How To Check The Status Of A Medicaid Application
You can check your Medicaid application status through your program office. Insurance representatives can review your claim and see whether a decision has been reached regarding your case. If you applied online, you may also be able to check the status of a Medicaid application by going to the same portal you applied through.
Pps Survey: Weve Heard Your Concerns
Top 3 Concerns from the PPS:
- Transportation that shows up late to pick up or drop off patients
- Unable to schedule pickups for support groups, care management, pharmacy, etc.
- The need to schedule transport 3 days in advance of appointment
Top Questions from the PPS:
- What process improvements will be implemented?
- Will there be changes in funding for transportation services?
- Can transport services be offered for same day appointments?
- Will PPS be able to work directly with these companies to ensure services are accessible and target the areas of greatest need?
- How does the FFS Medicaid transportation fit into the DSRIP way of thinking ?
Who Are The Transportation Managers
- Currently the Department contracts with two Transportation Managers
- Medical Answering Services, LLC
- All Counties North of NYC https://www.medanswering.com/ 8505340
You May Like: Iowa Dhs Medicaid Income Guidelines
Public Transportation Automated Reimbursement
- NYC
- Medical providers prepurchase Metrocards from the Metropolitan Transportation Authority and distribute them to eligible Medicaid enrollees at the time of appointment.
- The medical provider submits realtime for reimbursement of the MetroCard.
- PTAR reimburses the medical provider $5.50/claim.
What Does Medicaid Cover In New York
Medicaid gives beneficiaries quite a broad range of coverage with regards to health insurance. This includes visits to the doctor, hospital stays, care in a nursing home, home health care, and more.
Medicaid also pays for prescriptions. If you ever have to pay a copay, it will be one that is relatively small.
Read Also: Does Medicaid Cover Therapy In Michigan
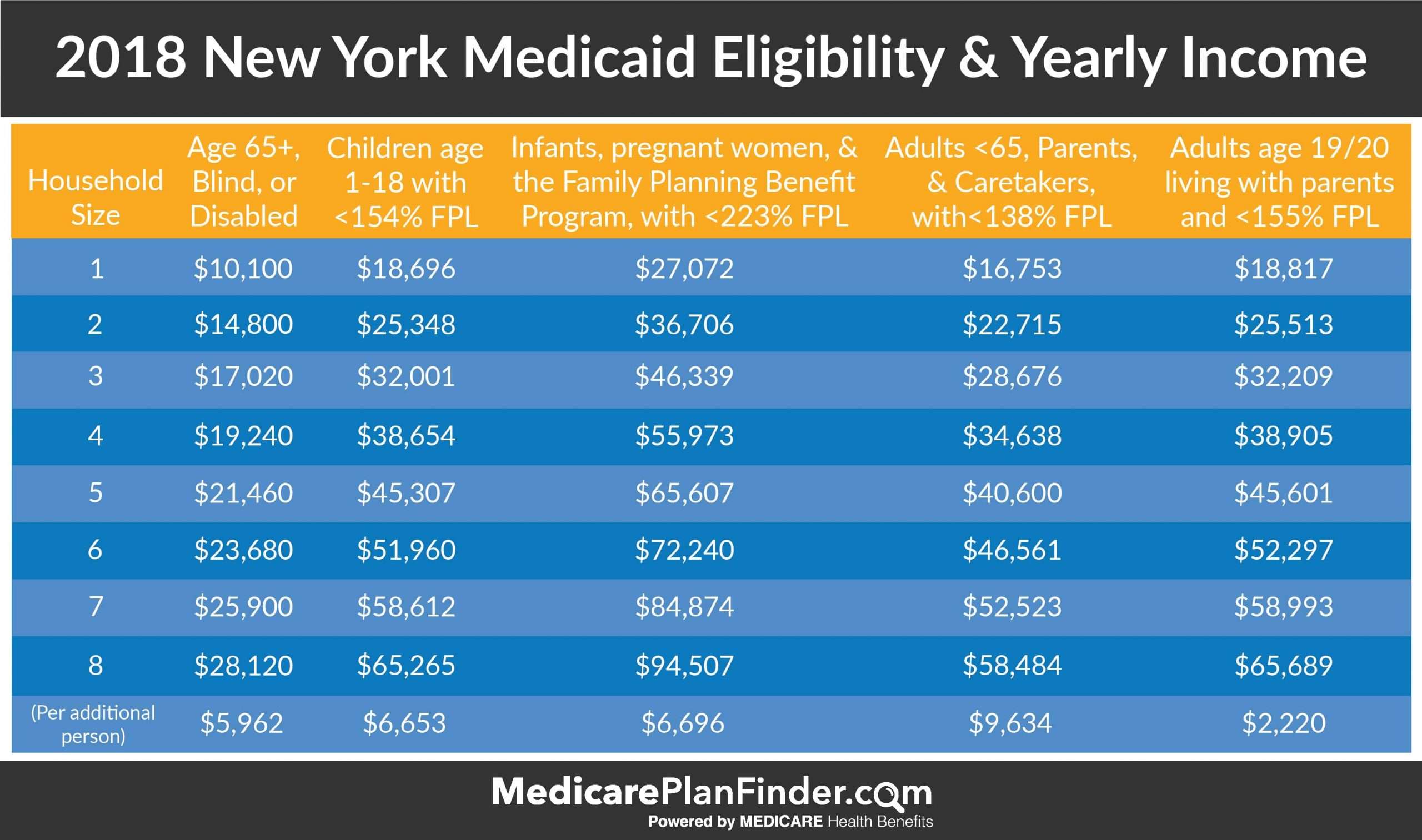
New Yorks Requirements For Medicaid Qualification
Eligibility for New York Medicaid is something that is determined by a few different factors that have been developed by the New York state department. The benefits given by Medicaid will aid those who are unable to pay their medical bills, such as those on SSI and others who meet the requirements for eligibility. Before those requirements even come in to play though, you first have to fall into one of the following categories:
- Adults who have an income that does not exceed 138% of the FPL
- Infants and/or women who are pregnant whose income does not exceed 218% of the Federal Poverty Level
To qualify for Medicaid – aside from being in one of the preceding two categories – you need to meet predetermined requirements for eligibility. You have to reach, without exceeding certain income thresholds. Additionally, you have to prove that you are a citizen of the US as well as proving that you are a state resident. You also need to have documentation regarding your living situation and your marriage license if you are married, along with your SSN .
How To Apply For Medicaid In In New York
Due to the fact that you must stick to specific instructions with regards to submitting your paperwork, the application guidelines are different in New York than those in other states. The qualifying criteria are actually spread into two separate groups. These are MAGI and non-MAGI groups. You have to file differently depending on which group you fall into.
When it comes to MAGI application guidelines, this group includes foster children, children under 19, beneficiaries of the FPBP , relatives of caregivers or parents, women undergoing fertility treatments and pregnant women. If you fall into this group, you will have to apply for the Medicaid program via the New York State Department of Health Marketplace.
To be eligible under the non-MAGI eligibility group, you must be a recipient of one of the following:
- Medicaid Cancer Treatment Program
- ADC-related medical needy, or the
- Medicare Savings Program
If you belong to this group, you should apply for Medicaid at your local Department of Social Services.
Also Check: What Is The Household Income Limit For Medicaid
How Long Does A Medicaid Application Take To Process
When you apply for Medicaid, the processing agency generally has 45 days to review your application. However, there can be delays regarding how quickly your application is processed if you do not provide all the necessary materials when you first submit your petition. To avoid delays in coverage, make sure you submit a complete application as soon as possible. Likewise, remember that there are no restrictions as to when you can submit your Medicaid application. The best time for you to file your application is as soon as you believe you qualify for support.
Which Mode Of Transportation Is Necessary
Assessing the most cost effective and medically appropriate mode of transportation.
Medical Justification “2015” Form:
- Requires a medical professional to provide the mobilityrelated reason why the enrollee requires a specific mode of transportation
- Reasons for decreased mobility could be that the enrollee is wheelchairbound, underwent recent surgery to a limb, is blind, or has an unstable gate.
Form 2015
Maintain Original in Medical Record
VERIFICATION OF MEDICAID TRANSPORTATION ABILITIES
Patient Name: _______________________________ Patient Date of Birth __ /__ /____ Patient Medicaid Number: ___________________
Patient Address: ___________________________________________________ Patient Telephone: _______________________________
You May Like: Blue Cross Blue Shield Medicaid Dental Providers
How To Apply If In Ny City:
If you are in New York City, you can easily obtain applications from Human Resources Administration. You can also request information and applications on phone by calling at 718 557 1399.
NOTE: If you need any further assistance, you can call helpline at 693-6765.
Other requirements for applying
In order to apply for Medicaid, you will need to provide
- Proof of age
- Proof of citizenship
- If someone above 65 years of age, disabled or blind lives with you, you will need to provide proof of your income and resources
- Proof of your residence
- If you have any other insurance, you’ll be required to provide its proof and information about it
Medicaid Benefits
Medicaid provides a comprehensive coverage for various health services including
- Inpatient and outpatient services
- Home health care through approved agencies
- Access to smoking cessation agents
- Lab facilities and access to tests
- Eye, dental and mental health services
- Prescription drugs, medical supplies, and necessary medical equipment
- Transportation services
If You Qualify Under A Magi Eligibility Group You Will Have To Provide Documents To Verify Eligibility If Necessary
- If you are applying for Medicaid through the Marketplace , you may attest to your household income for the upcoming year. If your income is different than the income found on the data matches, income documentation may need to be provided.
- Citizenship/Immigration status and social security number will be verified through federal data sources. If citizenship/immigration status or social security number does not match, documentation must be provided.
Recommended Reading: Blue Choice Healthy Connections Medicaid
Medicaid Eligibility For Nursing Home Care
In order to qualify for Medicaid, your life savings cannot be greater than the Medicaid resource limit. Certain assets are not counted as being part of your life savings. For example, if you have a spouse living in the family home, then the home does not count for Medicaid resource limit purposes.
If your life savings is higher than the Medicaid limit, you will not be eligible to receive Medicaid coverage for your nursing home or home care costs. You will be told to spend your life savings towards your cost of care until you are down to the Medicaid levels.
You should never assume that it is too late. Quite often you have legal options to save some or all of your life savings even if you are already in a nursing home. The Koldin Law Center, P.C. Medicaid Law Attorneys can represent you throughout the entire Medicaid process. There is something you can do.
There are many special exceptions to the basic Medicaid rules where additional assets can be protected.
How To File New York Medicaid Applications By Phone
Filling out a Medicaid application form on your own can be confusing and time-consuming. Instead of calling up Medicaid caseworkers to ask where to apply for Medicaid, employ a representative for assistance by phone from the comfort of your home. Let a knowledgeable agent assist you immediately. Just call the designated number provided by the NY Department of Health, and you can get started right away.
When it comes to your application for Medicaid, a lot of private and personal information is necessary. However, there is no cause for concern when speaking with an official Medicaid worker by phone, as these representatives work directly on behalf of the state. Do not hesitate to call the helpline for Medicaid information such as assistance with completing your application forms, so you can be on your way to collecting health benefits soon.
Recommended Reading: Wellcare Of North Carolina Medicaid
Eligibility Requirements For Medicaid In Ny
Since Medicaid is designed for low-income individuals and families, there are specific income and asset requirements that you must meet, depending on various factors, as we will discuss below.
To be eligible for Medicaid in NY, you must also meet the following eligibility criteria.
- You must be a U.S. national, citizen, permanent resident, or legal alien.
- You must be a resident of New York.
- You must need help with medical care/insurance coverage.
- Your financial situation must fall within the low-income category .
In addition to these requirements, you must also be one of the following:
- Pregnant
- 65 years of age or older
Does Medicaid Cost Me Anything
Some services may include a small copay, such as clinic visits, laboratory tests, medical supplies, overnight hospital stays, emergency room visits for nonâemergency services, prescription drugs, and over the counter drugs.
Certain people are exempt from copays entirely, including anyone who opts for a Managed Care Plan. Talk to your caseworker for more details about copays specific to you.
There is an annual limit of $200 for out of pocket copayments, after which you will not need to pay any more copays that year. No provider can refuse treatment for inability to pay and must bill you for unpaid copays if needed.
Recommended Reading: Vermont Medicaid Dental Fee Schedule
What Proofs Will You Have To Bring To Apply For Medicaid
The evidence you need will vary depending on your age, medical conditions, and a few other factors.
These are some general requirements to give you an idea of what is needed.
Your case worker will let you know if there are any specific requirements for your application. Contact your local Medicaid office for more details.
Here is a list of the documents that you will need when applying for Medicaid in NY.
Nys Medicaid Otc Formulary And Prescription Drug Coverage
The NYS Medicaid formulary is very comprehensive the PDF is 659 pages long! NYS Medicaid providers are expected to select the cheapest option of any drug they prescribe to a New York Medicaid beneficiary. In most cases, this means that the generic form of the drug will be selected. If you notice that your doctor prescribes a brand-name drug, ask and make sure that it is the most affordable option. NYS Medicaid may cover brand-name drugs as well, but generic options are almost always cheaper. Generic drugs usually provide the same benefits as their brand-name counterparts.
In some cases, New York Medicaid may provide reimbursements for over-the-counter products as well. To get that reimbursement, your doctor will need to provide a fiscal order, which is sort of like a prescription for over-the-counter drugs and products.
You May Like: Georgia Application For Medicaid And Medicare Savings
Frequently Asked Questions For Current Medicaid Beneficiaries
What is a Community Spouse?
A community spouse is someone whose husband/wife is currently institutionalized or living in a nursing home. The community spouse is not currently living in a nursing home and usually resides at the couple´s home.
I am a community spouse. Will I be allowed to keep any income or resources?
If your spouse is institutionalized or living in a nursing home, you will be permitted to keep some income known as a minimum monthly maintenance needs allowance . If you are currently receiving income in excess of the minimum monthly maintenance needs allowance, you may be asked to contribute twenty-five percent of the excess income to the cost of care for the institution
How do I find my local Medicaid office?
The Medicaid office is located in your local department of social services. A listing of offices can be located here:
If you live in the five boroughs of New York City, your offices are run by the Human Resources Administration . A listing of offices can be found here:
How do I order a new benefit card?
If your Medicaid is with your LDSS, to order a new Medicaid Benefit Identification Card, please call or visit your
If your Medicaid is with the and you need to order a new benefit card please call the call center at 1-855-355-5777.
Members residing in the five boroughs of NYC can call the HRA Infoline at 1 557-1399 or the HRA Medicaid Helpline at 1 692-6116.
How often do I have to renew?
Notification Of Determination By Nys Doh
A written determination of approval or denial of the submitted application will be sent to the provider.
If the application is approved, a letter containing the provider’s MMIS ID Number, the effective date when services may be provided to an enrolled client, and other information related to their enrollment will be sent to the enrollee.
Also Check: What’s Better Medicare Or Medicaid
How Do I Apply For Medicaid
You can apply for Medicaid in any one of the following ways:
- Write, phone, or go to your .
- In New York City, contact the Human Resources Administration by calling 557-1399.
- Pregnant women and children can apply at many clinics, hospitals, and provider offices. Call your local department of social services to find out where you can apply.
> >
How Do Enrollees Get Transportation
- The medical provider or the enrollee contacts the appropriate transportation manager to request transportation:
- The Department of Health´s policy requires 3 days´ notice for nonurgent trips. Every effort is made to assign trips made with less than 3 days´ notice, as available transportation options decrease as vendors shore up their daily trip rosters.
- Urgent trips and hospital discharges are not subject to the 3day window, and are considered priority.
Recommended Reading: Is Medical Marijuana Covered By Medicaid
From The County To The State
- Prior to 2011 Medicaid transportation was administered by county Departments of Social Services.
- The 201011 State Budget gave the Commissioner of Health the authority to assume the administration of Medicaid transportation from the counties.
- The 2010 Medicaid Administration Reform and subsequent Medicaid Redesign Team initiatives intended to improve the program by:
- Relieving the counties with the burden administering Medicaid transportation
- Improving program quality
- Achieving greater department accountability
- Standardizing the application of Medicaid transportation policy
If You Qualify Under A Non
- If you are a U.S. citizen and provide a valid Social Security Number , a match with the Social Security Administration will verify your SSN, date of birth and U.S. citizenship. If SSA verifies this information, no further proof is needed. The SSA match cannot verify birth information for a naturalized citizen. You will need to submit proof of naturalization or a U.S. passport.
- Proof of citizenship or immigration status*
- Proof of age , like a birth certificate
- Four weeks of recent paycheck stubs
- Proof of your income from sources like Social Security, Veteran´s Benefits , retirement benefits, Unemployment Insurance Benefits , Child Support payments
- If you are age 65 or older, or certified blind or disabled, and applying for nursing home care waivered services, or other community based long term care services, you need to provide information on bank accounts, insurance policies and other resources
- Proof of where you live, such as a rent receipt, landlord statement, mortgage statement, or envelope from mail you received recently
- Insurance benefit card or the policy
- Medicare Benefit Card **
Proof of Medicare application can be:
- Your award or denial letter from the Social Security Administration, OR
- Your on-line confirmation letter stating that you have applied for Medicare with the Social Security Administration.
Apply Now:
The following are exempt from all Medicaid co-payments:
Recommended Reading: Does Medicaid Cover Auto Accidents In Michigan
