operative nutritional and psychological services are available.
- How the patient will accept post-operative surgical, nutritional, and psychological services.
- To correct complications from bariatric surgery such as band malfunction, obstruction or stricture.
- To convert to a Roux-en-Y gastroenterostomy or to correct pouch failure.
Behavioral health services are not considered part of the bariatric surgery proper, but may be provided as part of the pre-operative or post-operative phase of bariatric surgery.
Gastric Sleeve Requirements: Do I Qualify For It
Posted by Jet Medical Tourism® | Last updated Nov 29, 2021 | Gastric Sleeve Surgery, Medical Tourism Mexico, Obesity, Weight Loss Surgery Mexico
Gastric sleeve requirements have largely been standardized by the medical community, but individual factors still make a difference. During your initial consultation with a bariatric surgeon, one of the first questions you should ask is: Do I qualify for gastric sleeve? Your surgeon will determine your candidacy within defined parameters, but they do have a wide discretion while making a decision.
Meeting the requisite gastric sleeve qualifications is vital for your own safety and success of the procedure. Any bariatric surgery is a major procedure, and not everyone is a solid candidate for it. A responsible weight loss surgeon will educate you about VSG surgery qualifications and provide you a clear medical opinion. They will only recommend you for this surgery, if you are comfortably able to meet all the criteria for gastric sleeve.
Learn about your gastric sleeve requirements from a leading bariatric surgeon. Call or email Jet Medical Tourism® today to schedule a free consultation.
Recommended Reading: What Is The Difference Between Medicare & Medicaid
Which Weight Loss Procedures Does Medicaid Cover
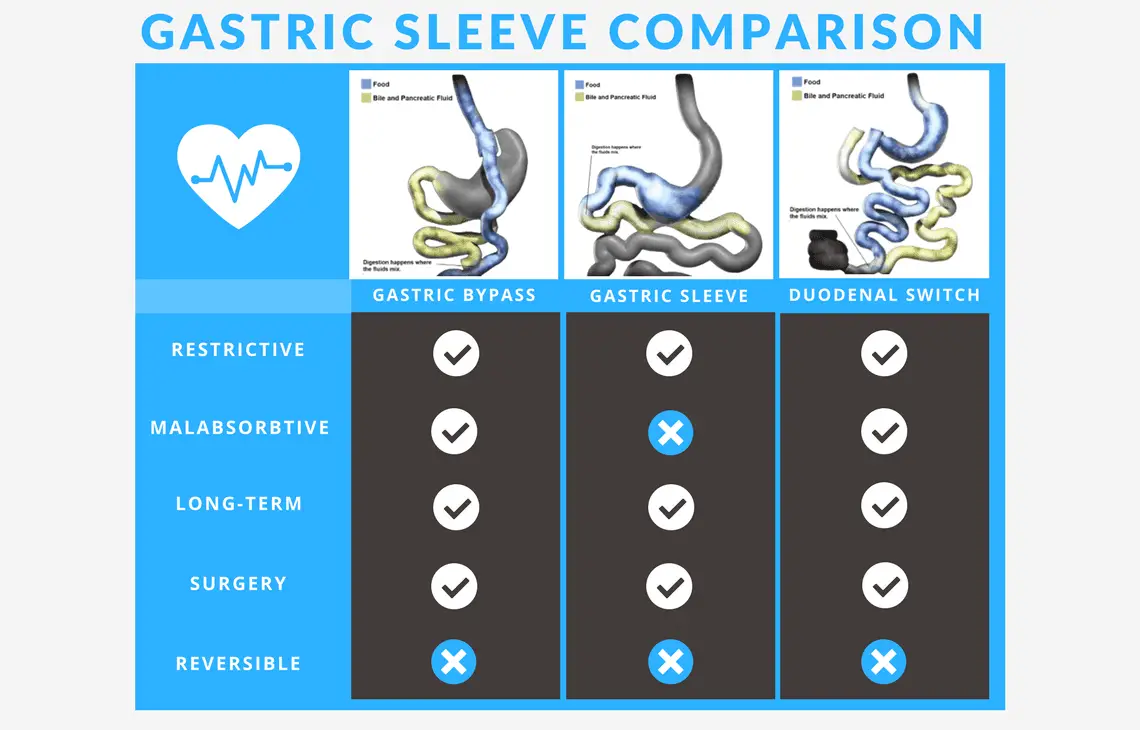
In most cases, Medicaid covers Lap-Band Surgery, gastric sleeve surgery, and gastric bypass. These are not only readily covered by Medicaid, but also among the most common surgeries recommended. In certain situations, these are accepted as medically vital to the life and wellbeing of the patient.
Gastric bypass reduces the stomach size and bypasses a part of the intestine. Hence, you eat less and the food is also sent straight to the lower part of your intestine. Due to this bypass, absorption of nutrients and calories is reduced. Hence, it reduces food intake and additionally helps result in weight loss. In Lap-Band surgery, the top part of the stomach is covered with silicone bands with balloons. This reduces the space for holding food. Also, the entry to the stomach becomes smaller. The procedure is less invasive compared to others and is done laparoscopically. Additionally, it is preferable as it is easy to reverse and the band can be adjusted. Finally, in gastric sleeve surgery, a sleeve-shaped, smaller stomach is created. As the food does not have much space to sit, it is readily passed to the intestines. Hence, it too reduces intake of food and calorie absorption.
State Insurance Law Analysis
We reviewed state laws and regulations for private insurance in both the individual and small-group markets for statutory provisions that expressly prohibit or regulate medical insurers’ medical underwriting or eligibility exclusion practices where obesity or health status is used as an independent risk factor and statutory provisions mandating coverage of obesity-related treatments. The 2004 CMS policy change allowed obesity to be considered a medical condition, and, thus, considered under the term health status.
We conducted a state-by-state document review of state insurance laws and regulations obtained via Internet search of the following websites: each state’s Department of Insurance, National Association of Health Underwriters, Georgetown University Health Policy Institute, National Association of Insurance Commissioners, and legal searches of state insurance codes from Westlaw and Lexis Nexis®. We searched state legislature websites for relevant enrolled legislation that had not yet been compiled into the official state code.
Key words included obesity, weight loss, bariatric surgery, mandated coverage, nutritional counseling, morbid obesity, gastric bypass, underwriting, risk factors for underwriting, exclusions, and preexisting conditions.
Also Check: Pregnancy Medicaid Texas Phone Number
State Regulation Of Insurers’ Obesity
About 68% of Americans obtain health-care benefits through private health insurance plans, many of which are regulated at the state level. Some states require insurers to offer specific health benefits or access to certain types of providers. Other state regulations affect the rating rules that insurers use to set premiums or to evaluate people for coverage through medical underwriting.
Privately insured people are overwhelmingly insured in the employer-based group market, with only 6% of insured people covered through the individual market. In the small-group market, we found that 41 states and the District of Columbia either explicitly or implicitly allow insurers to use health status or obesity as an independent factor in determining rates. Only nine states require small-group health plans to use a community or an adjusted community rating, where the premiums would be based on the expected claims of the community, not the individual employer group. These findings are consistent with the consumer information available from the National Association of Health Underwriters.
Thus, in most states, an employer’s health insurance premiums can be affected by the weight of his or her employees. Obesity carries high health-care costs thus, as obesity rates rise, increasing health insurance premiums may lead employers to drop health insurance coverage, increase premiums and cost-sharing for employees, or lower wages for workers.
Medicaid Requirements For Bariatric Surgery 2020
To qualify for Medicaid weight loss surgery, you must meet the following criteria:
- Your BMI must be over 35.
- Your BMI must be over 40 if you are below the age of 21.
- You must have at least one obesity-related illness.
- You must have documentation showing that you tried to manage your weight in the past, but those attempts failed.
- You must have completed a 6-months long weight loss program under medical supervision .
- You must have a printed letter from your doctor recommending the medical necessity of bariatric surgery.
- You need to pass a psychological evaluation showing you can change your lifestyle for the better after surgery.
- Your weight loss surgery must be performed at a Center for Excellence only.
Also Check: Does Medicaid Cover Gastric Balloon
State Medicaid Coverage Of Adult Obesity Treatment
All state Medicaid programs covered at least one obesity treatment modality. Eight states covered all three treatment categories with various restrictions. Twenty-six states explicitly covered nutritional consultation, while 20 explicitly did not. Drug therapy was the least frequently covered and discussed treatment category only 10 states covered it, while 33 states made no mention of it in their provider manuals. Bariatric surgery was the most frequently covered treatment it was also the least likely to be explicitly not covered . Three states explicitly excluded nutritional assessment/counseling and drug therapy, while covering bariatric surgery .
Find A Gastric Sleeve Surgeon
SECTION SUMMARY:
- You can ask a local bariatric practice for a free insurance check or cost quote
- You can attend a free in-person seminar or an online webinar offered by a local weight loss surgeon
- You should schedule a phone or in-person consultation , if you are interested in learning more about weight loss surgery
Do You Qualify for a Bariatric Procedure?
Patients who qualify for bariatric surgery usually:
- Are at least 80 lbs overweight
- Are between 18 and 75 years old
- Have a history of failed weight loss attempts
- Thoroughly understand that the procedure is just a tool long-term success requires significant diet and lifestyle changes
The minimum bariatric surgery qualifications include:
- A body mass index of 40 or more
- OR a BMI between 30 and 39.9 with a serious obesity-related health problem like diabetes, high blood pressure, sleep apnea, high cholesterol, joint problems, or others
- OR a BMI of 30 to 40 with or without health issues for the gastric balloon procedure
To calculate your BMI, enter your height and weight into the tool, then click the Calculate BMI button.
Check My Insurance Tool
Bariatric surgery insurance coverage varies by insurance policy:
Individual/Family Plans & Small Group Plans Coverage varies by state coverage is required by the Affordable Care Act in some states
Large Group Plans Coverage depends on whether your employer has chosen to add it to your policy
Medicare and Medicaid Bariatric surgery is covered
- Gastric sleeve
Don’t Miss: Eye Places That Take Medicaid
Does Humana Cover Weight Loss Surgery
Yes, Humana covers weight loss surgery unless you have chosen a plan that specifically excludes bariatric procedures.
Assuming you are covered, you have to meet the following criteria to qualify for Humana weight loss surgery:
- You must be 18 years of age or older.
- You must have a BMI of 40 or higher.
- You must have a BMI of 35-39, and at least one obesity-related illness including joint disease, diabetes, and hypertension.
- You must have tried a medically-supervised weight loss program for at least 6 months.
- You must have a signed letter from your primary doctor recommending mandatory bariatric surgery.
- You must be able pass a psychological evaluation that shows you can adopt a healthier lifestyle.
Reasons You Wont Qualify For Gastric Sleeve
SECTION SUMMARY:
- Your BMI is not high enough
- You have only limited previous diet attempts
- You have certain physical or mental health conditions
- You are pregnant or plan to be pregnant in the near future
Characteristics that may disqualify you from having gastric sleeve surgery include:
- Low body mass index see BMI requirements at the top of this page
- Under 18 years old
- Limited past diet attempts
- Current pregnancy click here and here for surgeon Q & A about getting pregnant after having the gastric sleeve procedure
- Current infection
- Having very high operative risks, such as a patients with a severe heart or lung disease
- Substance abuse
- Major mental health issues that may prevent firm understanding of surgery and required lifestyle changes
- inflammatory disease or condition of the gastrointestinal tract, such as ulcers, severe esophagitis, Barretts esophagus, or Crohns disease
- Portal hypertension
- Abnormal esophagus, stomach, or intestine
- Cirrhosis
- On chronic, long-term steroid treatment
- Not willing to follow long-term diet, vitamin, or exercise regimen
- Autoimmune connective tissue disease
- Uncontrolled or untreated psychiatric disorder
- Suicide attempt in last 18 months or multiple attempts within last 5 years
Conditions that may or may not disqualify you include:
- Severe GERD
If you have any of the above issues, contact a weight loss surgeon to discuss your options.
Don’t Miss: Anthem Medicaid Ky Dental Providers
Weight Requirements For Vsg Surgery
When you ask your surgeon about How do I qualify for gastric sleeve, they will focus on your BMI, and not your body weight. This is because the body weight is meaningful as a parameter only in related to your height. In other words, a person who weighs less than you, but has a shorter height might be considered clinically obese, while you may not. This is because the BMI is function of both weight and height.
While weight requirements for gastric sleeve matter only indirectly, what is more important is whether you have tried to reduce weight through natural means. Reputable bariatric surgeons will prefer a gastric sleeve candidate who has first tried to reduce weight through diet and exercise, but failed. When your body weight becomes resistant and does not respond to natural diet and exercise, you may fulfill VSG surgery qualifications more ideally.
United Healthcare Bariatric Surgery
Most insurance policies by the United Healthcare dont cover bariatric surgery. But there are some rare plans that include it as long as it is deemed medically necessary by your primary care physician.
Also, if you live in a state where insurance companies are required to cover bariatric procedures, your United Healthcare insurance policy may provide partial or full coverage for the same.
Don’t Miss: Dermatologist In Lake Charles That Accept Medicaid
What Is Gastric Bypass
A gastric bypass procedure involves two primary components that change the way your digestive tract is routed.
- The first part of gastric bypass involves sectioning off the top of the stomach. This is done by creating a small pouch at the top of the stomach that is roughly one ounce in volume.
- The second part of gastric bypass involves dividing the small intestine into two parts. First, the bottom portion of the divided small intestine is connected to the new stomach pouch. Then, the top portion of the divided small intestine is reconnected further down the bottom portion of the small intestine.
There are two types of gastric bypass surgery: open gastric bypass and laparoscopic gastric bypass. Open gastric bypass surgery is performed using a large incision in the abdomen and is typically invasive. Laparoscopic gastric bypass surgery is performed using a laparoscope and is typically much less invasive.
The entire gastric bypass procedure creates a bypass of the normal functions of the digestive system, which greatly decreases the amount of food a person can eat. In turn, this decreases caloric intake, as well as the absorption of nutrients. The decreased intake and absorption of foods from gastric bypass contribute to long-term weight loss.
